Abstract
Background
Patients hospitalized with cirrhosis, ascites, and elevated INR often experience delays in timely diagnostic paracentesis.
Aims
Identify whether delays in diagnostic paracentesis were associated with adverse outcomes in a hospital system serving a large disadvantaged population.
Methods
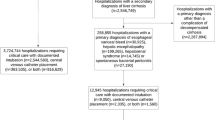
Retrospective cohort analysis of patients admitted from January 2017 to October 2019 with cirrhosis, ascites, and INR ≥ 1.5 across a multi-hospital health system in central Texas. We examined demographic and clinical characteristics of patients with diagnostic paracentesis (1) ≤ 24 h; (2) > 24 h; (3) therapeutic only or no paracentesis. We used logistic regression to examine differences in clinical outcomes controlling for confounders.
Results
479 patients met inclusion criteria. 30.0% (N = 143) were Latino, 6.7% (N = 32) African American, and 67.8% (N = 325) under or uninsured. 54.1% of patients received a diagnostic paracentesis ≤ 24 h of admission and 21.1% did not receive a diagnostic paracentesis during the hospitalization. Undergoing diagnostic paracentesis > 24 h of admission was associated with a 2.3 day increase in length of stay (95% CI 0.8–3.8), and OR 1.7 for an Emergency Room visit within 30 days of discharge (95% CI 1.1–2.7) compared to receiving a diagnostic paracentesis ≤ 24 h. Patients receiving diagnostic paracentesis in radiology were more likely to have a delay in procedure OR 5.8 (95% CI 2.8–8.6).
Conclusion
Delayed diagnostic paracentesis is associated with increased preventable healthcare utilization compared with timely diagnostic paracentesis. Health systems should support efforts to ensure timely diagnostic paracentesis for patients with advanced liver disease, including performance at the bedside.

Similar content being viewed by others
References
Hirode G, Saab S, Wong RJ. Trends in the Burden of Chronic Liver Disease Among Hospitalized US Adults. JAMA Network Open 2020;3:e201997.
Tapper EB, Parikh ND. Mortality due to cirrhosis and liver cancer in the United States, 1999–2016: observational study. BMJ. 2018. https://doi.org/10.1136/bmj.k2817.
Gines P, Quintero E, Arroyo V et al. Compensated cirrhosis: natural history and prognostic factors. Hepatology 1987;7:122–128.
Lucena MI, Andrade RJ, Tognoni G et al. Multicenter hospital study on prescribing patterns for prophylaxis and treatment of complications of cirrhosis. Eur J Clin Pharmacol 2002;58:435–440.
Planas R, Montoliu S, Balleste B et al. Natural history of patients hospitalized for management of cirrhotic ascites. Clin Gastroenterol Hepatol 2006;4:1385–1394.
Evans LT, Kim WR, Poterucha JJ, Kamath PS. Spontaneous bacterial peritonitis in asymptomatic outpatients with cirrhotic ascites. Hepatology 2003;37:897–901.
Nousbaum JB, Cadranel JF, Nahon P et al. Diagnostic accuracy of the Multistix 8 SG reagent strip in diagnosis of spontaneous bacterial peritonitis. Hepatology 2007;45:1275–1281.
Giovambattista, Simonetti RG, Craxí A et al. Spontaneous Bacterial Peritonitis: A Prospective Investigation in Predominantly Nonalcoholic Cirrhotic Patients. Hepatology 2007;3:545–549.
Runyon BA, Aasld. Introduction to the revised American Association for the Study of Liver Diseases Practice Guideline management of adult patients with ascites due to cirrhosis. Hepatology 2013;57:1651–1653.
Orman ES, Hayashi PH, Bataller R, Barritt AS. Paracentesis Is Associated With Reduced Mortality in Patients Hospitalized With Cirrhosis and Ascites. Clinical Gastroenterology and Hepatology 2014;12:496-503.e1.
Kanwal F, Kramer JR, Buchanan P et al. The quality of care provided to patients with cirrhosis and ascites in the Department of Veterans Affairs. Gastroenterology 2012;143:70–77.
Caldwell SH, Hoffman M, Lisman T et al. Coagulation disorders and hemostasis in liver disease: Pathophysiology and critical assessment of current management. Hepatology 2006;44:1039–1046.
Kumar M, Ahmad J, Maiwall R et al. Thromboelastography-Guided Blood Component Use in Patients With Cirrhosis With Nonvariceal Bleeding: A Randomized Controlled Trial. Hepatology 2020;71:235–246.
Zanetto A, Rinder HM, Senzolo M, Simioni P, Garcia-Tsao G. Reduced Clot Stability by Thromboelastography as a Potential Indicator of Procedure-Related Bleeding in Decompensated Cirrhosis. Hepatology Communications 2021;5:272–282.
Lee WM, Stravitz RT, Larson AM. Introduction to the revised American Association for the Study of Liver Diseases Position Paper on acute liver failure 2011. Hepatology 2012;55:965–967.
O’Leary JG, Greenberg CS, Patton HM, Caldwell SH. AGA Clinical Practice Update: Coagulation in Cirrhosis. Gastroenterology 2019;157:34-43 e1.
Barsuk JH, Cohen ER, Feinglass J, McGaghie WC, Wayne DB. Clinical outcomes after bedside and interventional radiology paracentesis procedures. Am J Med 2013;126:349–356.
Millington SJ, Koenig S. Better With Ultrasound: Paracentesis. Chest 2018;154:177–184.
Gottumukkala RV, Prabhakar AM, Hemingway J, Hughes DR, Duszak R Jr. Disparities over Time in Volume, Day of the Week, and Patient Complexity between Paracentesis and Thoracentesis Procedures Performed by Radiologists versus Those Performed by Nonradiologists. J Vasc Interv Radiol 2019;30:1769-1778 e1.
Rosenblatt R, Tafesh Z, Shen N et al. Early Paracentesis in High-Risk Hospitalized Patients: Time for a New Quality Indicator. Am J Gastroenterol 2019;114:1863–1869.
Tocia C, Dumitru A, Alexandrescu L, Popescu R, Dumitru E. Timing of paracentesis and outcomes in hospitalized patients with decompensated cirrhosis. World Journal of Hepatology 2020;12:1267–1275.
Kim JJ, Tsukamoto MM, Mathur AK et al. Delayed paracentesis is associated with increased in-hospital mortality in patients with spontaneous bacterial peritonitis. Am J Gastroenterol 2014;109:1436–1442.
Gaetano JN, Micic D, Aronsohn A et al. The benefit of paracentesis on hospitalized adults with cirrhosis and ascites. Journal of Gastroenterology and Hepatology 2016;31:1025–1030.
Glasheen WP, Cordier T, Gumpina R et al. Charlson Comorbidity Index: ICD-9 Update and ICD-10 Translation. Am Health Drug Benefits 2019;12:188–197.
Kim WR, Biggins SW, Kremers WK et al. Hyponatremia and mortality among patients on the liver-transplant waiting list. N Engl J Med 2008;359:1018–1026.
Morales BP, Planas R, Bartoli R et al. Early hospital readmission in decompensated cirrhosis: Incidence, impact on mortality, and predictive factors. Dig Liver Dis 2017;49:903–909.
Gaspar R, Rodrigues S, Silva M et al. Predictive models of mortality and hospital readmission of patients with decompensated liver cirrhosis. Dig Liver Dis 2019;51:1423–1429.
Scaglione SJ, Metcalfe L, Kliethermes S et al. Early Hospital Readmissions and Mortality in Patients With Decompensated Cirrhosis Enrolled in a Large National Health Insurance Administrative Database. J Clin Gastroenterol 2017;51:839–844.
Abdu B, Akolkar S, Picking C, Boura J, Piper M. Factors Associated with Delayed Paracentesis in Patients with Spontaneous Bacterial Peritonitis. Dig Dis Sci 2021;66:4035–4045.
Le S, Spelman T, Chong CP et al. Could Adherence to Quality of Care Indicators for Hospitalized Patients With Cirrhosis-Related Ascites Improve Clinical Outcomes? Am J Gastroenterol 2016;111:87–92.
Funding
This publication was made possible by the Kozmetsky Family Foundation in health services research fellowship with funding of Cristal Brown’s effort.
Author information
Authors and Affiliations
Contributions
LF, CB: Conceptualization, LF, CB, MP, NA: Methodology, CB, NA, PC, PJ, MgO: Formal analysis and investigation, CB: Writing—original draft preparation, CB, NA, MP, LF: Writing—review and editing, MP, LF: Supervision. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
There are no conflicts of interests for any of the authors.
Ethical approval
This study was IRB approved by the University of Texas at Austin with additional approval from Ascension Seton Research Enterprise.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Brown, C., Aksan, N., Chang, P. et al. Delayed Diagnostic Paracentesis Is Associated with Increased Preventable Healthcare Utilization in Disadvantaged Patient Populations with Advanced Liver Disease and Elevated INR. Dig Dis Sci 68, 2954–2962 (2023). https://doi.org/10.1007/s10620-023-07937-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-023-07937-x