Abstract
Introduction
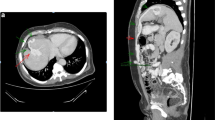
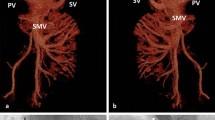
Encephalopathy secondary to hyperammonemia due to Congenital Extra-hepatic Porto-systemic shunt (CEPS) in the absence of liver cirrhosis is an exceptionally unusual condition. We describe the case of a 54-year-old woman admitted to the Emergency Department complaining of recurrent episodes of confusion and worsening cognitive impairment. At admission, the patient displayed slowing cognitive-motor skills with marked static ataxia and impaired gait. Hyperammonemia was detected in the serum. An abdominal computed tomography (CT) excluded portal hypertension and liver cirrhosis, detecting a congenital extra-hepatic porto-systemic shunt which is a highly unusual vascular malformation. The patient was treated by interventional radiologists with a successful endovascular closure.
Areas Covered
We have performed a review of the last three decades of the literature, starting from the introduction of CT scanning in common clinical practice. Eighteen studies (case reports) described 29 patients with encephalopathy secondary to hyperammonemia due to CEPS in the absence of liver cirrhosis: They underwent treatment similar to our case report of CEPS.
Expert Commentary
Encephalopathy secondary to hyperammonemia in the absence of hepatic dysfunction is an important diagnostic dilemma to many clinicians. An interventional radiologic approach is currently preferred.


Similar content being viewed by others
Availability of data and materials
Not applicable.
Abbreviations
- CEPS:
-
Congenital extra-hepatic porto-systemic shunt
- CT:
-
Computed tomography
- HE:
-
Hepatic encephalopathy
- PSS:
-
Porto-systemic shunt
References
Montagnese S, Russo FP, Amodio P, et al. Hepatic encephalopathy 2018: a clinical practice guideline by the Italian Association for the Study of the Liver (AISF). Dig Liver Dis. 2019;51:190–205.
Philips CA, Arora A, Shetty R, et al. A comprehensive review of portosystemic collaterals in cirrhosis: historical aspects, anatomy, and classifications. Int J Hepatol. 2016;6:170–243.
Philips CA, Rajesh S, Augustine P, et al. Portosystemic shunts and refractory hepatic encephalopathy: patient selection and current options. Hepat Med. 2019;11:23–34.
Aldridge DR, Tranah EJ, Shawcross DL. Pathogenesis of hepatic encephalopathy: role of ammonia and systemic inflammation. J Clin Exp Hepatol. 2015;5:S7–S20.
Ellul MA, Gholkar SA, Cross TJ. Hepatic encephalopathy due to liver cirrhosis. BMJ. 2015;351:h4187.
Nencki M, Pavlov J, Zaleski J. Ueber den ammoniakgehalt des blutes under der organe und die harnstoffbildug bei den saugethieren. Arch Exp Pathol Pharmakol. 1896;37:26–51. (in German).
Prakash R, Mullen KD. Mechanisms, diagnosis and management of hepatic encephalopathy. Nat Rev Gastroenterol Hepatol. 2010;7:515–525.
Ferenci P, Lockwood A, Mullen K, et al. Hepatic encephalopathy–definition, nomenclature, diagnosis, and quantification: final report of the working party at the 11th World Congresses of Gastroenterology, Vienna, 1998. Hepatology. 2002;35:716–721.
Cichoż-Lach H, Michalak A. Current pathogenetic aspects of hepatic encephalopathy and noncirrhotic hyperammonemic encephalopathy. World J Gastroenterol. 2013;19:26–34.
Häberle J. Clinical practice: the management of hyperammonemia. Eur J Pediatr. 2011;170:21–34.
Walker V. Severe hyperammonaemia in adults not explained by liver disease. Ann Clin Biochem. 2012;49:214–228.
Odigwe CC, Khatiwada B, Holbrook C, et al. Noncirrhotic hyperammonemia causing relapsing altered mental status. Proc Bayl Univ Med Cent. 2015;28:472–474.
Salcedo JD, Goldstein JS, Quinonez JM, et al. Nonfatal hyperammonemic encephalopathy as a late complication of Roux-en-y gastric bypass. Case Rep Gastrointest Med. 2019;2019:9031087.
Hajime T, Yoko T, Miyo T, et al. A rare congenital extrahepatic portosystemic shunt affecting the inferior mesenteric vein, inferior vena cava, and left ovarian vein. Surg Radiol Anat. 2014;36:729–732.
Howard ER, Davenport M. Congenital extrahepatic portocaval shunts—the Abernethy malformation. J Pediatr Surg. 1997;32:494–497.
Papamichail M, Pizanias M, Heaton N. Congenital portosystemic venous shunt. Eur J Pediatr. 2018;177:285–294.
Alonso-Gamarra E, Parrón M, Pérez A, et al. Clinical and radiologic manifestations of congenital extrahepatic portosystemic shunts: a comprehensive review. Radiographics. 2011;31:707–722.
Morgan G, Superina R. Congenital absence of the portal vein: two cases and proposed classification system for portasystemic vascular anomalies. J Pediatr Surg. 1994;29:1239–1241.
Lautz TB, Tantemsapya N, Rowell E, et al. Management and classification of type II congenital portosystemic shunts. J Pediatr Surg. 2011;46:308–314.
Ito S, Miyaji H, Azuma T, et al. Hyperammonaemia and Helicobacter pylori. Lancet. 1995;346:124–125.
Ohwada S, Hamada Y, Morishita Y, et al. Hepatic encephalopathy due to congenital splenorenal shunts: report of a case. Surg Today. 1994;24:145–149.
Watanabe A. Encefalopatia portale-sistemica in pazienti non cirrotici: classificazione dei tipi clinici, diagnosi e trattamento. J Gastroenterol Hepatol. 2000;15:969–979. (in Italian).
Kiriyama M, Takashima S, Sahara H, et al. Case report: portal-systemic encephalopathy due to a congenital extrahepatic portosystemic shunt. J Gastroenterol Hepatol. 1996;11:626–629.
Kuramitsu T, Komatsu M, Matsudaira N, et al. Portal-systemic encephalopathy from a spontaneous gastrorenal shunt diagnosed by three-dimensional computed tomography and treated effectively by percutaneous vascular embolization. Liver. 1998;18:208–212.
Akahoshi T, Nishizaki T, Wakasugi K, et al. Portal-systemic encephalopathy due to a congenital extrahepatic portosystemic shunt: three cases and literature review. Hepatogastroenterology. 2000;47:1113–1116.
Ishii Y, Inagaki Y, Hirai K, et al. Hepatic encephalopathy caused by congenital extrahepatic portosystemic venous shunt. J Hepatobiliary Pancreat Surg. 2000;7:524–528.
Otake M, Kobayashi Y, Hashimoto D, et al. An inferior mesenteric-caval shunt via the internal iliac vein with portosystemic encephalopathy. Intern Med. 2001;40:887–890.
Tanaka O, Ishihara K, Oyamada H, et al. Successful portal-systemic shunt occlusion with balloon-occluded retrograde transvenous obliteration for portosystemic encephalopathy without liver cirrhosis. J Vasc Interv Radiol. 2006;17:1951–1955.
Ali S, Stolpen AH, Schmidt WN. Portosystemic encephalopathy due to mesoiliac shunt in a patient without cirrhosis. J Clin Gastroenterol. 2010;44:381–383.
He C, Qi X, Guo W, et al. Education and imaging. Hepatobiliary and pancreatic: inferior mesenteric vein-left gonadal vein shunt aggravating hepatic encephalopathy. J Gastroenterol Hepatol. 2012;27:1645.
Rogal SS, Hu A, Bandi R, et al. Novel therapy for non-cirrhotic hyperammonemia due to a spontaneous splenorenal shunt. World J Gastroenterol. 2014;20:8288–8291.
González-Partida I, Hernández Conde M, Llop Herrera E, et al. Extrahepatic shunt. Unusual cause of hepatic encephalopathy. Rev Esp Enferm Dig. 2015;107:518–519.
Asakura T, Ito N, Sohma T, et al. Portosystemic encephalopathy without liver cirrhosis masquerading as depression. Intern Med. 2015;54:1619–1622.
Elnekave E, Belenky E, Van der Veer L. Noncirrhotic extrahepatic portosystemic shunt causing adult-onset encephalopathy treated with endovascular closure. Rep Radiol. 2015;2015:853.
Srinivasa RN, Sutphin PD, Anderson ME, et al. Spontaneous portosystemic shunts in noncirrhotic patients presenting with encephalopathy. Indian J Gastroenterol. 2015;34:256–260.
Brader RA, Kim KR. Transhepatic embolization of a congenital intrahepatic portosystemic shunt for the treatment of hepatic encephalopathy in a noncirrhotic patient using Amplatzer vascular plug device. Radiol Case Rep. 2017;12:318–322.
de Martinis L, Groppelli G, Corti R, et al. Disabling portosystemic encephalopathy in a non-cirrhotic patient: successful endovascular treatment of a giant inferior mesenteric-caval shunt via the left internal iliac vein. World J Gastroenterol. 2017;23:8426–8431.
Degos B, Daelman L, Huberfeld G, et al. Portosystemic shunts: an underdiagnosed but treatable cause of neurological and psychiatric disorders. J Neurol Sci. 2012;321:58–64.
Lux D, Naito A, Harikrishnan S. Congenital extrahepatic portosystemic shunt with progressive myelopathy and encephalopathy. Pract Neurol. 2019;19:368–371.
Ikeda S, Sera Y, Ohshiro H, et al. Surgical indications for patients with hyperammonemia. J Pediatr Surg. 1999;34:1012–1015.
Chiu SN, Chien YH, Wu MH, et al. Transcatheter closure of portal-systemic shunt combining congenital double extrahepatic inferior vena cava with vascular plug. J Pediatr. 2008;153:723.
Acknowledgments
The authors are the only ones responsible for the content and writing of the paper.
Funding
No funding was obtained for this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed equally to the manuscript drafting. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval and consent to participate
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Allegritti, M., Enrico, B., Basile, E. et al. Non-cirrhotic Extra-Hepatic Porto-Systemic Shunt Causing Adult-Onset Encephalopathy Treated with Endovascular Closure. Dig Dis Sci 65, 946–951 (2020). https://doi.org/10.1007/s10620-019-06024-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-019-06024-4