Abstract
Background
Early readmissions in acute pancreatitis (AP) are common. The impact of opiate prescriptions on readmissions is unknown.
Aims
To determine whether the prescription of opiates at hospital discharge and the dose prescribed are associated with early readmissions in AP.
Methods
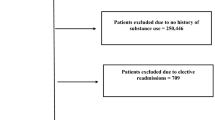
Direct admissions from the Emergency Department (ED) for AP from September 1, 2013, to August 31, 2016 were identified. Opiate prescription was defined as a new prescription at discharge in an opiate-naïve patient. Early readmission was ED visit or hospitalization within 30 days for an AP-related reason. Multivariable logistic regression was performed, adjusted for age, Charlson Comorbidity Index, pancreatic necrosis, baseline opiate use, non-opiate analgesics, and pain score at discharge.
Results
A total of 318 AP patients were identified; the overall early readmission rate was 18%. One hundred and twenty-one (38%) were prescribed opiates at discharge, and 22% had an early readmission. One hundred and ninety-seven (62%) were not prescribed opiates, and 16% had an early readmission. Median opiate dose was 48 mg (24-h morphine equivalents). On multivariable analysis, neither the prescription of opiates (OR 1.2, 95% CI 0.6–2.4, p = 0.55) nor the dose of opiates (OR 0.99, 95% CI 0.99–1.00, p = 0.39) was associated with early readmission. In subset analysis of patients discharged with an opiate prescription, those on opiates at baseline were significantly more likely to have an early readmission (OR 4.19, 95% CI 1.04–16.94, p = 0.04).
Conclusions
In AP patients, neither prescription of opiates at discharge nor prescribed dose was associated with early readmission. Patients on opiates at baseline discharged with an opiate prescription were more likely to have an early readmission.
Similar content being viewed by others
References
Peery AF, Crockett SD, Barritt AS, et al. Burden of gastrointestinal, liver, and pancreatic diseases in the United States. Gastroenterology. 2015;149:1731–1741.
Lee PJ, Bhatt A, Lopez R, Stevens T. Thirty-day readmission predicts 1-year mortality in acute pancreatitis. Pancreas. 2016;45:561–564.
Whitlock TL, Repas K, Tignor A, et al. Early readmission in acute pancreatitis: incidence and risk factors. Am J Gastroenterol. 2010;105:2492–2497.
Jencks SF, Williams MV, Coleman EA. Rehospitalizations among patients in the Medicare fee-for-service program. N Engl J Med. 2009;360:1418–1428.
Kind AJ, Smith MA, Pandhi N, Frytak JR, Finch MD. Bouncing-back: rehospitalization in patients with complicated transitions in the first thirty days after hospital discharge for acute stroke. Home Health Care Serv Q. 2007;26:37–55.
Weissman JS, Ayanian JZ, Chasan-Taber S, Sherwood MJ, Roth C, Epstein AM. Hospital readmissions and quality of care. Med Care. 1999;37:490–501.
Banks PA, Freeman ML. Practice Parameters Committee of the American College of, G. Practice guidelines in acute pancreatitis. Am J Gastroenterol. 2006;101:2379–2400.
Tenner S, Baillie J, DeWitt J, Vege SS. American College of, G. American College of Gastroenterology guideline: management of acute pancreatitis. Am J Gastroenterol. 2013;108:1400–1415.
Vipperla K, et al. Risk of and factors associated with readmission after a sentinel attack of acute pancreatitis. Clin Gastroenterol Hepatol. 2014;12:1911–1919.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
None.
Research involving human participants and/or animals
This article does not contain any studies with human participants or animals performed by any of the authors. For this type of study, formal consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yang, A.L., Jin, D.X., Rudder, M. et al. Opiate Prescriptions at Discharge Are Not Associated with Early Readmissions in Acute Pancreatitis. Dig Dis Sci 65, 611–614 (2020). https://doi.org/10.1007/s10620-019-05799-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-019-05799-w