Abstract
Background
The role of portal vein thrombosis (PVT) in the natural history of cirrhosis is controversial.
Aims
We analyzed the safety and effect of anticoagulant therapy (AT) on PVT recanalization and orthotopic liver transplant (OLT)-free survival.
Methods
Eighty consecutive patients from a prospective registry of cirrhosis and non-tumoral PVT at a tertiary center were analyzed. AT effect on PVT recanalization and OLT-free survival was determined by time-dependent Cox regression analysis.
Results
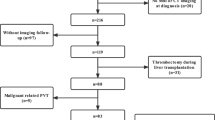
Average MELD score was 15 ± 7. Portal hypertension-related complications at PVT diagnosis were present in 65 (81.3%) patients. Isolated portal vein trunk/branch thrombosis was present in 53 (66.3%) patients. AT was started in 37 patients. AT was stopped in 17 (45.9%) patients, in 4 (10.8%) due to bleeding events. No variceal bleeding occurred while on AT. Anticoagulation was restarted in 6/17 (35.2%) patients due to rethrombosis. In 67 patients with adequate follow-up imaging, AT significantly increased the rate of PVT recanalization compared with those who did not receive anticoagulation [51.4% (18/35) vs 6/32 (18.8%), p = 0.005]. OLT-free survival after a median follow-up of 25 (1–146) months was 32 (40%). Although there was no significant effect of AT on overall OLT-free survival, OLT-free survival was higher among patients with MELD ≥ 15 receiving AT compared to those who did not (p = 0.011). Baseline MELD at PVT detection independently predicted PVT recanalization (HR 1.11, 95% CI 1.01–1.21, p = 0.027) and mortality/OLT (HR 1.12, 95% CI 1.05–1.19, p < 0.001).
Conclusions
Although AT did not improve overall OLT-free survival, it was associated with higher survival in advanced cirrhosis. Anticoagulation increased PVT recanalization and should be maintained after PVT recanalization to avoid rethrombosis.






Similar content being viewed by others
Abbreviations
- PVT:
-
Portal vein thrombosis
- US:
-
Ultrasound
- OLT:
-
Orthotopic liver transplantation
- LMWH:
-
Low molecular weight heparin
- AT:
-
Anticoagulant therapy
- HCC:
-
Hepatocellular carcinoma
- CT:
-
Computerized tomography
- MRI:
-
Magnetic resonance imaging
- TIPS:
-
Transjugular intrahepatic portosystemic shunt
- KM:
-
Kaplan–Meier
- MELD:
-
Model for End-Stage Liver Disease
- GOV1:
-
Gastroesophageal varices type 1
- IGV:
-
Isolated gastric varices
- GOV2:
-
Gastroesophageal varices type 2
- UGIB:
-
Upper gastrointestinal bleeding
References
Tsochatzis EA, Senzolo M, Germani G, Gatt A, Burroughs AK. Systematic review: portal vein thrombosis in cirrhosis. Aliment Pharmacol Ther. 2010;31:366–374.
Francoz C, Valla D, Durand F. Portal vein thrombosis, cirrhosis, and liver transplantation. J Hepatol. 2012;57:203–212.
Nery F, Chevret S, Condat B, et al. Causes and consequences of portal vein thrombosis in 1243 patients with cirrhosis: results of a longitudinal study. Hepatology. 2015;61:660–667.
Dumortier J, Czyglik O, Poncet G, et al. Eversion thrombectomy for portal vein thrombosis during liver transplantation. Am J Transpl. 2002;2:934–938.
Lendoire J, Raffin G, Cejas N, et al. Liver transplantation in adult patients with portal vein thrombosis: risk factors, management and outcome. HPB (Oxford). 2007;9:352–356.
Francoz C, Belghiti J, Vilgrain V, et al. Splanchnic vein thrombosis in candidates for liver transplantation: usefulness of screening and anticoagulation. Gut. 2005;54:691–697.
Englesbe MJ, Kubus J, Muhammad W, et al. Portal vein thrombosis and survival in patients with cirrhosis. Liver Transpl. 2010;16:83–90.
Villa E, Cammà C, Marietta M, et al. Enoxaparin prevents portal vein thrombosis and liver decompensation in patients with advanced cirrhosis. Gastroenterology. 2012;143:1253–1260.e1-4.
La Mura V, Braham S, Tosetti G, et al. Harmful and beneficial effects of anti-coagulants in patients with cirrhosis and portal vein thrombosis. Clin Gastroenterol Hepatol. 2018;16:1146–1152.
Loffredo L, Pastori D, Farcomeni A, Violi F. Effects of anticoagulants in patients with cirrhosis and portal vein thrombosis: a systematic review and meta-analysis. Gastroenterology. 2017;45:1105–1110.
Pettinari I, Vukotic R, Stefanescu H, et al. Clinical impact and safety of anticoagulants for portal vein thrombosis in cirrhosis. Am J Gastroenterol. 2019;114:258–266.
Tublin ME, Dodd GD, Baron RL. Benign and malignant portal vein thrombosis: differentiation by CT characteristics. AJR. 1997;168:719–723.
Ageno W, Riva N, Schulman S, et al. Long-term clinical outcomes of splanchnic vein thrombosis. JAMA Intern Med. 2015;175:1474.
Ha NB, Regal RE. Anticoagulation in patients with cirrhosis: caught between a rock-liver and a hard place. Ann Pharmacother. 2016;50:402–409.
Englesbe MJ, Schaubel DE, Cai S, Guidinger MKMR. Portal vein thrombosis and liver transplant survival benefit. Liver Transpl. 2010;16:999–1005.
Amitrano L, Guardascione MA, Menchise A, et al. Safety and efficacy of anticoagulation therapy with low molecular weight heparin for portal vein thrombosis in patients with liver cirrhosis. J Clin Gastroenterol. 2010;44:448–451.
Ghabril M, Agarwal S, Lacerda M, Chalasani N, Kwo P, Joseph Tector A. Portal vein thrombosis is a risk factor for poor early outcomes after liver transplantation: analysis of risk factors and outcomes for portal vein thrombosis in waitlisted patients. Transplantation. 2016;100:126–133.
de Franchis R. Baveno VI Faculty. Expanding consensus in portal hypertension report of the Baveno VI Consensus workshop: stratifying risk and individualizing care for portal hypertension. J Hepatol. 2015;63:743–752.
EASL Clinical Practical Guidelines. Vascular diseases of the liver. J Hepatol. 2016;64:179–202.
Delgado MG, Seijo S, Yepes I, et al. Efficacy and safety of anticoagulation on patients with cirrhosis and portal vein thrombosis. Clin Gastroenterol Hepatol. 2012;10:776–783.
Ageno W, Riva N, Schulman S, et al. Antithrombotic treatment of splanchnic vein thrombosis: results of an international registry. Semin Thromb Hemost. 2014;40:99–105.
Cerini F, Gonzalez JM, Torres F, et al. Impact of anticoagulation on upper-gastrointestinal bleeding in cirrhosis. A retrospective multicenter study. Hepatology. 2015;62:575–583.
Qi X, De Stefano V, Li H, Dai J, Guo X, Fan D. Anticoagulation for the treatment of portal vein thrombosis in liver cirrhosis: a systematic review and meta-analysis of observational studies. Eur J Intern Med. 2015;26:23–29.
Kwon J, Koh Y, Jong YS, Yoon JH. Low-molecular-weight heparin treatment for portal vein thrombosis in liver cirrhosis: efficacy and the risk of hemorrhagic complications. Thromb Res. 2018;163:71–76.
Werner KT, Sando S, Carey EJ, et al. Portal vein thrombosis in patients with end stage liver disease awaiting liver transplantation: outcome of anticoagulation. Dig Dis Sci. 2013;58:1776–1780. https://doi.org/10.1007/s10620-012-2548-y.
De Gottardi A, Trebicka J, Klinger C, et al. Antithrombotic treatment with direct-acting oral anticoagulants in patients with splanchnic vein thrombosis and cirrhosis. Liver Int. 2017;37:694–699.
Chen H, Liu L, Qi X, et al. Efficacy and safety of anticoagulation on more advanced portal vein thrombosis in patients with liver cirrhosis. Eur J Gastroenterol Hepatol. 2016;28:82–89.
Maruyama H, Okugawa H, Takahashi M, Yokosuka O. De novo portal vein thrombosis in virus-related cirrhosis: predictive factors and long-term outcomes. Am J Gastroenterol. 2013;108:568–574.
Berry K, Taylor J, Liou IW, Ioannou GN. Portal vein thrombosis is not associated with increased mortality among patients with cirrhosis. Clin Gastroenterol Hepatol. 2015;13:585–593.
Karvellas CJ, Cardoso FS, Wells MM, et al. Clinical impact of portal vein thrombosis prior to liver transplantation: a retrospective cohort study. Ann Hepatol. 2017;16:236–436.
Andriulli A, Tripodi A, Angeli P, et al. Hemostatic balance in patients with liver cirrhosis: report of a consensus conference. Dig Liver Dis. 2016;48:455–467.
Anstee QM, Goldin RD, Wright M, Martinelli A, Cox R, Thursz MR. Coagulation status modulates murine hepatic fibrogenesis: implications for the development of novel therapies. J Thromb Haemost. 2008;6:1336–1343.
Anstee QM, Wright M, Goldin R, Thursz MR. Parenchymal extinction: coagulation and hepatic fibrogenesis. Clin Liver Dis. 2009;13:117–126.
Northup PG, Sundaram V, Fallon MB, et al. Hypercoagulation and thrombophilia in liver disease. J Thromb Haemost. 2008;6:2–9.
Wanless IR, Wong F, Blendis LM, Greig P, Heathcote EJ, Levy G. Hepatic and portal vein thrombosis in cirrhosis: possible role in development of parenchymal extinction and portal hypertension. Hepatology. 1995;21:1238–1247.
Acknowledgments
We would like to express our sincere thanks to Professors Dominique Valla and Juan Carlos García-Pagán for their constructive comments and expert advice in preparation of this manuscript, Dr. Teresa Rodrigues for her valuable support and advice regarding statistical analysis of this manuscript, and Drs. Filipe Calinas, Joana Saiote, and Mario Silva for their help in data collection in some patients.
Author information
Authors and Affiliations
Contributions
Carlos Noronha Ferreira, MD, was involved in study design, patient inclusion, data collection, data analysis and preparation, and critical review of the manuscript. Daniela Reis, MD, performed data collection and critical review of the manuscript. Helena Cortez-Pinto, PhD, Rui Tato Marinho, PhD, Afonso Gonçalves, MD, Sónia Palma, MD, Inês Leite, MD, Tiago Rodrigues, MD, Ana Júlia Pedro, MD, Paula Alexandrino, MD, Fátima Serejo, PhD, Margarida Sobral Dias, MD, Paula Ferreira, MD, Mariana Vasconcelos, MD, Filipe Damião, MD, Leonor Xavier Brito, MD, Cilenia Baldaia, MD, Narcisa Fatela, MD, Fernando Ramalho, PhD, José Velosa, PhD, were all involved in patient inclusion and critical review of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None of the authors have any conflicts of interest to declare related to the study.
Ethics standards
Individual formal consent was not required, and institutional ethics committee approval was obtained, and the study was conducted according to the 1964 Declaration of Helsinki, later amendments, or comparable ethics standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Noronha Ferreira, C., Reis, D., Cortez-Pinto, H. et al. Anticoagulation in Cirrhosis and Portal Vein Thrombosis Is Safe and Improves Prognosis in Advanced Cirrhosis. Dig Dis Sci 64, 2671–2683 (2019). https://doi.org/10.1007/s10620-019-05572-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-019-05572-z