Abstract
Background
An association between inlet patches and proximal esophageal adenocarcinomas is currently suspected because of numerous case reports of simultaneous occurrence of both diseases.
Aims
To analyze whether inlet patches are significantly associated with proximal esophageal adenocarcinomas in a large population.
Methods
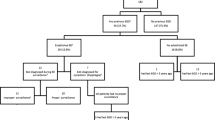
Computerized search of pathology and EGD reports revealed 398 cases of esophageal adenocarcinomas among 156,236 EGDs (performed on 106,510 patients) diagnosed by histopathology performed at Royal Oak/Troy, William Beaumont Hospitals, 2003–2016. Adenocarcinomas localized as distal, middle, or proximal; and characterized as associated versus unassociated with inlet patches. Medical records were reviewed. Endoscopic photographs, radiologic images, and pathologic slides were re-reviewed. Two researchers independently performed systematic computerized literature searches; cases of simultaneous diseases identified by consensus.
Results
Adenocarcinoma locations included: distal-381, middle-14, and proximal esophagus-3. Five patients had inlet patches with esophageal adenocarcinomas located at: distal-2, middle-0, and proximal esophagus-3 (relative frequency of inlet patches with cancers of distal/middle esophagus = 2/395 [.5%] vs. proximal esophagus = 3/3 [100%], p < .000001, 95% OR CI > 50.1, Fisher’s exact test). Cases of proximal esophageal adenocarcinomas within inlet patches included: (1) Seventy-eight-year-old man presented with dysphagia. Neck CT showed proximal esophageal mass. EGD revealed semi-circumferential, multinodular, 3.0 × 1.5 cm mass within inlet patch. Histopathology of biopsies revealed moderately-to-poorly differentiated adenocarcinoma. Patient received chemoradiotherapy and expired 2 years later. (2) Seventy-nine-year-old man presented with anorexia and weight loss. EGD demonstrated proximal esophageal mass within inlet patch. Histopathology of biopsies revealed poorly differentiated, signet ring cell adenocarcinoma. Chest CT revealed 3.4 × 2.1-cm-proximal esophageal mass. Patient expired 4 months later. (3) Sixty-year-old man presented with dysphagia. EGD revealed 4-cm-long, semi-circumferential, proximal esophageal mass within inlet patch. Histopathology of biopsies revealed poorly differentiated adenocarcinoma. Patient underwent emergency esophagectomy for esophageal perforation 2 weeks after initiating chemoradiotherapy, and died shortly thereafter. Literature review revealed 39 cases of simultaneous disease.
Study Limitations
Potential underreporting by endoscopists of inlet patches at EGD.
Conclusions
Study supplements 39 previously reported cases of simultaneous disease, by adding three new cases, and by novel report of statistically significant association between these two entities, which has important implications in the pathophysiology of proximal esophageal adenocarcinoma.



Similar content being viewed by others
References
Enzinger PC, Mayer RJ. Esophageal cancer. N Engl J Med. 2003;349:2241–2252.
von Rahden BH, Stein HJ, Becker K, Liebermann-Meffert D, Siewert JR. Heterotopic gastric mucosa of the esophagus: literature-review and proposal of a clinicopathologic classification. Am J Gastroenterol. 2004;99:543–551.
SEER cancer statistics factsheets: esophageal cancer. National Cancer Institute. Bethesda, MD. http://seer.cancer.gov/statfacts/html/esoph.html.
Zhang Y. Epidemiology of esophageal cancer. World J Gastroenterol. 2013;19:5598–5606. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3769895/.
Abe T, Hosokawa M, Kusumi T, et al. Adenocarcinoma arising from ectopic gastric mucosa in the cervical esophagus. Am J Clin Oncol. 2004;27:644–645.
Dawson JL. Adenocarcinoma of the middle oesophagus arising in an oesophagus lined by gastric (parietal) epithelium. Br J Surg. 1964;51:940–942.
Kadota T, Fujii S, Oono Y, Imajoh M, Yano T, Kaneko K. Adenocarcinoma arising from heterotopic gastric mucosa in the cervical esophagus and upper thoracic esophagus: two case reports and literature review. Expert Rev Gastroenterol Hepatol. 2016;10:405–414. https://doi.org/10.1586/17474124.2016.1125780.
Ajmal S, Young JS, Ng T. Adenocarcinoma arising from cervical esophageal gastric inlet patch. J Thorac Cardiovasc Surg. 2015;149:1664–1665. https://doi.org/10.1016/j.jtcvs.2015.03.050.
Cartabuke RH, Thota PN. High-grade dysplasia in thoracic inlet patch treated by focal endoscopic mucosal resection and radiofrequency ablation. Gastrointest Endosc. 2015;81:1297–1298. https://doi.org/10.1016/j.gie.2014.12.004.
Nomura K, Iizuka T, Inoshita N, et al. Adenocarcinoma of the cervical esophagus arising from ectopic gastric mucosa: report of two cases and review of the literature. Clin J Gastroenterol. 2015;8:367–376.
Probst A, Schaller T, Messmann H. Adenocarcinoma arising from ectopic gastric mucosa in an esophageal inlet patch: treatment by endoscopic submucosal dissection. Endoscopy. 2015;47:1. https://doi.org/10.1055/s-0034-1392423.
Hudspeth VR, Smith DS, Pacicco T, Lewis JJ. Successful endoscopic resection of adenocarcinoma arising in an esophageal inlet patch. Dis Esophagus. 2014. https://doi.org/10.1111/dote.12249.
Möschler O, Vieth M, Müller MK. Endoscopic resection of an adenocarcinoma occurring in ectopic gastric mucosa within the proximal esophagus. Endoscopy. 2014;46:E24–E25. https://doi.org/10.1055/s-0033-1358807.
Tanaka M, Ushiku T, Ikemura M, Shibahara J, Seto Y, Fukavama M. Esophageal adenocarcinoma arising in cervical inlet patch with synchronous Barrett’s esophagus-related dysplasia. Pathol Int. 2014;64:397–401. https://doi.org/10.1111/pin.12181.
Yasar B, Tarcin O, Benek D, Goksel S. Intramucosal adenocarcinoma arising from ectopic gastric mucosa in the upper esophagus treated successfully with endoscopic mucosal resection. J Gastrointest Cancer. 2014;45:201–204. https://doi.org/10.1007/s12029-014-9628-5.
Kitajima T, Kaida S, Lee S, et al. Mixed adeno(neuro)endocrine carcinoma arising from the ectopic gastric mucosa of the upper thoracic esophagus. World J Surg Oncol. 2013;11:218. https://doi.org/10.1186/1477-7819-11-218.
Nonaka K, Watanabe M, Yuruki H, et al. Narrow band imaging of adenocarcinoma arising from ectopic gastric mucosa in the upper esophagus. Endoscopy. 2013;45:E112–E113. https://doi.org/10.1055/s-0032-1325865.
Verma YP, Chauhan AK, Sen R. Primary adenocarcinoma of the upper oesophagus. Ecancermedicalscience. 2013;7:314. https://doi.org/10.3332/ecancer.2013.314.
Akanuma N, Hoshino I, Akutsu Y, et al. Primary esophageal adenocarcinoma arising from heterotopic gastric mucosa: report of a case. Surg Today. 2013;43:446–451. https://doi.org/10.1007/s00595-012-0206-9.
Fashoyin A, Hartig G, Schelman WR, et al. Aggressive adenocarcinoma of the cervical esophagus: importance of a multidisciplinary approach. Case Rep Gastrointest Med. 2012;2012:826246. https://doi.org/10.1155/2012/826246.
Komoro S, Osada S, Tanaka Y, et al. A case of esophageal adenocarcinoma arising from the ectopic gastric mucosa in the thoracic esophagus. Rare Tumors. 2010;2:e5. https://doi.org/10.4081/rt.2010.e5.
Yoshida T, Shimizu Y, Kato M. Image of the month. Use of magnifying endoscopy to identify early esophageal adenocarcinoma in ectopic gastric mucosa of the cervical esophagus. Clin Gastroenterol Hepatol. 2010. https://doi.org/10.1016/j.cgh.2010.02.025.
Alagozlu H, Ergun M, Cindoruk M, et al. The rare presentations of a large polyp and an esophageal carcinoma in heterotropic gastric mucosa: a case series. J Med Case Rep. 2007;1:127.
Alrawi SJ, Winston J, Tan D, et al. Primary adenocarcinoma of cervical esophagus. J Exp Clin Cancer Res. 2004;24:325–330.
von Rahden BH, Stein HJ, Becker K, Siewert RJ. Esophageal adenocarcinomas in heterotopic gastric mucosa: review and report of a case with complete response to neoadjuvant radiochemotherapy. Dig Surg. 2005;22:107–112.
Hirayama N, Arima M, Miyazaki S, et al. Endoscopic mucosal resection of adenocarcinoma arising in ectopic gastric mucosa in the cervical esophagus: case report. Gastrointest Endosc. 2003;57:263–266.
Chatelain D, de Lajarte-Thirouard AS, Tiret E, Flejou JF. Adenocarcinoma of the upper esophagus arising in heterotopic gastric mucosa: common pathogenesis with Barrett’s adenocarcinoma? Virchows Arch. 2002;441:406–411.
Klaase JM, Lemaire LC, Rauws EA, Offerhaus GJ, van Lanschot JJ. Heterotopic gastric mucosa of the cervical esophagus: a case of high-grade dysplasia treated with argon plasma coagulation and a case of adenocarcinoma. Gastrointest Endosc. 2001;53:101–104.
Pech O, May A, Gossner L, et al. Early stage adenocarcinoma of the esophagus arising in the circular heterotopic gastric mucosa treated by endoscopic mucosal resection. Gastrointest Endosc. 2001;54:656–658.
Noguchi T, Takeno S, Takahashi Y, Sato T, Uchida Y, Yokoyama S. Primary adenocarcinoma of the cervical esophagus arising from heterotopic gastric mucosa. J Gastroenterol. 2001;26:704–709.
Lauwers GY, Scott GV, Vauthey JN. Adenocarcinoma of the upper esophagus arising in cervical ectopic gastric mucosa: rare evidence of malignant potential of so-called “inlet patch”. Dig Dis Sci. 1998;43:901–907.
Berkelhammer C, Bhagavan M, Templeton A, Raines R, Walloch J. Gastric inlet patch containing submucosally infiltrating adenocarcinoma. J Clin Gastroenterol. 1997;25:678–681.
Pai S, Deshpande R, Naresh KN. Adenocarcinoma of cervical esophagus arising in aberrant gastric mucosa. Indian J Gastroenterol. 1997;16:157–158.
Sperling RM, Grendell JH. Adenocarcinoma arising in an inlet patch of the esophagus. Am J Gastroenterol. 1995;90:150–152.
Takagi A, Ema Y, Horii S, Morishita M, Miyaishi O, Kino I. Early adenocarcinoma arising from ectopic gastric mucosa in the cervical esophagus. Gastrointest Endosc. 1995;41:167–170.
Ishii K, Ota H, Nakayama J, et al. Adenocarcinoma of the cervical oesohagus arising from ectopic gastric mucosa. The histochemical determination of its origin. Virchows Arch A Pathol Anat Histopathol. 1991;419:159–164.
Christensen WN, Sternberg SS. Adenocarcinoma of the upper esophagus arising in ectopic gastric mucosa. Two case reports and review of the literature. Am J Surg Pathol. 1987;11:397–402.
Danoff B, Cooper J, Klein M. Primary adenocarcinoma of the upper oesophagus. Clin Radiol. 1978;29:519–522.
Jernstrom P, Brewer LA 3rd. Primary adenocarcinoma of the mid-esohagus arising in ectopic gastric mucosa with associated hiatal hernia and reflux esophagitis (Dawson’s syndrome). Cancer. 1970;26:1343–1348.
Davis WM, Goodwin MN Jr., Black HC Jr., Hawk JC. Polypoid adenocarcinoma of the cervical esophagus. Arch Pathol. 1969;88:367–370.
Morson BC, Belcher JR. Adenocarcinoma of the oesophagus and ectopic gastric mucosa. Br J Cancer. 1952;6:127–130.
Carrie A. Adenocarcinoma of the upper end of the oesophagus arising from ectopic gastric epithelium. Br J Surg. 1950;37:474.
Jacobs E, Dehou MF. Heterotopic gastric mucosa in the upper esophagus: a prospective study of 33 cases and review of literature. Endoscopy. 1997;29:710–715.
Jabbari M, Goresky CA, Lough J, Yaffe C, Daly D, Côté C. The inlet patch: heterotopic gastric mucosa in the upper esophagus. Gastroenterology. 1985;89:352–356.
Weickert U, Wolf A, Schröder C, Autschbach F, Vollmer H. Frequency, histopathological findings, and clinical significance of cervical heterotopic gastric mucosa (gastric inlet patch): a prospective study in 300 patients. Dis Esophagus. 2011;24:63–68. https://doi.org/10.1111/j.1442-2050.2010.01091.x. http://onlinelibrary.wiley.com/doi/10.1111/j.1442-2050.2010.01091.x/full.
Borhan-Manesh F, Farnum JB. Incidence of heterotopic gastric mucosa in the upper oesophagus. Gut. 1991;32:968–972.
Wang GQ, Dawsey SM, Zhou MH, Lewin KJ. Gastric heterotopia in the upper esophagus (inlet patch) in endoscopic surveys in northern China. J Clin Gastroenterol. 1994;19:321–324. http://www.archivesofpathology.org/doi/pdf/10.1043%2F1543-2165(2004)128%3C444%3AIPPHTA%3E2.0.CO%3B2.
Azar C, Jamali F, Tamim H, Abdul-Baki H, Soweid A. Prevalence of endoscopically identified heterotopic gastric mucosa in the proximal esophagus: endoscopist dependent? J Clin Gastroenterol. 2007;41:468–471.
Avidan B, Sonnenberg A, Chejfec G, Schnell TG, Sontag SJ. Is there a link between cervical inlet patch and Barrett’s esophagus? Gastrointest Endosc. 2001;53:717–721. https://doi.org/10.1067/mge.2001.114782.
Neumann WL, Luján GM, Genta RM. Gastric heterotopia in the proximal oesophagus (“inlet patch”): Association with adenocarcinomas arising in Barrett mucosa. Dig Liver Dis. 2012;44:292–296. https://doi.org/10.1016/j.dld.2011.11.008.
Rosztóczy A, Izbéki F, Németh IB, et al. Detailed esophageal function and morphological analysis shows high prevalence of gastroesophageal reflux disease and Barrett’s esophagus in patients with cervical inlet patch. Dis Esophagus. 2012;25:498–504. https://doi.org/10.1111/j.1442-2050.2011.01281.x.
Yüksel I, Usküdar O, Köklü S, et al. Inlet patch: associations with endoscopic findings in the upper gastrointestinal system. Scand J Gastroenterol. 2008;43:910–914.
Weickert U, Wolf A, Schröder C, Autschbach F, Vollmer H. Frequency, histopathological findings, and clinical significance of cervical heterotopic gastric mucosa (gastric inlet patch): a prospective study in 300 patients. Dis Esophagus. 2011;24:63–68. https://doi.org/10.1111/j.1442-2050.2010.01091.x.
Jacobs E, Dehou MF. Heterotopic gastric mucosa in the upper esophagus: a prospective study of 33 cases and review of literature. Endoscopy. 1997;29:710–715. https://doi.org/10.1055/s-2007-1004294.
Peitz U, Vieth M, Evert M, Arand J, Roessner A, Malfertheiner P. The prevalence of gastric heterotopia of the proximal esophagus is underestimated, but preneoplasia is rare—correlation with Barrett’s esophagus. BMC Gastroenterol. 2017;17:87. https://doi.org/10.1186/s12876-017-0644-3.
Author information
Authors and Affiliations
Contributions
MO performed the chart reviews of the patients, wrote the three case reports, performed the literature review, and wrote preliminary versions of the three tables. MA performed the entire pathology review, including retrospectively re-reviewing all the pathology slides. MC conceived the project, wrote the introduction and discussion, edited the case reports and tables, and acted as a mentor for MO who is a medical resident.
Corresponding author
Ethics declarations
Conflict of interest
None for all authors. This paper does not discuss any confidential pharmaceutical industry data reviewed by Dr. Cappell as a consultant for the United States Food and Drug Administration (FDA) Advisory Committee on Gastrointestinal Drugs. Dr. Cappell is a member of the speaker’s bureau for AstraZeneca and Daiichi Sankyo, co-marketers of Movantik. This work does not discuss any drug manufactured or marketed by AstraZeneca or Daiichi Sankyo.
IRB approval
Initially approved by William Beaumont Hospital IRB on 6/9/2016.
Rights and permissions
About this article
Cite this article
Orosey, M., Amin, M. & Cappell, M.S. A 14-Year Study of 398 Esophageal Adenocarcinomas Diagnosed Among 156,256 EGDs Performed at Two Large Hospitals: An Inlet Patch Is Proposed as a Significant Risk Factor for Proximal Esophageal Adenocarcinoma. Dig Dis Sci 63, 452–465 (2018). https://doi.org/10.1007/s10620-017-4878-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-017-4878-2