Abstract
Introduction
Case control studies suggest an inverse association between Helicobacter pylori (H. pylori) and Crohn’s disease (CD). It is possible this could be accounted for by confounders such as antibiotic therapy. Analyzing the geographic distribution of H. pylori and the links with the incidence and prevalence of CD would be an alternative approach to circumvent these confounders.
Methods
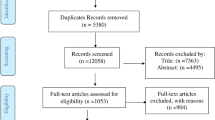
The literature was searched for studies published between 1990 and 2016 that reported incidence or prevalence data for CD in random population samples in developed countries (GDP per capita >20,000 USD/year). Corresponding prevalence studies for H. pylori in these same regions were then sought matched to the same time period (±6 years). The association between the incidence and prevalence of CD and H. pylori prevalence rates were assessed before and after adjusting for GDP and life expectancy.
Results
A total of 19 CD prevalence and 22 CD incidence studies from 10 European countries, Japan, USA, and Australia with date-matched H. pylori prevalence data were identified. The mean H. pylori prevalence rate was 43.4% (range 15.5–85%), and the mean rates for incidence and prevalence for CD were 6.9 and 91.0/100,000 respectively. The incidence (r = −0.469, p < 0.03) and prevalence (r = −0.527, p = 0.02) of CD was inversely and significantly associated with prevalence of H. pylori infection.
Conclusions
Our data demonstrate a significant inverse association between geographic distribution of H. pylori and CD. Thus, it is highly unlikely that the findings of previous case control studies were simply due to confounding factors such as concomitant antibiotic use in CD patients.



Similar content being viewed by others
References
Koloski NA, Bret L, Radford-Smith G. Hygiene hypothesis in inflammatory bowel disease: a critical review of the literature. World J Gastroenterol: WJG. 2008;14:165–173.
Amre D. Gene-environment interactions in the etiopathogenesis of inflammatory bowel disease. J Pediatr Gastroenterol Nutr. 2005;40:S39.
Uniken Venema WT, Voskuil MD, Dijkstra G, Weersma RK, Festen EA. The genetic background of inflammatory bowel disease: from correlation to causality. J Pathol. 2017;241:146–158.
Loftus CG, Loftus EV Jr., Harmsen WS, et al. Update on the incidence and prevalence of Crohn’s disease and ulcerative colitis in Olmsted County, Minnesota, 1940–2000. Inflamm Bowel Dis. 2007;13:254–261.
Prideaux L, Kamm MA, De Cruz PP, Chan FK, Ng SC. Inflammatory bowel disease in Asia: a systematic review. J Gastroenterol Hepatol. 2012;27:1266–1280.
Jostins L, Ripke S, Weersma RK, et al. Host-microbe interactions have shaped the genetic architecture of inflammatory bowel disease. Nature. 2012;491:119–124.
Amre DK, Lambrette P, Law L, et al. Investigating the hygiene hypothesis as a risk factor in pediatric onset Crohn’s disease: a case-control study. Am J Gastroenterol. 2006;101:1005–1011.
Bernstein CN, Rawsthorne P, Cheang M, Blanchard JF. A population-based case control study of potential risk factors for IBD. Am J Gastroenterol. 2006;101:993–1002.
Lashner BA, Loftus EV Jr. True or false? The hygiene hypothesis for Crohn’s disease. Am J Gastroenterol. 2006;101:1003–1004.
Kao JY, Zhang M, Miller MJ, et al. Helicobacter pylori immune escape is mediated by dendritic cell—induced Treg skewing and Th17 suppression in mice. Gastroenterology. 2010;138:1046–1054.
Sonnenberg A, Genta RM. Low prevalence of Helicobacter pylori infection among patients with inflammatory bowel disease. Aliment Pharmacol Ther. 2012;35:469–476.
Deeks JJ, Dinnes J, D’Amico R, et al. Evaluating non-randomised intervention studies. Health Technol Assess. 2003;7:iii–x. (1–173).
Levesque R. SPSS Programming and Data Management: A Guide for SPSS and SAS Users. 4th ed. Chicago, Ill: SPSS Inc.; 2007. PDF ISBN 1-56827-390-8.
Rokkas T, Gisbert JP, Niv Y, O’Morain C. The association between Helicobacter pylori infection and inflammatory bowel disease based on meta-analysis. United Eur Gastroenterol J. 2015;3:539–550.
Wu X-W, Ji H-Z, Yang M-F, Wu L, Wang F-Y. Helicobacter pylori infection and inflammatory bowel disease in Asians: a meta-analysis. World J Gastroenterol: WJG. 2015;21:4750–4756.
Castaño-Rodriguez N, Kaakoush NO, Lee WS, Mitchell HM. Dual role of Helicobacter and Campylobacter species in IBD: a systematic review and meta-analysis. Gut. 2017;66:235–249.
Luther J, Dave M, Higgins PD, Kao JY. Association between Helicobacter pylori infection and inflammatory bowel disease: a meta-analysis and systematic review of the literature. Inflamm Bowel Dis. 2010;16:1077–1084.
Gong YH, Sun LP, Jin SG, Yuan Y. Comparative study of serology and histology based detection of Helicobacter pylori infections: a large population-based study of 7,241 subjects from China. Eur J Clin Microbiol Infect Dis. 2010;29:907–911.
Guarner J, Kalach N, Elitsur Y, Koletzko S. 2010 Helicobacter pylori diagnostic tests in children: review of the literature from 1999 to 2009. Eur J Pediatr. 2010;169:15–25.
Mascie-Taylor CG, Karim E. The burden of chronic disease. Science. 2003;302:1921–1922.
Nakajima S, Nishiyama Y, Yamaoka M, Yasuoka T, Cho E. Changes in the prevalence of Helicobacter pylori infection and gastrointestinal diseases in the past 17 years. J Gastroenterol Hepatol. 2010;25:S99–S110.
Jess T, Riis L, Vind I, et al. Changes in clinical characteristics, course, and prognosis of inflammatory bowel disease during the last 5 decades: a population-based study from Copenhagen, Denmark. Inflamm Bowel Dis. 2007;13:481–489.
Sewell JL, Yee HF Jr., Inadomi JM. Hospitalizations are increasing among minority patients with Crohn’s disease and ulcerative colitis. Inflamm Bowel Dis. 2010;16:204–207.
Molodecky NA, Soon IS, Rabi DM, et al. Increasing incidence and prevalence of the inflammatory bowel diseases with time, based on systematic review. Gastroenterology. 2012;142:46e42–54e42. (quiz e30).
Gearry RB, Richardson AK, Frampton CM, Dodgshun AJ, Barclay ML. Population-based cases control study of inflammatory bowel disease risk factors. J Gastroenterol Hepatol. 2010;25:325–333.
Wilson J, Hair C, Knight R, et al. High incidence of inflammatory bowel disease in Australia: a prospective population-based Australian incidence study. Inflamm Bowel Dis. 2010;16:1550–1556.
Thia KT, Loftus EV Jr., Sandborn WJ, Yang SK. An update on the epidemiology of inflammatory bowel disease in Asia. Am J Gastroenterol. 2008;103:3167–3182.
Zheng JJ, Zhu XS, Huangfu Z, Gao ZX, Guo ZR, Wang Z. Crohn’s disease in mainland China: a systematic analysis of 50 years of research. Chin J Dig Dis. 2005;6:175–181.
Yao T, Matsui T, Hiwatashi N. Crohn’s disease in Japan: diagnostic criteria and epidemiology. Dis Colon Rectum. 2000;43:S85–S93.
Garcia Rodriguez LA, Ruigomez A, Panes J. Acute gastroenteritis is followed by an increased risk of inflammatory bowel disease. Gastroenterology. 2006;130:1588–1594.
Darfeuille-Michaud A, Boudeau J, Bulois P, et al. High prevalence of adherent-invasive Escherichia coli associated with ileal mucosa in Crohn’s disease. Gastroenterology. 2004;127:412–421.
Gradel KO, Nielsen HL, Schonheyder HC, Ejlertsen T, Kristensen B, Nielsen H. Increased short- and long-term risk of inflammatory bowel disease after salmonella or campylobacter gastroenteritis. Gastroenterology. 2009;137:495–501.
Peeters H, Bogaert S, Laukens D, et al. CARD15 variants determine a disturbed early response of monocytes to adherent-invasive Escherichia coli strain LF82 in Crohn’s disease. Int J Immunogenet. 2007;34:181–191.
Bernstein CN, Nayar G, Hamel A, Blanchard JF. Study of animal-borne infections in the mucosas of patients with inflammatory bowel disease and population-based controls. J Clin Microbiol. 2003;41:4986–4990.
Bernstein CN, Blanchard JF, Rawsthorne P, Collins MT. Population-based case control study of seroprevalence of Mycobacterium paratuberculosis in patients with Crohn’s disease and ulcerative colitis. J Clin Microbiol. 2004;42:1129–1135.
Naser SA, Ghobrial G, Romero C, Valentine JF. Culture of Mycobacterium avium subspecies paratuberculosis from the blood of patients with Crohn’s disease. Lancet. 2004;364:1039–1044.
Ryan P, Bennett MW, Aarons S, et al. PCR detection of Mycobacterium paratuberculosis in Crohn’s disease granulomas isolated by laser capture microdissection. Gut. 2002;51:665–670.
Bull TJ, McMinn EJ, Sidi-Boumedine K, et al. Detection and verification of Mycobacterium avium subsp. paratuberculosis in fresh ileocolonic mucosal biopsy specimens from individuals with and without Crohn’s disease. J Clin Microbiol. 2003;41:2915–2923.
Feller M, Huwiler K, Stephan R, et al. Mycobacterium avium subspecies paratuberculosis and Crohn’s disease: a systematic review and meta-analysis. Lancet Infect Dis. 2007;7:607–613.
Selby W, Pavli P, Crotty B, et al. Two-year combination antibiotic therapy with clarithromycin, rifabutin, and clofazimine for Crohn’s disease. Gastroenterology. 2007;132:2313–2319.
Quirke P. Antagonist. Mycobacterium avium subspecies paratuberculosis is a cause of Crohn’s disease. Gut. 2001;49:757–760.
Korzenik JR. Past and current theories of etiology of IBD: toothpaste, worms, and refrigerators. J Clin Gastroenterol. 2005;39:S59–S65.
Standaert-Vitse A, Sendid B, Joossens M, et al. Candida albicans colonization and ASCA in familial Crohn’s disease. Am J Gastroenterol. 2009;104:1745–1753.
Kalkanci A, Tuncer C, Degertekin B, et al. Detection of Candida albicans by culture, serology and PCR in clinical specimens from patients with ulcerative colitis: re-evaluation of an old hypothesis with a new perspective. Folia Microbiol. 2005;50:263–267.
McKenzie H, Main J, Pennington CR, Parratt D. Antibody to selected strains of Saccharomyces cerevisiae (baker’s and brewer’s yeast) and Candida albicans in Crohn’s disease. Gut. 1990;31:536–538.
Bernstein CN, Kraut A, Blanchard JF, Rawsthorne P, Yu N, Walld R. The relationship between inflammatory bowel disease and socioeconomic variables. Am J Gastroenterol. 2001;96:2117–2125.
Cardenas VM, Mulla ZD, Ortiz M, Graham DY. Iron deficiency and Helicobacter pylori infection in the United States. Am J Epidemiol. 2006;163:127–134.
Everhart JE, Kruszon-Moran D, Perez-Perez GI, Tralka TS, McQuillan G. Seroprevalence and ethnic differences in Helicobacter pylori infection among adults in the United States. J Infect Dis. 2000;181:1359–1363.
Lane JA, Murray LJ, Harvey IM, Donovan JL, Nair P, Harvey RF. Randomised clinical trial: Helicobacter pylori eradication is associated with a significantly increased body mass index in a placebo-controlled study. Aliment Pharmacol Ther. 2011;33:922–929.
Gunesh S, Thomas GA, Williams GT, Roberts A, Hawthorne AB. The incidence of Crohn’s disease in Cardiff over the last 75 years: an update for 1996–2005. Aliment Pharmacol Ther. 2008;27:211–219.
Martin-de-Argila C, Boixeda D, Canton R, et al. Helicobacter pylori infection in a healthy population in Spain. Eur J Gastroenterol Hepatol. 1996;8:1165–1168.
Garrido A, Martinez MJ, Ortega JA, Lobato A, Rodriguez MJ, Guerrero FJ. Epidemiology of chronic inflammatory bowel disease in the Northern area of Huelva. Rev Esp Enferm Dig. 2004;96:687–691. (91–94).
Sanchez Ceballos F, Taxonera Samso C, Garcia Alonso M, Alba Lopez C, Sainz de Los Terreros Soler L, Diaz-Rubio M. Prevalence of Helicobacter pylori infection in the healthy population of Madrid (Spain). Rev Esp Enferm Dig. 2007;99:497–501.
Lopez-Serrano P, Perez-Calle JL, Carrera-Alonso E, et al. Epidemiologic study on the current incidence of inflammatory bowel disease in Madrid. Rev Esp Enferm Dig. 2009;101:768–772.
Macenlle Garcia R, Gayoso Diz P, Sueiro Benavides RA, Fernandez Seara J. Prevalence of Helicobacter pylori infection in the general adult population of the province of Ourense. Rev Esp Enferm Dig. 2006;98:241–248.
Arin Letamendia A, Burusco Paternain MJ, Borda Celaya F, Pueyo Royo A, Martinez Echeverria A, Jimenez Perez FJ. Epidemiological aspects of inflammatory bowel disease in the Pamplona area. Rev Esp Enferm Dig. 1999;91:769–776.
Senra-Varela A, Lopez-Saez JB, Gomez-Biondi V. Prevalence of Helicobacter pylori infection in two Spanish regions with different incidence of gastric cancer. Eur J Epidemiol. 1998;14:491–494.
Monferrer Guardiola R, Martin Jimenez JA, Pedraza Sanz RG, Moreno Sanchez I, Soler Bahilo E, Hinojosa del Val J. Incidence of inflammatory bowel disease in the 02 health area of Castellon (1992–1996). Rev Esp Enferm Dig. 1999;91:33–46.
Rodrigo Saez L, Riestra Menendez S, Fernandez Rodriguez E, Fernandez Velazquez MR, Garcia Alonso S, Lauret Brana ME. Epidemiological study of the prevalence of Helicobacter pylori infection in the general population in Asturias. Spain Revista espanola de enfermedades digestivas. 1997;89:511–522.
Pozzati L, Cabanillas A. Hospital study of the incidence of inflammatory bowel disease in the health district of Merida (Spain). Gastroenterol Hepatol. 2002;25:541–544.
Nishise Y, Fukao A, Takahashi T. Risk factors for Helicobacter pylori infection among a rural population in Japan: relation to living environment and medical history. J Epidemiol. 2003;13:266–273.
Morita N, Toki S, Hirohashi T, et al. Incidence and prevalence of inflammatory bowel disease in Japan: nationwide epidemiological survey during the year 1991. J Gastroenterol. 1995;30:1–4.
Asaka M, Kato M, Kudo M, et al. Relationship between Helicobacter pylori infection, atrophic gastritis and gastric carcinoma in a Japanese population. Eur J Gastroenterol Hepatol. 1995;7:S7–S10.
De Bastiani R, Gabrielli M, Ubaldi E, et al. High prevalence of Cag-A positive H. pylori strains in ischemic stroke: a primary care multicenter study. Helicobacter. 2008;13:274–277.
Dal Pont E, Lecis P, Galliani EA, Cavallaro LG, et al. Inflammatory bowel disease (IBD) incidence and prevalence in a north eat limited area of Italy. Dig Liver Dis. 2010;42S:S61–S192.
Russo A, Eboli M, Pizzetti P, et al. Determinants of Helicobacter pylori seroprevalence among Italian blood donors. Eur J Gastroenterol Hepatol. 1999;11:867–873.
Tragnone A, Corrao G, Miglio F, Caprilli R, Lanfranchi GA. Incidence of inflammatory bowel disease in Italy: a nationwide population-based study. Gruppo Italiano per lo Studio del Colon e del Retto (GISC). Int J Epidemiol. 1996;25:1044–1052.
Iszlai E, Kiss E, Toldy E, et al. Seroprevalence of Helicobacter pylori infection and anti-CagA positivity in the county Szabolcs–Szatmar–Bereg. Orv Hetil. 2003;144:1713–1718.
Lakatos L, Mester G, Erdelyi Z, et al. [Epidemiology of inflammatory bowel diseases in Veszprem county of Western Hungary between 1977 and 2001]. Orv Hetil. 2001;144:1819–1827.
Stettin D, Waldmann A, Wolters M, Trunz B. Schauder P and Hahn A 2007 Infection with Helicobacter pylori–outcome of a cross-sectional investigation. Dtsch Med Wochenschr. 1946;132:2677–2682.
Ott C, Obermeier F, Thieler S, et al. The incidence of inflammatory bowel disease in a rural region of Southern Germany: a prospective population-based study. Eur J Gastroenterol Hepatol. 2008;20:917–923.
Holtmann G, Goebell H, Holtmann M, Talley NJ. Dyspepsia in healthy blood donors. Pattern of symptoms and association with Helicobacter pylori. Dig Dis Sci. 1994;39:1090–1098.
Timmer A, Breuer-Katschinski B, Goebell H. Time trends in the incidence and disease location of Crohn’s disease 1980–1995: a prospective analysis in an urban population in Germany. Inflamm Bowel Dis. 1999;5:79–84.
Salomaa-Rasanen A, Kosunen TU, Aromaa AR, Knekt P, Sarna S, Rautelin H. A “screen-and-treat” approach for Helicobacter pylori infection: a population-based study in Vammala, Finland. Helicobacter. 2010;15:28–37.
Manninen P, Karvonen AL, Huhtala H, Rasmussen M, Collin P. The epidemiology of inflammatory bowel diseases in Finland. Scand J Gastroenterol. 2010;45:1063–1067.
Moayyedi P, Axon AT, Feltbower R, et al. Relation of adult lifestyle and socioeconomic factors to the prevalence of Helicobacter pylori infection. Int J Epidemiol. 2002;31:624–631.
Rubin GP, Hungin AP, Kelly PJ, Ling J. Inflammatory bowel disease: epidemiology and management in an English general practice population. Aliment Pharmacol Ther. 2000;14:1553–1559.
Rosenstock S, Jorgensen T, Andersen L, Bonnevie O. Seroconversion and seroreversion in IgG antibodies to Helicobacter pylori: a serology based prospective cohort study. J Epidemiol Community Health. 2000;54:444–450.
Munkholm P, Langholz E, Nielsen OH, Kreiner S, Binder V. Incidence and prevalence of Crohn’s disease in the county of Copenhagen, 1962–87: a sixfold increase in incidence. Scand J Gastroenterol. 1992;27:609–614.
Munkholm P, Langholz E, Nielsen OH, Kreiner S, Binder V. Increased incidence of Crohn disease in the county of Copenhagen. Ugeskr Laeger. 1993;155:3199–3202.
Babus V, Presecki V, Katicic M, et al. Distribution of Helicobacter pylori infection in the adult population of Croatia. Lijec Vjesn. 1997;119:139–142.
Sincic BM, Vucelic B, Persic M, et al. Incidence of inflammatory bowel disease in Primorsko-goranska County, Croatia, 2000–2004: a prospective population-based study. Scand J Gastroenterol. 2006;41:437–444.
Naja F, Kreiger N, Sullivan T. Helicobacter pylori infection in Ontario: prevalence and risk factors. Can J Gastroenterol. 2007;21:501–506.
Lowe AM, Roy PO, Poulin MB, et al. Epidemiology of Crohn’s disease in Quebec, Canada. Inflamm Bowel Dis. 2009;15:429–435.
Veldhuyzen van Zanten SJ, Pollak PT, Best LM, Bezanson GS, Marrie T. Increasing prevalence of Helicobacter pylori infection with age: continuous risk of infection in adults rather than cohort effect. J Infect Dis. 1994;169:434–437.
Green C, Elliott L, Beaudoin C, Bernstein CN. A population-based ecologic study of inflammatory bowel disease: searching for etiologic clues. Am J Epidemiol. 2006;164:615–623. (discussion 24–28).
Whiteman DC, Parmar P, Fahey P, et al. Association of Helicobacter pylori infection with reduced risk for esophageal cancer is independent of environmental and genetic modifiers. Gastroenterology. 2010;139:73–83. (quiz e11–e12).
Anseline PF. Crohn’s disease in the Hunter Valley region of Australia. Aust N Z J Surg. 1995;65:564–569.
Iantorno G, Cinquetti M, Mazzocchi A, Morelli A, Bassotti G. Audit of constipation in a gastroenterology referral center. Dig Dis Sci. 2007;52:317–320.
Kappelman MD, Rifas-Shiman SL, Kleinman K, et al. The prevalence and geographic distribution of Crohn’s disease and ulcerative colitis in the United States. Clin Gastroenterol Hepatol. 2007;5:1424–1429.
Graham DY, Malaty HM, Evans DG, Evans DJ Jr., Klein PD, Adam E. Epidemiology of Helicobacter pylori in an asymptomatic population in the United States. Effect of age, race, and socioeconomic status. Gastroenterology. 1991;100:1495–1501.
Loftus EV Jr., Silverstein MD, Sandborn WJ, Tremaine WJ, Harmsen WS, Zinsmeister AR. Crohn’s disease in Olmsted County, Minnesota, 1940–1993: incidence, prevalence, and survival. Gastroenterology. 1998;114:1161–1168.
Stone MA, Mayberry JF, Baker R. Prevalence and management of inflammatory bowel disease: a cross-sectional study from central England. Eur J Gastroenterol Hepatol. 2003;15:1275–1280.
Saro Gismera C, Lacort Fernandez M, Arguelles Fernandez G, et al. Incidence and prevalence of inflammatory bowel disease in Gijon, Asturias, Spain. Gastroenterol Hepatol. 2000;23:322–327.
Saro Gismera C, Riestra Menendez S, Milla Crespo A, et al. Incidence and prevalence of inflammatory bowel disease. Asturian study in 5 areas (EIICEA), Spain. Anales de medicina interna. 2003;20:3–9.
Peleteiro B, Lopes C, Figueiredo C, Lunet N. Salt intake and gastric cancer risk according to Helicobacter pylori infection, smoking, tumour site and histological type. Br J Cancer. 2011;104:198–207.
Azevedo LF, Magro F, Portela F, et al. Estimating the prevalence of inflammatory bowel disease in Portugal using a pharmaco-epidemiological approach. Pharmacoepidemiol Drug Saf. 2010;19:499–510.
Asakura K, Nishiwaki Y, Inoue N, Hibi T, Watanabe M, Takebayashi T. Prevalence of ulcerative colitis and Crohn’s disease in Japan. J Gastroenterol. 2009;44:659–665.
Bazzoli F, Palli D, Zagari RM, et al. The Loiano-Monghidoro population-based study of Helicobacter pylori infection: prevalence by 13C-urea breath test and associated factors. Aliment Pharmacol Ther. 2001;15:1001–1007.
Trallori G, Palli D, Saieva C, et al. A population-based study of inflammatory bowel disease in Florence over 15 years (1978–92). Scand J Gastroenterol. 1996;31:892–899.
Breuer T, Sudhop T, Hoch J, Sauerbruch T, Malfertheiner P. Prevalence of and risk factors for Helicobacter pylori infection in the western part of Germany. Eur J Gastroenterol Hepatol. 1996;8:47–52.
Loffler A, Glados M. Data on the epidemiology of Crohn disease in the city of Cologne. Med Klin. 1993;88:516–519.
Dirks E, Forster S, Thom M, Quebe-Fehling E, Goebell H. Prospective study of the incidence and prevalence of ulcerative colitis in a large urban population in Germany (western Ruhr area). Z Gastroenterol. 1994;32:332–337.
Jovanovic Z. Epidemiology of Crohn’s disease in the Rijeka–Istra region. Lijec Vjesn. 1999;121:8–13.
Acknowledgments
The authors acknowledge Associate Professor Linda Fletcher for her the review of the manuscript.
Author’s contribution
GH was involved in study idea, concept and design, analysis and interpretation of data, drafting of the manuscript, and critical revision of the manuscript. AS was involved in study concept and design, data extraction and interpretation of data, drafting of the manuscript. NJT was involved in study concept and interpretation of data and drafting of the manuscript. MW, NK, and DB interpreted the data and drafted the manuscript. JMA, MM, and MM interpreted the data and revised the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Shah, A., Talley, N.J., Walker, M. et al. Is There a Link Between H. Pylori and the Epidemiology of Crohn’s Disease?. Dig Dis Sci 62, 2472–2480 (2017). https://doi.org/10.1007/s10620-017-4496-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-017-4496-z