Abstract
Background
Accurate inflammation reporting in capsule endoscopy (CE) is important for diagnosis and monitoring of treatment of inflammatory bowel disease (IBD). Fecal calprotectin (FC) is a highly specific biomarker of gut inflammation. Lewis score (LS) was developed to standardize quantification of inflammation in small-bowel (SB) CE images.
Goals
Multicenter retrospective study aiming to investigate correlation between LS and FC in a large group of patients undergoing CE for suspected or known small-bowel IBD, and to develop a model for prediction of CE results (LS) based on FC levels.
Study
Five academic centers and a district general hospital offering CE in UK, Finland, Sweden, Canada, and Israel. In total, 333 patients were recruited. They had small-bowel CE and FC done within 3 months.
Results
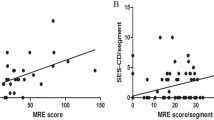
Overall, correlation between FC and LS was weak (r s: 0.232, P < 0.001). When two clinically significant FC thresholds (100 and 250 μg/g) were examined, the r s between FC and LS was 0.247 (weak) and 0.337 (moderate), respectively (P = 0.307). For clinically significant (LS ≥ 135) or negative (LS < 135) for SB inflammation, ROC curves gave an optimum cutoff point of FC 76 μg/g with sensitivity 0.59 and specificity 0.41. Limitations: Retrospective design.
Conclusions
LS appears to show low correlation with FC as well as other serology markers of inflammation. FC does not appear to be a reliable biomarker for significant small-bowel inflammation. Nevertheless, FC level ≥ 76 μg/g may be associated with appreciable visual inflammation on small-bowel CE in patients with negative prior diagnostic workup.

Similar content being viewed by others
References
Koulaouzidis A, Iakovidis DK, Karargyris A, Rondonotti E. Wireless endoscopy in 2020: Will it still be a capsule? World J Gastroenterol. 2015;21:5119–5130. doi:10.3748/wjg.v21.i17.5119.
Gralnek IM, Defranchis R, Seidman E, Leighton JA, Legnani P, Lewis BS. Development of a capsule endoscopy scoring index for small bowel mucosal inflammatory change. Aliment Pharmacol Ther. 2008;27:146–154.
Gal E, Geller A, Fraser G, Levi Z, Niv Y. Assessment and validation of the new capsule endoscopy Crohn’s disease activity index (CECDAI). Dig Dis Sci. 2008;53:1933–1937.
Niv Y, Ilani S, Levi Z, et al. Validation of the Capsule Endoscopy Crohn’s Disease Activity Index (CECDAI or Niv score): a multicenter prospective study. Endoscopy. 2012;44:21–26. doi:10.1055/s-0031-1291385.
Rosa B, Moreira MJ, Rebelo A, Cotter J. Lewis Score: a useful clinical tool for patients with suspected Crohn’s Disease submitted to capsule endoscopy. J Crohns Colitis. 2012;6:692–697. doi:10.1016/j.crohns.2011.12.002.
Cotter J. Dias de Castro F, Magalhães J, Moreira MJ, Rosa B. Validation of the Lewis score for the evaluation of small-bowel Crohn’s disease activity. Endoscopy. 2015;47:330–335. doi:10.1055/s-0034-1390894.
Höög CM, Bark LÅ, Broström O, Sjöqvist U. Capsule endoscopic findings correlate with fecal calprotectin and C-reactive protein in patients with suspected small-bowel Crohn’s disease. Scand J Gastroenterol. 2014;49:1084–1090. doi:10.3109/00365521.2014.920915.
Koulaouzidis A, Douglas S, Plevris JN. Lewis score correlates more closely with fecal calprotectin than Capsule Endoscopy Crohn’s Disease Activity Index. Dig Dis Sci. 2012;57:987–993. doi:10.1007/s10620-011-1956-8.
Gurudu SR, Leighton JA. Correlation of two capsule endoscopy scoring systems with fecal calprotectin: does it really matter? Dig Dis Sci. 2012;57:827–829. doi:10.1007/s10620-012-2079-6.
Fagerhol MK, Dale I, Andersson T. Release and quantitation of a leukocyte derived protein (L1). Scand J Haematol. 1980;24:393–398.
Sipponen T. Diagnostics and prognostics of inflammatory bowel disease with fecal neutrophil-derived biomarkers calprotectin and lactoferrin. Dig Dis. 2013;31:336–344. doi:10.1159/000354689.
Sipponen T, Kolho KL. Fecal calprotectin in diagnosis and clinical assessment of inflammatory bowel disease. Scand J Gastroenterol. 2015;50:74–80. doi:10.3109/00365521.2014.987809.
Logan R. Faecal calprotectin for the diagnosis of inflammatory bowel disease. BMJ. 2010;341:c3636. doi:10.1136/bmj.c3636.
Røseth AG. Determination of faecal calprotectin, a novel marker of organic gastrointestinal disorders. Dig Liver Dis. 2003;35:607–609.
Sipponen T, Haapamäki J, Savilahti E, et al. Fecal calprotectin and S100A12 have low utility in prediction of small bowel Crohn’s disease detected by wireless capsule endoscopy. Scand J Gastroenterol. 2012;47:778–784. doi:10.3109/00365521.2012.677953.
van Rheenen PF, Van de Vijver E, Fidler V. Faecal calprotectin for screening of patients with suspected inflammatory bowel disease: diagnostic meta-analysis. BMJ. 2010;341:c3369. doi:10.1136/bmj.c3369.
Koulaouzidis A, Douglas S, Rogers MA, Arnott ID, Plevris JN. Fecal calprotectin: a selection tool for small bowel capsule endoscopy in suspected IBD with prior negative bi-directional endoscopy. Scand J Gastroenterol. 2011;46:561–566. doi:10.3109/00365521.2011.551835.
Kopylov U, Nemeth A, Koulaouzidis A, et al. Small bowel capsule endoscopy in the management of established Crohn’s disease: clinical impact, safety, and correlation with inflammatory biomarkers. Inflamm Bowel Dis. 2015;21:93–100. doi:10.1097/MIB.0000000000000255.
Sliker LJ, Ciuti G. Flexible and capsule endoscopy for screening, diagnosis and treatment. Expert Rev Med Devices. 2014;11:649–666. doi:10.1586/17434440.2014.941809.
Koulaouzidis A, Iakovidis DK, Karargyris A, Plevris JN. Optimizing lesion detection in small-bowel capsule endoscopy: from present problems to future solutions. Expert Rev Gastroenterol Hepatol. 2015;9:217–235. doi:10.1586/17474124.2014.952281.
Koulaouzidis A, Giannakou A, Yung DE, Dabos KJ, Plevris JN. Do prokinetics influence the completion rate in small-bowel capsule endoscopy? A systematic review and meta-analysis. Curr Med Res Opin. 2013;29:1171–1185. doi:10.1185/03007995.2013.818532.
Koulaouzidis A, Douglas S, Plevris JN. Blue mode does not offer any benefit over white light when calculating Lewis score in small-bowel capsule endoscopy. World J Gastrointest Endosc. 2012;4:33–37. doi:10.4253/wjge.v4.i2.33.
Kopylov U, Seidman EG. Role of capsule endoscopy in inflammatory bowel disease. World J Gastroenterol. 2014;20:1155–1164. doi:10.3748/wjg.v20.i5.1155.
http://www.statstutor.ac.uk/resources/uploaded/spearmans.pdf.
Koulaouzidis A, Nemeth A, Johansson GW, Toth E. Dissecting Lewis score under the light of fecal calprotectin; an analysis of correlation of score components with calprotectin levels in capsule endoscopy. Ann Gastroenterol. 2015;28:259–264.
Bolanis P, Stauropoulou E. The ratio of monocytes to CRP correlates to symptoms induction time of the acute phase. 37 Annual Panhellenic Medical congress, May 2011.
Sandler RS, Everhart JE, Donowitz M, et al. The burden of selected digestive diseases in the United States. Gastroenterology. 2002;122:1500–1511.
Dhaliwal A, Zeino Z, Tomkins C, et al. Utility of faecal calprotectin in inflammatory bowel disease (IBD): what cut-offs should we apply? Frontline Gastroenterol. 2015;6:14–19.
Kopylov U, Yablecovitch D, Lahat A, et al. Detection of small bowel mucosal healing and deep remission in patients with known small bowel Crohn’s disease using biomarkers, capsule endoscopy and imaging. Am J Gastroenterol. 2015;110:1316–1323.
Olsen PA, Fossmark R, Qvigstad G. Fecal calprotectin in patients with suspected small bowel disease–a selection tool for small bowel capsule endoscopy? Scand J Gastroenterol. 2015;50:272–277. doi:10.3109/00365521.2014.1003395.
Gisbert JP, McNicholl AG. Questions and answers on the role of faecal calprotectin as a biological marker in inflammatory bowel disease. Dig Liver Dis. 2009;41:56–66.
Mao R, Xiao YL, Gao X, et al. Fecal calprotectin in predicting relapse of inflammatory bowel diseases: A meta-analysis of prospective studies. Inflamm Bowel Dis. 2012;18:1894–1899.
Summerton CB, Longlands MG, Wiener K, et al. Faecal calprotectin: a marker of inflammation throughout the intestinal tract. Eur J Gastroenterol Hepatol. 2002;14:841–845.
Stawczyk-Eder K, Eder P, Lykowska-Szuber L, et al. Is faecal calprotectin equally useful in all Crohn’s disease locations? A prospective, comparative study. AMS. 2015;1:353–361.
Jensen MD, Kjeldsen J, Nathan T. Fecal calprotectin is equally sensitive in Crohn’s disease affecting the small bowel and colon. Scand J Gastroenterol. 2011;46:694–700.
Lasson A, Stotzer PO, Öhman L, Isaksson S, Sapnara M, Strid H. The intra-individual variability of faecal calprotectin: a prospective study in patients with active ulcerative colitis. J Crohns Colitis. 2015;9:26–32. doi:10.1016/j.crohns.2014.06.002.
Calafat M, Cabré E, Mañosa M, Lobatón T, Marín L, Domènech E. High within-day variability of fecal calprotectin levels in patients with active ulcerative colitis: what is the best timing for stool sampling? Inflamm Bowel Dis. 2015;21:1072–1076. doi:10.1097/MIB.0000000000000349.
Acknowledgments
The authors thank Pirkko Tuukkala and Virpi Pelkonen (both with Helsinki University Central Hospital, Finland) for their invaluable help with the data collection.
Authors’ contributions
All authors contributed to data collection. Dr. A Koulaouzidis created the first draft. All authors critically reviewed the document and provided changes. All authors approved the final version of the article, including the authorship list.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Koulaouzidis received an Given Imaging Ltd/ESGE Ltd research Grant in 2011. He has also accepted material support for research from SynMedUK Ltd. Dr. Seidman has received in-kind research support from Given Imaging/Medtronic Inc., 2011–2015. Rami Eliakim received consultation fees from Given Imaging. The rest of the authors have no disclosure to make.
Competing interests
None.
Patient consent
None.
Ethics approval
Clinical Audit Department at the Royal Infirmary of Edinburgh.
Rights and permissions
About this article
Cite this article
Koulaouzidis, A., Sipponen, T., Nemeth, A. et al. Association Between Fecal Calprotectin Levels and Small-bowel Inflammation Score in Capsule Endoscopy: A Multicenter Retrospective Study. Dig Dis Sci 61, 2033–2040 (2016). https://doi.org/10.1007/s10620-016-4104-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-016-4104-7