Abstract
Background
Antiglycan antibodies have recently been reported to be associated with Crohn’s disease (CD). These antibodies include anti-Saccharomyces cerevisiae mannan antibodies (ASCA), anti-laminariobioside carbohydrate antibodies (ALCA), anti-chitobioside carbohydrate antibodies (ACCA), and anti-mannobioside carbohydrate antibodies (AMCA).
Aims
The aim of this study was to evaluate their diagnostic accuracy in Greek patients with inflammatory bowel disease (IBD).
Methods
Serum was collected from 191 patients with IBD (85 with ulcerative colitis (UC) and 106 with CD), 29 cases with other causes of intestinal inflammation and 96 healthy controls. Antiglycan antibodies were measured using commercially available enzyme immunoassays.
Results
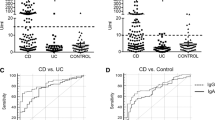
Higher levels of antiglycan antibodies were detected in patients with CD compared to patients with UC and controls. Although all types of antiglycan antibodies had a high specificity for diagnosing CD, their sensitivity was rather low, with best results obtained with ASCA and ALCA (41.5 and 52.8%, respectively). Increased levels of ASCA and ALCA were associated with stricturing and penetrating disease phenotype, and the need for surgery (p < 0.05).
Conclusions
Antiglycan antibodies in Greek IBD patients are significantly associated with CD, and especially to phenotypes of complicated disease, with ASCA and ALCA exhibiting the highest sensitivity.





Similar content being viewed by others
References
Quinton JF, Sendid B, Reumaux D, et al. Anti- Saccharomyces cerevisiae mannan antibodies combined with antineutrophil cytoplasmic autoantibodies in inflammatory bowel disease: prevalence and diagnostic role. Gut. 1998;42:788–791.
Peeters M, Joossens S, Vermeire S, Vlietinck R, Bossuyt X, Rutgeerts P. Diagnostic value of anti-Saccharomyces cerevisiae and antineutrophil cytoplasmic autoantibodies in inflammatory bowel disease. Am J Gastroenterol. 2001;96:730–734.
Sandborn WJ, Loftus EV Jr, Colombel JF, et al. Evaluation of serologic disease markers in a population-based cohort of patients with ulcerative colitis and Crohn’s disease. Inflamm Bowel Dis. 2001;7:192–201.
Koutroubakis IE, Petinaki E, Mouzas IA, et al. Anti Saccharomyces cerevisiae mannan antibodies and antineutrophil cytoplasmic autoantibodies in Greek patients with inflammatory bowel disease. Am J Gastroenterol. 2001;96:449–454.
Zholudev A, Zurakowski D, Young W, Leichtner A, Bousvaros A. Serologic testing with ANCA, ASCA, and anti-OmpC in children and young adults with Crohn’s disease and ulcerative colitis: diagnostic value and correlation with disease phenotype. Am J Gastroenterol. 2004;99:2235–2241.
Mow WS, Vasiliauskas EA, Lin YC, et al. Association of antibody responses to microbial antigens and complications of small bowel Crohn’s disease. Gastroenterology. 2004;126:414–424.
Targan SR, Landers CJ, Yang H, et al. Antibodies to CBir1 flagellin define a unique response that is associated independently with complicated Crohn’s disease. Gastroenterology. 2005;128:2020–2028.
Dubinsky MC, Lin YC, Dutridge D, et al. Serum immune responses predict rapid disease progression among children with Crohn’s disease: immune responses predict disease progression. Am J Gastroenterol. 2006;101:360–367.
Dotan I, Fishman S, Dgani Y, et al. Antibodies against laminaribioside and chitobioside are novel serologic markers in Crohn’s disease. Gastroenterology. 2006;131:366–378.
Li X, Conklin L, Alex P. New serological biomarkers of inflammatory bowel disease. World J Gastroenterol. 2008;14:5115–5124.
Ferrante M, Henckaerts L, Joossens M, et al. New serological markers in inflammatory bowel disease are associated with complicated disease behaviour. Gut. 2007;56:1394–1403.
Papp M, Altorjay I, Dotan N, et al. New serological markers for inflammatory bowel disease are associated with earlier age at onset, complicated disease behavior, risk for surgery, and NOD2/CARD15 genotype in a Hungarian IBD cohort. Am J Gastroenterol. 2008;103:665–681.
Simondi D, Mengozzi G, Betteto S, et al. Antiglycan antibodies as serological markers in the differential diagnosis of inflammatory bowel disease. Inflamm Bowel Dis. 2008;14:645–651.
Rieder F, Schleder S, Wolf A, et al. Association of the novel serologic anti-glycan antibodies anti-laminarin and anti-chitin with complicated Crohn’s disease behavior. Inflamm Bowel Dis. 2010;16:263–274.
Stange EF, Travis SPL, Vermeire S, et al. European Crohn’s and Colitis Organisation. European evidence based consensus on the diagnosis and management of Crohn’s disease: definitions and diagnosis. Gut. 2006;55:1–15.
Silverberg MS, Satsangi J, Ahmad T, et al. Toward an integrated clinical, molecular and serological classification of inflammatory bowel disease: Report of a Working Party of the 2005 Montreal World Congress of Gastroenterology. Can J Gastroenterol. 2005;19(Suppl A):5–36.
Best WR, Becktel JM, Singleton JW, Kern F Jr. Development of a Crohn’s disease activity index. National Cooperative Crohn’s Disease Study. Gastroenterology. 1976;70:439–444.
Walmsley RS, Ayres RC, Pounder RE, Allan RN. A simple clinical colitis activity index. Gut. 1998;43:29–32.
Dotan N, Altstock RT, Schwarz M, Dukler A. Anti-glycan antibodies as biomarkers for diagnosis and prognosis. Lupus. 2006;15:442–450.
Rieder F, Schleder S, Wolf A, et al. Serum anti-glycan antibodies predict complicated Crohn’s disease behavior: A cohort study. Inflamm Bowel Dis. 2010 [Epub ahead of print] PMID: 20024902.
Joossens M, Van Steen K, Branche J, et al. Familial aggregation and antimicrobial response dose-dependently affect the risk for Crohn’s disease. Inflamm Bowel Dis. 2010;16:58–67.
Joossens S, Reinisch W, Vermeire S, et al. The value of serologic markers in indeterminate colitis: a prospective follow-up study. Gastroenterology. 2002;122:1242–1247.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Koutroubakis, I.E., Drygiannakis, D., Tsirogianni, A. et al. Antiglycan Antibodies in Greek Patients with Inflammatory Bowel Disease. Dig Dis Sci 56, 845–852 (2011). https://doi.org/10.1007/s10620-010-1328-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-010-1328-9