Abstract
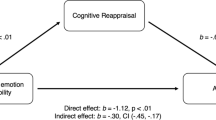
Emotion processing has been demonstrated to have a strong impact on somatic symptom perception. In the current quasi-experimental trial associations between the application of emotion regulation strategies and symptom-related outcomes were examined in subjects with medically unexplained physical symptoms (MUS; n = 48) and in mentally healthy individuals (n = 48). Somatic symptoms were repeatedly induced four times in both samples. After each symptom induction, participants were instructed to apply another of four emotion regulation strategies. Symptom-related outcomes were rated before and after a strategy was applied. Hierarchical linear models showed that in the MUS group cognitive reappraisal was significantly and acceptance was marginally associated with lower symptom annoyance scores compared with compassionate self-support. In healthy subjects distraction was associated with better mood scores compared with compassionate self-support. Future research should examine the effects of acceptance and cognitive reappraisal strategies applied by MUS subjects over a longer period of time.



Similar content being viewed by others
References
Allen, L. A., Woolfolk, R. L., Escobar, J. I., Gara, M. A., & Hamer, R. M. (2006). Cognitive-behavioral therapy for somatization disorder: A randomized controlled trial. Archives of Internal Medicine, 166, 1512–1518. https://doi.org/10.1001/archinte.166.14.1512.
Arnold, B. S., Alpers, G. W., Suess, H., Friedel, E., Kosmuetzky, G., Geier, A., et al. (2008). Affective pain modulation in fibromyalgia, somatoform pain disorder, back pain, and healthy controls. European Journal of Pain, 12, 329–338. https://doi.org/10.1016/j.ejpain.2007.06.007.
Beck, A. T., Steer, R. A., & Brown, G. K. (1996). Beck Depression Inventory II (BDI-II). Manual. San Antonio: Psychological Corporation.
Berking, M., & Whitely, B. (2014). Affect regulation training. A practitioners` manual. Heidelberg: Springer.
Bogaerts, K., Janssens, T., De Peuter, S., Van Diest, I., & Van den Bergh, O. (2010). Negative affective pictures can elicit physical symptoms in high habitual symptom reporters. Psychology & Health, 25, 685–698. https://doi.org/10.1080/08870440902814639.
Bogaerts, K., Notebaert, K., Van Diest, I., Devriese, S., De Peuter, S., & Van den Bergh, O. (2005). Accuracy of respiratory symptom perception in different affective contexts. Journal of Psychosomatic Research, 58, 537–543. https://doi.org/10.1016/j.jpsychores.2004.12.005.
Bogaerts, K., Rayen, L., Lavrysen, A., Van Diest, I., Janssens, T., Schruers, K., et al. (2015). Unraveling the relationship between trait negative affectivity and habitual symptom reporting. PLoS ONE, 10, e0115748. https://doi.org/10.1371/journal.pone.0115748.
Bowen, D. J., Kreuter, M., Spring, B., Cofta-Woerpel, L., Linnan, L., Weiner, D., et al. (2009). How we design feasibility studies. American Journal of Preventive Medicine, 36, 452–457. https://doi.org/10.1016/j.amepre.2009.02.002.
Bowers, H., & Wroe, A. (2016). Beliefs about emotions mediate the relationship between emotional suppression and quality of life in irritable bowel syndrome. Journal of Mental Health, 25, 154–158. https://doi.org/10.3109/09638237.2015.1101414.
Bowers, H., Wroe, A. L., & Pincus, T. (2017). ‘Isn’t it ironic?’ Beliefs about the unacceptability of emotions and emotional suppression relate to worse outcomes in fibromyalgia. Clinical Rheumatology, 36, 1121–1128. https://doi.org/10.1007/s10067-017-3590-0.
Branstetter-Rost, A., Cushing, C., & Douleh, T. (2009). Personal values and pain tolerance: Does a values intervention add to acceptance? Journal of Pain, 10, 887–892. https://doi.org/10.1016/j.jpain.2009.01.001.
Brooks, S. K., Chalder, T., & Rimes, K. A. (2017). Chronic fatigue syndrome: Cognitive, behavioural and emotional processing vulnerability factors. Behavioural and Cognitive Psychotherapy, 45, 156–169. https://doi.org/10.1017/S1352465816000631.
Cohen, J. (1992). A power primer. Psychological Bulletin, 112, 155–159. https://doi.org/10.1037/0033-2909.112.1.155.
Constantinou, E., Bogaerts, K., Van Oudenhove, L., Tack, J., Van Diest, I., & Van den Bergh, O. (2015). Healing words: Using affect labeling to reduce the effects of unpleasant cues on symptom reporting in IBS patients. International Journal of Behavioral Medicine, 22, 512–520. https://doi.org/10.1007/s12529-014-9449-8.
De Gucht, V., & Heiser, W. (2003). Alexithymia and somatisation: A quantitative review of the literature. Journal of Psychosomatic Research, 54, 425–434. https://doi.org/10.1016/S0022-3999(02)00467-1.
de Waal, M. W., Arnold, I. A., Eekhof, J. A., & van Hemert, A. M. (2004). Somatoform disorders in general practice: Prevalence, functional impairment and comorbidity with anxiety and depressive disorders. British Journal of Psychiatry, 184, 470–476. https://doi.org/10.1192/bjp.184.6.470.
Deary, I. J., Scott, S., & Wilson, J. A. (1997). Neuroticism, alexithymia and medically unexplained symptoms. Personality and Individual Differences, 22, 551–564. https://doi.org/10.1016/S0191-8869(96)00229-2.
Derogatis, L. R. (1992). The Brief Symptom Inventory (BSI): Administration, scoring, and procedures manual II. Baltimore: Clinical Psychometric Research.
Diedrich, A., Grant, M., Hofmann, S. G., Hiller, W., & Berking, M. (2014). Self-compassion as an emotion regulation strategy in major depressive disorder. Behaviour Research and Therapy, 58, 43–51. https://doi.org/10.1016/j.brat.2014.05.006.
First, M. B., Spitzer, R. L., Gibbon, M., & Williams, J. B. W. (1996). Structured clinical interview for DSM-IV axis I disorders (SCID). New York: New York State Psychiatric Institute, Biometrics Research.
Fletcher, L., & Hayes, S. C. (2005). Relational frame theory, acceptance and commitment therapy, and a functional analytic definition of mindfulness. Journal of Rational-Emotive and Cognitive Behavior Therapy, 23, 315–336. https://doi.org/10.1007/s10942-005-0017-7.
Gross, J. (1998). The emerging field of emotion regulation: An integrative review. Review of General Psychology, 2, 271–299. https://doi.org/10.1037/1089-2680.2.3.271.
Gutierrez, O., Luciano, C., Rodriguez, M., & Fink, B. C. (2004). Comparison between an acceptance-based and a cognitive-control-based protocol for coping with pain. Behavior Therapy, 35, 767–783. https://doi.org/10.1016/S0005-7894(04)80019-4.
Hayes, S. C., Bissett, R. T., Korn, Z., Zettle, R. D., Rosenfarb, I. S., Cooper, L. D., et al. (1999). The impact of acceptance versus control rationales on pain tolerance. Psychological Record, 49, 33–47. https://doi.org/10.1007/BF03395305.
Hayes, S. C., Strosahl, K. D., & Wilson, K. G. (2012). Acceptance and Commitment Therapy: An experiential approach to behavior change (2nd ed.). New York: The Guilford Press.
Hiller, W., Rief, W., & Brähler, E. (2006). Somatization in the population: From mild bodily misperceptions to disabling symptoms. Social Psychiatry and Psychiatric Epidemiology, 41, 704–712. https://doi.org/10.1007/s00127-006-0082-y.
Hyphantis, T., Goulia, P., & Carvalho, A. F. (2013). Personality traits, defense mechanisms and hostility features associated with somatic symptom severity in both health and disease. Journal of Psychosomatic Research, 75, 362–369. https://doi.org/10.1016/j.jpsychores.2013.08.014.
Jackson, T., Yang, Z., Li, X., Chen, H., Huang, X., & Meng, J. (2012). Coping when pain is a potential threat: The efficacy of acceptance versus cognitive distraction. European Journal of Pain, 16, 390–400. https://doi.org/10.1002/j.1532-2149.2011.00019.x.
Klaus, K., Rief, W., Brahler, E., Martin, A., Glaesmer, H., & Mewes, R. (2013). The distinction between “medically unexplained” and “medically explained” in the context of somatoform disorders. International Journal of Behavioral Medicine, 20, 161–171. https://doi.org/10.1007/s12529-012-9245-2.
Koechlin, H., Coakley, R., Schechter, N., Werner, C., & Kossowskya, J. (2018). The role of emotion regulation in chronic pain: A systematic literature review. Journal of Psychosomatic Research, 107, 38–45. https://doi.org/10.1016/j.jpsychores.2018.02.002.
Kohl, A., Rief, W., & Glombiewski, J. A. (2013). Acceptance, cognitive restructuring, and distraction as coping strategies for acute pain. Journal of Pain, 14, 305–315. https://doi.org/10.1016/j.jpain.2012.12.005.
Kohl, A., Rief, W., & Glombiewski, J. A. (2014). Do fibromyalgia patients benefit from cognitive restructuring and acceptance? An experimental study. Journal of Behavior Therapy and Experimental Psychiatry, 45, 467–474. https://doi.org/10.1016/j.jbtep.2014.06.006.
Köteles, F., & Witthöft, M. (2017). Somatosensory amplification—An old construct from a new perspective. Journal of Psychosomatic Research, 101, 1–9. https://doi.org/10.1016/j.jpsychores.2017.07.011.
Kroenke, K., Spitzer, R. L., & Williams, J. B. W. (2002). The PHQ-15: Validity of a new measure for evaluating the severity of somatic symptoms. Psychosomatic Medicine, 64, 258–266. https://doi.org/10.1097/00006842-200203000-00008.
Leventhal, H., Phillips, L. A., & Burns, E. (2016). The common-sense model of self-regulation (CSM): A dynamic framework for understanding illness self-management. Journal of Behavioral Medicine, 39, 935–946. https://doi.org/10.1007/s10865-016-9782-2.
Lininger, M., Spybrook, J., & Cheatham, C. C. (2015). Hierarchical linear model: Thinking outside the traditional repeated-measures analysis-of-variance box. Journal of Athletic Training, 50, 438–441. https://doi.org/10.4085/1062-6050-49.5.09.
Lumley, M. A., Schubiner, H., Lockhart, N. A., Kidwell, K. M., Harte, S. E., Clauw, D. J., et al. (2017). Emotional awareness and expression therapy, cognitive behavioral therapy, and education for fibromyalgia: A cluster-randomized controlled trial. Pain, 158, 2354–2363. https://doi.org/10.1097/j.pain.0000000000001036.
Margraf, J. (1994). Mini-DIPS: Diagnostic short-interview for mental disorders [Mini-DIPS: Diagnostisches Kurz-Interview bei psychischen Störungen]. Berlin: Springer.
Masedo, A. I., & Esteve, M. R. (2007). Effects of suppression, acceptance and spontaneous coping on pain tolerance, pain intensity and distress. Behaviour Research and Therapy, 45, 199–209. https://doi.org/10.1016/j.brat.2006.02.006.
Mewes, R., Rief, W., Stenzel, N., Glaesmer, H., Martin, A., & Brahler, E. (2009). What is “normal” disability? An investigation of disability in the general population. Pain, 142, 36–41. https://doi.org/10.1016/j.pain.2008.11.007.
Neff, K. (2003). Self-compassion: An alternative conceptualization of a healthy attitude toward oneself. Self and Identity, 2, 85–101. https://doi.org/10.1080/15298860390129863.
Neff, K. D., Kirkpatrick, K. L., & Rude, S. S. (2007). Self-compassion and adaptive psychological functioning. Journal of Research in Personality, 41, 139–154. https://doi.org/10.1016/j.jrp.2006.03.004.
Nix, G., Watson, C., Pyszczynski, T., & Greenberg, J. (1995). Reducing depressive affect through external focus of attention. Journal of Social and Clinical Psychology, 14, 36–52. https://doi.org/10.1521/jscp.1995.14.1.36.
Paez-Blarrina, M., Luciano, C., Gutierrez-Martinez, O., Valdivia, S., Rodriguez-Valverde, M., & Ortega, J. (2008). Coping with pain in the motivational context of values: Comparison between an acceptance-based and a cognitive control-based protocol. Behavior Modification, 32, 403–422. https://doi.org/10.1177/0145445507309029.
Raudenbush, S. W., & Bryk, A. S. (2002). Hierarchical linear models: Applications and data analysis methods (2nd ed.). Thousand Oaks: Sage Publications.
Rief, W., Burton, C., Frostholm, L., Henningsen, P., Kleinstäuber, M., Kop, W. J., et al. (2017). Core outcome domains for clinical trials on somatic symptom disorder, bodily distress disorder and functional somatic syndromes: EURONET-SOMA recommendations. Psychosomatic Medicine, 79, 1008–1015. https://doi.org/10.1097/PSY.0000000000000502.
Rief, W., Heuser, J., & Fichter, M. M. (1996a). What does the Toronto Alexithymia Scale TAS-R measure? Journal of Clinical Psychology. 52, 423–429. https://doi.org/10.1002/(Sici)1097-4679(199607)52:4%3C423::Aid-Jclp6%3E3.0.Co;2-Q
Rief, W., Heuser, J., Mayrhuber, E., Stelzer, I., Hiller, W., & Fichter, M. M. (1996b). The classification of multiple somatoform symptoms. Journal of Nervous and Mental Disease, 184, 680–687.
Rief, W., Hiller, W., & Margraf, J. (1998). Cognitive aspects of hypochondriasis and the somatization syndrome. Journal of Abnormal Psychology, 107, 587–595. https://doi.org/10.1037//0021-843X.107.4.587.
Rief, W., Mewes, R., Martin, A., Glaesmer, H., & Braehler, E. (2010). Are psychological features useful in classifying patients with somatic symptoms? Psychosomatic Medicine, 72, 648–655. https://doi.org/10.1097/Psy.0b013e3181d73fce.
Rimes, K. A., Ashcroft, J., Bryan, L., & Chalder, T. (2016). Emotional suppression in chronic fatigue syndrome: Experimental study. Health Psychology, 35, 979–986. https://doi.org/10.1037/hea0000341.
Roche, B., Forsyth, J. P., & Maher, E. (2007). The impact of demand characteristics on brief acceptance- and control-based interventions for pain tolerance. Cognitive and Behavioral Practice, 14, 381–393. https://doi.org/10.1016/j.cbpra.2006.10.010.
Schobel, J., Pryss, R., Probst, T., Schlee, W., Schickler, M., & Reichert, M. (2018). Learnability of a configurator empowering end users to create mobile data collection instruments: Usability study. JMIR Mhealth and Uhealth, 6, e148. https://doi.org/10.2196/mhealth.9826.
Schwarz, J., Gottschalk, J.-M., Ruckmann, J., Rief, W., & Kleinstäuber, M. (2016). An experimental paradigm to repeatedly induce somatic symptoms. Journal of Psychosomatic Research, 82, 24–30. https://doi.org/10.1016/j.jpsychores.2016.01.007.
Sharpe, M., Mayou, R., & Bass, C. (1995). Concepts, theories and terminology. In R. Mayou, C. Bass, & M. Sharpe (Eds.), Treatment of functional somatic symptoms (pp. 3–16). Oxford: Oxford University Press.
Sibelli, A., Chalder, T., Everitt, H., Chilcot, J., & Moss-Morris, R. (2018). Positive and negative affect mediate the bidirectional relationship between emotional processing and symptom severity and impact in irritable bowel syndrome. Journal of Psychosomatic Research, 105, 1–13. https://doi.org/10.1016/j.jpsychores.2017.11.016.
Singer, J. D., & Willett, J. B. (2003). Applied longitudinal data analysis: Modeling change and event occurrence. New York: Oxford University Press.
Thakur, E. R., Holmes, H. J., Lockhart, N. A., Carty, J. N., Ziadni, M. S., Doherty, H. K., et al. (2017). Emotional awareness and expression training improves irritable bowel syndrome: A randomized controlled trial. Neurogastroenterology and Motility. https://doi.org/10.1111/nmo.13143.
Torous, J., Kiang, M. V., Lorme, J., & Onnela, J. P. (2016). New tools for new research in psychiatry: A scalable and customizable platform to empower data driven smartphone research. JMIR Mental Health, 3, e16. https://doi.org/10.2196/mental.5165.
Van Breukelen, G. J. (2006). ANCOVA versus change from baseline: More power in randomized studies, more bias in nonrandomized studies [corrected]. Journal of Clinical Epidemiology, 59, 920–925. https://doi.org/10.1016/j.jclinepi.2006.02.007.
Van Dessel, N., Den Boeft, M., Van der Wouden, J. C., Kleinstäuber, M., Leone, S. S., Terluin, B., et al. (2014). Non-pharmacological interventions for somatoform disorders and medically unexplained physical symptoms (MUPS) in adults. Cochrane Database of Systematic Reviews, 11, CD011142. https://doi.org/10.1002/14651858.CD011142.pub2.
van Eck van der Sluijs, J. V., Ten Have, M., Rijnders, C., van Marwijk, H., de Graaf, R., & van der Feltz-Cornelis, C. (2015). Medically unexplained and explained physical symptoms in the general population: Association with prevalent and incident mental disorders. PLoS ONE, 10, e0123274. https://doi.org/10.1371/journal.pone.0123274.
van Ravesteijn, H. J., Suijkerbuijk, Y. B., Langbroek, J. A., Muskens, E., Lucassen, P. L., van Weel, C., et al. (2014). Mindfulness-based cognitive therapy (MBCT) for patients with medically unexplained symptoms: Process of change. Journal of Psychosomatic Research, 77, 27–33. https://doi.org/10.1016/j.jpsychores.2014.04.010.
Vowles, K. E., McNeil, D. W., Gross, R. T., McDaniel, M. L., Mouse, A., Bates, M., et al. (2007). Effects of pain acceptance and pain control strategies on physical impairment in individuals with chronic low back pain. Behavior Therapy, 38, 412–425. https://doi.org/10.1016/j.beth.2007.02.001.
Weiss, F. D., Rief, W., Martin, A., Rauh, E., & Kleinstäuber, M. (2016). The heterogeneity of illness behaviors in patients with medically unexplained physical symptoms. International Journal of Behavioral Medicine, 23, 319–326. https://doi.org/10.1007/s12529-015-9533-8.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Maria Kleinstäuber, Japhia-Marie Gottschalk, Judith Ruckmann, Thomas Probst and Winfried Rief declare that they have no conflicts of interest.
Ethical Approval
The research was approved by the Ethics Committee of the Department of Psychology, Philipps-Universität Marburg, Germany (2012-26K).
Informed Consent
All participants provided written informed consent.
Animal Rights
No animal studies were carried out by the authors for this article.
Appendix: Emotion Regulation Task Instructions
Appendix: Emotion Regulation Task Instructions
Acceptance Strategy
First, please focus on your somatic symptom right now, even if it is unpleasant. [Short break]
We will start this strategy by practicing mindfulness; focus on your breathing sensations without trying to control them. When you become distracted, you should find a word to describe what is happening and gently bring your attention back to your breathing. Now, we are going to practice shifting your focus and awareness onto your somatic symptom, your thoughts, and your emotions in the moment. Consider that when emotions, symptoms, and thoughts are accepted, they can no longer control behavioral tendencies and cannot interfere with your personal goals. Try to label your somatic symptoms, your feelings, and your thoughts with short mental notes without evaluating them. Name everything as accurately as possible at this moment. Then, try to rate the intensity of these symptoms, feelings, and thoughts on a scale from 0 to 10. Now, do your best to create a positive attitude toward your feelings, symptoms, and thoughts. Next, remind yourself that you can tolerate challenging feelings, symptoms, and thoughts, at least for a while. Think of ways you have been able to endure intensely negative situations in the past. Now, continue by reminding yourself that feelings, symptoms, and thoughts are not permanent.
Now, you will hear the audio recording of your symptom report again. Try to accept all of your thoughts, your emotions, and your symptoms to make it easier for you to deal with and to put up with your somatic symptom. Try to apply the strategy you just heard described. [Two-minute break] Now, slowly bring your attention back to this room at your own pace and open your eyes.
Cognitive Reappraisal Strategy
[Material needed: sheet of paper, pen]
First, please focus on your somatic symptom right now, even if it is unpleasant. [Short break] Please write down on this sheet of paper two different thoughts concerning your somatic symptom. For example, you might think that it is getting worse, it will never stop, or that you cannot put up with it. [One-minute break] Now, I would like you to put down your pen. [Short break]
Sometimes, it helps to consider a situation from different perspectives and to develop another point of view. Depending on how we judge a certain situation, we have different feelings and behavioral tendencies. On the one hand, negative thoughts may influence bodily sensations in a negative way. On the other hand, positive thoughts may cause pleasant bodily sensations. The way you feel and the way your body responds depends on how you appraise the situation. Unpleasant thoughts can be replaced by helpful thoughts. Therefore, you act differently depending on your point of view. Please read again through your thoughts. I want you to try to develop another point of view of the somatic symptoms. Here are some examples of helpful thoughts: “I feel really bad right now, but I’m certain I do not have a serious illness” or “Other people are worse off than me.” To help yourself, imagine what a good friend might advise you to do when you experience somatic symptoms. Try to modify your thoughts and evolve alternative and helpful thoughts that will make it easier for you to endure the discomfort. Please collect these thoughts and write them down. [One-minute break]
Now, you will hear the audio recording of your symptom report again. Try to use your alternative and helpful thoughts to make it easier for you to deal with and to put up with your somatic symptom. Try to apply the strategy you just heard described. [Two-minute break] Now, slowly bring your attention back to this room at your own pace and open your eyes.
Compassionate Self-Support Strategy
First, please focus on your somatic symptom right now, even if it is unpleasant. [Short break]
Do your best to let a feeling of compassion toward yourself rise within you—a strong and warm feeling of empathy for yourself that is accompanied by the desire to help yourself and to end your suffering. Visualize yourself entering this scene. Observe yourself and try to become aware of what distresses you in this scenario. Tell yourself that this somatic symptom creates a difficult situation. Normalize your negative emotions and provide reassurance by telling yourself that you are there to support and reassure yourself (not to give advice). If it seems appropriate, visualize giving yourself a gesture of compassion (e.g., laying a hand on your shoulder or giving yourself a hug). Provide encouragement to yourself. You might say something like, “You have gone through a lot in the past and you will get through this too. I will be with you as you work through this. We will get through this together.” Give yourself a big, kind, reassuring smile. Take your time as you give yourself all the support you need in this situation. Then, when the moment feels right, you can begin to mentally say goodbye to yourself at your own pace. Remember that this is not a goodbye forever. You will always be able to mentally return to this place and provide support for yourself when needed. If there is something you want to say to yourself before leaving, feel free to do so now.
Now, you will hear the audio recording of your symptom report again. Try to provide support for yourself to make it easier for you to deal with and to put up with your somatic symptom. Try to apply the strategy you just heard described [Two-minute break]. Now, slowly bring your attention back to this room at your own pace and open your eyes.
Distraction Strategy
First, please focus on your somatic symptom right now, even if it is unpleasant. [Short break]
Distraction can lead to reduced perception of thoughts, feelings, and somatic symptoms. Our attention works like a spotlight. Therefore, shifting attention to other aspects can help us to cope with somatic symptoms, unpleasant thoughts, and feelings. [At this point, a story about a famous botanic garden and its gardener was narrated. The story is written in a way to stimulate an imagining which arouses all senses and distracts the participant.]
Now, you will hear the audio recording of your symptom report again. Try to shift your attention and apply the strategy you just heard described. [Two-minute break] Now, slowly bring your attention back to this room at your own pace and open your eyes.
Rights and permissions
About this article
Cite this article
Kleinstäuber, M., Gottschalk, JM., Ruckmann, J. et al. Acceptance and Cognitive Reappraisal as Regulation Strategies for Symptom Annoyance in Individuals with Medically Unexplained Physical Symptoms. Cogn Ther Res 43, 570–584 (2019). https://doi.org/10.1007/s10608-018-9973-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10608-018-9973-y