Abstract
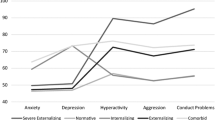
We sought to identify needs for behavioral health care in a large, urban pediatric primary care (PPC) clinic serving a population covered by Medicaid. Specifically, children (N = 197; 120 girls; 91 % African American) ages 8–17 years and their caregivers completed measures of internalizing and externalizing symptoms (RCADS, RCADS-P, MASC, and SDQ). Clinical elevations on all but one domain of the SDQ were significantly higher than expected. However, self-reported anxiety and depression symptoms were consistent with expectations. These findings suggest urban, low-income, primarily African American youth presenting at a PPC clinic demonstrate significant levels of behavioral and emotional symptoms. Implications of the findings include the need to ask both parents and children about child behavioral health problems and the possible influence of screening tool selection on detection.
Similar content being viewed by others
References
Reef J, van Meurs I, Verhulst FC, van der Ende J (2010) Children’s problems predict adults’ DSM-IV disorders across 24 years. J Am Acad Child Adolesc Psychiatry 49:1117–1124
Lehrer JA, Shrier LA, Gortmaker S, Buka S (2006) Depressive symptoms as a longitudinal predictor of sexual risk behaviors among US middle and high school students. Pediatrics 118:189–200
Kaplow JB, Curran PJ, Angold A, Costello EJ (2001) The prospective relation between dimensions of anxiety and the initiation of adolescent alcohol use. J Clin Child Psychol 30:316–326
Foley DL, Goldston DB, Costello EJ, Angold A (2006) Proximal psychiatric risk factors for suicidality in youth: the Great Smoky Mountains study. Arch Gen Psychiatry 63:1017–1024
Copeland WE, Miller-Johnson S, Keeler G, Angold A, Costello JE (2007) Childhood psychiatric disorders and young adult crime: a prospective, population-based study. Am J Psychiatry 164:1668–1675
Kataoka SH, Zhang L, Wells KB (2002) Unmet need for mental health care among US children: variation by ethnicity and insurance status. Am J Psychiatry 159:1548–1555
Alegria M, Vallas M, Pumariega AJ (2010) Racial and ethnic disparities in pediatric mental health. Child Adolesc Psychiatr Clin N Am 19:759–774
Slopen N, Fitzmaurice G, Williams DR, Gilman SE (2010) Poverty, food insecurity, and the behavior for childhood internalizing and externalizing disorders. J Am Acad Child Adolesc Psychiatry 49:444–452
Flannery DJ, Wester KL, Singer MI (2004) Impact of exposure to violence in school on child and adolescent mental health and behavior. J Commun Psychol 32:559–573
Horowitz K, Weine S, Jekel J (1995) PTSD symptoms in urban adolescent girls: compounded community trauma. J Am Acad Child Adolesc Psychiatry 34:1353
Grant KE, Compas BE, Thurm AE, McMahon SD, Gipson PY, Campbell AJ et al (2006) Stressors and child and adolescent psychopathology: evidence of moderating and mediating effects. Clin Psychol Rev 26:257–283
Qi CH, Kaiser AP (2003) Behavior problems of preschool children from low-income families: review of the literature. Topics Early Child Spec Educ 23:188–216
Kelleher KJ, McInerny JK, Gardner WP, Childs GE, Wasserman RC (2000) Increasing identification of psychosocial problems. Pediatrics 105:1313–1321
Chavira AD, Stein MB, Bailey K, Stein MT (2004) Child anxiety in primary care: prevalent but untreated. Depress Anxiety 20:155–164
Costello EJ, Edelbrock C, Costello AJ, Dulcan MK, Burns BJ, Brent D (1988) Psychopathology in pediatric primary care: the new hidden morbidity. Pediatrics 82:415–424
Polaha J, Dalton WT, Allen S (2011) The prevalence of emotional and behavior problems in pediatric primary care serving rural children. J Pediatr Psychol 36:652–660
Costello EJ, Mustillo S, Erkanli A, Keeler G, Angold A (2003) Prevalence and development of psychiatric disorders in childhood and adolescence. Arch Gen Psychiatry 60:837–844
Lefler EK, Hartung CM, Fedele DA (2012) Psychometric properties of a primary care mental health screening tool for young children. Child Health Care 41:79–96
Brown JD, Riley AW, Wissow LS (2007) Identification of youth psychosocial problems during pediatric primary care visits. Adm Policy Ment Health 34:269–281
Costello EJ, Shugart MA (1992) Above and below the threshold: severity of psychiatric symptoms and functional impairment in a pediatric sample. Pediatrics 90:359–368
Neal AM, Turner SM (1991) Anxiety disorders research with African Americans: current status. Psychol Bull 109:400–410
Neighbors HW (1988) The help-seeking behavior of Black Americans: a summary of findings from the national survey of Black Americans. J Natl Med Assoc 80:1009–1012
Wren FJ, Berg EA, Heiden LA, Kinnamon CJ, Ohlson LA, Bridge JA et al (2007) Childhood anxiety in a diverse primary care population: parent-child reports, ethnicity, and SCARED factor structure. J Am Acad Child Adolesc Psychiatry 46:332–340
Weersing VR, Iyengar S, Kolko DJ, Birmaher B, Brent DA (2006) Effectiveness of cognitive-behavioral therapy for adolescent depression: a benchmarking investigation. Behav Ther 37:36–48
Chorpita BF, Yim L, Moffitt C, Umemoto LA, Francis SE (2000) Assessment of symptoms of DSM-IV anxiety and depression in children: a revised child anxiety and depression scale. Behav Res Ther 38:835–855
Ebesutani C, Bernstein A, Nakamura BJ, Chorpita BF, Weisz JR (2010) A psychometric analysis of the Revised Child Anxiety and Depression Scale—Parent Version in a clinical sample. J Abnorm Child Psychol 38:249–260
Brown RC, Yaroslavsky I, Quinoy AM, Friedman AD, Brookman RR, Southam-Gerow MA (2013) Factor structure of measures of anxiety and depression symptoms in African American youth. Child Psychiatry Hum Dev 44:525–536
March JS, Parker JDA, Sullivan K, Stallings P, Conners CK (1997) The Multidimensional Anxiety Scale for Children (MASC): factor structure, reliability, and validity. J Am Acad Child Adolesc Psychiatry 36:554–565
Brown RC, Yaroslavsky I, Quinoy AM, Friedman AD, Brookman RR, Southam-Gerow MA (2013) Psychometric evaluation of measures of anxiety and depression symptoms in an urban African American sample. Child Psychiatry Hum Dev 44:525–536
Goodman R (1997) The Strengths and Difficulties Questionnaire: a research note. J Child Psychol Psychiatry 38:581–586
Bourdon KH, Goodman R, Rae DS, Simpson G, Koretz DS (2005) The Strengths and Difficulties Questionnaire: U.S. normative data and psychometric properties. J Am Acad Child Adolesc Psychiatry 44:557–564
Shirk SR, Kaplinski H, Gudmundsen G (2009) School-based cognitive-behavioral therapy for depression: a benchmarking study. J Emot Behav Disord 17:106–117
US Department of Health and Human Services (2009) Annual update of the HHS poverty guidelines. Fed Regist 74:4199–4201
Holm S (1979) A simple sequentially rejective multiple test procedure. Scand Stat Theory Appl 6:65–70
Jaccard J, Guilamo-Ramos V (2002) Analysis of variance frameworks in clinical child and adolescent psychology: issues and recommendations. J Clin Child Adolesc Psychol 31:130–146
Centers for Disease Control and Prevention (2010) Youth risk behavior surveillance—United States, 2009. MMWR Surveill Summ 59:1–142
Fitzpatrick KM, Boldizar JP (1993) The prevalence and consequences of exposure to violence among African American youth. J Am Acad Child Adolesc Psychiatry 32:424–430
Manassis K, Ickowicz A, Picard E, Antle B, McNeill T, Chahaver A et al (2009) An innovative child CBT training model for community mental health practitioners in Ontario. Acad Psychiatry 33:394–399
De Los Reyes A, Kazdin AE (2005) Informant discrepancies in the assessment of childhood psychopathology: a critical review, theoretical framework, and recommendations for further study. Psychol Bull 131:483–509
Goodman A, Goodman R (2009) Strengths and difficulties questionnaire as a dimensional measure of child mental health. J Am Acad Child Adolesc Psychiatry 48:400–403
Goodman A, Goodman R (2011) Population mean scores predict child mental disorder rates: validating SDQ prevalence estimators in Britain. J Child Psychol Psychiatry 52:100–108
Dickey WC, Blumberg SJ (2004) Revisiting the factor structure of the Strengths and Difficulties Questionnaire: United States, 2001. J Am Acad Child Adolesc Psychiatry 43:1159–1167
Ruchkin V, Jones S, Vermeiren R, Schwab-Stone M (2008) The Strengths and Difficulties Questionnaire: the self-report version in American urban and suburban youth. Psychol Assess 20:175–182
McLean CP, Anderson ER (2009) Brave men and timid women? A review of the gender differences in fear and anxiety. Clin Psychol Rev 29:496–505
Poulton R, Milne BJ, Craske MG, Menzies RG (2001) A longitudinal study of the etiology of separation anxiety. Behav Res Ther 39:1395–1410
Foster JD, Kuperminc GP, Price AW (2004) Gender differences in posttraumatic stress and related symptoms among inner-city minority youth exposed to community violence. J Youth Adolesc 33:59–69
Kingery JN, Ginsburg GS, Burstein M (2009) Factor structure and psychometric properties of the Multidimensional Anxiety Scale for Children in an African American adolescent sample. Child Psychiatry Hum Dev 40:287–300
Lambert SF, Cooley MR, Campbell KDM, Benoit MZ, Stansbury R (2004) Assessing anxiety sensitivity in inner-city African American children: psychometric properties of the Childhood Anxiety Sensitivity Index. J Clin Child Adolesc Psychol 33:248–259
Wissow LS, Brown J, Fothergill KE, Gadomski A, Hacker K, Salmon P et al (2013) Universal mental health screening in pediatric primary care: a systematic review. J Am Acad Child Adolesc Psychiatry 52:1134–1147
Bailey KA, Chavira DA, Stein MT, Stein MB (2006) Brief measures to screen for social phobia in primary care pediatrics. J Pediatr Psychol 31:512–521
Foy JM, Kelleher KJ, Laraque D, the American Academy of Pediatrics Task Force on Mental Health, (2010) Enhancing pediatric mental health care: strategies for preparing a primary care practice. Pediatrics 125:S87–S108
Weersing VR, Gonzalez A, Campo JV, Lucas AN (2008) Brief behavioral therapy for pediatric anxiety and depression: piloting an integrated treatment approach. Cogn Behav Pract 15:126–139
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hourigan, S.E., Southam-Gerow, M.A. & Quinoy, A.M. Emotional and Behavior Problems in an Urban Pediatric Primary Care Setting. Child Psychiatry Hum Dev 46, 289–299 (2015). https://doi.org/10.1007/s10578-014-0469-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10578-014-0469-z