Abstract
Postoperative adhesions commonly cause severe complications, and also increase the risk of adhesiolysis. To improve postoperative adhesion, a series of 2-methacryloyloxy ethyl phosphorylcholine conjugated methylcellulose (MC-g-MPC) derivatives were synthesized to utilize the anti-protein adsorption of 2-methacryloyloxy ethyl phosphorylcholine and the thermosensitivity of methylcellulose. The structures of MC-g-MPC derivatives were characterized by Fourier transform infrared spectroscopy (FTIR) and 1H nuclear magnetic resonance (1H NMR) analyses, and their thermosensitivities were studied by rheological analysis. The gelling temperature of the MC-g-MPC hydrogel was 33 °C and gelling time of the hydrogel under body temperature was 2.5 min. The morphology of the MC-g-MPC hydrogel was observed by scanning electron microscopy (SEM). The results of in vitro cytotoxicity and immunotoxicity, and hemolysis assays demonstrated the good biocompatibility of MC-g-MPC hydrogels. Following the injection of the MC-g-MPC hydrogel, the postoperative adhesion of damaged ceca in Sprague–Dawley rats was improved when compared with a control group (no treatment). In addition, MC-g-MPC-0.25 hydrogel could downregulate the expression of Col-I and Col-IV collagen proteins, thus exert its anti-protein absorption capacity. Therefore, the MC-g-MPC hydrogel is a promising biomaterial for preventing postoperative adhesion.
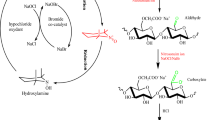
Graphic abstract











Similar content being viewed by others
References
Bang S, Ko YG, Kim WI, Cho D, Park WH, Kwon OH (2017) Preventing postoperative tissue adhesion using injectable carboxymethyl cellulose-pullulan hydrogels. Int J Biol Macromol 105:886–893
Belluco C, Meggiolaro F, Pressato D, Pavesio A, Bigon E, DonàM Forlin M, Nitti D, Lise M (2001) Prevention of postsurgical adhesions with an auto crosslinked hyaluronan derivative gel. J Surg Res 100(2):217–221
Bertelli R, Valenti F, Oleggini R, Caridi G, Altieri P, Coviello DA, Botti G, Ravazzolo R, Ghiggeri GM (1998) Cell-specific regulation of a 1(III) and a 2(V) collagen by TGF-b1 in tubulointerstitial cell models. Nephrol Dial Transpl 13(3):573–579
Broek RPG, Stommel MWJ, Strik C, Van Laarhoven CJHM, Keus F, Van Goor H (2014) Benefits and harms of adhesion barriers for abdominal surgery: a systematic review and meta-analysis. Lancet 383:48–59
Chen C, Chen S, Mao S, Tsai M, Chou P, Liao C, Chen J (2017) Injectable thermosensitive hydrogel containing hyaluronic acid and chitosan as a barrier for prevention of postoperative peritoneal adhesion. Carbohydr Polym 173:721–731
Cheng F, Wu Y, Li H, Yan T, Wei X, Wu G (2019) Biodegradable N, O-carboxymethyl chitosan/oxidized regenerated cellulose composite gauze as a barrier for preventing postoperative adhesion. Carbohydr Polym 207:180–190
Chou P, Chen S, Chen C, Chen S, Teng Y, Chen J (2017) Thermo-responsive in situ forming hydrogels as barriers to prevent post-operative peritendinous adhesion. Acta Biomater 63:85–95
Coleman MG, McLain AD, Moran BJ (2000) Impact of previous surgery on time taken for incision and division of adhesions during laparotomy. Dis Colon Rectum 43(9):1297–1299
Davey AK, Maher PJ (2007) Surgical adhesions: a timely update, a great challenge for the future. J Minim Invasive Gynecol 14(1):15–22
Ellis H (1997) The clinical significance of adhesions: focus on intestinal obstruction. Eur J Surg Suppl Acta Chir 577:5–9
Ellis H (2001) Medicolegal consequences of postoperative intra-abdominal adhesions. J R Soc Med 94(7):331–332
Gao W, Feng Y, Lu J, Khan M, Guo J (2012) Biomimetic surface modification of polycarbonateurethane film via phosphorylcholine-graft for resisting platelet adhesion. Macromol Res 20(10):1063–1069
Gao B, Feng Y, Lu J, Zhang L, Zhao M, Shi C, Khan M, Guo J (2013) Grafting of phosphorylcholine functional groups on polycarbonate urethane surface for resisting platelet adhesion. Mater Sci Eng C 33(5):2871–2878
Guo W, Deng L, Yu J, Chen Z, Woo Y, Liu H, Li T, Lin T, Chen H, Zhao M, Zhang L, Li G, Hu Y (2018a) Sericin nanomicelles with enhanced cellular uptake and pH-triggered release of doxorubicin reverse cancer drug resistance. Drug Deliv 25(1):1103–1116
Guo W, Deng L, Chen Z, Chen Z, Yu J, Liu H, Li T, Lin T, Chen H, Zhao M, Zhang L, Li G, Hu Y (2018b) Vitamin B12-conjugated sericin micelles for targeting CD320-overexpressed gastric cancer and reversing drug resistance. Nanomedicine 14(3):353–370
Haney AF, Hesla J, Hurst BS, Kettel LM, Murphy AA, Rock JA, Rowe G, Schlaff WD (1995) Expanded polytetrafluoroethylene (Gore-lex Surgical Membrane*) is superior to oxidized regenerated cellulose (Interceed lC7+) in preventing adhesions. Fertil Steril 63(5):1021–1026
Healy MW, Schexnayder B, Connell MT, Terry N, Decherney AH, Csokmay J, Yauger BJ, Hill MJ (2016) Intrauterine adhesion prevention after hysteroscopy: a systematic review and meta-analysis. Am J Obstet Gynecol 215(3):267–275
Hershlag A, Diamond MP, DeCherney Ah (1999) Adhesiolysis. Clin Obstet Gynecol 34(2):395–402
Kamel RM (2010) Prevention of postoperative peritoneal adhesions. Eur J Obstet Gynecol Reprod Biol 150(2):111–118
Kim EJ, Choi JS, Kim JS, Choi YC, Cho YW (2016) Injectable and thermosensitive soluble extracellular matrix and methylcellulose hydrogels for stem cell delivery in skin wounds. Biomacromol 17(1):4–11
Kokubo T, Takadama H (2006) How useful is SBF in predicting in vivo bone bioactivity? Biomaterials 27(15):2907–2915
Lauder CIW, Garcea G, Strickland A, Maddern GJ (2010) Abdominal adhesion prevention: still a sticky subject? Dig Surg 27(15):347–358
Li L, Shan H, Yue CY, Lam YC, Tam KC, Hu X (2002) Thermally induced association and dissociation of methylcellulose in aqueous solutions. Langmuir 18(20):7291–7298
Li J, Feng X, Liu B, Yu Y, Sun L, Liu T, Wang Y, Ding J, Chen X (2017) Polymer materials for prevention of postoperative adhesion. Acta Biomater 61:21–40
Lodge AJ, Wells WJ, Backer CL, O’Brien JE, Austin EH, Bacha EA, Weinstein S (2008) A novel bioresorbable film reduces postoperative adhesions after infant cardiac surgery. Ann Thorac Surg 86(2):614–621
Luo Z, Hu Y, Xin R, Zhang B, Li J, Ding X, Hou Y, Yang L, Cai K (2014) Surface functionalized mesoporous silica nanoparticles with natural proteins for reduced immunotoxicity. J Biomed Mater Res 102(11):3781–3794
Lustenberger T, Inaba K, Demetriades D, Ph D (2011) Prevention of postoperative peritoneal adhesions: a review of the literature. Am J Surg 201(1):111–121
Matsuda S, Se N, Iwata H, Ikada Y (2002) Evaluation of the antiadhesion potential of UV cross-linked gelatin films in a rat abdominal model. Biomaterials 23:2901–2908
Metwally M, Cheong Y, Li TC (2008) A review of techniques for adhesion prevention after gynaecological surgery. Curr Opin Obstet Gynecol 20(4):345–352
Mohan H, Krumbholz M, Sharma R, Eisele S, Junker A, Sixt M, Newcombe J, Wekerle H, Hohlfeld R, Lassmann H, Meinl E (2010) Extracellular matrix in multiple sclerosis lesions: fibrillar collagens, biglycan and decorin are upregulated and associated with infiltrating immune cells. Brain Pathol 20(5):966–975
Ohya S, Sonoda H, Nakayama Y, Matsuda T (2005) The potential of poly(N-isopropylacrylamide) (PNIPAM)-grafted hyaluronan and PNIPAM-grafted gelatin in the control of post-surgical tissue adhesions. Biomaterials 26(6):655–659
Shi K, Xue B, Liao J, Qu Y, Qian Z (2017) Polymeric hydrogels for post-operative adhesion prevention: a review. Mater Express 7(6):417–438
Sikirica V, Bapat B, Candrilli SD, Davis KL, Wilson M, Johns A (2011) The inpatient burden of abdominal and gynecological adhesiolysis in the US. BMC Surg 11(13):1–9
Suvik A, Effendy AMN (2012) The use of modified masson’s trichrome staining in collagen evaluation in wound healing study. Mal J Vet Res 3(1):39–47
Tate MC, Shear DA, Hoffman SW, Stein DG, LaPlaca MC (2011) Biocompatibility of methylcellulose-based constructs designed for intracerebral gelation following experimental traumatic brain injury. Biomaterials 22(10):1113–1123
Ward BC, Panitch A (2011) Abdominal adhesions: current and novel therapies. J Surg Res 165(1):91–111
Wells MR, Kraus K, Batter DK, Blunt DG, Weremowitz J, Lynch SE, Antoniades HN, Hansson HA (1997) Gel matrix vehicles for growth factor application in nerve gap injuries repaired with tubes: a comparison of biomatrix, collagen, and methylcellulose. Exp Neurol 146(2):395–402
Wiseman DM, Gottlick-Iarkowski L, Kamp L (1999) Effect of different barriers of oxidized regenerated cellulose (ORC) on cecal and sidewall adhesions in the presence and absence of bleeding. J Invest Surg 12(3):141–146
Wu W, Cheng R, Neves J, Tang J, Xiao J, Ni Q, Liu X, Pan G, Li D, Cui W, Sarmento B (2017) Advances in biomaterials for preventing tissue adhesion. J Controll Release 261:318–336
Xiao K, Wang Z, Wu Y, Lin W, He Y, Zhan J, Luo F, Li Z, Li J, Tan H, Fu Q (2019) Biodegradable anti-adhesive and tough polyurethane hydrogels crosslinked by triol crosslinkers. J Biomed Mater Res 107A:2205–2221
Yeo Y, Highley CB, Bellas E, Ito T, Marini R, Langer R, Kohane DS (2006) In situ cross-linkable hyaluronic acid hydrogels prevent post-operative abdominal adhesions in a rabbit model. Biomaterials 27(27):4698–4705
Yeo Y, Adil M, Bellas E, Astashkina A, Chaudhary N, Kohane DS (2007) Prevention of peritoneal adhesions with an in situ cross-linkable hyaluronan hydrogel delivering budesonide. J Controlled Release 120(3):178–185
Yuan J, Lin S, Shen J (2008) Enhanced blood compatibility of polyurethane functionalized with sulfobetaine. Colloids Surf B 66(1):90–95
Yuan B, He C, Dong X, Wang J, Gao Z, Wang Q, Tian H, Chen X (2015) 5-Fluorouracil loaded thermosensitive PLGA–PEG–PLGA hydrogels for the prevention of postoperative tendon adhesion. RSC Adv 5:25295–25303
Yumoto H, Hirota K, Hirao K, Miyazaki T, Yamamoto N, Miyamoto K, Murakami K, Fujiwara N, Matsuo T, Miyake Y (2015) Anti-inflammatory and protective effects of 2-methacryloyloxyethyl phosphorylcholine polymer on oral epithelial cells. J Biomed Mat Res Part A 103(2):555–563
Zhang Z, Ni J, Chen L, Yu L, Xu J, Ding J (2011) Biodegradable and thermoreversible PCLA–PEG–PCLA hydrogel as a barrier for prevention of post-operative adhesion. Biomaterials 32(21):4725–4736
Zhang Y, Gao C, Li X, Xu C, Zhang Y, Sun Z, Liu Y, Gao J (2014) Thermosensitive methyl cellulose-based injectable hydrogels for post-operation anti-adhesion. Carbohydr Polym 101:171–178
Zhang E, Li J, Zhou Y, Chen P, Ren B, Qin Z, Ma L, Cui J, Sun H, Yao F (2017) Biodegradable and injectable thermoreversible xyloglucan based hydrogel for prevention of postoperative adhesion. Acta Biomater 55:420–433
Zhang X, Sun G, Tian M, Wang Y, Qu C, Cheng X, Feng C, Chen X (2019) Mussel-inspired antibacterial polydopamine/chitosan/temperature-responsive hydrogels for rapid hemostasis. Int J Biol Macromol 138:321–333
Zhu L, Zhang YQ (2016) Postoperative anti-adhesion ability of a novel carboxymethyl chitosan from silkworm pupa in a rat cecal abrasion model. Mater Sci Eng C 61:387–395
Zou W, Chen Y, Zhang X, Li J, Sun L, Gui Z, Du B, Chen S (2018) Cytocompatible chitosan based multi-network hydrogels with antimicrobial, cell anti-adhesive and mechanical properties. Carbohydr Polym 202:246–257
Acknowledgments
We acknowledge support from the Special Funds for Public Welfare Research and Capacity Building of Guangdong Province in China (2016A020222017 and 2016A010103014), the Key project of Guangdong Natural Science Foundation of China (2017B030311007), and the Science and Technology Planning Project of Guangdong Province in China (2012B091100356).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
There is no conflict of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary material 1 (MOV 21941 kb)
Supplementary material 2 (MOV 37227 kb)
Rights and permissions
About this article
Cite this article
Huang, Y., Guo, W., Zhang, J. et al. Thermosensitive hydrogels based on methylcellulose derivatives for prevention of postoperative adhesion. Cellulose 27, 1555–1571 (2020). https://doi.org/10.1007/s10570-019-02857-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10570-019-02857-4