Abstract
Objective
In this retrospective cohort study of consecutive patients with atrial fibrillation and surgical or transcatheter bioprosthetic valve, we compared the efficacy and safety of direct oral anticoagulants with warfarin.
Methods
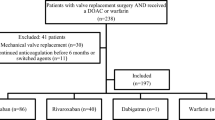
Using linked health administrative databases housed at the Institute for Clinical Evaluative Sciences, we identified consecutive patients in Ontario (Canada) 65 years of age or older with AF who underwent bioprosthetic valve replacement between 1 April 2012 and 31 March 2017. We created a time-varying Cox model to examine the relationship between the type of anticoagulant and time to thrombotic or bleeding events after adjustment for baseline risk of thrombosis using the CHA2DS2-VASc score and risk of bleeding using the HAS-BLED scores. We conducted prespecified subgroup analyses according to whether valve implantation was surgical or transcatheter.
Results
We identified 2245 eligible patients. The mean age was 79 years, 41% were female, and 39% had transcatheter aortic valve replacement. Risk of death or thrombosis was not different between direct oral anticoagulants and warfarin after adjustment for CHA2DS2-VASc score (hazard ratio [HR] 1.02, 95% confidence interval [CI], 0.83–1.25). Risk of death or bleeding was not different between direct oral anticoagulants and warfarin after adjustment for HAS-BLED score (HR 0.89, 95% CI 0.75–1.07). Subgroup analyses of surgical or transcatheter valves were consistent with overall results.
Conclusions
In a real-world population of patients with atrial fibrillation and bioprosthetic valve replacement, we found no difference between direct oral anticoagulants and warfarin with regard to the risk of thrombosis or bleeding.

Similar content being viewed by others
Data Availability
Available upon request.
Code Availability
Not applicable.
References
Kornej J, Börschel CS, Benjamin EJ, Schnabel RB. Epidemiology of atrial fibrillation in the 21st century: novel methods and new insights. Circ Res. 2020;127(1):4–20.
Heart & Stroke. Atrial fibrillation. Available from: http://www.heartandstroke.ca/heart/conditions/atrial-fibrillation. Accessed 16 March 2022
Kozieł M, Teutsch C, Bayer V, et al. Changes in anticoagulant prescription patterns over time for patients with atrial fibrillation around the world. J Arrhythm. 2021;37(4):990–1006.
Ruff CT, Giugliano RP, Braunwald E, et al. Comparison of the efficacy and safety of new oral anticoagulants with warfarin in patients with atrial fibrillation: a meta-analysis of randomised trials. Lancet. 2014;383(9921):955–62.
Thomas KL, Jackson LR 2nd, Shrader P, et al. Prevalence, characteristics, and outcomes of valvular heart disease in patients with atrial fibrillation: insights from the ORBIT-AF (outcomes registry for better informed treatment for atrial fibrillation). J Am Heart Assoc. 2017;6(12).
Banerjee A, Allan V, Denaxas S, et al. Subtypes of atrial fibrillation with concomitant valvular heart disease derived from electronic health records: phenotypes, population prevalence, trends and prognosis. Europace. 2019;21(12):1776–84.
Eikelboom JW, Connolly SJ, Brueckmann M, et al. Dabigatran versus warfarin in patients with mechanical heart valves. N Engl J Med. 2013;369(13):1206–14.
Olesen JB, Lip GY, Hansen ML, et al. Validation of risk stratification schemes for predicting stroke and thromboembolism in patients with atrial fibrillation: nationwide cohort study. BMJ. 2011;342:d124.
Pisters R, Lane DA, Nieuwlaat R, de Vos CB, Crijns HJ, Lip GY. A novel user-friendly score (HAS-BLED) to assess 1-year risk of major bleeding in patients with atrial fibrillation: the Euro Heart Survey. Chest. 2010;138(5):1093–100.
Otto CM, Nishimura RA, Bonow RO, et al. 2020 ACC/AHA guideline for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. J Am Coll Cardiol. 2021;77(4):e25–197.
Vahanian A, Beyersdorf F, Praz F, et al. 2021 ESC/EACTS Guidelines for the management of valvular heart disease. Eur Heart J. 2022;43(7):561–632.
Guimarães HP, Lopes RD, de Barros E, et al. Rivaroxaban in patients with atrial fibrillation and a bioprosthetic mitral valve. N Engl J Med. 2020;383(22):2117–26.
Afilalo J, Eisenberg MJ, Morin JF, et al. Gait speed as an incremental predictor of mortality and major morbidity in elderly patients undergoing cardiac surgery. J Am Coll Cardiol. 2010;56(20):1668–76.
Shim CY, Seo J, Kim YJ, et al. Efficacy and safety of edoxaban in patients early after surgical bioprosthetic valve implantation or valve repair: a randomized clinical trial. J Thorac Cardiovasc Surg. 2021.
Van Mieghem NM, Unverdorben M, Valgimigli M, et al. Edoxaban versus standard of care and their effects on clinical outcomes in patients having undergone transcatheter aortic valve implantation in atrial fibrillation-rationale and design of the ENVISAGE-TAVI AF trial. Am Heart J. 2018;205:63–9.
Collet JP, Van Belle E, Thiele H, et al. Apixaban vs. standard of care after transcatheter aortic valve implantation: the ATLANTIS trial. Eur Heart J. 2022.
Izumi C, Miyake M, Fujita T, et al. Antithrombotic therapy for patients with atrial fibrillation and bioprosthetic valves- real-world data from the multicenter, prospective, observational BPV-AF registry. Circ J. 2022;86(3):440–8.
Izumi C, Miyake M, Amano M, et al. Registry of antithrombotic therapy in atrial fibrillation patients with bioprosthetic valves: a retrospective observational study. J Cardiol. 2020;76(1):44–50.
Giugliano RP, Ruff CT, Braunwald E, et al. Edoxaban versus warfarin in patients with atrial fibrillation. N Engl J Med. 2013;369(22):2093–104.
Granger CB, Alexander JH, McMurray JJ, et al. Apixaban versus warfarin in patients with atrial fibrillation. N Engl J Med. 2011;365(11):981–92.
Kawashima H, Watanabe Y, Hioki H, et al. Direct oral anticoagulants versus vitamin K antagonists in patients with atrial fibrillation after TAVR. JACC Cardiovasc Interv. 2020;13(22):2587–97.
Young MN, Kearing S, Malenka D, Goodney PP, Skinner J, Iribarne A. Geographic and demographic variability in transcatheter aortic valve replacement dispersion in the United States. J Am Heart Assoc. 2021;10(12):e019588.
Ranasinghe MP, Peter K, McFadyen JD. Thromboembolic and bleeding complications in transcatheter aortic valve implantation: insights on mechanisms, prophylaxis and therapy. J Clin Med. 2019;8(2).
Funding
This study was supported by ICES, which is funded by an annual grant from the Ontario Ministry of Health (MOH) and the Ministry of Long-Term Care (MLTC).
Author information
Authors and Affiliations
Contributions
Study conception and design, all authors. Data analysis, FN and RP. Draft manuscript preparation, RE. All authors reviewed the results and approved the final version of the manuscript.
Corresponding author
Ethics declarations
This study was supported by ICES, which is funded by an annual grant from the Ontario Ministry of Health (MOH) and the Ministry of Long-Term Care (MLTC). Parts of this material are based on data and information compiled and provided by CIHI and by the Ontario MOH. The analyses, conclusions, opinions, and statements expressed herein are solely those of the authors and do not reflect those of the funding or data sources; no endorsement is intended or should be inferred. The authors acknowledge that the clinical registry data used in this manuscript is from participating hospitals through CorHealth Ontario, which serves as an advisory body to the Ministry of Health (MOH), is funded by the MOH, and is dedicated to improving the quality, efficiency, access, and equity in the delivery of the continuum of adult cardiac, vascular, and stroke services in Ontario, Canada. We thank IQVIA Solutions Canada Inc. for use of their Drug Information File.
Ethics Approval
The study was approved by the Hamilton Integrated Research Ethics Board (Hamilton, Ontario, Canada).
Consent to Participate
Individual patient consent was not required because only anonymized administrative data were interrogated.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This paper was presented at the American Association for Thoracic Surgery 102nd Annual Meeting, May 14–17, 2022, Boston, MA.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Eikelboom, R., Whitlock, R.P., Sibilio, S. et al. Direct Oral Anticoagulation Versus Warfarin in Patients with Atrial Fibrillation and Bioprosthetic Heart Valves: a Retrospective, Real-World Cohort Study. Cardiovasc Drugs Ther 38, 109–117 (2024). https://doi.org/10.1007/s10557-022-07381-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10557-022-07381-5