Abstract
Purpose
To compare the effect of ticagrelor with clopidogrel in reducing the risk of ischemic cardiovascular events in patients with late or very late stent thrombosis (LST/VLST) after primary percutaneous coronary intervention (PCI).
Methods
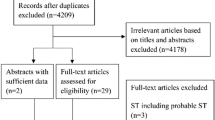
A total of 4538 patients with acute coronary syndrome were screened for angiographically determined LST/VLST. Two hundred and forty-one patients were included in the analysis and grouped according to ticagrelor (n = 81) or clopidogrel (n = 160) at discharge. The clinical outcome was major adverse cardiovascular events (MACE) defined as death, myocardial infarction (MI), ischemic stroke, and revascularization during the 1-yr follow-up period.
Results
After propensity score matching, 65 pairs were generated. The incidence of MACE was significantly lower in the ticagrelor group compared with the clopidogrel group (9.3% vs. 21.5%, log-rank p = 0.048). However, no difference was observed in event rates of death, MI, ischemic stroke, and revascularization between the ticagrelor group and the clopidogrel group.
Conclusion
Following successful primary PCI, patients with LST/VLST who received ticagrelor had fewer ischemic cardiovascular events at 1-yr follow-up, compared with those who received clopidogrel.



Similar content being viewed by others
References
Wenaweser P, Daemen J, Zwahlen M, van Domburg R, Juni P, Vaina S, et al. Incidence and correlates of drug-eluting stent thrombosis in routine clinical practice. 4-year results from a large 2-institutional cohort study. J Am Coll Cardiol. 2008;52:1134–40.
Rozemeijer R, WingWong C, Leenders G, Timmers L, Koudstaal S, Rittersma SZ, et al. Incidence, angiographic and clinical predictors, and impact of stent thrombosis: a 6-year survey of 6,545 consecutive patients. Neth Heart J. 2019;27:321–9.
Ergelen M, Gorgulu S, Uyarel H, Norgaz T, Aksu H, Ayhan E, et al. The outcome of primary percutaneous coronary intervention for stent thrombosis causing ST-elevation myocardial infarction. Am Heart J. 2010;159:672–6.
Levine GN, Bates ER, Bittl JA, et al. 2016 ACC/AHA guideline focused update on duration of dual antiplatelet therapy in patients with coronary artery disease: a report of the American College of Cardiology/American Heart Association task force on clinical practice guidelines. J Am Coll Cardiol. 2016;68:1082–115.
Neumann FJ, Sousa-Uva M, Ahlsson A, Alfonso F, Banning AP, Benedetto U, et al. 2018 ESC/EACTS guidelines on myocardial revascularization. Eur Heart J. 2019;40:87–5.
von Elm E, Altman D, Egger M, Pocock S, Gøtzsche P, Vandenbroucke J, et al. Strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. BMJ. 2007;20:806–8.
Levine GN, Bates ER, Blankenship JC, Bailey SR, Bittl JA, Cercek B, et al. 2011 ACCF/AHA/SCAI guideline for percutaneous coronary intervention. A report of the American College of Cardiology Foundation/American Heart Association task force on practice guidelines and the Society for Cardiovascular Angiography and Interventions. J Am Coll Cardiol. 2011;58:e44–2.
Thygesen K, Alpert JS, Jaffe AS, Chaitman BR, Bax JJ, Morrow DA, et al. Fourth universal definition of myocardial infarction (2018). Circulation. 2018;138:e618–1.
Armstrong EJ, Feldman DN, Wang TY, Kaltenbach LA, Yeo KK, Wong SC, et al. Clinical presentation, management, and outcomes of angiographically documented early, late, and very late stent thrombosis. JACC Cardiovasc Interv. 2012;5:131–0.
Dangas GD, Claessen BE, Mehran R, Brener S, Brodie BR, Dudek ED, et al. Clinical outcomes following stent thrombosis occurring in-hospital versus out-of-hospital: results from the HORIZONS-AMI (harmonizing outcomes with revascularization and stents in acute myocardial infarction) trial. J Am Coll Cardiol. 2012;59:1752–9.
Xi Z, Zhou Y, Zhao Y, Liu X, Liang J, Chai M, et al. Ticagrelor versus clopidogrel in patients with two CYP2C19 loss-of-function alleles undergoing percutaneous coronary intervention. Cardiovasc Drugs Ther. 2020;34:179–8
Klein MD, Lee CR, Stouffer GA. Clinical outcomes of CYP2C19 genotype-guided antiplatelet therapy: existing evidence and future directions. Pharmacogenomics. 2018;19:1039–6.
Martin J, Williams AK, Klein MD, Sriramoju VB, Madan S, Rossi JS, et al. Frequency and clinical outcomes of CYP2C19 genotype-guided escalation and de-escalation of antiplatelet therapy in a real-world clinical setting. Genet Med. 2020;22:160–9.
Sibbing D, Aradi D, Alexopoulos D, TenBerg J, Bhatt DL, Bonello L, et al. Updated expert consensus statement on platelet function and genetic testing for guiding P2Y12 receptor inhibitor treatment in percutaneous coronary intervention. JACC Cardiovasc Interv. 2019;12:1521–7.
Boden WE, O'Rourke RA, Teo KK, Hartigan PM, Maron DJ, Kostuk WJ, et al. Optimal medical therapy with or without PCI for stable coronary disease. N Engl J Med. 2007;356:1503–6.
Bansilal S, Bonaca MP, Cornel JH, Storey RF, Bhatt DL, Steg PG, et al. Ticagrelor for secondary prevention of atherothrombotic events in patients with multivessel coronary disease. J Am Coll Cardiol. 2018;71:489–6.
Bhatt DL, Bonaca MP, Bansilal S, Angiolillo DJ, Cohen M, Storey RF et al. Reduction in ischemic events with ticagrelor in diabetic patients with prior myocardial infarction in PEGASUS–TIMI 54. J Am Coll Cardiol. 2016;67:2732–0.
Filippo OD, D’Ascenzo F, Raposeiras-Roubin S, Abu-Assi E, Peyracchia M, Bocchino PP, et al. P2Y12 inhibitors in acute coronary syndrome patients with renal dysfunction: an analysis from the RENAMI and BleeMACS projects. Eur Heart J Cardiovasc Pharmacother. 2019;6:31–2.
Almalla M, Schröder J, Hennings V, Marx N, Hoffmann R. Long-term outcome after angiographically proven coronary stent thrombosis. Am J Cardiol. 2013;111:1289–4.
Bonaca MP, Bhatt DL, Steg G, Storey RF, Cohen M, Im K, et al. Ischaemic risk and efficacy of ticagrelor in relation to time from P2Y12 inhibitor withdrawal in patients with prior myocardial infarction: insights from PEGASUS-TIMI 54. Eur Heart J. 2016;37:1133–2.
Acknowledgements
We thank Yang Wang, MSc, from the Medical Research and Biometrics Center, National Center for Cardiovascular Diseases, for his professional suggestions regarding statistical analyses.
Funding
This research was supported by the Chinese Academy of Medical Sciences Innovation Fund for Medical Sciences (No. 2016-I2M-1-009) and the National Natural Science Foundation of China (No. 81970308).
Author information
Authors and Affiliations
Contributions
Hongbing Yan, Li Song, and Hanjun Zhao contributed to the study conception and design. Material preparation was performed by Yu Tan, Chen Liu, and Peng Zhou. Data collection was performed by Zhaoxue Sheng, Jiannan Li, and Runzhen Chen. Analysis was performed by Jinying Zhou. The first draft of the manuscript was written by Jinying Zhou and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Ethics Approval
This is an observational study. The Review Board of Fuwai Hospital has confirmed that no ethical approval is required.
Data Availability
The datasets used and/or analyzed during this study are available from the corresponding author on reasonable request.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhou, J., Tan, Y., Liu, C. et al. Ticagrelor Versus Clopidogrel in Patients with Late or Very Late Stent Thrombosis. Cardiovasc Drugs Ther 34, 677–684 (2020). https://doi.org/10.1007/s10557-020-07021-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10557-020-07021-w