Summary
Aim of the study: To assess whether variations in antioxidant and anti-inflammatory parameters occur with short term administration and discontinuation of atorvastatin in normocholesterolemic coronary artery disease (CAD) patients.
Methods: Forty CAD patients with near normal serum cholesterol levels (total cholesterol <240 mg/dl, LDL cholesterol <130 mg/dl) were continuously enrolled and randomized to groups A & B (20 patients taking atorvastatin) and groups C & D (20 patients not taking atorvastatin). Atorvastatin (10 mg/day) was continued in group A, withdrawn in group B and started in groups C & D for 6 weeks. Thereafter atorvastatin was withdrawn in group A and C, restarted in group B, and continued in group D for further 6 weeks. CRP, FRAP and TBARS were assessed at baseline, 6 weeks and 12 weeks in all the groups.
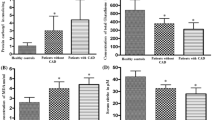
Results: Baseline CRP, TBARS and FRAP levels were significantly different (p < 0.05) between groups A & B and C & D at the time of enrollment, indicating lower levels of oxidative stress (FRAP—172.40 ± 23.41 nmol Fe2+/l vs 142.62 ± 15.73 nmol Fe2+/l and TBARS—3.66 ± 1.14 nmol/ml vs 6.11 ± 1.85 nmol/ml) and low grade inflammation (CRP—1.38 ± 0.69 mg/l vs 3.19 ± 1.77 mg/l) in statin treated groups. In group B, discontinuation resulted in increase in CRP (2.87 ± 0.98 mg/l) and TBARS (5.75 ± 1.35 nmol/ml) and decrease in FRAP (133.132 ± 13.32 nmol Fe2+/l) and whereas group A patients did not show significant variation in values compared to baseline (CRP—1.36 ± 0.33 mg/l, FRAP—155.45 ± 19.51 and TBARS—4.22 ± 0.81). Administration of atorvastatin caused a marked reduction in oxidative stress and inflammation in groups C & D (CRP—1.13 ± 0.99 mg/l & 1.73 ± 1.60 mg/l, FRAP—166.54 ± 34.11 & 177.44 ± 13.31 nmol Fe2+/l, TBARS—4.66 ± 2.33 & 3.55 ± 1.25 nmol/ml respectively). The values returned to pretreatment levels on discontinuation of the drug in group C (CRP—2.61 ± 1.28 mg/l, FRAP—138.49 ± 19.62 nmol Fe2+/l, TBARS—6.13 ± 0.74 nmol/ml) whereas the decline was maintained in group D (CRP—1.62 ± 1.48 mg/l, FRAP—173.07 ± 9.03 nmol Fe2+/l, TBARS—3.75 ± 1.03 nmol/ml).
Conclusion: Administration and withdrawal of atorvastatin caused changes in markers of oxidative stress which closely correlated with changes in marker of inflammation. Further, the salutary effects were of quick onset, but were rapidly reversed on withdrawal of atorvastatin.
Similar content being viewed by others
References
Ross R. Atherosclerosis—an inflammatory disease. N Engl J Med 1999;340:115–23.
Ridker PM, Cannon CP, Morrow D, et al. C-reactive protein levels and outcomes after statin therapy. Pravastatin or Atorvastatin Evaluation and Infection Therapy-Thrombolysis in Myocardial Infarction 22 (PROVE IT-TIMI 22). N Engl J Med 2005;352:20–28.
Steinberg D, Parthasarathy S, Carew TE, Khoo JC, Witztum JL. Beyond cholesterol. Modifications of low-density lipoprotein that increase its atherogenicity. N Engl J Med 1989;320:915–924.
Russwurm S, Krause S, Finkelberg L, Ruhling K, Schauer U, Losche W. Generation of reactive oxygen species and activity of platelet-activating factor acetylhydrolase in human monocyte-derived macrophages. Thromb Res 1994;74:505–514.
Jialal I, Devaraj S, Venugopal SK. C-reactive protein: Risk marker or mediator in atherothrombosis? Hypertension 2004;44:6–11.
Khuseyinova N, Imhof A, Trischler G, et al. Determination of C-reactive protein: Comparison of three high-sensitivity immunoassays. Clin Chem 2003;49:1691–1695.
Albert MA, Danielson E, Rifai N, Ridker PM. PRINCE Investigators. Effect of statin therapy on C-reactive protein levels: The pravastatin inflammation/CRP evaluation (PRINCE): A randomized trial and cohort study. JAMA 2001;286:64–70.
Downs JR, Clearfield M, Weis S, et al. Primary prevention of acute coronary events with lovastatin in men and women with average cholesterol levels: Results of AFCAPS/TexCAPS. Air Force/Texas Coronary Atherosclerosis Prevention Study. JAMA 1998;279:1615–1622.
Karatzis E, Lekakis J, Papamichael C, et al. Rapid effect of pravastatin on endothelial function and lipid peroxidation in unstable angina. Int J Cardiol 2005;101:65–70.
Schwartz GG, Olsson AG, Ezekowitz, et al. Effects of atorvastatin on early recurrent ischemic events in acute coronary syndromes: The MIRACL study: A randomized controlled trial. Myocardial Ischemia Reduction with Aggressive Cholesterol Lowering (MIRACL) Study Investigators. JAMA 2001;285:1711–1718.
Heeschen C, Hamm CW, Laufs U, Snapinn S, Bohm M, White HD. Platelet Receptor Inhibition in Ischemic Syndrome Management (PRISM) Investigators. Withdrawal of statins increases event rates in patients with acute coronary syndromes. Circulation 2002;105:1446–1452.
Laufs U, Wassmann S, Hilgers S, Ribaudo N, Bohm M, Nickenig G. Rapid effects on vascular function after initiation and withdrawal of atorvastatin in healthy, normocholesterolemic men. Am J Cardiol 2001;88:1306–1307.
Ridker PM, Rifai N, Pfeffer MA, et al. Long-term effects of pravastatin on plasma concentration of C-creative protein. The Cholesterol and Recurrent Events (CARE) Investigators. Circulation 1999;100:230–235.
Ohkawa H, Ohishi N, Yogi K. Assay of lipid peroxidase in animal tissues by thiobarbituric acid reaction 1979. Anal Biochem 1979;95:351–358.
Benzie IFF, Strain JJ. Ferric Reducing Ability of Plasma (FRAP) as a measure of “Antioxidant Power”: The FRAP assay. Anal Biochem 1996;239:70–76.
Ledue TB, Weiner DL, Sipe J, Poulin SE, Collins MF, Rifai N. Analytical evaluation of particle-enhanced immunonephelometric assays for C-reactive protein, serum amyloid A, and mannose binding protein in human serum. Ann Clin Biochem 1998;35:745–753.
Lopes HF, Martin KL, Nashar K, Morrow JD, Goodfriend TL, Egan BM. DASH diet lowers blood pressure and lipid-induced oxidative stress in obesity. Hypertension 2003r;41:422–430.
Vassalle C, Masini S, Carpeggiani C, L’Abbate A, Boni C, Zucchelli GC. In vivo total antioxidant capacity: Comparison of two different analytical methods. Clin Chem Lab Med 2004;42:84–89.
Sanguigni V, Pignatelli P, Caccese D, et al. Atorvastatin decreases superoxide anion production in hypercholesterolemic patients. Eur Heart J 2002;4:372.
John D, Peter W, Mary W, et al. Low Grade inflammation and coronary heart disease: Prospective study and updated meta-analysis. BMJ 2000;321:199–204.
James HB, Patrocia AH, Patrick MM. Role of C Reactive protein in cardiovascular disease. Ann Pharmacother 2004;38:110–118.
Cai H, Harrison DG. Endothelial dysfunction in cardiovascular diseases: The role of oxidant stress. Circ Res 2000;87:840–844.
Ulf L, David GH. Oxidant stress as a marker for cardiovascular events. Circulation 2001;104:2638.
Macy EM, Hayes TE, Tracy RP. Variability in the measurement of C-reactive protein in healthy subjects: Implications for reference intervals and epidemiological applications. Clin Chem 1997;43:52–58.
Ridker PM, Cushman M, Stampfer MJ, et al. Inflammation, aspirin, and the risk of cardiovascular disease in apparently healthy men. N Engl J Med 1997;336(14):973–979.
Karen EJ, Wendy AG, Vic H, et al. Effect of Angiotensin-converting Enzyme Inhibitors, Beta Blockers, Statins, and Aspirin on C-reactive protein Levels in Outpatients with Heart Failure. Am J Cardiol 2004;93:783–785.
Stroes ES, Koomans HA, de Bruin TW, Rabelink TJ. Vascular function in the forearm of hypercholesterolaemic patients off and on lipid-lowering medication. Lancet 1995;346:467–471.
Scandinavian Simvastatin Survival Study Group. Randomized trial of cholesterol lowering in 4444 patients with coronary heart disease: The Scandinavian Simvastatin Survival Study (45). Lancet 1994;344:1383–1389.
Sacks FM, Pfeffer MA, Moya LA, et al. The effect of pravastatin on coronary events after myocardial infarction in patients with average cholesterol levels. Cholesterol and Recurrent Events (CARE) Trial investigators. N Engl J Med 1996;335:1001–1009.
Riesen WF, Engler H, Risch M, Korte W, Noseda G. Short-term effects of atorvastatin on C-reactive protein. Eur Heart J 2002;23:794–799.
Laufs U, La Fata V, Plutzky J, Liao JK. Upregulation of endothelial nitric oxide synthase by HMG CoA reductase inhibitors. Circulation 1998;97:1129–1135.
Landmesser U, Bahlmann F, Mueller M, et al. Simvastatin versus ezetimibe: Pleiotropic and lipid-lowering effects on endothelial function in humans. Circulation 2005;111:2356–2363.
Raffaele De C, Francesco C, Francesca Paola F, et al. Low Density Lipoprotein level reduction by the 3-Hydroxy-3-Methyglutaryl Coenzyme-A Inihibior Simavastatin is accompanied by a related reduction of F2-Isoprostane formation in hypercholesterolemic subjects. No further effect of Vitamin E. Circulation 2002;106:2543–2549.
Jula A, Marniemi J, Huupponen R, Virtanen A, et al. Effects of diet and simvastatin on serum lipids, insulin, and antioxidants in hypercholesterolemic men: A randomized controlled trial. JAMA 2002;287:598–605.
Brown B.G., X.Q. Zhao, Chait A., et al. Simvastain and niacin, antioxidant vitamins, or the combination for the prevention of coronary disease. N Eng J Med 2001;345:1583–1591.
Tall AR. C-reactive protein reassessed. N Engl J Med 2004;350:1450–1452.
Ornish D, Brown SE, Scherwtz LW, et al. Can lifestyle changes reverse coronary heart disease? Lancet 1990;336:129–133.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Thomas, M.K., Narang, D., Lakshmy, R. et al. Correlation Between Inflammation and Oxidative Stress in Normocholesterolemic Coronary Artery Disease Patients ‘on’ and ‘off’ Atorvastatin for Short Time Intervals. Cardiovasc Drugs Ther 20, 37–44 (2006). https://doi.org/10.1007/s10557-006-6752-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10557-006-6752-x