Abstract
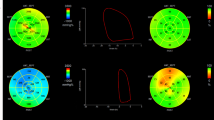
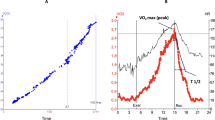
COVID-19 may have residual consequences in multiple organs, including the cardiovascular system. The purpose of the present investigation is to quantify myocardial function in symptomatic individuals with long COVID and investigate the association between illness severity and myocardial function. A retrospective cross-sectional study was conducted in which symptomatic individuals with previous COVID-19 underwent echocardiographic analysis of left ventricle global longitudinal strain (LVGLS) and myocardial work (MW). Individuals also performed cardiopulmonary testing (CPX) to assess peak oxygen uptake (VO2peak). Differences between illness severity subgroups were analyzed by the Mann–Whitney test. Correlations were calculated using the Spearman correlation test. Multilinear regressions were performed to evaluate the influences of COVID-19 severity, body mass index, age, and sex on MW. Fifty-six individuals were included (critical subgroup: 17; moderate/severe subgroup: 39), 59% females; median age: 56 years (IQR: 43–63). CPX revealed a substantial reduction in VO2peak (median of 53% of predicted values). LVGLS were not statistically different between subgroups. Global wasted work (GWW) was higher in the critical subgroup [146 (104–212) versus 121 (74–163) mmHg%, p = 0.01], and global work efficiency (GWE) was lower in this subgroup [93 (91–95) versus 94 (93–96), p = 0.03]. Illness severity was the only independent predictor of GWW and GWE (GWW: r2 = 0.167; p = 0.009; GWE: r2 = 0.172; p = 0.005) in multilinear regressions. In our study with long COVID-19 individuals, despite having a similar LVGLS, patients had subclinical LV dysfunction, demonstrated only by an increase in GWW and a decrease in GWE.
Graphical abstract




Similar content being viewed by others
Data availability
The data supporting this article are available in the article and can be shared upon reasonable request to the corresponding author (A).
References
Han E, Tan MMJ, Turk E, Sridhar D, Leung GM, Shibuya K et al (2020) Lessons learnt from easing COVID-19 restrictions: an analysis of countries and regions in Asia Pacific and Europe. Lancet 396(10261):1525–1534
Zhou P, Yang XL, Wang XG, Hu B, Zhang L, Zhang W et al (2020) A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 579(7798):270–273
Gupta A, Madhavan MV, Sehgal K, Nair N, Mahajan S, Sehrawat TS et al (2020) Extrapulmonary manifestations of COVID-19. Nat Med 26(7):1017–1032
Madjid M, Safavi-Naeini P, Solomon SD, Vardeny O (2020) Potential effects of coronaviruses on the cardiovascular system: a review. JAMA Cardiol 5(7):831–840
Nishiga M, Wang DW, Han Y, Lewis DB, Wu JC (2020) COVID-19 and cardiovascular disease: from basic mechanisms to clinical perspectives. Nat Rev Cardiol 17(9):543–558
Driggin E, Madhavan MV, Bikdeli B, Chuich T, Laracy J, Biondi-Zoccai G et al (2020) Cardiovascular considerations for patients, health care workers, and health systems during the COVID-19 pandemic. J Am Coll Cardiol 75(18):2352–2371
Milani M, Milani JGPO, Cipriano GFB, Cahalin LP, Stein R, Cipriano Jr. G. Cardiopulmonary Exercise Testing in Post-COVID-19 Patients: Where Does Exercise Intolerance Come From? Arquivos Brasileiros de Cardiologia 120(2) https://doi.org/10.36660/abc.20220150
Szekely Y, Lichter Y, Taieb P, Banai A, Hochstadt A, Merdler I et al (2020) Spectrum of cardiac manifestations in COVID-19: a systematic echocardiographic study. Circulation 142(4):342–353
Rey JR, Caro-Codon J, Rosillo SO, Iniesta AM, Castrejon-Castrejon S, Marco-Clement I et al (2020) Heart failure in COVID-19 patients: prevalence, incidence and prognostic implications. Eur J Heart Fail 22(12):2205–2215
Carfi A, Bernabei R, Landi F (2020) Gemelli against C-P-ACSG persistent symptoms in patients after acute COVID. JAMA 324(6):603–605
Huang C, Huang L, Wang Y, Li X, Ren L, Gu X et al (2021) 6-month consequences of COVID-19 in patients discharged from hospital: a cohort study. Lancet 397(10270):220–232
Puntmann VO, Carerj ML, Wieters I, Fahim M, Arendt C, Hoffmann J et al (2020) Outcomes of Cardiovascular Magnetic Resonance Imaging in Patients Recently Recovered From Coronavirus Disease 2019 (COVID-19). JAMA Cardiol 5(11):1265–1273
Rajpal S, Tong MS, Borchers J, Zareba KM, Obarski TP, Simonetti OP et al (2021) Cardiovascular magnetic resonance findings in competitive athletes recovering from COVID-19 infection. JAMA Cardiol 6(1):116–118
Kotecha T, Knight DS, Razvi Y, Kumar K, Vimalesvaran K, Thornton G et al (2021) Patterns of myocardial injury in recovered troponin-positive COVID-19 patients assessed by cardiovascular magnetic resonance. Eur Heart J 42(19):1866–1878
Moody WE, Liu B, Mahmoud-Elsayed HM, Senior J, Lalla SS, Khan-Kheil AM et al (2021) Persisting adverse ventricular remodeling in COVID-19 survivors: a longitudinal echocardiographic study. J Am Soc Echocardiogr 34(5):562–566
Tryfou ES, Kostakou PM, Chasikidis CG, Kostopoulos VS, Serafetinidis II, Ferdianaki EK et al (2021) Biventricular myocardial function in Covid-19 recovered patients assessed by speckle tracking echocardiography: a prospective cohort echocardiography study. Int J Cardiovasc Imaging 38(5):995–1003
Herrmann J, Lenihan D, Armenian S, Barac A, Blaes A, Cardinale D et al (2022) Defining cardiovascular toxicities of cancer therapies: an International Cardio-Oncology Society (IC-OS) consensus statement. Eur Heart J 43(4):280–299
Laufer-Perl M, Arnold JH, Mor L, Amrami N, Derakhshesh M, Moshkovits Y et al (2020) The association of reduced global longitudinal strain with cancer therapy-related cardiac dysfunction among patients receiving cancer therapy. Clin Res Cardiol 109(2):255–262
Houard L, Benaets MB et al (2019) Additional prognostic value of 2d right ventricular speckle-tracking strain for prediction of survival in heart failure and reduced ejection fraction: a comparative study with cardiac magnetic resonance. JACC Cardiovasc Imaging. 12(12):2373–2385
Russell K, Eriksen M, Aaberge L, Wilhelmsen N, Skulstad H, Remme EW et al (2012) A novel clinical method for quantification of regional left ventricular pressure-strain loop area: a non-invasive index of myocardial work. Eur Heart J 33(6):724–733
Russell K, Eriksen M, Aaberge L, Wilhelmsen N, Skulstad H, Gjesdal O et al (2013) Assessment of wasted myocardial work: a novel method to quantify energy loss due to uncoordinated left ventricular contractions. Am J Physiol Heart Circ Physiol 305(7):H996-1003
Roemer S, Jaglan A, Santos D, Umland M, Jain R, Tajik AJ et al (2021) The utility of myocardial work in clinical practice. J Am Soc Echocardiogr 34(8):807–818
COVID-19 Treatment Guidelines Panel. Coronavirus Disease 2019 (COVID-19) Treatment Guidelines. [Internet]. 2022 [cited https://www.covid19treatmentguidelines.nih.gov].
A clinical case definition of post COVID-19 condition by a Delphi consensus [Internet]. 2021 [cited WHO/2019-nCoV/Post_COVID-19_condition/Clinical_case_definition/2021.1].
Raveendran AV, Jayadevan R, Sashidharan S (2021) Long COVID: an overview. Diabetes Metab Syndr 15(3):869–875
Balady GJ, Arena R, Sietsema K, Myers J, Coke L, Fletcher GF et al (2010) Clinician’s guide to cardiopulmonary exercise testing in adults: a scientific statement from the American Heart Association. Circulation 122(2):191–225
Herdy AH, Ritt LE, Stein R, Araujo CG, Milani M, Meneghelo RS et al (2016) Cardiopulmonary exercise test: background, applicability and interpretation. Arq Bras Cardiol 107(5):467–481
Meneghelo RSAC, Stein R, Mastrocolla LE, Albuquerque PF, Serra SM et al (2010) III Diretrizes da Sociedade Brasileira de Cardiologia Sobre Teste Ergométrico. Arq Bras Cardiol 95(5):1–26
Juliana Goulart Prata Oliveira, Milani Mauricio, Milani Graziella França Bernardelli, Cipriano Isac, de Castro Dominique, Hansen Gerson, Cipriano Junior (2023) Oxygen Uptake Efficiency Slope in South American Healthy Adults Journal of Cardiopulmonary Rehabilitation and Prevention 43(4) 290–300 https://doi.org/10.1097/hcr.0000000000000778
ReizoBaba M, Nagashima M, Goto M, Nagano Y, Yokota M, Tauchi N, Nishibata K (1996) Oxygen Uptake Efficjenq’ Slop’e: A ‘New Index of Cardiorespiratory, FuntitJonal reserve derived from the relation between oxygen uptake and minute ventilation during incremental exercise. J Am College Cardiol 28:1567–1572
Milani M, Milani J, Cipriano GFB, de Castro I, Cipriano JG (2022) Reference standards for cardiorespiratory fitness in Brazil: A Pooled Analysis And Overview Of Heterogeneity In National And International Studies. J Cardiopulm Rehabil Prev 42(5):366–372
Hirofumi Tanaka P, Monahan KD, Seals DR (2001) Age-predicted maximal heart rate revisited. J Am College Cardiol 37:153–156
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L et al (2015) Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging 16(3):233–270
Nagueh SF, Smiseth OA, Appleton CP, Byrd BF 3rd, Dokainish H, Edvardsen T et al (2016) Recommendations for the evaluation of left ventricular diastolic function by echocardiography: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr 29(4):277–314
Voigt JU, Pedrizzetti G, Lysyansky P, Marwick TH, Houle H, Baumann R et al (2015) Definitions for a common standard for 2D speckle tracking echocardiography: consensus document of the EACVI/ASE/Industry Task Force to standardize deformation imaging. Eur Heart J Cardiovasc Imaging 16(1):1–11
Badano LP, Kolias TJ, Muraru D, Abraham TP, Aurigemma G, Edvardsen T et al (2018) Standardization of left atrial, right ventricular, and right atrial deformation imaging using two-dimensional speckle tracking echocardiography: a consensus document of the EACVI/ASE/Industry Task Force to standardize deformation imaging. Eur Heart J Cardiovasc Imaging 19(6):591–600
Papadopoulos K, OzdenTok O, Mitrousi K, Ikonomidis I (2021) Myocardial work: methodology and clinical applications. Diagnostics 11:3
Manganaro R, Marchetta S, Dulgheru R, Ilardi F, Sugimoto T, Robinet S et al (2019) Echocardiographic reference ranges for normal non-invasive myocardial work indices: results from the EACVI NORRE study. Eur Heart J Cardiovasc Imaging 20(5):582–590
Raman B, Bluemke DA, Luscher TF, Neubauer S (2022) Long COVID: post-acute sequelae of COVID-19 with a cardiovascular focus. Eur Heart J 43(11):1157–1172
Singh I, Joseph P, Heerdt PM, Cullinan M, Lutchmansingh DD, Gulati M et al (2022) Persistent exertional intolerance after covid-19: insights from invasive cardiopulmonary exercise testing. Chest 161(1):54–63
Baratto C, Caravita S, Faini A, Perego GB, Senni M, Badano LP et al (2021) Impact of COVID-19 on exercise pathophysiology: a combined cardiopulmonary and echocardiographic exercise study. J Appl Physiol 130(5):1470–1478
Minhas AS, Gilotra NA, Goerlich E, Metkus T, Garibaldi BT, Sharma G et al (2021) Myocardial work efficiency, a novel measure of myocardial dysfunction, is reduced in covid-19 patients and associated with in-hospital mortality. Front Cardiovasc Med 8:667721
Mahajan S, Kunal S, Shah B, Garg S, Palleda GM, Bansal A et al (2021) Left ventricular global longitudinal strain in COVID-19 recovered patients. Echocardiography 38(10):1722–1730
Sorensen J, Harms HJ, Aalen JM, Baron T, Smiseth OA, Flachskampf FA (2020) Myocardial efficiency: a fundamental physiological concept on the verge of clinical impact. JACC Cardiovasc Imaging 13(7):1564–1576
Lairez O, Blanchard V, Houard V, Vardon-Bounes F, Lemasle M, Cariou E et al (2021) Cardiac imaging phenotype in patients with coronavirus disease 2019 (COVID-19): results of the cocarde study. Int J Cardiovasc Imaging 37(2):449–457
Luchian ML, Motoc A, Lochy S, Magne J, Belsack D, De Mey J et al (2021) Subclinical myocardial dysfunction in patients with persistent dyspnea one year after covid-19. Diagnostics 12(1):57
Cui C, Li Y, Liu Y, Huang D, Hu Y, Wang Y et al (2021) Association between echocardiographic non-invasive myocardial work indices and myocardial fibrosis in patients with dilated cardiomyopathy. Front Cardiovasc Med 8:704251
Petrilli CM, Jones SA, Yang J, Rajagopalan H, O’Donnell L, Chernyak Y et al (2020) Factors associated with hospital admission and critical illness among 5279 people with coronavirus disease 2019 in New York City: prospective cohort study. BMJ 369:m1966
Gupta S, Hayek SS, Wang W, Chan L, Mathews KS, Melamed ML et al (2020) Factors associated with death in critically ill patients with coronavirus disease 2019 in the US. JAMA Intern Med 180(11):1436–1447
Clark A, Jit M, Warren-Gash C, Guthrie B, Wang HHX, Mercer SW et al (2020) Global, regional, and national estimates of the population at increased risk of severe COVID-19 due to underlying health conditions in 2020: a modelling study. Lancet Glob Health 8(8):e1003–e1017
Sharma J, Rajput R, Bhatia M, Arora P, Sood V (2021) Clinical predictors of covid-19 severity and mortality: a perspective. Front Cell Infect Microbiol 11:674277
Morbach C, Sahiti F, Tiffe T, Cejka V, Eichner FA, Gelbrich G et al (2020) Myocardial work - correlation patterns and reference values from the population-based STAAB cohort study. PLoS ONE 15(10):e0239684
Sahiti F, Morbach C, Cejka V, Tiffe T, Wagner M, Eichner FA et al (2022) Impact of cardiovascular risk factors on myocardial work-insights from the STAAB cohort study. J Hum Hypertens 36(3):235–245
Foldi M, Farkas N, Kiss S, Zadori N, Vancsa S, Szako L et al (2020) Obesity is a risk factor for developing critical condition in COVID-19 patients: a systematic review and meta-analysis. Obes Rev 21(10):e13095
Kass DA, Duggal P, Cingolani O (2020) Obesity could shift severe COVID-19 disease to younger ages. Lancet 395(10236):1544–1545
Acknowledgements
We would like to thank the laboratory staff, the University of Brasilia, primary physicians, and other health professionals who referred patients for CPET assessment.
Funding
This study was funded in part by Brazilian public research grants and scholarships from Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq [National Council of Scientific and Technological Development]) (author H),Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES [Coordination for the Advancement of Higher Education Personnel]) (authors B and E) and Fundação de Apoio à Pesquisa do Distrito Federal (FAPDF [Federal District Research Support Foundation] (author H). There were also fundings from the Special Research Fund (BOF) from Hasselt University, Belgium (Number: BOF23DOCBL10 and BOF23KV10).
Author information
Authors and Affiliations
Contributions
LBOD (A): conception and design, acquisition of data, analysis and interpretation of the results, drafted the article; MM (B): conception and design, interpretation of data, analysis and interpretation of the results revised it critically, supervision; DLB (C): conception and design, acquisition of data, analysis and interpretation of the results, revised it critically; ACGBL(D): conception and design, revised it critically; JGPOM(E): conception and design, revised it critically;GFBC (F): conception and design, revised it critically; VZMS(G): conception and design, interpretation of data, analysis and interpretation of the results revised it critically; GCJ(H): conception and design, analysis and interpretation of data, revised it critically, supervision. All authors gave final approval of the version to be published and agreed to be responsible for all aspects of the research.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to disclose. There is no relationship with the industry.
Ethical approval
This study received approval from the Human Research Ethics Committee (certificate number: 56994822.5.0000.809) (Supplementary File S1).
Consent to participate
Written informed consent was obtained from all participants (Supplementary File S2).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
D’Ávila, L.B.O., Milani, M., Le Bihan, D.C.S. et al. Longitudinal strain and myocardial work in symptomatic patients having recovered from COVID-19 and possible associations with the severity of the disease. Int J Cardiovasc Imaging 40, 745–756 (2024). https://doi.org/10.1007/s10554-023-03042-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-023-03042-2