Abstract
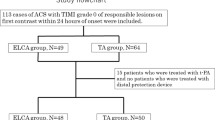
Clinical outcomes concerning the efficacy of excimer laser coronary angioplasty (ELCA) in real-world cases of acute myocardial infarction (MI) are limited. We evaluated and compared the impact of ELCA with manual aspiration thrombectomy on myocardial salvage and left ventricular (LV) systolic/diastolic function in patients with ST-segment elevation MI (STEMI) using nuclear scintigraphy. We enrolled 143 consecutive patients with STEMI treated with ELCA (63 patients) or manual aspiration thrombectomy (80 patients) between September 2016 and December 2020 in a single-center hospital. We evaluated the peak creatine kinase (CK)/ creatine kinase-myocardial band (CK-MB) levels and performed single-photon emission computed tomography (SPECT) analyses with Quantitative Gated SPECT and Quantitative Perfusion SPECT (Auto QUANT 7.2) at 3–10 days using 123I-BMIPP and 3 months following percutaneous coronary intervention using 99mTc-tetrofosmin to evaluate myocardial salvage and LV systolic/diastolic function. No significant difference was observed in the patient and periprocedural characteristics. Peak CK-MB level was significantly different between the groups (ELCA group, 190.0 [70.5–342.0] IU/L vs. aspiration group, 256.5 [157.0–354.8] IU/L, p = 0.047). Although no significant difference was observed in myocardial salvage, significant improvement in the LV ejection fraction (14.1 [6.2–19.8]% vs. 9.5 [3.9–15.3]%, respectively, p = 0.018) and peak emptying rate (-0.54 [-1.02– (-0.27)] mL/s vs. -0.38 [-0.76– (-0.05)] mL/s, respectively, p = 0.017) were detected. ELCA could suppress the myocardial deviation enzymes and potentially improve systolic function compared to manual aspiration thrombectomy in patients with STEMI.




Similar content being viewed by others
Data availability
The deidentified participant data will be shared on a request basis. Kindly directly contact the corresponding author to request data sharing. All the analyzable datasets related to the study, study protocol, and statistical analysis plan will be made available. The data will become available immediately following publication, ending a year after the publication. For any purpose, the data will be shared as Excel files via E-mail.
References
Kimura K, Kimura T, Ishihara M, Nakagawa Y, Nakao K, Miyauchi K et al (2019) JCS 2018 guideline on diagnosis and treatment of acute coronary syndrome. Circ J 83:1085–1196. https://doi.org/10.1253/circj.CJ-19-0133
Morishima I, Sone T, Okumura K, Tsuboi H, Kondo J, Mukawa H et al (2000) Angiographic no-reflow phenomenon as a predictor of adverse long-term outcome in patients treated with percutaneous transluminal coronary angioplasty for first acute myocardial infarction. J Am Coll Cardiol 36:1202–1209. https://doi.org/10.1016/s0735-1097(00)00865-2
Morishima I, Sone T, Mokuno S, Taga S, Shimauchi A, Oki Y, Kondo J, Tsuboi H, Sassa H (1995) Clinical significance of no-reflow phenomenon observed on angiography after successful treatment of acute myocardial infarction with percutaneous transluminal coronary angioplasty. Am Heart J 130:239–243. https://doi.org/10.1016/0002-8703(95)90434-4
De Luca G, Ernst N, Zijlstra F, van ’t Hof AWJ, Hoorntje JCA, Dambrink JH et al (2004) Preprocedural TIMI flow and mortality in patients with acute myocardial infarction treated by primary angioplasty. J Am Coll Cardiol 43:1363–1367. https://doi.org/10.1016/j.jacc.2003.11.042
Ikari Y, Sakurada M, Kozuma K, Kawano S, Katsuki T, Kimura K et al (2008) Upfront thrombus aspiration in primary coronary intervention for patients with ST-segment elevation acute myocardial infarction: report of the VAMPIRE (VAcuuM asPIration thrombus REmoval) trial. JACC Cardiovasc Interv 1:424–431. https://doi.org/10.1016/j.jcin.2008.06.004
Jolly SS, James S, Džavík V, Cairns JA, Mahmoud KD, Zijlstra F et al (2017) Thrombus aspiration in ST-segment-elevation myocardial infarction: an individual patient meta-analysis: thrombectomy trialists collaboration. Circulation 135:143–152. https://doi.org/10.1161/CIRCULATIONAHA.116.025371
Elgendy IY, Huo T, Bhatt DL, Bavry AA (2015) Is aspiration thrombectomy beneficial in patients undergoing primary percutaneous coronary intervention? Meta-analysis of randomized trials. Circ Cardiovasc Interv 8:e002258. https://doi.org/10.1161/CIRCINTERVENTIONS.114.002258
Rawlins J, Din JN, Talwar S, O’Kane P (2016) Coronary intervention with the excimer laser: review of the technology and outcome data. Interv Cardiol 11:27–32. https://doi.org/10.15420/icr.2016:2:2
Sintek M, Coverstone E, Bach R, Zajarias A, Lasala J, Kurz H et al (2021) Excimer laser coronary angioplasty in coronary lesions: use and safety from the NCDR/CATH PCI registry. Circ Cardiovasc Interv 14:e010061. https://doi.org/10.1161/CIRCINTERVENTIONS.120.010061
Shibata N, Takagi K, Morishima I, Yoshioka N, Furui K, Nagai H et al (2020) The impact of the excimer laser on myocardial salvage in ST-elevation acute myocardial infarction via nuclear scintigraphy. Int J Cardiovasc Imaging 36:161–170. https://doi.org/10.1007/s10554-019-01690-x
Nishino M, Mori N, Takiuchi S, Shishikura D, Doi N, Kataoka T et al (2017) Indications and outcomes of excimer laser coronary atherectomy: efficacy and safety for thrombotic lesions-The ULTRAMAN registry. J Cardiol 69:314–319. https://doi.org/10.1016/j.jjcc.2016.05.018
Topaz O, Ebersole D, Das T, Alderman EL, Madyoon H, Vora K et al (2004) Excimer laser angioplasty in acute myocardial infarction (the CARMEL multicenter trial). Am J Cardiol 93:694–701. https://doi.org/10.1016/j.amjcard.2003.11.050
Shishikura D, Otsuji S, Takiuchi S, Fukumoto A, Asano K, Ikushima M et al (2013) Vaporizing thrombus with excimer laser before coronary stenting improves myocardial reperfusion in acute coronary syndrome. Circ J 77:1445–1452. https://doi.org/10.1253/circj.cj-12-1064
Ilkay E, Karaca I, Yavuzkir M, Akbulut M, Pekdemir M (2005) The effect of interventional treatment in acute myocardial infarction on ST resolution: a comparison of coronary angioplasty with excimer laser angioplasty. Angiology 56:377–384. https://doi.org/10.1177/000331970505600403
Gibson CM, Cannon CP, Daley WL, Dodge JT Jr, Alexander B Jr, Marble SJ et al (1996) TIMI frame count: a quantitative method of assessing coronary artery flow. Circulation 93:879–888. https://doi.org/10.1161/01.cir.93.5.879
Cerqueira MD, Weissman NJ, Dilsizian V, Jacobs AK, Kaul S, Laskey WK et al (2002) Standardized myocardial segmentation and nomenclature for tomographic imaging of the heart. A statement for healthcare professionals from the Cardiac Imaging Committee of the Council on Clinical Cardiology of the American Heart Association. Circulation 105:539–542. https://doi.org/10.1161/hc0402.102975
Nakajima K, Nishimura T (2006) Inter-institution preference-based variability of ejection fraction and volumes using quantitative gated SPECT with 99mTc-tetrofosmin: a multicentre study involving 106 hospitals. Eur J Nucl Med Mol Imaging 33:127–133. https://doi.org/10.1007/s00259-005-1916-7
Laskey WK, Yancy CW, Maisel WH (2007) Thrombosis in coronary drug-eluting stents: report from the meeting of the circulatory system medical devices advisory panel of the food and drug administration center for devices and radiologic health, December 7–8, 2006. Circulation 115:2352–2357. https://doi.org/10.1161/CIRCULATIONAHA.107.688416
Kanda Y (2013) Investigation of the freely available easy-to-use software “EZR” for medical statistics. Bone Marrow Transplant 48:452–458. https://doi.org/10.1038/bmt.2012.244
Vlaar PJ, Svilaas T, van der Horst IC, Diercks GF, Fokkema ML, de Smet BJ et al (2008) Cardiac death and reinfarction after 1 year in the Thrombus Aspiration during Percutaneous coronary intervention in acute myocardial infarction Study (TAPAS): a 1-year follow-up study. Lancet 371:1915–1920. https://doi.org/10.1016/S0140-6736(08)60833-8
Fröbert O, Lagerqvist B, Olivecrona GK, Omerovic E, Gudnason T, Maeng M et al (2013) Thrombus aspiration during ST-segment elevation myocardial infarction. N Engl J Med 369:1587–1597. https://doi.org/10.1056/NEJMoa1308789
Jolly SS, Cairns JA, Yusuf S, Meeks B, Gao P, Hart RG et al (2015) Stroke in the TOTAL trial: a randomized trial of routine thrombectomy vs. percutaneous coronary intervention alone in ST elevation myocardial infarction. Eur Heart J 36:2364–2372. https://doi.org/10.1093/eurheartj/ehv296
Hibi K, Kozuma K, Maejima N, Sonoda S, Endo T, Tanaka H et al (2020) Long-term clinical outcomes after filter protection during percutaneous coronary intervention in patients with attenuated plaque – 1-year follow up of the VAMPIRE 3 (vacuum aspiration Thrombus Reemoval 3) trial. Circ J 85:44–49. https://doi.org/10.1253/circj.CJ-20-0449
Stone GW, Maehara A, Witzenbichler B, Godlewski J, Parise H, Dambrink JH et al (2012) Intracoronary abciximab and aspiration thrombectomy in patients with large anterior myocardial infarction: the INFUSE-AMI randomized trial. JAMA 307:1817–1826. https://doi.org/10.1001/jama.2012.421
Hartman MHT, Eppinga RN, Vlaar PJJ, Lexis CPH, Lipsic E, Haeck JDE et al (2017) The contemporary value of peak creatine kinase-MB after ST-segment elevation myocardial infarction above other clinical and angiographic characteristics in predicting infarct size, left ventricular ejection fraction, and mortality. Clin Cardiol 40:322–328. https://doi.org/10.1002/clc.22663
Topaz O, Minisi AJ, Bernardo NL, McPherson RA, Martin E, Carr SL, Carr ME (2001) Alterations of platelet aggregation kinetics with ultraviolet laser emission: the “stunned platelet” phenomenon. Thromb Haemost 86:1087–1093. https://doi.org/10.1055/s-0037-1616537
Topaz O, Ebersole D, Dahm JB, Alderman EL, Madyoon H, CARMEL Excimer Laser Interventional Study Group et al (2008) Excimer laser in myocardial infarction: a comparison between STEMI patients with established Q-wave versus patients with non-STEMI (non-Q). Lasers Med Sci 23:1–10. https://doi.org/10.1007/s10103-007-0444-z
Oraevsky AA, Jacques SL, Pettit GH, Saidi IS, Tittel FK, Henry PD (1992) XeCl laser ablation of atherosclerotic aorta: optical properties and energy pathways. Lasers Surg Med 12:585–597. https://doi.org/10.1002/lsm.1900120604
Backhaus SJ, Kowallick JT, Stiermaier T, Lange T, Koschalka A, Navarra JL et al (2020) Culprit vessel-related myocardial mechanics and prognostic implications following acute myocardial infarction. Clin Res Cardiol 109:339–349. https://doi.org/10.1007/s00392-019-01514-x
Asanuma T, Fukuta Y, Masuda K, Hioki A, Iwasaki M, Nakatani S (2012) Assessment of myocardial ischemic memory using speckle tracking echocardiography. JACC Cardiovasc Imaging 5:1–11. https://doi.org/10.1016/j.jcmg.2011.09.019
Ishii K, Suyama T, Imai M, Maenaka M, Yamanaka A, Makino Y et al (2009) Abnormal regional left ventricular systolic and diastolic function in patients with coronary artery disease undergoing percutaneous coronary intervention: clinical significance of post-ischemic diastolic stunning. J Am Coll Cardiol 54:1589–1597. https://doi.org/10.1016/j.jacc.2009.06.030
Baumbach A, Bittl JA, Fleck E, Geschwind HJ, Sanborn TA, Tcheng JE, Karsch KR (1994) Acute complications of excimer laser coronary angioplasty: a detailed analysis of multicenter results. Coinvestigators of the U.S. and European percutaneous excimer laser coronary angioplasty (PELCA) Registries. J Am Coll Cardiol 23:1305–1313. https://doi.org/10.1016/0735-1097(94)90371-9
Bittl JA (2008) Physical aspects of excimer laser angioplasty for undilatable lesions. Catheter Cardiovasc Interv 71:808–809. https://doi.org/10.1002/ccd.21593
Acknowledgements
None.
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All the authors contributed to the study conception, design, material preparation, data collection and analysis. The first draft of the manuscript was written by KS and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
This study was conducted in accordance with the Declaration of Helsinki. Approval was granted by the Medical Ethics Committee of Ogaki Municipal Hospital (Reference number: 20210916-9).
Consent to participate
Written informed consent was obtained from each patient or a relative before or after undergoing PCI.
Consent to publish
The authors affirm that human research participants provided informed consent for publication of the images in Figure
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shimojo, K., Shibata, N., Takagi, K. et al. Excimer laser coronary angioplasty versus manual aspiration thrombectomy in patients with ST-segment elevation myocardial infarction: analyzed by nuclear scintigraphy. Int J Cardiovasc Imaging 39, 831–842 (2023). https://doi.org/10.1007/s10554-022-02771-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-022-02771-0