Abstract
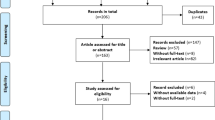
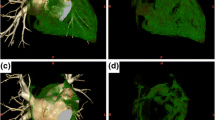
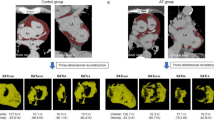
To assess the association between epicardial adipose tissue (EAT) index derived from cardiac computed tomography and atrial fibrillation (AF) recurrence after ablation by comparing with a propensity score matched non-recurrence AF patients. A total of 506 patients with AF recurrence and 174 patients without AF recurrence were enrolled in this retrospective study. Density and volume of total EAT surrounding the heart (Total-EAT) and EAT surrounding the left atrium (LA-EAT) were measured, propensity score matching(PSM) analyses were used to compare the outcomes of the two groups while controlling for confounders. Total-EAT density (HU) value (-81.27 ± 4.67 vs -84.05 ± 3.84, P < 0.001) and LA-EAT density (HU) value (-76.16 ± 4.11 vs -78.83 ± 3.81, P < 0.001) were significantly higher in the patients with AF recurrence than in those without recurrence. LA-EAT density (HU) value was significantly higher than Total-EAT (− 77.50 ± 4.18 vs -82.66 ± 4.49, P = 0.000). In a multiple logistic regression analysis, a higher LA-EAT density (odds ratio: 1.12; 95% CI: 1.02–1.22, p = 0.015) was significantly associated with the AF recurrence after adjusting for other risk factors. The LA-EAT density plays an important role in the AF recurrence after ablation. Assessment of LA-EAT density can improve ablation outcomes by refining patient selection.


Similar content being viewed by others
References
Björck S, Palaszewski B, Friberg L, Bergfeldt L (2013) Atrial fibrillation, stroke risk, and warfarin therapy revisited: a population-based study. Stroke 44:3103–3108. https://doi.org/10.1161/strokeaha.113.002329
Pastori D, Pignatelli P, Angelico F, Farcomeni A, Del Ben M, Vicario T et al (2015) Incidence of myocardial infarction and vascular death in elderly patients with atrial fibrillation taking anticoagulants: relation to atherosclerotic risk factors. Chest 147:1644–1650. https://doi.org/10.1378/chest.14-2414
Gómez-Outes A, Lagunar-Ruíz J, Terleira-Fernández AI, Calvo-Rojas G, Suárez-Gea ML, Vargas-Castrillón E (2016) Causes of Death in Anticoagulated Patients With Atrial Fibrillation. J Am Coll Cardiol 68:2508–2521. https://doi.org/10.1016/j.jacc.2016.09.944
Pokorney SD, Piccini JP, Stevens SR, Patel MR, Pieper KS, Halperin JL et al (2016) Cause of death and predictors of all-cause mortality in anticoagulated patients with nonvalvular atrial fibrillation: data from ROCKET AF. J Am Heart Assoc 5:e002197. https://doi.org/10.1161/jaha.115.002197
Lee HY, Yang PS, Kim TH, Uhm JS, Pak HN, Lee MH et al (2017) Atrial fibrillation and the risk of myocardial infarction: a nation-wide propensity-matched study. Sci Rep 7:12716. https://doi.org/10.1038/s41598-017-13061-4
Takahashi A (2010) Catheter ablation is established as a treatment option for atrial fibrillation–is catheter ablation established as a treatment option of atrial fibrillation? (Pro). Circ J 74:1972–1977. https://doi.org/10.1253/circj.cj-10-0693
Yi F, Hou W, Zhou C, Yin Y, Lu S, Duan C et al (2019) Radiofrequency ablation versus antiarrhythmic drug therapy for atrial fibrillation: meta-analysis of safety and efficacy. J Cardiovasc Pharmacol 73:241–247. https://doi.org/10.1097/fjc.0000000000000654
Al Chekakie MO, Welles CC, Metoyer R, Ibrahim A, Shapira AR, Cytron J et al (2010) Pericardial fat is independently associated with human atrial fibrillation. J Am Coll Cardiol 56:784–788. https://doi.org/10.1016/j.jacc.2010.03.071
Tsao HM, Hu WC, Wu MH, Tai CT, Lin YJ, Chang SL et al (2011) Quantitative analysis of quantity and distribution of epicardial adipose tissue surrounding the left atrium in patients with atrial fibrillation and effect of recurrence after ablation. Am J Cardiol 107:1498–1503. https://doi.org/10.1016/j.amjcard.2011.01.027
Acet H, Ertaş F, Akıl MA, Oylumlu M, Polat N, Yıldız A et al (2014) New inflammatory predictors for non-valvular atrial fibrillation: echocardiographic epicardial fat thickness and neutrophil to lymphocyte ratio. Int J Cardiovasc Imaging 30:81–89. https://doi.org/10.1007/s10554-013-0317-4
Mazurek T, Kiliszek M, Kobylecka M, Skubisz-Gluchowska J, Kochman J, Filipiak K et al (2014) Relation of proinflammatory activity of epicardial adipose tissue to the occurrence of atrial fibrillation. Am J Cardiol 113:1505–1508. https://doi.org/10.1016/j.amjcard.2014.02.005
Packer M (2019) Drugs that ameliorate epicardial adipose tissue inflammation may have discordant effects in heart failure with a preserved ejection fraction as compared with a reduced ejection fraction. J Card Fail 25:986–1003. https://doi.org/10.1016/j.cardfail.2019.09.002
Liu Q, Zhang F, Yang M, Zhong J (2020) Increasing level of interleukin-1β in epicardial adipose tissue is associated with persistent atrial fibrillation. J Interferon Cytokine Res 40:64–69. https://doi.org/10.1089/jir.2019.0098
Wong CX, Ganesan AN, Selvanayagam JB (2017) Epicardial fat and atrial fibrillation: current evidence, potential mechanisms, clinical implications, and future directions. Eur Heart J 38:1294–1302. https://doi.org/10.1093/eurheartj/ehw045
Ciuffo L, Nguyen H, Marques MD, Aronis KN, Sivasambu B, de Vasconcelos HD et al (2019) Periatrial Fat Quality Predicts Atrial Fibrillation Ablation Outcome. Circ Cardiovasc Imaging 12:e008764. https://doi.org/10.1161/circimaging.118.008764
Batal O, Schoenhagen P, Shao M, Ayyad AE, Van Wagoner DR, Halliburton SS et al (2010) Left atrial epicardial adiposity and atrial fibrillation. Circ Arrhythm Electrophysiol 3:230–236. https://doi.org/10.1161/circep.110.957241
Kogo H, Sezai A, Osaka S, Shiono M, Tanaka M (2019) Does epicardial adipose tissue influence postoperative atrial fibrillation? Ann Thorac Cardiovasc Surg 25:149–157. https://doi.org/10.5761/atcs.oa.18-00212
Nguyen BL, Fishbein MC, Chen LS, Chen PS, Masroor S (2009) Histopathological substrate for chronic atrial fibrillation in humans. Heart Rhythm 6:454–460. https://doi.org/10.1016/j.hrthm.2009.01.010
Marcus GM, Smith LM, Ordovas K, Scheinman MM, Kim AM, Badhwar N et al (2010) Intracardiac and extracardiac markers of inflammation during atrial fibrillation. Heart Rhythm 7:149–154. https://doi.org/10.1016/j.hrthm.2009.10.004
Gaborit B, Venteclef N, Ancel P, Pelloux V, Gariboldi V, Leprince P et al (2015) Human epicardial adipose tissue has a specific transcriptomic signature depending on its anatomical peri-atrial, peri-ventricular, or peri-coronary location. Cardiovasc Res 108:62–73. https://doi.org/10.1093/cvr/cvv208
Calkins H, Hindricks G, Cappato R, Kim YH, Saad EB, Aguinaga L et al (2017) 2017 HRS/EHRA/ECAS/APHRS/SOLAECE expert consensus statement on catheter and surgical ablation of atrial fibrillation. Heart Rhythm 14:e275–e444. https://doi.org/10.1016/j.hrthm.2017.05.012
Austin PC (2011) An Introduction to Propensity Score Methods for Reducing the Effects of Confounding in Observational Studies. Multivariate Behav Res 46:399–424. https://doi.org/10.1080/00273171.2011.568786
Wels MG, Lades F, Muehlberg A, Suehling M (2019) General purpose radiomics for multi-modal clinical research. InMedical Imaging 2019: Computer-Aided Diagnosis 2019 Mar 13. Vol 10950, pp 1047–1054. SPIE
Zhang M, Kono M (1997) Solitary pulmonary nodules: evaluation of blood flow patterns with dynamic CT. Radiology 205:471–478. https://doi.org/10.1148/radiology.205.2.9356631
Venteclef N, Guglielmi V, Balse E, Gaborit B, Cotillard A, Atassi F et al (2015) Human epicardial adipose tissue induces fibrosis of the atrial myocardium through the secretion of adipo-fibrokines. Eur Heart J 36:795–805a. https://doi.org/10.1093/eurheartj/eht099
Vyas V, Lambiase P (2019) Obesity and Atrial Fibrillation: Epidemiology, Pathophysiology and Novel Therapeutic Opportunities. Arrhythm Electrophysiol Rev 8:28–36. https://doi.org/10.15420/aer.2018.76.2
Chung MK, Martin DO, Sprecher D, Wazni O, Kanderian A, Carnes CA et al (2001) C-reactive protein elevation in patients with atrial arrhythmias: inflammatory mechanisms and persistence of atrial fibrillation. Circulation 104:2886–2891. https://doi.org/10.1161/hc4901.101760
Aviles RJ, Martin DO, Apperson-Hansen C, Houghtaling PL, Rautaharju P, Kronmal RA et al (2003) Inflammation as a risk factor for atrial fibrillation. Circulation 108:3006–3010. https://doi.org/10.1161/01.Cir.0000103131.70301.4f
Malouf JF, Kanagala R, Al Atawi FO, Rosales AG, Davison DE, Murali NS et al (2005) High sensitivity C-reactive protein: a novel predictor for recurrence of atrial fibrillation after successful cardioversion. J Am Coll Cardiol 46:1284–1287. https://doi.org/10.1016/j.jacc.2005.06.053
Rotter M, Jaïs P, Vergnes MC, Nurden P, Takahashi Y, Sanders P et al (2006) Decline in C-reactive protein after successful ablation of long-lasting persistent atrial fibrillation. J Am Coll Cardiol 47:1231–1233. https://doi.org/10.1016/j.jacc.2005.12.038
Liu T, Li G. Periatrial epicardial fat, local pro- and anti-inflammatory balance, and atrial fibrillation. J Am Coll Cardiol 2011;57:1249. https://doi.org/10.1016/j.jacc.2010.09.068
Shin SY, Yong HS, Lim HE, Na JO, Choi CU, Choi JI et al (2011) Total and interatrial epicardial adipose tissues are independently associated with left atrial remodeling in patients with atrial fibrillation. J Cardiovasc Electrophysiol 22:647–655. https://doi.org/10.1111/j.1540-8167.2010.01993.x
Frustaci A, Chimenti C, Bellocci F, Morgante E, Russo MA, Maseri A (1997) Histological substrate of atrial biopsies in patients with lone atrial fibrillation. Circulation 96:1180–1184. https://doi.org/10.1161/01.cir.96.4.1180
Hell MM, Achenbach S, Schuhbaeck A, Klinghammer L, May MS, Marwan M (2016) CT-based analysis of pericoronary adipose tissue density: Relation to cardiovascular risk factors and epicardial adipose tissue volume. J Cardiovasc Comput Tomogr 10:52–60. https://doi.org/10.1016/j.jcct.2015.07.011
Balcer B, Dykun I, Schlosser T, Forsting M, Rassaf T, Mahabadi AA (2018) Pericoronary fat volume but not attenuation differentiates culprit lesions in patients with myocardial infarction. Atherosclerosis 276:182–188. https://doi.org/10.1016/j.atherosclerosis.2018.05.035
Sepehri Shamloo A, Dagres N, Dinov B, Sommer P, Husser-Bollmann D, Bollmann A et al (2019) Is epicardial fat tissue associated with atrial fibrillation recurrence after ablation? A systematic review and meta-analysis. Int J Cardiol Heart Vasc 22:132–138. https://doi.org/10.1016/j.ijcha.2019.01.003
Nagashima K, Okumura Y, Watanabe I, Nakai T, Ohkubo K, Kofune T et al (2011) Association between epicardial adipose tissue volumes on 3-dimensional reconstructed CT images and recurrence of atrial fibrillation after catheter ablation. Circ J 75:2559–2565. https://doi.org/10.1253/circj.cj-11-0554
D’Ascenzo F, Corleto A, Biondi-Zoccai G, Anselmino M, Ferraris F, di Biase L et al (2013) Which are the most reliable predictors of recurrence of atrial fibrillation after transcatheter ablation?: a meta-analysis. Int J Cardiol 167:1984–1989. https://doi.org/10.1016/j.ijcard.2012.05.008
Krummen DE, Swarup V, Narayan SM (2015) The role of rotors in atrial fibrillation. J Thorac Dis 7:142–151. https://doi.org/10.3978/j.issn.2072-1439.2014.11.15
Mayyas F, Niebauer M, Zurick A, Barnard J, Gillinov AM, Chung MK et al (2010) Association of left atrial endothelin-1 with atrial rhythm, size, and fibrosis in patients with structural heart disease. Circ Arrhythm Electrophysiol 3:369–379. https://doi.org/10.1161/circep.109.924985
Funding
(1) Shanghai Rising Stars of Medical Talent Youth Development Program, Youth Medical Talents—Medical Imaging Practitioner Program: SHWRS(2020)_087. (2) Three-Year Initiative Plan for Strengthening Public Health System Construction in Shanghai—Youth Medical Talents: GWV-10.2-YQ30. (3) Shanghai Sailing Program. (4) Natural Science Foundation of China under Grant: 8217070113.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by MY, WB, ZX, LQ and NZh. Conceptualization, resources, and methodology were performed by WY, and FY. The first draft of the manuscript was written by MY. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The approval for this study had been granted by the local Institutional Review board prior to its conduct and informed consent was waived. The study therefore had been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. No patient identifiers were collected, and details that might disclose the identity of the subjects under study should were omitted.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yang, M., Bao, W., Xu, Z. et al. Association between epicardial adipose tissue and recurrence of atrial fibrillation after ablation: a propensity score-matched analysis. Int J Cardiovasc Imaging 38, 1865–1872 (2022). https://doi.org/10.1007/s10554-022-02557-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-022-02557-4