Abstract
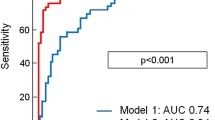
Although myocardial contrast echocardiography (MCE) can evaluate microvascular perfusion abnormalities, its prognostic value is uncertain in acute anterior wall ST-Segment elevation myocardial infarction (STEMI) with successful epicardial recanalization. Therefore, the study aims to investigate the prognostic role of qualitative and quantitative MCE in acute anterior wall STEMI with successful epicardial recanalization. 153 STEMI patients were assessed by MCE within 7 days after successful epicardial recanalization. Qualitative perfusion parameters (microvascular perfusion score index, MPSI) and quantitative perfusion parameters (A, β, and Aβ) were acquired using a 17-segment model. And corrected A and Aβ were calculated. Patients were all followed for major adverse cardiovascular events (MACEs). During median follow-up of 27 (4) months, 39 (25.49%) patients experienced MACEs, while 114 (74.51%) were free from MACEs. Patients with MACEs had higher MPSI (1.65 ± 0.13 vs. No-MACEs 1.35 ± 0.20, P < 0.001), lower β (1.09 ± 0.19 s−1 vs. No-MACEs 1.34 ± 0.30 s−1, P < 0.001), corrected A (0.17 ± 0.03 dB vs. No-MACEs 0.19 ± 0.04 dB, P = 0.039) and lower corrected Aβ (0.19 ± 0.06 dB/s vs. No-MACEs 0.25 ± 0.08 dB/s, P < 0.001). MPSI of 1.44 provided an area under the curve (AUC) of 0.872, while β of 1.18 s−1 and corrected Aβ of 0.22 dB/s provided AUCs of 0.759 and 0.724, respectively. The combination of MPSI, β and corrected Aβ provided an increased AUC of 0.964 (all P < 0.05). Time-dependent ROC analysis showed that the AUCs of the MPSI, β, corrected Aβ and the combination at 1, 1.5 and 2 years indicated a strong predictive power for MACEs (AUC = 0.900/0.894/0.881 for MPSI, 0.648/0.704/0.732 for β, 0.674/0.686/0.722 for corrected Aβ, and 0.947/0.962/0.967 for the combination, respectively). Patients with MPSI < 1.44, β > 1.18 s−1, or corrected Aβ > 0.22 dB/s had lower event rate (all Log Rank P ≤ 0.001). MPSI, β, corrected Aβ, GLS and WBC were independent predictors of MACEs with adjusted hazard ratio of 34.41 (8.18–144.87), P < 0.001 for MPSI; 39.29 (27.46–65.44), P < 0.001 for β; 8.93 (1.46–54.55), P = 0.018 for corrected Aβ; 10.88 (2.83–41.86), P = 0.001 for GLS; and 1.43 (1.16–1.75), P = 0.001 for WBC. Qualitative and quantitative MCE can accurately predict MACEs in acute anterior wall STEMI with successful epicardial recanalization, and their combined predictive value is higher.



Similar content being viewed by others
References
Levine GN, Bates ER, Blankenship JC et al (2011) 2011 ACCF/AHA/SCAI guideline for percutaneous coronary intervention. A report of the american college of cardiology foundation/american heart association task force on practice guidelines and the society for cardiovascular angiography and interventions. J Am Coll Cardiol 58:e44-122. https://doi.org/10.1016/j.jacc.2011.08.007
Ogara PT, Kushner FG, Ascheim DD et al (2013) 2013 ACCF/AHA guideline for the management of st-elevation myocardial infarction: Executive summary: A report of the american college of cardiology foundation/american heart association task force on practice guidelines. J Am Coll Cardiol 61:485–510. https://doi.org/10.1016/j.jacc.2012.11.018
Savic L, Mrdovic I, Asanin M et al (2019) Using the RISK-PCI score in the long-term prediction of major adverse cardiovascular events and mortality after primary percutaneous coronary intervention. J Interv Cardiol 2019:2679791. https://doi.org/10.1155/2019/2679791
Bethke A, Halvorsen S, Bøhmer E et al (2015) Myocardial perfusion grade predicts final infarct size and left ventricular function in patients with ST-elevation myocardial infarction treated with a pharmaco-invasive strategy (thrombolysis and early angioplasty). EuroIntervention 11:518–524. https://doi.org/10.4244/eijy15m04_02
Fearon WF, Low AF, Yong AS et al (2013) Prognostic value of the index of microcirculatory resistance measured after primary percutaneous coronary intervention. Circulation 127:2436–2441. https://doi.org/10.1161/circulationaha.112.000298
Wei K, Peters D, Belcik T et al (2010) A predictive instrument using contrast echocardiography in patients presenting to the emergency department with chest pain and without ST-segment elevation. J Am Soc Echocardiogr 23:636–642. https://doi.org/10.1016/j.echo.2010.03.013
Jiang L, Yao H, Liang ZG (2017) Postoperative assessment of myocardial function and microcirculation in patients with acute coronary syndrome by myocardial contrast echocardiography. Med Sci Monit 23:2324–2332. https://doi.org/10.12659/msm.901233
Xie F, Qian L, Goldsweig A et al (2020) Event-free survival following successful percutaneous intervention in acute myocardial infarction depends on microvascular perfusion. Circ Cardiovasc Imaging 13:e010091. https://doi.org/10.1161/CIRCIMAGING.119.010091
Aggarwal S, Xie F, High R et al (2018) Prevalence and predictive value of microvascular flow abnormalities after successful contemporary percutaneous coronary intervention in acute ST-segment elevation myocardial infarction. J Am Soc Echocardiogr 31:674–682. https://doi.org/10.1016/j.echo.2018.01.009
Porter TR, Xie F (2010) Myocardial perfusion imaging with contrast ultrasound. JACC Cardiovasc Imaging 3:176–187. https://doi.org/10.1016/j.jcmg.2009.09.024
O’Gara PT, Kushner FG, Ascheim DD et al (2013) 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol 61:e78–e140. https://doi.org/10.1016/j.jacc.2012.11.019
Galiuto L, Garramone B, Scarà A et al (2008) The extent of microvascular damage during myocardial contrast echocardiography is superior to other known indexes of post-infarct reperfusion in predicting left ventricular remodeling: results of the multicenter AMICI study. J Am Coll Cardiol 51:552–559. https://doi.org/10.1016/j.jacc.2007.09.051
Min SY, Song JM, Shin Y et al (2017) Quantitative segmental analysis of myocardial perfusion to differentiate stress cardiomyopathy from acute myocardial infarction: A myocardial contrast echocardiography study. Clin Cardiol 40:679–685. https://doi.org/10.1002/clc.22714
Galea N, Dacquino GM, Ammendola RM et al (2019) Microvascular obstruction extent predicts major adverse cardiovascular events in patients with acute myocardial infarction and preserved ejection fraction. Eur Radiol 29:2369–2377. https://doi.org/10.1007/s00330-018-5895-z
Kaul S, Jayaweera AR (1997) Coronary and myocardial blood volumes: noninvasive tools to assess the coronary microcirculation? Circulation 96:719–724. https://doi.org/10.1161/01.cir.96.3.785
Porter TR, Adolphson M, High RR et al (2011) Rapid detection of coronary artery stenoses with real-time perfusion echocardiography during regadenoson stress. Circ Cardiovasc Imaging 4:628–635. https://doi.org/10.1161/circimaging.111.966341
Sun L, Wang Z, Xu T et al (2018) The value of real-time myocardial contrast echocardiography for detecting coronary microcirculation function in coronary artery disease patients. Anatol J Cardiol 19:27–33. https://doi.org/10.14744/AnatolJCardiol.2017.8041
Wu J, Barton D, Xie F et al (2016) Comparison of fractional flow reserve assessment with demand stress myocardial contrast echocardiography in angiographically intermediate coronary stenoses. Circ Cardiovasc Imaging 9:e004129. https://doi.org/10.1161/circimaging.116.004129
Abdelmoneim SS, Dhoble A, Bernier M et al (2009) Quantitative myocardial contrast echocardiography during pharmacological stress for diagnosis of coronary artery disease: a systematic review and meta-analysis of diagnostic accuracy studies. Eur J Echocardiogr 10:813–825. https://doi.org/10.1093/ejechocard/jep084
Janardhanan R, Moon JC, Pennell DJ, Senior R (2005) Myocardial contrast echocardiography accurately reflects transmurality of myocardial necrosis and predicts contractile reserve after acute myocardial infarction. Am Heart J 149:355–362. https://doi.org/10.1016/j.ahj.2004.06.018
Janardhanan R, Swinburn JM, Greaves K, Senior R (2003) Usefulness of myocardial contrast echocardiography using low-power continuous imaging early after acute myocardial infarction to predict late functional left ventricular recovery. Am J Cardiol 92:493–497. https://doi.org/10.1016/s0002-9149(03)00713-6
Coggins MP, Sklenar J, Le DE et al (2001) Noninvasive prediction of ultimate infarct size at the time of acute coronary occlusion based on the extent and magnitude of collateral-derived myocardial blood flow. Circulation 104:2471–2477. https://doi.org/10.1161/hc4501.098954
Mathias W, Tsutsui JM, Tavares BG et al (2016) Diagnostic ultrasound impulses improve microvascular flow in patients with STEMI receiving intravenous microbubbles. J Am Coll Cardiol 67:2506–2515. https://doi.org/10.1016/j.jacc.2016.03.542
Li X, He S, Zhang YS et al (2016) Resting myocardial contrast echocardiography for the evaluation of coronary microcirculation dysfunction in patients with early coronary artery disease. Clin Cardiol 39:453–458. https://doi.org/10.1002/clc.22548
Baks T, van Geuns RJ, Biagini E et al (2006) Effects of primary angioplasty for acute myocardial infarction on early and late infarct size and left ventricular wall characteristics. J Am Coll Cardiol 47:40–44. https://doi.org/10.1016/j.jacc.2005.09.008
Sattler SM, Skibsbye L, Linz D et al (2019) Ventricular arrhythmias in first acute myocardial infarction: epidemiology, mechanisms, and interventions in large animal models. Front Cardiovasc Med 6:158. https://doi.org/10.3389/fcvm.2019.00158
Nijveldt R, Beek AM, Hirsch A et al (2008) Functional recovery after acute myocardial infarction: comparison between angiography, electrocardiography, and cardiovascular magnetic resonance measures of microvascular injury. J Am Coll Cardiol 52:181–189. https://doi.org/10.1016/j.jacc.2008.04.006
Yang L, Xia C, Mu Y et al (2016) Prognostic value of real time myocardial contrast echocardiography after percutaneous coronary intervention. Echocardiography 33:421–430. https://doi.org/10.1111/echo.13061
Bolognese L, Carrabba N, Parodi G et al (2004) Impact of microvascular dysfunction on left ventricular remodeling and long-term clinical outcome after primary coronary angioplasty for acute myocardial infarction. Circulation 109:1121–1126. https://doi.org/10.1161/01.cir.0000118496.44135.a7
Dwivedi G, Janardhanan R, Hayat SA et al (2007) Prognostic value of myocardial viability detected by myocardial contrast echocardiography early after acute myocardial infarction. J Am Coll Cardiol 50:327–334. https://doi.org/10.1016/j.jacc.2007.03.036
Abdelmoneim SS, Martinez MW, Mankad SV et al (2015) Resting qualitative and quantitative myocardial contrast echocardiography to predict cardiac events in patients with acute myocardial infarction and percutaneous revascularization. Heart Vessels 30:45–55. https://doi.org/10.1007/s00380-013-0460-9
Funding
This study was supported by “the Fundamental Research Funds for the Central Universities” (2042021kf0121).
Author information
Authors and Affiliations
Contributions
YXZ and YGH carried out the studies, participated in data collection, established the framework of this study, performed the statistical analysis, and drafted the manuscript under the supervision of QZ and JLC. The MCE examination was performed by SC, JRL and YX. WYY helped to proofread the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
All authors declare that there is no conflict of interest.
Ethical approval
The study protocol was approved by the local medical ethics committee (WDRY2020- K189).
Informed consent
Informed consent was obtained from all patients participants included in the study.
Consent for publication
All patients signed informed consent regarding publishing their anonymized data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhou, Yx., Hu, Yg., Cao, S. et al. Prognostic value of myocardial contrast echocardiography in acute anterior wall ST-segment elevation myocardial infarction with successful epicardial recanalization. Int J Cardiovasc Imaging 38, 1487–1497 (2022). https://doi.org/10.1007/s10554-022-02545-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-022-02545-8