Abstract
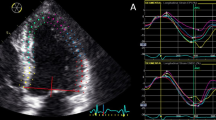
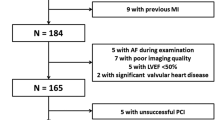
Two-dimensional speckle tracking echocardiography (2D-STE) multilayer analysis of myocardial deformation is a non-invasive method that enables discrimination of transmural differences owing to myocardial ischemia or necrosis. We wished to ascertain if multilayer longitudinal strains at rest are associated with significant (≥70 %) stenosis of the left anterior descending coronary artery (LAD) in patients with suspected non-ST-elevation acute coronary syndrome (NSTE-ACS). Our cohort comprised 113 consecutive patients with suspected NSTE-ACS and preserved ejection fraction (EF). Using coronary angiography, we diagnosed 63 patients with significant stenosis of the LAD and 50 patients without significant coronary artery disease. Echocardiography was done ≤48 h before angiography. Multilayer longitudinal strains were assessed from the endocardium, mid-myocardium and epicardium by 2D-STE. Regional longitudinal strain in LAD territory (RLSLAD) was calculated as the mean peak systolic longitudinal strain of segments subtended by the LAD for all myocardial layers. Significant differences were observed in all strain parameters between the two groups. RLSLAD and global longitudinal strain in the endocardium showed higher accuracy than that in the mid-myocardium and epicardium, wall motion score index (WMSI), WMSI in LAD territory, and EF for detection of significant LAD stenosis (all P < 0.05), with areas under the receiver operating characteristic curve of 0.87 and 0.91, respectively. An endocardial RLSLAD cutoff of −23.52 % showed optimal sensitivity and specificity (88.9/80.0 %). In patients with suspected NSTE-ACS, multilayer longitudinal strain analysis at rest might enable prediction of significant LAD stenosis, and could help to identify patients requiring reperfusion.



Similar content being viewed by others
References
Bassand JP, Hamm CW, Ardissino D et al. (2007) Guidelines for the diagnosis and treatment of non-ST-segment elevation acute coronary syndromes. EUR HEART J 28:1598–1660
Levine GN, Bates ER, Blankenship JC et al (2011) ACCF/AHA/SCAI Guideline for Percutaneous Coronary Intervention. A report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines and the Society for Cardiovascular Angiography and Interventions. J Am Coll Cardiol 58:e44–e122
Abbate A, Vetrovec G, Crea F (2010) Low diagnostic yield of elective coronary angiography. N Engl J Med 363:92–93
Montgomery DE, Puthumana JJ, Fox JM, Ogunyankin KO (2012) Global longitudinal strain aids the detection of non-obstructive coronary artery disease in the resting echocardiogram. Eur Heart J Cardiovasc Imaging 13:579–587
Choi JO, Cho SW, Song YB et al (2009) Longitudinal 2D strain at rest predicts the presence of left main and three vessel coronary artery disease in patients without regional wall motion abnormality. Eur J Echocardiogr 10:695–701
Nucifora G, Schuijf JD, Delgado V et al (2010) Incremental value of subclinical left ventricular systolic dysfunction for the identification of patients with obstructive coronary artery disease. Am Heart J 159:148–157
Biering-Sorensen T, Hoffmann S, Mogelvang R et al (2014) Myocardial strain analysis by 2-dimensional speckle tracking echocardiography improves diagnostics of coronary artery stenosis in stable angina pectoris. Circ Cardiovasc Imaging 7:58–65
Leitman M, Lysyansky P, Sidenko S et al (2004) Two-dimensional strain- a novel software for real-time quantitative echocardiographic assessment of myocardial function. J Am Soc Echocardiogr 17:1021–1029
Greenbaum RA, Ho SY, Gibson DG, Becker AE, Anderson RH (1981) Left ventricular fiber architecture in man. Br Heart J 45:248–263
Sabbah HN, Marzilli M, Stein PD (1981) The relative role of subendocardium and subepicardium in left ventricular mechanics. Am J Physiol 240:H920–H926
Duncker DJ, Traverse JH, Ishibashi Y, Bache RJ (1999) Effect of NO on transmural distribution of blood flow in hypertrophied left ventricle during exercise. Am J Physiol 276:H1305–H1312
Geer JC, Crago CA, Little WC, Gardner LL, Bishop SP (1980) Subendocardial ischemic myocardial lesions associated with severe coronary atherosclerosis. Am J Pathol 98:663–680
Grenne B, Eek C, Sjoli B et al (2010) Changes of myocardial function in patients with non-ST-elevation acute coronary syndrome awaiting coronary angiography. Am J Cardiol 105:1212–1218
Sarvari SI, Haugaa KH, Zahid W et al (2013) Layer-specific quantification of myocardial deformation by strain echocardiography may reveal significant CAD in patients with non-ST-segment elevation acute coronary syndrome. JACC Cardiovasc Imaging 6:535–544
Lang RM, Badano LP, Mor-Avi V et al (2015) Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging 16:233–270
Scanlon PJ, Faxon DP, Audet AM et al (1999) ACC/AHA guidelines for coronary angiography: executive summary and recommendations: a report of the american college of cardiology/american heart association task force on practice guidelines (committee on coronary angiography) developed in collaboration with the society for cardiac angiography and interventions. Circulation 99:2345–2357
DeLong ER, DeLong DM, Clarke-Pearson DL (1988) Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44:837–845
Hashimoto I, Li X, Hejmadi Bhat A, Jones M, Zetts AD, Sahn DJ (2003) Myocardial strain rate is a superior method for evaluation of left ventricular subendocardial function compared with tissue doppler imaging. J Am Coll Cardiol 42:1574–1583
Altiok E, Neize lM, Tiemann S et al (2012) Quantitative analysis of endocardial and epicardial left ventricular myocardial deformation-comparison of strain-encoded cardiac magnetic resonance imaging with two-dimensional speckle-tracking echocardiography. J Am Soc Echocardiogr 25:1179–1188
Adamu U, Schmitz F, Becker M, Kelm M, Hoffmann R (2009) Advanced speckle tracking echocardiography allowing a three-myocardial layer-specific analysis of deformation parameters. Eur J Echocardiogr 10:303–308
Leitman M, Lysiansky M, Lysyansky P et al (2010) Circumferential and longitudinal strain in 3 myocardial layers in normal subjects and in patients with regional left ventricular dysfunction. J Am Soc Echocardiogr 23:64–70
Reimer KA, Jennings RB (1979) The “wavefront phenomenon” of myocardial ischemic cell death. Ii. Transmural progression of necrosis within the framework of ischemic bed size (myocardium at risk) and collateral flow. Lab Invest 40:633–644
Kloner RA, Jennings RB (2001) Consequences of brief ischemia: stunning, preconditioning, and their clinical implications. Circulation 104:3158–3167
Wijns W, Vatner SF, Camici PG (1998) Hibernating myocardium. N Engl J Med 339:173–181
Gotte MJ, van Rossum AC, Twisk JWR, Kuijer JPA, Marcus JT, Visser CA (2001) Quantification of regional contractile function after infarction: strain analysis superior to wall thickening analysis in discriminating infarct from remote myocardium. J Am Coll Cardiol 37:808–817
Stankovic I, Putnikovic B, Cvjetan R et al (2015) Visual assessment vs. strain imaging for the detection of critical stenosis of the left anterior descending coronary artery in patients without a history of myocardial infarction. Eur Heart J Cardiovasc Imaging 16:402–409
Nahrendorf M, Hiller KH, Greiser A et al (2003) Chronic coronary artery stenosis induces impaired function of remote myocardium: MRI and spectroscopy study in rat. Am J Physiol Heart Circ Physiol 285:H2712–H2721
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Liu, C., Li, J., Ren, M. et al. Multilayer longitudinal strain at rest may help to predict significant stenosis of the left anterior descending coronary artery in patients with suspected non-ST-elevation acute coronary syndrome. Int J Cardiovasc Imaging 32, 1675–1685 (2016). https://doi.org/10.1007/s10554-016-0959-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-016-0959-0