Abstract
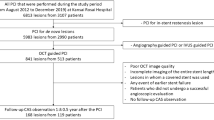
Several characteristics of neointimal tissues, including neoatherosclerotic progression, have been reported in lesions with in-stent restenosis (ISR). However, the effects of these characteristics on outcomes after percutaneous coronary intervention (PCI) for ISR lesions remain unclear. We assessed the relationships between neointimal tissue characteristics and the occurrence of periprocedural myonecrosis (PMN) after PCI in ISR lesions. We investigated 72 ISR lesions in 72 patients with stable angina pectoris (SAP) who underwent pre- and post-revascularization optical coherence tomography (OCT) and coronary angioscopy (CAS). All lesions were classified as with PMN, defined by an elevated peak high-sensitivity cardiac troponin-T level during the 24-h post-PCI period, and without PMN. PMN was observed in 23 (31.9 %) lesions. PMN lesions had higher frequencies of OCT-derived thin-cap fibroatheroma (26.1 vs. 6.1 %, P = 0.03), CAS-derived intensive yellow neointima (30.4 vs. 10.2 %, P = 0.04), neointima with complex surface (60.9 vs. 28.6 %, P = 0.01), and CAS-derived atheromatous appearance (CAS-AAP), defined as yellow plaque including complex thrombi underneath disrupted neointimal coverage after ballooning (47.8 vs. 16.3 %, P = 0.008) at the most stenotic sites inside stents, compared to lesions without PMN. Multivariate logistic regression analysis identified CAS-AAP (odds ratio: 3.568, 95 % confidence interval: 1.109–11.475, P = 0.033) as an independent predictor of PMN. For ISR lesions in SAP patients, an OCT- and CAS-based assessment of neointimal tissue characteristics might help to predict the occurrence of PMN.





Similar content being viewed by others
References
Daemen J, Wenaweser P, Tsuchida K et al (2007) Early and late coronary stent thrombosis of sirolimus-eluting and paclitaxel-eluting stents in routine clinical practice: data from a large two-institutional cohort study. The Lancet 369:667–678
Inoue K, Abe K, Ando K et al (2014) Pathological analyses of long-term intracoronary Palmaz-Schatz stenting; Is its efficacy permanent? Cardiovasc Pathol 13:109–115
Nakazawa G, Otsuka F, Nakano M et al (2011) The pathology of neoatherosclerosis in human coronary implants bare-metal and drug-eluting stents. J Am Coll Cardiol 57:1314–1322
Yamaji K, Inoue K, Nakahashi T et al (2012) Bare metal stent thrombosis and in-stent neoatherosclerosis. Circ Cardiovasc Interv 5:47–54
Amabile N, Souteyrand G, Ghostine S et al (2014) Very late stent thrombosis related to incomplete neointimal coverage or neoatherosclerotic plaque rupture identified by optical coherence tomography imaging. Eur Heart J Cardiovasc Imaging 5:24–31
Yabushita H, Bouma BE, Houser SL et al (2002) Characterization of human atherosclerosis by optical coherence tomography. Circulation 106:1640–1645
Jang IK, Tearney GJ, MacNeill B et al (2005) In vivo characterization of coronary atherosclerotic plaque by use of optical coherence tomography. Circulation 111:1551–1555
Takano M, Yamamoto M, Inami S et al (2009) Appearance of lipid-laden neointima and neovascularization after implantation of bare-metal stents extended late-phase observation by intracoronary optical coherence tomography. J Am Coll Cardiol 55:26–32
Kang SJ, Mintz GS, Akasaka T et al (2011) Optical coherence tomographic analysis of in-stent neoatherosclerosis after drug-eluting stent implantation. Circulation 123:2954–2963
Yonetsu T, Kim JS, Kato K et al (2012) Comparison of incidence and time course of neoatherosclerosis between bare metal stents and drug-eluting stents using optical coherence tomography. Am J Cardiol 110:933–939
Kotani J, Awata M, Nanto S et al (2006) Incomplete neointimal coverage of sirolimus-eluting stents: angioscopic findings. J Am Coll Cardiol 47:2108–2111
Thieme T, Wernecke KD, Meyer R et al (1996) Angioscopic evaluation of atherosclerotic plaques: validation by histomorphologic analysis and association with stable and unstable coronary syndromes. J Am Coll Cardiol 28:1–6
Awata M, Kotani J, Uematsu M et al (2007) Serial angioscopic evidence of incomplete neointimal coverage after sirolimus-eluting stent implantation: comparison with bare-metal stents. Circulation 116:910–916
Higo T, Ueda Y, Oyabu J et al (2009) Atherosclerotic and thrombogenic neointima formed over sirolimus drug-eluting stent: an angioscopic study. J Am Coll Cardiol Img 2:616–624
Abdelmeguid AE, Topol EJ, Whitlow PL et al (1996) Significance of mild transient release of creatine kinase-MB fraction after percutaneous coronary interventions. Circulation 94:1528–1536
Kimura S, Kakuta T, Yonetsu T et al (2009) Clinical significance of echo signal attenuation on intravascular ultrasound in patients with coronary artery disease. Circ Cardiovasc Interv 2:444–454
Lee T, Yonetsu T, Koura K et al (2011) Impact of coronary plaque morphology assessed by optical coherence tomography on cardiac troponin elevation in patients with elective stent implantation. Circ Cardiovasc Interv 4:378–386
Porto I, Di Vito L, Burzotta F et al (2012) Predictors of periprocedural (type IVa) myocardial infarction, as assessed by frequency-domain optical coherence tomography. Circ Cardiovasc Interv 5:89–96
Murakami D, Takano M, Yamamoto M et al (2011) Intense yellow culprit plaque coloration is closely associated with troponin-T elevation and flow complications following elective coronary stenting. J Atheroscler Thromb 18:906–913
Ali ZA, Roleder T, Narula J et al (2013) Increased thin-cap neoatheroma and periprocedural myocardial infarction in drug-eluting stent restenosis: multimodality intravascular imaging of drug-eluting and bare-metal stents. Circ Cardiovasc Interv 6:507–517
Lee SY, Hong MK, Shin DH et al (2015) Optical coherence tomography-based predictors for creatine kinase-myocardial band elevation after elective percutaneous coronary intervention for in-stent restenosis. Catheter Cardiovasc Interv 85:564–572
Thygesen K, Alpert JS, Jaffe AS et al (2012) Third universal definition of myocardial infarction. Eur Heart J 20:2551–2567
Kimura S, Sugiyama T, Hishikari K et al (2015) Association of intravascular ultrasound- and optical coherence tomography-assessed coronary plaque morphology with periprocedural myocardial injury in patients with stable angina pectoris. Circ J 79:1944–1953
The TIMI Study Group (1985) The thrombolysis in myocardial infarction (TIMI) trial. N Engl J Med 312:932–936
Gibson CM, Cannon CP, Daley WL et al (1996) TIMI frame count: a quantitative method of assessing coronary artery flow. Circulation 93:879–888
van‘t Hof AW, Liem A, Suryapranata H et al (1998) Angiographic assessment of myocardial reperfusion in patients treated with primary angioplasty for acute myocardial infarction: myocardial blush grade. Zwolle Myocardial Infarction Study Group. Circulation 97:2302–2306
Gonzalo N, Serruys PW, Okamura T et al (2009) Optical coherence tomography patterns of stent restenosis. Am Heart J 158:284–293
Tearney GJ, Regar E, Akasaka T et al (2012) Consensus standards for acquisition, measurement, and reporting of intravascular optical coherence tomography studies: a report from the international working group for intravascular optical coherence tomography standardization and validation. J Am Coll Cardiol 59:1058–1072
Ueda Y, Asakura M, Hirayama A et al (1996) Intracoronary morphology of culprit lesions after reperfusion in acute myocardial infarction: serial angioscopic observations. J Am Coll Cardiol 27:606–610
Sakai S, Mizuno K, Yokoyama S et al (2003) Morphologic changes in infarct-related plaque after coronary stent placement: a serial angioscopy study. J Am Coll Cardiol 42:1558–1565
Shibuya M, Fujii K, Hao H et al (2015) Tissue Characterization of in-stent neointima using optical coherence tomography in the late phase after bare-metal stent implantation-an ex vivo validation study. Circ J 79:2224–2230
Nagoshi R, Shinke T, Otake H et al (2013) Qualitative and quantitative assessment of stent restenosis by optical coherence tomography: comparison between drug-eluting and bare-metal stents. Circ J 77:652–660
Takano M, Jang IK, Inami S et al (2008) In vivo comparison of optical coherence tomography and angioscopy for the evaluation of coronary plaque characteristics. Am J Cardiol 101:471–476
Tada T, Byrne RA, Simunovic I et al (2013) Risk of stent thrombosis among bare-metal stents, first-generation drug-eluting stents, and second-generation drug-eluting stents: results from a registry of 18,334 patients. JACC Cardiovasc Interv 6:1267–1274
Otsuka F, Vorpahl M, Nakano M et al (2014) Pathology of second-generation everolimus-eluting stents versus first-generation sirolimus- and paclitaxel-eluting stents in humans. Circulation 129:211–223
Lee SY, Hur SH, Lee SG et al (2015) Optical coherence tomographic observation of in-stent neoatherosclerosis in lesions with more than 50 % neointimal area stenosis after second-generation drug-eluting stent implantation. Circ Cardiovasc Interv 2:e001878
Herrmann J, Lennon RJ, Jaffe AS et al (2014) Defining the optimal cardiac troponin T threshold for predicting death caused by periprocedural myocardial infarction after percutaneous coronary intervention. Circ Cardiovasc Interv 7:533–542
Moussa ID, Klein LW, Shah B et al (2013) Consideration of a new definition of clinically relevant myocardial infarction after coronary revascularization: an expert consensus document from the Society for Cardiovascular Angiography and Interventions (SCAI). J Am Coll Cardiol 62:1563–1570
Inoue T, Shinke T, Otake H et al (2014) Neoatherosclerosis and mural thrombus detection after sirolimus-eluting stent implantation. Circ J 78:92–100
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interests.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kimura, S., Sugiyama, T., Hishikari, K. et al. Impact of optical coherence tomography- and coronary angioscopy-assessed neointimal tissue characteristics on occurrence of periprocedural myonecrosis in patients with in-stent restenosis. Int J Cardiovasc Imaging 32, 1483–1494 (2016). https://doi.org/10.1007/s10554-016-0941-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-016-0941-x