Abstract
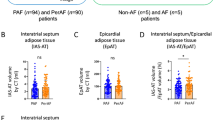
Epicardial adipose tissue (EAT), as an endocrine organ, may serve as a source of pro-inflammatory cytokines. Also, given the strong relationship between atrial fibrillation (AF), obesity and inflammation, the purpose of this study was to investigate the association of non-valvular AF with epicardial and periatrial fat. A total of 618 (192 in sinus rhythm, 169 with paroxysmal AF, 133 with persistent AF and 124 with permanent AF) patients who underwent CT angiography for the evaluation of CAD or pulmonary vein anatomy before catheter ablation were enrolled in this study. Thickness of the EAT and periatrial fat were measured by CT angiography. Together with body mass index, these were examined in relation to the presence and severity of AF and left atrial (LA) diameter. Patients with AF had significantly more total EAT and periatrial fat thickness compared with patients in sinus rhythm (p < 0.001). EAT thickness was significantly higher in permanent, persistent and paroxysmal AF compared with sinus rhythm group (p < 0.001). Multivariable multinomial logistic regression analysis comparing patients with sinus rhythm and subtypes of AF revealed a significant association between periatrial fat and total EAT thickness with all AF subtypes. Correlation analysis demonstrated that both total EAT thickness and periatrial fat thickness were significantly correlated with LA diameter (p < 0.05). Epicardial fat thickness is associated with both the presence and severity of AF independent of all other risk factors including LA diameter. Mediators for the association of EAT with AF pathophysiology requires future large scale prospective studies.




Similar content being viewed by others
References
January CT, Wann LS, Alpert JS et al. (2014) 2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the Heart Rhythm Society. J Am Coll Cardiol
European Heart Rhythm A, European Association for Cardio-Thoracic S, Camm AJ et al (2010) Guidelines for the management of atrial fibrillation: the task force for the management of atrial fibrillation of the european society of cardiology (ESC). Eur Heart J 31:2369–2429
Lin YK, Chen YJ, Chen SA (2011) Potential atrial arrhythmogenicity of adipocytes: implications for the genesis of atrial fibrillation. Med Hypotheses 74:1026–1029
Friedrichs K, Klinke A, Baldus S (2011) Inflammatory pathways underlying atrial fibrillation. Trends Mol Med 17:556–563
Mazurek T, Zhang L, Zalewski A et al (2003) Human epicardial adipose tissue is a source of inflammatory mediators. Circulation 108:2460–2466
Rosito GA, Massaro JM, Hoffmann U et al (2008) Pericardial fat, visceral abdominal fat, cardiovascular disease risk factors, and vascular calcification in a community-based sample: the framingham heart study. Circulation 117:605–613
Al Chekakie MO, Welles CC, Metoyer R et al (2010) Pericardial fat is independently associated with human atrial fibrillation. J Am Coll Cardiol 56:784–788
Batal O, Schoenhagen P, Shao M et al (2010) Left atrial epicardial adiposity and atrial fibrillation. Circ Arrhythm Electrophysiol 3:230–236
Wong CX, Abed HS, Molaee P et al (2011) Pericardial fat is associated with atrial fibrillation severity and ablation outcome. J Am Coll Cardiol 57:1745–1751
Nagashima K, Okumura Y, Watanabe I et al (2012) Does location of epicardial adipose tissue correspond to endocardial high dominant frequency or complex fractionated atrial electrogram sites during atrial fibrillation? Circ Arrhythm Electrophysiol 5:676–683
Greif M, Von Ziegler F, Wakili R et al (2013) Increased pericardial adipose tissue is correlated with atrial fibrillation and left atrial dilatation. Clin Res Cardiol 102:555–562
Nakanishi K, Fukuda S, Tanaka A et al (2012) Peri-atrial epicardial adipose tissue is associated with new-onset nonvalvular atrial fibrillation. Circ J 76:2748–2754
Austen WG, Edwards JE, Frye RL et al (1975) A reporting system on patients evaluated for coronary artery disease. Report of the Ad Hoc Committee for Grading of Coronary Artery Disease, Council on Cardiovascular Surgery, American Heart Association. Circulation 51:5–40
Girerd N, Scridon A, Bessiere F et al (2013) Periatrial epicardial fat is associated with markers of endothelial dysfunction in patients with atrial fibrillation. PLoS One 8:e77167
Thanassoulis G, Massaro JM, O'Donnell CJ et al (2010) Pericardial fat is associated with prevalent atrial fibrillation: the framingham heart study. Circ Arrhythm Electrophysiol 3:345–350
Tsao HM, Hu WC, Wu MH et al (2011) Quantitative analysis of quantity and distribution of epicardial adipose tissue surrounding the left atrium in patients with atrial fibrillation and effect of recurrence after ablation. Am J Cardiol 107:1498–1503
Shinohara T, Shen MJ, Han S et al (2012) Heart failure decreases nerve activity in the right atrial ganglionated plexus. J Cardiovasc Electrophysiol 23:404–412
Shin SY, Yong HS, Lim HE et al (2011) Total and interatrial epicardial adipose tissues are independently associated with left atrial remodeling in patients with atrial fibrillation. J Cardiovasc Electrophysiol 22:647–655
Kanazawa H, Yamabe H, Enomoto K et al (2014) Importance of pericardial fat in the formation of complex fractionated atrial electrogram region in atrial fibrillation. Int J Cardiol 174:557–564
Yorgun H, Canpolat U, Hazirolan T et al (2012) Epicardial adipose tissue thickness predicts descending thoracic aorta atherosclerosis shown by multidetector computed tomography. Int J Cardiovasc Imaging 28:911–919
Conflict of interest
Authors of this study do not have any conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yorgun, H., Canpolat, U., Aytemir, K. et al. Association of epicardial and peri-atrial adiposity with the presence and severity of non-valvular atrial fibrillation. Int J Cardiovasc Imaging 31, 649–657 (2015). https://doi.org/10.1007/s10554-014-0579-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-014-0579-5