Abstract
Purpose
Populations with high cancer risk that are targeted for screening, education, and vaccination have been shown to increase rates of screening, which ultimately may improve timing of diagnosis and overall outcome for certain cancers. Spatial scan analysis provides a visual representation of areas with higher rates of disease. Limited research has used this methodology to assess HPV-associated cancers. Using, spatial scan statistics, our goal was to identify regions within Kentucky having significantly higher rates of HPV-associated tumors. These regions can be targeted for public health efforts in the form of education, vaccination, screening, and physician recruitment.
Methods
The Kentucky Cancer Registry data from 1995 to 2016 and spatial scan statistics were used to identify county-level clusters with high-incidence of HPV-associated cancers after adjustment for age and sex. Anatomic sites included in this analysis were oropharynx, cervix, anus, penis, and vulva.
Results
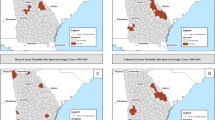
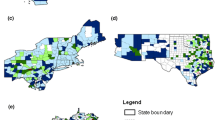
There was one high-rate cluster of oropharyngeal cancer, which was observed in the Louisville metropolitan region (Relative Risk [RR] = 1.24, p < 0.001). One high-rate cluster of anal and penile cancer incidence in men was identified that partially overlapped with the oropharyngeal cluster. There were five clusters of higher cervical, vulvar, and anal cancer incidence in females, one of which overlapped with the oropharyngeal cluster.
Conclusion
Overlapping clusters of HPV-associated cancers were identified at the county-level and included both urban and rural counties of Kentucky. Findings can assist in the design of public health interventions to increase screenings, promote vaccination, and recruit physicians in these regions to improve prevention, diagnosis, and early treatment of HPV-associated cancers.


Similar content being viewed by others
Data availability
Study data available upon request.
References
Saraiya M, Unger ER, Thompson TD et al (2015) US assessment of HPV types in cancers: implications for current and 9-valent HPV vaccines. J Natl Cancer Inst 107:djv086
Petca A, Borislavschi A, Zvanca ME, Petca RC, Sandru F, Dumitrascu MC (2020) Non-sexual HPV transmission and role of vaccination for a better future (review). Exp Ther Med 20:186
McBride AA, Warburton A (2017) The role of integration in oncogenic progression of HPV-associated cancers. PLoS Pathog 13:e1006211
Centers for Disease Control and Prevention (2022) Cancers associated with Human Papillomavirus, United States 2015-2019. Retrieved from: https://www.cdc.gov/cancer/uscs/about/data-briefs/no31-hpv-assoc-cancers-UnitedStates-2015-2019.htm
Saslow D, Castle PE, Cox JT et al (2007) American Cancer Society guideline for human papillomavirus (HPV) vaccine use to prevent cervical cancer and its precursors. CA Cancer J Clin 57:7–28
Tsentemeidou A, Fyrmpas G, Stavrakas M et al (2021) Human papillomavirus vaccine to end oropharyngeal cancer. A systematic review and meta-analysis. Sex Transm Dis 48:700–707
D’Souza G, Dempsey A (2011) The role of HPV in head and neck cancer and review of the HPV vaccine. Prev Med 53(Suppl 1):S5–S11
Centers for Disease Control and Prevention (2018) Cancers associated with Human Papillomavirus by State - 2010-2014. Retrieved from: https://www.cdc.gov/cancer/uscs/about/data-briefs/no2-hpv-assoc-cancers-by-state-2010-2014.htm
Smith EM, Rubenstein LM, Haugen TH, Hamsikova E, Turek LP (2010) Tobacco and alcohol use increases the risk of both HPV-associated and HPV-independent head and neck cancers. Cancer Causes Control 21:1369–1378
Hopenhayn C, Christian A, Christian WJ et al (2014) Prevalence of human papillomavirus types in invasive cervical cancers from 7 US cancer registries before vaccine introduction. J Low Genit Tract Dis 18:182–189
Walker TY, Elam-Evans LD, Yankey D et al (2019) National, regional, state, and selected local area vaccination coverage among adolescents aged 13–17 years—United States, 2018. Morb Mortal Wkly Rep 68:718–723
Hoss A, Meyerson BE, Zimet GD (2019) State statutes and regulations related to human papillomavirus vaccination. Hum Vaccines Immunother 15:1519–1526
Marcus MW, Raji OY, Field JK (2015) Lung cancer screening: identifying the high risk cohort. J Thorac Dis 7:S156–S162
Syrjanen S, Rautava J, Syrjanen K (2017) HPV in head and neck cancer-30 years of history. Recent Results Cancer Res 206:3–25
Mehanna H, Franklin N, Compton N et al (2016) Geographic variation in human papillomavirus-related oropharyngeal cancer: data from 4 multinational randomized trials. Head Neck 38(Suppl 1):E1863–E1869
Kentucky State Data Center (2022) KSC Data Downloads Estimates of Population. Retrieved from: http://ksdc.louisville.edu/data-downloads/estimates/
Gomez-Rubio V, Lopez-Quilez A (2010) Statistical methods for the geographical analysis of rare diseases. Adv Exp Med Biol 686:151–171
Glaz J, Balakrishnan N (1999) Scan statistics and applications. Birkhäuser, Boston
Kulldorff M (1997) A spatial scan statistic. Commun Stat Theory Methods 26:1481–1496
Pytynia KB, Dahlstrom KR, Sturgis EM (2014) Epidemiology of HPV-associated oropharyngeal cancer. Oral Oncol 50:380–386
United States Census Bureau (2023) Quick Facts Kentucky. Retrieved from: https://www.census.gov/quickfacts/KY
Chaturvedi AK, Engels EA, Pfeiffer RM et al (2011) Human papillomavirus and rising oropharyngeal cancer incidence in the United States. J Clin Oncol 29:4294–4301
Zahnd WE, Rodriguez C, Jenkins WD (2019) Rural-urban differences in human papillomavirus-associated cancer trends and rates. J Rural Health 35:208–215
Locklar LRB, Do DP (2022) Rural-urban differences in HPV testing for cervical cancer screening. J Rural Health 38:409–415
Centers for Disease Control and Prevention (2022) Cancers associated with Human Papillomavirus, United States 2015-2019. Retrieved from: https://www.cdc.gov/cancer/uscs/about/data-briefs/no31-hpv-assoc-cancers-UnitedStates-2015-2019.htm
Herrero R, Quint W, Hildesheim A et al (2013) Reduced prevalence of oral human papillomavirus (HPV) 4 years after bivalent HPV vaccination in a randomized clinical trial in Costa Rica. PLoS ONE 8:e68329
Hirth JM, Chang M, Resto VA, Group HPVS (2017) Prevalence of oral human papillomavirus by vaccination status among young adults (18–30 years old). Vaccine 35:3446–3451
Markowitz LE, Gee J, Chesson H, Stokley S (2018) Ten years of human papillomavirus vaccination in the United States. Acad Pediatr 18:S3–S10
Chaturvedi AK, Graubard BI, Broutian T et al (2018) Effect of prophylactic human papillomavirus (HPV) vaccination on oral HPV infections among young adults in the United States. J Clin Oncol 36:262–267
United States Census Bureau (2022) State of Residence by Place of Birth Flows. Retrieved from: https://www.census.gov/data/tables/time-series/demo/geographic-mobility/state-of-residence-place-of-birth-acs.htm
Geronimus AT, Bound J, Ro A (2014) Residential mobility across local areas in the United States and the geographic distribution of the healthy population. Demography 51:777–809
Funding
The authors have no funding to disclose for this study.
Author information
Authors and Affiliations
Contributions
ST—primary manuscript text drafting. FL—primary manuscript text drafting, study design, statistics, table/figure creation. XM—manuscript text drafting, study design, statistics, table/figure creation. WJC—manuscript text drafting, study design, statistics, table/figure creation. BL—manuscript text drafting. AK—manuscript text drafting, study design. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors have no competing interests to disclose.
Ethical approval
The Medical Institutional Review Board at the University of Kentucky reviewed and approved this study (IRB #47508).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Trott, S., Lei, F., Jay Christian, W. et al. Geographic variation of HPV-associated cancer incidence in Kentucky using spatial scan statistics. Cancer Causes Control 35, 817–824 (2024). https://doi.org/10.1007/s10552-023-01835-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-023-01835-3