Abstract
Background
For early-stage cancer surgery is often curative, yet refusal of recommended surgical interventions may be contributing to disparities in patient treatment. This study aims to assess predictors of early-stage cancers surgery refusal, and the impact on survival.
Methods
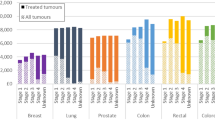
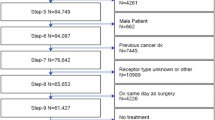
Patients recommended surgery with primary stage I and II lung, prostate, breast, and colon cancers, diagnosed between 2007–2014, were identified in the Surveillance, Epidemiology and End Results database (n = 498,927). Surgery refusal was reported for 5,757 (1.2%) patients. Associations between sociodemographic variables and surgery refusal by cancer type were assessed in adjusted multivariable logistic regression models. The impact of refusal on survival was investigated using adjusted Cox-Proportional Hazard regression in a propensity score-matched cohort.
Results
Increasing age (p < 0.0001 for all four cancer types), non-Hispanic Black race/ethnicity (ORadjBREAST 2.00, 95% CI 1.68–2.39; ORadjCOLON 3.04, 95% CI 2.17–4.26; ORadjLUNG 2.19, 95% CI 1.77–2.71; ORadjPROSTATE 2.02, 95% CI 1.86–2.20; vs non-Hispanic White), insurance status (uninsured: ORadjBREAST 2.75, 95% CI 1.89–3.99; ORadjPROSTATE 2.10, 95% CI 1.72–2.56; vs insured), marital status (ORadjBREAST 2.16, 95% CI 1.85–2.51; ORadjCOLON 1.56, 95% CI 1.16–2.10; ORadjLUNG 2.11, 95% CI 1.80–2.47; ORadjPROSTATE 1.94, 95% CI 1.81–2.09), and stage (ORadjBREAST 1.94, 95% CI 1.70–2.22; ORadjCOLON 0.13, 95% CI 0.09–0.18; ORadjLUNG 0.71, 95% CI 0.52–0.96) were all associated with refusal; patients refusing surgery were at increased risk of death compared to patients who underwent surgery.
Conclusions
More vulnerable patients are at higher risk of refusing recommended surgery, and this decision negatively impacts their survival.


Similar content being viewed by others
References
SEER Cancer Statistics Review, 1975–2015. SEER. [cited 2019 Mar 1]. https://seer.cancer.gov/csr/1975_2015/index.html
Lund MJ, Brawley OP, Ward KC, Young JL, Gabram SSG, Eley JW (2008) Parity and disparity in first course treatment of invasive breast cancer. Breast Cancer Res Treat 109(3):545–557
Akinyemiju T, Meng Q, Vin-Raviv N (2016) Race/ethnicity and socio-economic differences in colorectal cancer surgery outcomes: analysis of the nationwide inpatient sample. BMC Cancer 16:715
Taioli E, Flores R (2017) Appropriateness of surgical approach in black patients with lung cancer-15 years later, little has changed. J Thorac Oncol 12(3):573–577
Wolf A, Alpert N, Tran BV, Liu B, Flores R, Taioli E (2018) Persistence of racial disparities in early-stage lung cancer treatment. J Thorac Cardiovasc Surg 157:1670–1679
Groth SS, Al-Refaie WB, Zhong W, Vickers SM, Maddaus MA, D’Cunha J et al (2013) Effect of insurance status on the surgical treatment of early-stage non-small cell lung cancer. Ann Thorac Surg 95(4):1221–1226
Wu Y, Ai Z, Xu G (2017) Marital status and survival in patients with non-small cell lung cancer: an analysis of 70006 patients in the SEER database. Oncotarget 8(61):103518–103534
Aizer AA, Chen M-H, Parekh A, Choueiri TK, Hoffman KE, Kim SP et al (2014) Refusal of curative radiation therapy and surgery among patients with cancer. Int J Radiat Oncol Biol Phys 89(4):756–764
Gaitanidis A, Alevizakos M, Tsalikidis C, Tsaroucha A, Simopoulos C, Pitiakoudis M (2018) Refusal of cancer-directed surgery by breast cancer patients: risk factors and survival outcomes. Clin Breast Cancer 18(4):e469–e476
Zients J (2015) Revised delineations of metropolitan statistical areas, micropolitan statistical areas, and combined statistical areas, and guidance on uses of the delineations of these areas. Office of Management and Budget, Washington
Margolis ML, Christie JD, Silvestri GA, Kaiser L, Santiago S, Hansen-Flaschen J (2003) Racial differences pertaining to a belief about lung cancer surgery: results of a multicenter survey. Ann Intern Med 139(7):558–563
Boulware LE, Cooper LA, Ratner LE, LaVeist TA, Powe NR (2003) Race and trust in the health care system. Public Health Rep 118(4):358–365
Gopal N, Kozikowski A, Barginear MF, Fishbein J, Pekmezaris R, Wolf-Klein G (2017) Reasons for chemotherapy refusal or acceptance in older adults with cancer. South Med J. 110(1):47–53
Aizer AA, Chen M-H, McCarthy EP, Mendu ML, Koo S, Wilhite TJ et al (2013) Marital status and survival in patients with cancer. J Clin Oncol. 31(31):3869–3876
Bertakis KD, Azari R, Helms LJ, Callahan EJ, Robbins JA (2000) Gender differences in the utilization of health care services. J Fam Pract 49:147–152
Keene J, Li X (2005) Age and gender differences in health service utilization. J. Public Health 27:74–79
Huchcroft SA, Snodgrass T (1993) Cancer patients who refuse treatment. Cancer Causes Control 4:179–185
Rahouma M, Harrison S, Kamel M et al (2018) Consequences of refusing surgery for esophageal cancer: a national cancer database analysis. Ann Thorac Surg 106:1476–1483
Johnson SB, Park HS, Gross CP, Yu JB (2018) Complementary medicine, refusal of conventional cancer therapy, and survival among patients with curable cancers. JAMA Oncol 4(10):1375–1381. https://doi.org/10.1001/jamaoncol.2018.2487
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Rapp, J., Tuminello, S., Alpert, N. et al. Disparities in surgery for early-stage cancer: the impact of refusal. Cancer Causes Control 30, 1389–1397 (2019). https://doi.org/10.1007/s10552-019-01240-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-019-01240-9