Abstract
Purpose
Vitamin D has been implicated in lowering lung cancer risk, but serological data on the association among never-smoking women are limited. We report results examining the association of serum 25-hydroxyvitamin D [25(OH)D] concentrations with lung cancer risk among female never smokers. We also examined whether the association was modified by vitamin D supplementation and serum vitamin A concentrations.
Methods
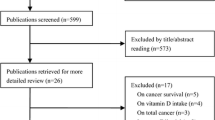
In the Women’s Health Initiative, including the calcium/vitamin D (CaD) Trial, we selected 298 incident cases [191 non-small cell lung cancer (NSCLC) including 170 adenocarcinoma] and 298 matched controls of never smokers. Baseline serum 25(OH)D was assayed by a chemiluminescent method. Logistic regression was used to estimate odds ratios (ORs) for quartiles and predefined clinical cutoffs of serum 25(OH)D concentrations.
Results
Comparing quartiles 4 versus 1 of serum 25(OH)D concentrations, ORs were 1.06 [95% confidence interval (CI) 0.61–1.84] for all lung cancer, 0.94 (95% CI 0.52–1.69) for NSCLC, and 0.91 (95% CI 0.49–1.68) for adenocarcinoma. Comparing serum 25(OH)D ≥ 75 (high) versus <30 nmol/L (deficient), ORs were 0.76 (95% CI 0.31–1.84) for all lung cancer, 0.71 (95% CI 0.27–1.86) for NSCLC, and 0.81 (95% CI 0.31–2.14) for adenocarcinoma. There is suggestive evidence that CaD supplementation (1 g calcium + 400 IU D3/day) and a high level of circulating vitamin A may modify the associations of 25(OH)D with lung cancer overall and subtypes (p interaction <0.10).
Conclusions
In this group of never-smoking postmenopausal women, the results did not support the hypothesis of an association between serum 25(OH)D and lung cancer risk.
Similar content being viewed by others
References
Samet JM, Avila-Tang E, Boffetta P et al (2009) Lung cancer in never smokers: clinical epidemiology and environmental risk factors. Clin Cancer Res 15:5626–5645
Menezes RJ, Cheney RT, Husain A et al (2008) Vitamin D receptor expression in normal, premalignant, and malignant human lung tissue. Cancer Epidemiol Biomarkers Prev 17:1104–1110
Hansdottir S, Monick MM, Hinde SL, Lovan N, Look DC, Hunninghake GW (2008) Respiratory epithelial cells convert inactive vitamin D to its active form: potential effects on host defense. J Immunol (Baltimore Md 1950) 181:7090–7099
Holick MF (2007) Vitamin D deficiency. N Engl J Med 357:266–281
Deeb KK, Trump DL, Johnson CS (2007) Vitamin D signalling pathways in cancer: potential for anticancer therapeutics. Nat Rev Cancer 7:684–700
Carlberg C, Bendik I, Wyss A et al. (1993) Two nuclear signaling pathways for vitamin D. Nature 361:657–360
Pereira F, Larriba MJ, Munoz A (2012) Vitamin D and colon cancer. Endocr Relat Cancer 19:R51–R71
Kilkkinen A, Knekt P, Heliövaara M et al (2008) Vitamin D status and the risk of lung cancer: a cohort study in Finland. Cancer Epidemiol Biomarkers Prev 17:3274–3278
Freedman DM, Looker AC, Abnet CC, Linet MS, Graubard BI (2010) Serum vitamin D and cancer mortality in the NHANES III Study (1988–2006). Cancer Res 70:8587–8597
Cheng TY, Neuhouser ML (2012) Serum 25-hydroxyvitamin D, interaction with vitamin A and lung cancer mortality in the U.S. population. Cancer Causes Control 23:1557–1565
Giovannucci E, Liu Y, Rimm EB et al (2006) Prospective study of predictors of vitamin D status and cancer incidence and mortality in men. J Natl Cancer Inst 98:451–459
Weinstein SJ, Yu K, Horst RL, Parisi D, Virtamo J, Albanes D (2011) Serum 25-hydroxyvitamin d and risk of lung cancer in male smokers: a nested case–control study. PLoS ONE 6:e20796
Skaaby T, Husemoen LL, Thuesen BH et al (2014) Prospective population-based study of the association between serum 25-hydroxyvitamin-D levels and the incidence of specific types of cancer. Cancer Epidemiol Biomarkers Prev 23:1220–1229
Ordonez-Mena JM, Schottker B, Haug U et al. (2013) Serum 25-hydroxyvitamin d and cancer risk in older adults: results from a large German prospective cohort study. Cancer Epidemiol Biomarkers Prev 22:905–916
Ordonez-Mena JM, Schottker B, Fedirko V et al. (2015) Pre-diagnostic vitamin D concentrations and cancer risks in older individuals: an analysis of cohorts participating in the CHANCES consortium. Eur J Epidemiol. doi:10.1007/s10654-015-0040-7
Afzal S, Bojesen SE, Nordestgaard BG. (2013) Low plasma 25-hydroxyvitamin D and risk of tobacco-related cancer. Clin Chem 59:771–780
Wong YY, Hyde Z, McCaul KA et al (2014) In older men, lower plasma 25-hydroxyvitamin D is associated with reduced incidence of prostate, but not colorectal or lung cancer. PLoS ONE 9:e99954
Chen GC, Zhang ZL, Wan Z et al (2015) Circulating 25-hydroxyvitamin D and risk of lung cancer: a dose-response meta-analysis. Cancer Causes Control 26:1719–1728
The Women’s Health Initiative Study Group (1998) Design of the Women’s Health Initiative clinical trial and observational study. Control Clin Trials 19:61–109
Jackson RD, LaCroix AZ, Gass M et al. (2006) Calcium plus vitamin D supplementation and the risk of fractures. N Engl J Med 354:669–683
Wactawski-Wende J, Kotchen JM, Anderson GL et al. (2006) Calcium plus vitamin D supplementation and the risk of colorectal cancer. N Engl J Med 354:684–696
Hays J, Hunt JR, Hubbell FA et al (2003) The Women’s Health Initiative recruitment methods and results. Ann Epidemiol 13:S18–S77
Curb JD, McTiernan A, Heckbert SR et al (2003) Outcomes ascertainment and adjudication methods in the Women’s Health Initiative. Ann Epidemiol 13:S122-8
Luo J, Margolis KL, Wactawski-Wende J et al (2011) Association of active and passive smoking with risk of breast cancer among postmenopausal women: a prospective cohort study. BMJ 342:d1016
Bondy SJ, Victor JC, Diemert LM. (2009) Origin and use of the 100 cigarette criterion in tobacco surveys. Tob Control 18:317–323
Krasinski SD, Russell RM, Otradovec CL et al. (1989) Relationship of vitamin A and vitamin E intake to fasting plasma retinol, retinol-binding protein, retinyl esters, carotene, alpha-tocopherol, and cholesterol among elderly people and young adults: increased plasma retinyl esters among vitamin A-supplement users. Am J Clin Nutr 49:112–120
Ballew C, Galuska D, Gillespie C (2001) High serum retinyl esters are not associated with reduced bone mineral density in the Third National Health And Nutrition Examination Survey, 1988–1994. J Bone Miner Res 16:2306–2312
Bauer SR, Richman EL, Sosa E et al (2013) Antioxidant and vitamin E transport genes and risk of high-grade prostate cancer and prostate cancer recurrence. Prostate 73:1786–1795
Patterson RE, Kristal AR, Tinker LF, Carter RA, Bolton MP, Agurs-Collins T (1999) Measurement characteristics of the Women’s Health Initiative food frequency questionnaire. Ann Epidemiol 9:178–187
Patterson RE, Levy L, Tinker LF, Kristal AR (1999) Evaluation of a simplified vitamin supplement inventory developed for the Women’s Health Initiative. Public Health Nutr 2:273–276
Wang Y, Jacobs EJ, McCullough ML et al (2009) Comparing methods for accounting for seasonal variability in a biomarker when only a single sample is available: insights from simulations based on serum 25-hydroxyvitamin d. Am J Epidemiol 170:88–94
Institute of Medicine (2011) Dietary reference intake for calcium and vitamin D. The National Academics Press, Washington, DC
Bischoff-Ferrari HA, Giovannucci E, Willett WC, Dietrich T, Dawson-Hughes B (2006) Estimation of optimal serum concentrations of 25-hydroxyvitamin D for multiple health outcomes. Am J Clin Nutr 84:18–28
Maldonado G, Greenland S (1993) Simulation study of confounder-selection strategies. Am J Epidemiol 138:923–936
Cheng TY, Millen AE, Wactawski-Wende J et al (2014) Vitamin D intake determines vitamin d status of postmenopausal women, particularly those with limited sun exposure. J Nutr 144:681–689
Schnatz PF, Jiang X, Vila-Wright S et al. (2014) Calcium/vitamin D supplementation, serum 25-hydroxyvitamin D concentrations, and cholesterol profiles in the Women’s Health Initiative calcium/vitamin D randomized trial. Menopause 21:823–833
Giovannucci E (2007) Can vitamin D reduce total mortality? Arch Intern Med 167:1709–1710
Brunner RL, Wactawski-Wende J, Caan BJ et al. (2011) The effect of calcium plus vitamin D on risk for invasive cancer: results of the Women’s Health Initiative (WHI) calcium plus vitamin D randomized clinical trial. Nutr Cancer 63:827–841
Pradhan AD, Manson JE (2016) Update on the vitamin D and omega-3 trial (VITAL). J Steroid Biochem Mol Biol 155:252–256
Cheng TY, Lacroix AZ, Beresford SA et al (2013) Vitamin D intake and lung cancer risk in the Women’s Health Initiative. Am J Clin Nutr 98:1002–1011
Zhang Q, Kanterewicz B, Shoemaker S et al. (2013) Differential response to 1alpha,25-dihydroxyvitamin D(3) (1alpha,25(OH)(2)D(3)) in non-small cell lung cancer cells with distinct oncogene mutations. J Steroid Biochem Mol Biol 136:264–270
Tong WM, Hofer H, Ellinger A, Peterlik M, Cross HS (1999) Mechanism of antimitogenic action of vitamin D in human colon carcinoma cells: relevance for suppression of epidermal growth factor-stimulated cell growth. Oncol Res 11:77–84
Herbst RS, Heymach JV, Lippman SM (2008) Lung cancer. N Engl J Med 359:1367–1380
Kaiser U, Schilli M, Wegmann B et al (1996) Expression of vitamin D receptor in lung cancer. J Cancer Res Clin Oncol 122:356–359
Cheng TY, Goodman GE, Thornquist MD et al (2014) Estimated intake of vitamin D and its interaction with vitamin A on lung cancer risk among smokers. Int J Cancer 135:2135–2145
Cheng TY, Cramb SM, Baade PD, Youlden DR, Nwogu C, Reid ME (2016) The international epidemiology of lung cancer: latest trends, disparities, and tumor characteristics. J Thorac Oncol 11:1653–1671
Sun S, Schiller JH, Gazdar AF. (2007) Lung cancer in never smokers–a different disease. Nat Rev Cancer 7:778–790
Meng JE, Hovey KM, Wactawski-Wende J et al. (2012) Intraindividual variation in plasma 25-hydroxyvitamin D measures 5 years apart among postmenopausal women. Cancer Epidemiol Biomarkers Prev 21:916–924
Acknowledgments
We thank Xiaojun Hu and Pamela Y. Yang for their technical assistance with the lab assays and Hui-Chun Tammy Hsu for her statistical assistance. We also thank WHI participants and the Program Office; Jacques Rossouw, Shari Ludlam, Joan McGowan, Leslie Ford, and Nancy Geller (National Heart, Lung, and Blood Institute, Bethesda, MD); Garnet Anderson, Ross Prentice, Andrea LaCroix, and Charles Kooperberg (the Clinical Coordinating Center at Fred Hutchinson Cancer Research Center, Seattle, WA); the Investigators and Academic Centers; JoAnn E Manson (Brigham and Women’s Hospital, Harvard Medical School, Boston, MA); Barbara V Howard (MedStar Health Research Institute/Howard University, Washington, DC); Marcia L Stefanick (Stanford Prevention Research Center, Stanford, CA); Rebecca Jackson (The Ohio State University, Columbus, OH); Cynthia A Thomson (University of Arizona, Tucson/Phoenix, AZ); Marian Limacher (University of Florida, Gainesville/Jacksonville, FL); Robert Wallace (University of Iowa, Iowa City/Davenport, IA); Lewis Kuller (University of Pittsburgh, Pittsburgh, PA); Sally Shumaker (Wake Forest University School of Medicine, Winston-Salem, NC).
Funding
This work was supported by NIH/NCI grants R03CA167696 and K07CA201334. The WHI program is funded by the National Heart, Lung, and Blood Institute, NIH, US Department of Health and Human Services through contracts HHSN268201100046C, HHSN268201100001C, HHSN268201100002C, HSN268201100003C, HHSN268201100004C, and HHSN271201100004C.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There are no conflicts of interest to disclose.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Cheng, TY.D., Song, X., Beresford, S.A.A. et al. Serum 25-hydroxyvitamin D concentrations and lung cancer risk in never-smoking postmenopausal women. Cancer Causes Control 28, 1053–1063 (2017). https://doi.org/10.1007/s10552-017-0956-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-017-0956-1