Abstract
Purpose
In an effort to explain racial disparities in breast cancer survival, this study aimed to investigate how comorbidity affects breast cancer-specific mortality by race.
Methods
A retrospective cohort study was conducted using the Surveillance, Epidemiology and End Results—Medicare linked data including 68,090 women 66+ years, who were diagnosed with stage I–III breast cancer in the United States from 1994 to 2004. Hospital and outpatient claims from the year prior to breast cancer diagnosis were used to identify comorbid conditions and patients were followed for survival through 2010.
Results
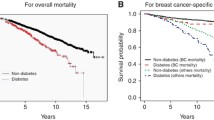
Competing risk survival analysis failed to demonstrate any negative comorbidity effects on breast cancer-specific survival for black women. An increased breast cancer-specific mortality hazard was observed for white women who had diabetes without complication relative to white women without this condition after adjusting for age and year of diagnosis (hazard ratio: 1.22, 95% confidence interval 1.13, 1.30). The Cochran–Armitage Test showed diabetes was associated with a later stage of diagnosis (p < 0.01) and a more aggressive tumor grade (p < 0.01) among white women in the study population.
Conclusion
Race specific comorbidity effects do not explain breast cancer-specific survival disparities. However, the relationship between diabetes and breast cancer, including the role of aggressive tumor characteristics, warrants special attention.

Similar content being viewed by others
References
Ooi SL, Martinez ME, Li CI (2011) Disparities in breast cancer characteristics and outcomes by race/ethnicity. Breast Cancer Res Treat 127(3):729–738. doi:10.1007/s10549-010-1191-6
DeSantis CE, Fedewa SA, Goding Sauer A, Kramer JL, Smith RA, Jemal A (2016) Breast cancer statistics, 2015: convergence of incidence rates between black and white women. CA Cancer J Clin 66(1):31–42. doi:10.3322/caac.21320
Daly B, Olopade OI (2015) A perfect storm: how tumor biology, genomics, and health care delivery patterns collide to create a racial survival disparity in breast cancer and proposed interventions for change. CA Cancer J Clin 65(3):221–238. doi:10.3322/caac.21271
Howlader NNA, Krapcho M, Garshell J, Miller D, Altekruse SF, Kosary CL, Yu M, Ruhl J, Tatalovich Z,Mariotto A, Lewis DR, Chen HS, Feuer EJ, Cronin KA SEER Cancer Statistics Review, 1975–2012. National Cancer Institute, Bethesda, MD
Land LH, Dalton SO, Jorgensen TL, Ewertz M (2012) Comorbidity and survival after early breast cancer, A review. Crit Rev Oncol Hematol 81(2):196–205. doi:10.1016/j.critrevonc.2011.03.001
Schonberg MA, Marcantonio ER, Li D, Silliman RA, Ngo L, McCarthy EP (2010) Breast cancer among the oldest old: tumor characteristics, treatment choices, and survival. J Clin Oncol 28(12):2038–2045. doi:10.1200/JCO.2009.25.9796
Dalton SO, Ross L, During M, Carlsen K, Mortensen PB, Lynch J, Johansen C (2007) Influence of socioeconomic factors on survival after breast cancer—a nationwide cohort study of women diagnosed with breast cancer in Denmark 1983–1999. Int J Cancer 121(11):2524–2531. doi:10.1002/ijc.22979
Patnaik JL, Byers T, DiGuiseppi C, Dabelea D, Denberg TD (2011) Cardiovascular disease competes with breast cancer as the leading cause of death for older females diagnosed with breast cancer: a retrospective cohort study. Breast Cancer Res 13(3):R64. doi:10.1186/bcr2901
Izano M, Satariano WA, Tammemagi MC, Ragland D, Moore DH, Allen E, Naeim A, Sehl ME, Hiatt RA, Kerlikowske K, Sofrygin O, Braithwaite D (2014) Long-term outcomes among African–American and white women with breast cancer: what is the impact of comorbidity? J Geriatr Oncol 5(3):266–275. doi:10.1016/j.jgo.2014.02.003
Ward BW, Schiller JS, Goodman RA (2014) Multiple chronic conditions among US adults: a 2012 update. Prev Chronic Dis 11:E62. doi:10.5888/pcd11.130389
Overview of the SEER Program. National Cancer Institute. http://seer.cancer.gov/about/overview.html. Accessed 29 Mar 2015
Warren JL, Klabunde CN, Schrag D, Bach PB, Riley GF (2002) Overview of the SEER-medicare data: content, research applications, and generalizability to the United States elderly population. Med Care 40 (8 Suppl):IV-3-18. doi:10.1097/01.MLR.0000020942.47004.03
Klabunde CN, Legler JM, Warren JL, Baldwin LM, Schrag D (2007) A refined comorbidity measurement algorithm for claims-based studies of breast, prostate, colorectal, and lung cancer patients. Ann Epidemiol 17(8):584–590. doi:10.1016/j.annepidem.2007.03.011
Sarfati D (2012) Review of methods used to measure comorbidity in cancer populations: no gold standard exists. J Clin Epidemiol 65(9):924–933. doi:10.1016/j.jclinepi.2012.02.017
Klabunde CN, Potosky AL, Legler JM, Warren JL (2000) Development of a comorbidity index using physician claims data. J Clin Epidemiol 53(12):1258–1267
Deyo RA, Cherkin DC, Ciol MA (1992) Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol 45(6):613–619
Romano PS, Roos LL, Jollis JG (1993) Adapting a clinical comorbidity index for use with ICD-9-CM administrative data: differing perspectives. J Clin Epidemiol 46(10):1075–1079
Comorbidity SAS Macro (2000 version). National Cancer Institute. https://healthcaredelivery.cancer.gov/seermedicare/considerations/macro-2000.html
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40(5):373–383
Kwan ML, Haque R, Lee VS, Joanie Chung WL, Avila CC, Clancy HA, Quinn VP, Kushi LH (2012) Validation of AJCC TNM staging for breast tumors diagnosed before 2004 in cancer registries. Cancer Causes Control 23(9):1587–1591. doi:10.1007/s10552-012-0026-7
Putter H, Fiocco M, Geskus RB (2007) Tutorial in biostatistics: competing risks and multi-state models. Stat Med 26(11):2389–2430. doi:10.1002/sim.2712
Gray RJ (1988) A class of K-sample tests for comparing the cumulative incidence of a competing risk. Ann Stat 16(3):1141–1154
Fine JG, Gray RJ (1999) A proportional hazards model for the subdistribution of a competing risk. J Am Stat Assoc 94(446):469–509
Wu AH, Kurian AW, Kwan ML, John EM, Lu Y, Keegan TH, Gomez SL, Cheng I, Shariff-Marco S, Caan BJ, Lee VS, Sullivan-Halley J, Tseng CC, Bernstein L, Sposto R, Vigen C (2015) Diabetes and other comorbidities in breast cancer survival by race/ethnicity: the California Breast Cancer Survivorship Consortium (CBCSC). Cancer Epidemiol Biomark Prev 24(2):361–368. doi:10.1158/1055-9965.EPI-14-1140
Luo J, Hendryx M, Virnig B, Wen S, Chlebowski R, Chen C, Rohan T, Tinker L, Wactawski-Wende J, Lessin L, Margolis KL (2015) Pre-existing diabetes and breast cancer prognosis among elderly women. Br J Cancer 113(5):827–832. doi:10.1038/bjc.2015.249
Beckman TJ, Cuddihy RM, Scheitel SM, Naessens JM, Killian JM, Pankratz VS (2001) Screening mammogram utilization in women with diabetes. Diabetes Care 24(12):2049–2053
Peairs KS, Barone BB, Snyder CF, Yeh HC, Stein KB, Derr RL, Brancati FL, Wolff AC (2011) Diabetes mellitus and breast cancer outcomes: a systematic review and meta-analysis. J Clin Oncol 29(1):40–46. doi:10.1200/JCO.2009.27.3011
Rose DP, Haffner SM, Baillargeon J (2007) Adiposity, the metabolic syndrome, and breast cancer in African–American and white American women. Endocr Rev 28(7):763–777. doi:10.1210/er.2006-0019
Ferroni P, Riondino S, Laudisi A, Portarena I, Formica V, Alessandroni J, D’Alessandro R, Orlandi A, Costarelli L, Cavaliere F, Guadagni F, Roselli M (2016) Pretreatment insulin levels as a prognostic factor for breast cancer progression. Oncologist. doi:10.1634/theoncologist.2015-0462
Nam S, Park S, Park HS, Kim S, Kim JY, Kim SI (2016) Association between insulin resistance and luminal B subtype breast cancer in postmenopausal women. Medicine (Baltimore) 95(9):e2825. doi:10.1097/MD.0000000000002825
Holmes MD, Chen WY (2012) Hiding in plain view: the potential for commonly used drugs to reduce breast cancer mortality. Breast Cancer Res 14(2):216. doi:10.1186/bcr3336
Vaklavas C, Chatzizisis YS, Tsimberidou AM (2011) Common cardiovascular medications in cancer therapeutics. Pharmacol Ther 130(2):177–190. doi:10.1016/j.pharmthera.2011.01.009
Vendramini-Costa DB, Carvalho JE (2012) Molecular link mechanisms between inflammation and cancer. Curr Pharm Des 18(26):3831–3852
Vinayak S, Kurian AW (2009) Statins may reduce breast cancer risk, particularly hormone receptor-negative disease. Curr Breast Cancer Rep 1(3):148–156. doi:10.1007/s12609-009-0021-5
Bo S, Benso A, Durazzo M, Ghigo E (2012) Does use of metformin protect against cancer in Type 2 diabetes mellitus? J Endocrinol Invest 35(2):231–235
Powe DG, Voss MJ, Zanker KS, Habashy HO, Green AR, Ellis IO, Entschladen F (2010) Beta-blocker drug therapy reduces secondary cancer formation in breast cancer and improves cancer specific survival. Oncotarget 1(7):628–638
Melhem-Bertrandt A, Chavez-Macgregor M, Lei X, Brown EN, Lee RT, Meric-Bernstam F, Sood AK, Conzen SD, Hortobagyi GN, Gonzalez-Angulo AM (2011) Beta-blocker use is associated with improved relapse-free survival in patients with triple-negative breast cancer. J Clin Oncol 29(19):2645–2652. doi:10.1200/JCO.2010.33.4441
Barron TI, Connolly RM, Sharp L, Bennett K, Visvanathan K (2011) Beta blockers and breast cancer mortality: a population- based study. J Clin Oncol 29(19):2635–2644. doi:10.1200/JCO.2010.33.5422
Barron TI, Sharp L, Visvanathan K (2012) Beta-adrenergic blocking drugs in breast cancer: a perspective review. Ther Adv Med Oncol 4(3):113–125. doi:10.1177/1758834012439738,10.1177_1758834012439738
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL, Jr., Jones DW, Materson BJ, Oparil S, Wright JT, Jr., Roccella EJ, Joint National Committee on Prevention DE, Treatment of High Blood Pressure. National Heart L, Blood I, National High Blood Pressure Education Program Coordinating C (2003) Seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension 42(6):1206–1252. doi:10.1161/01.HYP.0000107251.49515.c2
Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (1997) The sixth report of the Joint National Committee on prevention, detection, evaluation, and treatment of high blood pressure. Arch Intern Med 157(21):2413–2446
Rao S, Cherukuri M, Mayo HG, Sehgal M (2007) Clinical inquiries. What is the best treatment for hypertension in African Americans? J Fam Pract 56(2):149–151
Braithwaite D, Tammemagi CM, Moore DH, Ozanne EM, Hiatt RA, Belkora J, West DW, Satariano WA, Liebman M, Esserman L (2009) Hypertension is an independent predictor of survival disparity between African-American and white breast cancer patients. Int J Cancer 124(5):1213–1219. doi:10.1002/ijc.24054
Olson SH, Atoria CL, Cote ML, Cook LS, Rastogi R, Soslow RA, Brown CL, Elkin EB (2012) The impact of race and comorbidity on survival in endometrial cancer. Cancer Epidemiol Biomark Prev 21(5):753–760. doi:10.1158/1055-9965.EPI-11-0735
Ruterbusch JJ, Ali-Fehmi R, Olson SH, Sealy-Jefferson S, Rybicki BA, Hensley-Alford S, Elshaikh MA, Gaba AR, Schultz D, Munkarah AR, Cote ML (2014) The influence of comorbid conditions on racial disparities in endometrial cancer survival. Am J Obstet Gynecol. doi:10.1016/j.ajog.2014.06.036
McDonald M, Hertz RP, Unger AN, Lustik MB (2009) Prevalence, awareness, and management of hypertension, dyslipidemia, and diabetes among United States adults aged 65 and older. J Gerontol A 64(2):256–263. doi:10.1093/gerona/gln016
Yang Y, Mauldin PD, Ebeling M, Hulsey TC, Liu B, Thomas MB, Camp ER, Esnaola NF (2013) Effect of metabolic syndrome and its components on recurrence and survival in colon cancer patients. Cancer 119(8):1512–1520. doi:10.1002/cncr.27923
Mansourian M, Haghjooy-Javanmard S, Eshraghi A, Vaseghi G, Hayatshahi A, Thomas J (2016) Statins use and risk of breast cancer recurrence and death: a systematic review and meta-analysis of observational studies. J Pharm Pharm Sci 19(1):72–81. doi:10.18433/J3202B
Quan H, Sundararajan V, Halfon P, Fong A, Burnand B, Luthi JC, Saunders LD, Beck CA, Feasby TE, Ghali WA (2005) Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med Care 43(11):1130–1139
Griffiths RI, Gleeson ML, Valderas JM, Danese MD (2014) Impact of undetected comorbidity on treatment and outcomes of breast cancer. Int J Breast Cancer 2014:970780. doi:10.1155/2014/970780
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Dr. Steinberg received $500 from Arena Pharmaceuticals as a consultant in March 2015.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this type of study, formal consent is not required. This article does not contain any studies with animals performed by any of the authors.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Santorelli, M.L., Hirshfield, K.M., Steinberg, M.B. et al. Racial differences in the effects of comorbidity on breast cancer-specific survival. Cancer Causes Control 28, 809–817 (2017). https://doi.org/10.1007/s10552-017-0915-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-017-0915-x