Abstract
Purpose
A relationship of Epstein–Barr virus (EBV) and breast cancer etiology and outcome may have clinical utility and potential to enhance understanding of tumor biology. Research to date has yielded variable results, likely reflecting differing virus detection assays and unaddressed epidemiologic heterogeneity across studies.
Methods
Applying our novel, five-target assay detection strategy in an exploratory study, we examined demographic, clinical, and tumor characteristics, and overall survival, associated with EBV positivity in breast adenocarcinomas from 59 non-Hispanic white and 68 Hispanic women sampled by age (<50, 50+) and stage (localized, regional/remote) and examined associations based on single assay targets.
Results
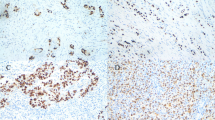
EBV was localized only to lymphocytes. Nevertheless, viral prevalence, although low, varied across patient subgroups. Adjusted odds ratios (OR) for EBV positivity were lower for younger Hispanic than white women (p interaction = 0.05), and marginally higher for larger [OR (95% confidence intervals) 1.03 (1.00–1.05) per mm increase] and right-sided [2.8 (0.97–7.8)] tumors. In whites, ORs were marginally higher for larger tumors [1.04 (1.00–1.07)] and marginally lower for age 50+ [0.24 (0.06–1.03)]; in Hispanics, ORs were higher for ER negative [5.6 (1.1–30.5)], and marginally higher for right-sided, tumors [5.8 (0.94–36.2)]. Survival was suggestively poorer for EBV-positive than EBV-negative tumors in older women with localized disease. EBV associations differed across single assay targets, indicating variation in prior findings likely due to assay performance.
Conclusions
The differing EBV associations by age and race/ethnicity suggest a non-random role of EBV in breast cancer and support further study using multi-target assays, relevant epidemiologic design, and a larger study sample.


Similar content being viewed by others
References
Huo Q, Zhang N, Yang Q (2012) Epstein–Barr virus infection and sporadic breast cancer risk: a meta-analysis. PLoS One 7:e31656
Joshi D, Buehring GC (2012) Are viruses associated with human breast cancer? Scrutinizing the molecular evidence. Breast Cancer Res Treat 135:1–15
Richardson AK, Currie MJ, Robinson BA et al (2015) Cytomegalovirus and Epstein–Barr virus in breast cancer. PLoS One 10:e0118989
Glaser SL, Hsu JL, Gulley ML (2004) Epstein–Barr virus and breast cancer: state of the evidence for viral carcinogenesis. Cancer Epidemiol Biomarkers Prev 13:688–697
Zekri AR, Bahnassy AA, Mohamed WS et al (2012) Epstein–Barr virus and breast cancer: epidemiological and molecular study on Egyptian and Iraqi women. J Egypt Natl Canc Inst 24:123–131
Rickinson AB (2014) Co-infections, inflammation and oncogenesis: future directions for EBV research. Semin Cancer Biol 26:99–115
Corbex M, Bouzbid S, Traverse-Glehen A et al (2014) Prevalence of papillomaviruses, polyomaviruses, and herpesviruses in triple-negative and inflammatory breast tumors from Algeria compared with other types of breast cancer tumors. PLoS One 9:e114559
Gyu Lee H, Kim H, Jung Kim E et al. (2015) Targeted therapy for Epstein–Barr virus-associated gastric carcinoma using low-dose gemcitabine-induced lytic activation. Oncotarget 6:31018–31029
Stoker S, Novalić Z, Wildeman M et al (2015) Epstein–Barr virus-targeted therapy in nasopharyngeal carcinoma. J Cancer Res Clin Oncol 141:1845–1857
Tse E, Kwong Y-L (2015) Epstein Barr virus-associated lymphoproliferative diseases: the virus as a therapeutic target. Exp Mol Med 47:e136
Murray PG (2006) Epstein–Barr virus in breast cancer: artefact or aetiological agent? J Pathol 209:427–429
Ransohoff DF, Gourlay ML (2010) Sources of bias in specimens for research about molecular markers for cancer. J Clin Oncol 28:698–704
Bonnet M, Guinebretiere JM, Kremmer E et al (1999) Detection of Epstein–Barr virus in invasive breast cancers. J Natl Cancer Inst 91:1376–1381
Fina F, Romain S, Ouafik L et al (2001) Frequency and genome load of Epstein–Barr virus in 509 breast cancers from different geographical areas. Br J Cancer 84:783–790
Joshi D, Quadri M, Gangane N, Joshi R, Gangane N (2009) Association of Epstein Barr virus infection (EBV) with breast cancer in rural Indian women. PLoS One 4:e8180
DeSantis C, Ma J, Bryan L, Jemal A (2014) Breast cancer statistics, 2013. CA Cancer J Clin 64:52–62
Hung MC, Ekwueme DU, Rim SH, White A (2016) Racial/ethnicity disparities in invasive breast cancer among younger and older women: An analysis using multiple measures of population health. Cancer Epidemiol 45:112–118
Glaser SL, Gulley ML, Clarke CA et al (2008) Racial/ethnic variation in EBV-positive classical Hodgkin lymphoma in California populations. Int J Cancer 123:1499–1507
Vo QN, Geradts J, Gulley ML, Boudreau DA, Bravo JC, Schneider BG (2002) Epstein–Barr virus in gastric adenocarcinomas: association with ethnicity and CDKN2A promoter methylation. J Clin Pathol 55:669–675
Ryan JL, Fan H, Glaser SL, Schichman SA, Raab-Traub N, Gulley ML (2004) Epstein–Barr virus quantitation by real-time PCR targeting multiple gene segments: a novel approach to screen for the virus in paraffin-embedded tissue and plasma. J Mol Diagn 6:378–385
Thorne LB, Ryan JL, Elmore SH, Glaser SL, Gulley ML (2005) Real-time PCR measures Epstein–Barr Virus DNA in archival breast adenocarcinomas. Diagn Mol Pathol 14:29–33
NAACCR Race and Ethnicity Work Group (2011) NAACCR Guideline for Enhancing Hispanic/Latino Identification: Revised NAACCR Hispanic/Latino Identification Algorithm [NHIA v2.2.1]. North American Association of Central Cancer Registries, Springfield, IL
Gomez SL, Glaser SL (2005) Quality of cancer registry birthplace data for Hispanics living in the United States. Cancer Causes Control 16:713–723
Keegan TH, John EM, Fish KM, Alfaro-Velcamp T, Clarke CA, Gomez SL (2010) Breast cancer incidence patterns among California Hispanic women: differences by nativity and residence in an enclave. Cancer Epidemiol Biomarkers Prev 19:1208–1218
Ryan J, Shen Y-J, Morgan D et al (2012) Epstein–Barr virus infection is common in inflamed gastrointestinal mucosa. Dig Dis Sci 57:1887–1898
Tang W, Fan H, Schroeder J et al (2013) Atypical Epstein–Barr viral genomic structure in lymphoma tissue and lymphoid cell lines. Diagn Mol Pathol 22:91–101
Gulley ML, Tang W (2008) Laboratory assays for Epstein–Barr virus-related disease. J Mol Diagn 10:279–292
Mazouni C, Fina F, Romain S, Ouafik LH, Bonnier P, Martin P-M (2015) Outcome of Epstein–Barr virus-associated primary breast cancer. Mol Clin Oncol 3:295–298
Hachana M, Amara K, Ziadi S, Romdhane E, Gacem RB, Trimeche M. (2011) Investigation of Epstein–Barr virus in breast carcinomas in Tunisia. Pathol Res Pract 207:695–700.
Fawzy S, Sallam M, Mohammad Awad N (2008) Detection of Epstein–Barr virus in breast carcinoma in Egyptian women. Clin Biochem 41:486–492
Mohammadizadeh F, Zarean M, Abbasi M (2014) Association of Epstein–Barr virus with invasive breast carcinoma and its impact on well-known clinicopathologic parameters in Iranian women. Advanced. Biomed Res 3:141
Ryan JL, Morgan DR, Dominguez RL et al (2009) High levels of Epstein–Barr virus DNA in latently infected gastric adenocarcinoma. Lab Invest J Tech Methods Pathol 89:80–90
Khan G, Philip PS, Al Ashari M, Houcinat Y, Daoud S (2011) Localization of Epstein–Barr virus to infiltrating lymphocytes in breast carcinomas and not malignant cells. Exp Mol Pathol 91:466–470
Khabaz MN (2013) Association of Epstein–Barr virus infection and breast carcinoma. Arch Med Sci 9:745–751
Hu H, Luo M-L, Desmedt C et al (2016) Epstein–Barr virus infection of mammary epithelial cells promotes malignant transformation. EBioMedicine 9:148–160
U.S. Department of Commerce Economics and Statistics Administration (2001) The Hispanic Population: Census 2000 Brief. U.S. Census Bureau, Washington, DC
Morales-Sánchez A, Molina-Muñoz T, Martínez-López JLE, et al. (2013) No association between Epstein–Barr virus and mouse mammary tumor virus with breast cancer in Mexican women. Sci Reports 3:2970
Hjalgrim H, Askling J, Rostgaard K et al (2003) Characteristics of Hodgkin’s lymphoma after infectious mononucleosis. N Engl J Med 349:1324–1332
Staras SAS, Dollard SC, Radford KW, Flanders WD, Pass RF, Cannon MJ (2006) Seroprevalence of cytomegalovirus infection in the United States, 1988–1994. Clin Infect Dis 43:1143–1151
Dowd JB, Palermo T, Brite J, McDade TW, Aiello A (2013) Seroprevalence of Epstein–Barr virus infection in U.S. children ages 6–19, 2003–2010. PLoS One 8:e64921
Dowd JB, Zajacova A, Aiello A (2009) Early origins of health disparities: Burden of infection, health, and socioeconomic status in U.S. children. Soc Sci Med 68:699–707
Hsu JL, Glaser SL (2000) Epstein–Barr virus-associated malignancies: epidemiologic patterns and etiologic implications. Crit Rev. Hematol Oncol 34:27–53
Glaser SL, Clarke CA, Chang ET, Yang J, Gomez SL, Keegan TH (2014) Hodgkin lymphoma incidence in California Hispanics: influence of nativity and tumor Epstein–Barr virus. Cancer Causes Control 25:709–725
Roychoudhuri R, Putcha V, Moller H (2006) Cancer and laterality: a study of the five major paired organs (UK). Cancer Causes Control 17:655–662
Sughrue T, Brody JP (2014) Breast tumor laterality in the United States depends upon the country of birth, but not race. PLoS One 9:e103313
Dane S, Erdem T, Gümüştekin K (2001) Cell-mediated immune hypersensitivity is stronger in the left side of the body than the right in healthy young subjects. Percept Mot Skills 93:329–332
Dane Ş (2009) Peripheral asymmetry of cell-mediated immunity. Int J Neurosci 119:611–615
Rickinson AB, Long HM, Palendira U, Münz C, Hislop AD (2014) Cellular immune controls over Epstein–Barr virus infection: new lessons from the clinic and the laboratory. Trends Immunol 35:159–169
Glenn WK, Heng B, Delprado W, Iacopetta B, Whitaker NJ, Lawson JS (2012) Epstein–Barr virus, human papillomavirus and mouse mammary tumour virus as multiple viruses in breast cancer. PLoS One 7:e48788
Aguayo F, Khan N, Koriyama C et al (2011) Human papillomavirus and Epstein–Barr virus infections in breast cancer from Chile. Infectious Agents Cancer 6:7-
Lorenzetti MA, De Matteo E, Gass H et al (2010) Characterization of Epstein Barr virus latency pattern in Argentine breast carcinoma. PLoS One 5:e13603
Mohammed ZMA, Going JJ, Edwards J, Elsberger B, McMillan DC (2013) The relationship between lymphocyte subsets and clinico-pathological determinants of survival in patients with primary operable invasive ductal breast cancer. Br J Cancer 109:1676–1684
Acknowledgments
The authors acknowledge contributions to this study by the late Sarah Shema, Sandra Elmore, Patricia Weeks, Rita Leung, David O. Nelson, and Meg McKinley. The collection of cancer incidence data used in this study was supported by the California Department of Health Services as part of the state-wide cancer-reporting program mandated by California Health and Safety Code, Section 103885; by the National Cancer Institute’s Surveillance, Epidemiology, and End Results Program under contracts N01-PC-35136 awarded to the Cancer Prevention Institute of California, N02-PC-15105 awarded to the Public Health Institute, HHSN261201000140C awarded to the Cancer Prevention Institute of California, HHSN261201000035C awarded to the University of Southern California, and HHSN261201000034C awarded to the Public Health Institute; and the Centers for Disease Control and Prevention’s National Program of Cancer Registries, under agreements U55/CCR921930-02 awarded to the Public Health Institute and U58DP003862-01 awarded to the California Department of Public Health. The ideas and opinions expressed herein are those of the authors, and endorsement by the State of California Department of Public Health, the National Cancer Institute, and the Centers for Disease Control and Prevention or their contractors and subcontractors is not intended nor should be inferred.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was supported in part by the California Breast Cancer Research Program (9WB-0005) (Dr. Glaser), the National Cancer Institute (R03 CA101500) (Dr. Gulley), and the Safeway Foundation (Dr. Glaser).
Conflict of interest
Dr. Clarke has received institutional support for breast cancer research from Genentech and Grail Bio. The other authors declare that they have no conflict of interest.
Research involving human participants and/or animals
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
This article did not involve human participants and informed consent was not required by the Institutional Review Boards reviewing the study.
Rights and permissions
About this article
Cite this article
Glaser, S.L., Canchola, A.J., Keegan, T.H.M. et al. Variation in risk and outcomes of Epstein–Barr virus-associated breast cancer by epidemiologic characteristics and virus detection strategies: an exploratory study. Cancer Causes Control 28, 273–287 (2017). https://doi.org/10.1007/s10552-017-0865-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-017-0865-3