Abstract
Background
Survival outcomes in metastatic breast cancer (MBC) have improved due to novel agents such as CDK4/6 inhibitors (CDK4/6i). Nevertheless, Black patients and patients with lower socioeconomic status (SES) continue to bear a disproportionate mortality burden.
Methods
We conducted a retrospective analysis of EHR-derived data from the Flatiron Health Database (FHD). A dataset was constructed to include Black/African-American (Black/AA) and White patients with hormone receptor (HR)-positive, HER2-negative MBC. Outcomes included CDK4/6i use (overall and first-line), and rates of leukopenia, dose reduction, and time on treatment for first-line CDK4/6i. Multivariable logistic regression was used to evaluate factors associated with use and outcomes.
Results
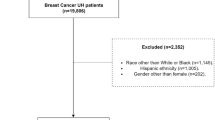
A total of 6802 patients with MBC were included, of which 5187 (76.3%) received CDK4/6i. Of those, 3186 (61.4%) received CDK4/6i first-line. Overall, 86.7% of patients were categorized as White and 13.3% as Black/AA; 22.4% were > 75 years old; 12.6% were treated at an academic site; 3.3% had Medicaid insurance. In addition to advanced age and poorer performance status, lower use of CDK4/6i was associated with Black/AA vs White race (72.9% vs 76.8%; OR 0.83, 95% CI 0.70–0.99, p = 0.04) and Medicaid vs commercial insurance (69.6% vs 77.4%; OR: 0.68, 95% CI 0.49–0.95, p = 0.02). Odds of CDK4/6i use were twofold higher for patients treated at an academic center (p < 0.001). Rates of CDK4/6i-induced leukopenia and dose reductions did not differ significantly by race, insurance type, or treatment site. Time on CDK4/6i was significantly lower among Medicaid patients (395 days) than patients with commercial insurance (558 days) or Medicare (643 days) (p = 0.03).
Conclusion
This analysis of real-world data suggests that Black race and lower SES are associated with decreased CDK4/6i use. However, among patients treated with CDK4/6i, subsequent toxicity outcomes are similar. Efforts to ensure access to these life-prolonging medications are warranted.

Similar content being viewed by others
Data availability
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Giaquinto AN, Sung H, Miller KD et al (2022) Breast cancer statistics, 2022. CA Cancer J Clin 72(6):524–541. https://doi.org/10.3322/caac.21754
Singh GK, Williams SD, Siahpush M, Mulhollen A (2011) Socioeconomic, rural-urban, and racial inequalities in US cancer mortality: part I-all cancers and lung cancer and part II-colorectal, prostate, breast, and cervical cancers. J Cancer Epidemiol 2011:107497. https://doi.org/10.1155/2011/107497
Ren JX, Gong Y, Ling H, Hu X, Shao ZM (2019) Racial/ethnic differences in the outcomes of patients with metastatic breast cancer: contributions of demographic, socioeconomic, tumor and metastatic characteristics. Breast Cancer Res Treat 173(1):225–237. https://doi.org/10.1007/s10549-018-4956-y
Leopold C, Wagner AK, Zhang F et al (2016) Racial disparities in all-cause mortality among younger commercially insured women with incident metastatic breast cancer. Breast Cancer Res Treat 158(2):333–340. https://doi.org/10.1007/s10549-016-3875-z
Finn RS, Martin M, Rugo HS et al (2016) Palbociclib and letrozole in advanced breast cancer. N Engl J Med 375(20):1925–1936. https://doi.org/10.1056/NEJMoa1607303
Hortobagyi GN, Stemmer SM, Burris HA et al (2022) Overall survival with ribociclib plus letrozole in advanced breast cancer. N Engl J Med 386(10):942–950. https://doi.org/10.1056/NEJMoa2114663
Goetz MP, Toi M, Campone M et al (2017) MONARCH 3: abemaciclib as initial therapy for advanced breast cancer. J Clin Oncol 35(32):3638–3646. https://doi.org/10.1200/JCO.2017.75.6155
National Comprehensive Cancer Network (2022) NCCN Guidelines. Breast cancer (version 4)
Reeder-Hayes K, Peacock Hinton S, Meng K, Carey LA, Dusetzina SB (2016) Disparities in use of human epidermal growth hormone receptor 2-targeted therapy for early-stage breast cancer. J Clin Oncol 34(17):2003–2009. https://doi.org/10.1200/JCO.2015.65.8716
Dreyer MS, Nattinger AB, McGinley EL, Pezzin LE (2018) Socioeconomic status and breast cancer treatment. Breast Cancer Res Treat 167(1):1–8. https://doi.org/10.1007/s10549-017-4490-3
Wu XC, Lund MJ, Kimmick GG et al (2012) Influence of race, insurance, socioeconomic status, and hospital type on receipt of guideline-concordant adjuvant systemic therapy for locoregional breast cancers. J Clin Oncol 30(2):142–150. https://doi.org/10.1200/JCO.2011.36.8399
Norris RP, Dew R, Sharp L et al (2020) Are there socio-economic inequalities in utilization of predictive biomarker tests and biological and precision therapies for cancer? A systematic review and meta-analysis. BMC Med 18(1):282. https://doi.org/10.1186/s12916-020-01753-0
Hortobagyi GN, Stemmer SM, Burris HA et al (2016) Ribociclib as first-line therapy for HR-positive, advanced breast cancer. N Engl J Med 375(18):1738–1748. https://doi.org/10.1056/NEJMoa1609709
Whitaker KD, Wang X, Ascha M et al (2022) Racial inequities in second-line treatment and overall survival among patients with metastatic breast cancer. Breast Cancer Res Treat 196(1):163–173. https://doi.org/10.1007/s10549-022-06701-5
Sachs RE, Gavulic KA, Donohue JM, Dusetzina SB (2021) Recent trends in medicaid spending and use of drugs with US Food and Drug Administration accelerated approval. JAMA Health Forum 2(10):e213177. https://doi.org/10.1001/jamahealthforum.2021.3177
Kullgren JT, McLaughlin CG, Mitra N, Armstrong K (2012) Nonfinancial barriers and access to care for US adults. Health Serv Res 47(1 Pt 2):462–485. https://doi.org/10.1111/j.1475-6773.2011.01308.x
Nardi EA, Wolfson JA, Rosen ST et al (2016) Value, access, and cost of cancer care delivery at academic cancer centers. J Natl Compr Canc Netw 14(7):837–847. https://doi.org/10.6004/jnccn.2016.0088
Moyers JT, Patel A, Shih W, Nagaraj G (2020) Association of sociodemographic factors with immunotherapy receipt for metastatic melanoma in the US. JAMA Netw Open 3(9):e2015656. https://doi.org/10.1001/jamanetworkopen.2020.15656
Lou Y, Dholaria B, Soyano A et al (2018) Survival trends among non-small-cell lung cancer patients over a decade: impact of initial therapy at academic centers. Cancer Med 7(10):4932–4942. https://doi.org/10.1002/cam4.1749
Reich D, Nalls MA, Kao WH et al (2009) Reduced neutrophil count in people of African descent is due to a regulatory variant in the duffy antigen receptor for chemokines gene. PLoS Genet 5(1):e1000360. https://doi.org/10.1371/journal.pgen.1000360
Atallah-Yunes SA, Ready A, Newburger PE (2019) Benign ethnic neutropenia. Blood Rev 37:100586. https://doi.org/10.1016/j.blre.2019.06.003
Schreier A, Munoz-Arcos L, Alvarez A, Sparano JA, Anampa JD (2022) Racial disparities in neutrophil counts among patients with metastatic breast cancer during treatment with CDK4/6 inhibitors. Breast Cancer Res Treat 194(2):337–351. https://doi.org/10.1007/s10549-022-06574-8
Liu M, Qi Y, Wang W, Sun X (2022) Toward a better understanding about real-world evidence. Eur J Hosp Pharm 29(1):8–11. https://doi.org/10.1136/ejhpharm-2021-003081
Arondekar B, Duh MS, Bhak RH et al (2022) Real-world evidence in support of oncology product registration: a systematic review of new drug application and biologics license application approvals from 2015–2020. Clin Cancer Res 28(1):27–35. https://doi.org/10.1158/1078-0432.CCR-21-2639
Funding
This research was partially funded by the American Cancer Society (DLH) and the Breast Cancer Research Foundation (DLH).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sathe, C., Accordino, M.K., DeStephano, D. et al. Social determinants of health and CDK4/6 inhibitor use and outcomes among patients with metastatic breast cancer. Breast Cancer Res Treat 200, 85–92 (2023). https://doi.org/10.1007/s10549-023-06957-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-023-06957-5