Abstract
Purpose
The extent to which evidence-based treatments are applied to populations not well represented in early stage breast cancer (EBC) trials remains unknown. This study evaluated treatment intensity for patients traditionally well represented, underrepresented, and unrepresented in clinical trials.
Methods
This retrospective cohort study used real-world data to evaluate the intensity (high or low) of EBC chemotherapy by patient characteristics (age, race and ethnicity, presence of comorbidity) denoting clinical trial representation status (well represented, underrepresented, unrepresented) for patients diagnosed from 2011 to 2020. Odds ratios (OR) from a logistic regression model was used to evaluate the association between receipt of high-intensity chemotherapy and clinical trial representation status characteristics adjusting for cancer stage and subtype.
Results
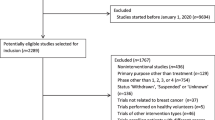
Of 970 patients with EBC, 41% were characterized as well represented, 45% as underrepresented, and 13% as unrepresented in clinical trials. In adjusted models, patients aged ≥ 70 versus 45–69 had lower odds of receiving a high-intensity treatment (OR 0.40, 95% CI 0.26–0.60), while those aged < 45 versus 45–69 had higher odds of receiving high-intensity treatment (OR 1.82, 95% CI 1.10–3.01). In predicted estimates, the proportion of patients receiving a high-intensity treatment was 87% for patients aged < 45, 79% for patients aged 45–69, and 60% for patients aged ≥ 70.
Conclusion
59% of the EBC population is not well represented in clinical trials. Age was associated with differential treatment intensity. Widening clinical trial eligibility criteria should be considered to better understand survival outcomes, toxicity effects, and ultimately make evidence-based treatment decisions using a more diverse sample.


Similar content being viewed by others
Availability of data, material, and code
The data that support the findings of this study are available from Flatiron Health. Restrictions apply to the availability of these data, which were used under license for this study. Data and code are available from the authors with the permission of Flatiron Health.
References
Center for Disease Control and Prevention (2015) United States Cancer Statistics: Data Visualizations (Female Breast). https://gis.cdc.gov/Cancer/USCS/DataViz.html
NIH, National Cancer Institute, Surveillance, Epidemiology, and End Results Program. Cancer Stat Facts: Female Breast Cancer. https://seer.cancer.gov/statfacts/html/breast.html. Accessed 18 Sept 2020
Murthy VH, Krumholz HM, Gross CP (2004) Participation in cancer clinical trials: race-, sex-, and age-based disparities. JAMA 291(22):2720–2726. https://doi.org/10.1001/jama.291.22.2720
Division of Cancer Prevention and Control (2019) Breast cancer in young women. https://www.cdc.gov/cancer/breast/young_women/index.htm. Accessed 18 Sept 2020
Ludmir EB, Mainwaring W, Lin TA et al (2019) Factors associated with age disparities among cancer clinical trial participants. JAMA Oncol. https://doi.org/10.1001/jamaoncol.2019.2055
Martin M, Pienkowski T, Mackey J et al (2005) Adjuvant docetaxel for node-positive breast cancer. N Engl J Med 352(22):2302–2313. https://doi.org/10.1056/NEJMoa043681
Sparano JA, Wang M, Martino S et al (2008) Weekly paclitaxel in the adjuvant treatment of breast cancer. N Engl J Med 358(16):1663–1671. https://doi.org/10.1056/NEJMoa0707056
Jones S, Holmes FA, O’Shaughnessy J et al (2009) Docetaxel with cyclophosphamide is associated with an overall survival benefit compared with doxorubicin and cyclophosphamide: 7-year follow-up of US Oncology Research Trial 9735. J Clin Oncol 27(8):1177–1183. https://doi.org/10.1200/JCO.2008.18.4028
Slamon D, Eiermann W, Robert N et al (2011) Adjuvant trastuzumab in HER2-positive breast cancer. N Engl J Med 365(14):1273–1283. https://doi.org/10.1056/NEJMoa0910383
National Comprehensive Cancer Network (2017) NCCN History. National Comprehensive Cancer Network. https://www.nccn.org/about/history.aspx. Accessed 16 July 2018
Gradishar WJ, Anderson BO, Balassanian R et al (2015) Breast cancer version 2.2015. J Natl Compr Canc Netw 13(4):448–475
DeSantis CE, Ma J, Gaudet MM et al (2019) Breast cancer statistics, 2019. CA Cancer J Clin 69(6):438–451. https://doi.org/10.3322/caac.21583
Reeder-Hayes KE, Wheeler SB, Mayer DK (2015) Health disparities across the breast cancer continuum. Semin Oncol Nurs 31(2):170–177. https://doi.org/10.1016/j.soncn.2015.02.005
Wallwiener CW, Hartkopf AD, Grabe E et al (2016) Adjuvant chemotherapy in elderly patients with primary breast cancer: are women >/=65 undertreated? J Cancer Res Clin Oncol 142(8):1847–1853. https://doi.org/10.1007/s00432-016-2194-4
Ewertz M, Land LH, Dalton SO et al (2018) Influence of specific comorbidities on survival after early-stage breast cancer. Acta Oncol 57(1):129–134. https://doi.org/10.1080/0284186X.2017.1407496
Birnbaum B, Nussbaum N, Seidl-Rathkopf K et al (2020) Model-assisted cohort selection with bias analysis for generating large-scale cohorts from the EHR for oncology research. arXiv
Ma X, Long L, Moon S et al (2020) Comparison of Population Characteristics in Real-World Clinical Oncology Databases in the US: Flatiron Health, SEER, and NPCR medRxiv, Preprint
Cohen J (1992) A power primer. Psychol Bull 112(1):155–159. https://doi.org/10.1037//0033-2909.112.1.155
Kim ES, Bruinooge SS, Roberts S et al (2017) Broadening eligibility criteria to make clinical trials more representative: American Society of Clinical Oncology and Friends of Cancer Research Joint Research Statement. J Clin Oncol 35(33):3737–3744. https://doi.org/10.1200/JCO.2017.73.7916
Muss HB, Polley MC, Berry DA et al (2019) Randomized trial of standard adjuvant chemotherapy regimens versus capecitabine in older women with early breast cancer: 10-year update of the CALGB 49907 trial. J Clin Oncol 37(26):2338–2348. https://doi.org/10.1200/JCO.19.00647
Leinert E, Singer S, Janni W et al (2017) The impact of age on quality of life in breast cancer patients receiving adjuvant chemotherapy: a comparative analysis from the prospective multicenter randomized ADEBAR trial. Clin Breast Cancer 17(2):100–106. https://doi.org/10.1016/j.clbc.2016.10.008
Mohile SG, Dale W, Somerfield MR et al (2018) Practical assessment and management of vulnerabilities in older patients receiving chemotherapy: ASCO guideline for geriatric oncology summary. J Oncol Pract 14(7):442–446. https://doi.org/10.1200/JOP.18.00180
Citron ML, Berry DA, Cirrincione C et al (2003) Randomized trial of dose-dense versus conventionally scheduled and sequential versus concurrent combination chemotherapy as postoperative adjuvant treatment of node-positive primary breast cancer: first report of Intergroup Trial C9741/Cancer and Leukemia Group B Trial 9741. J Clin Oncol 21(8):1431–1439. https://doi.org/10.1200/JCO.2003.09.081
Howard-Anderson J, Ganz PA, Bower JE et al (2012) Quality of life, fertility concerns, and behavioral health outcomes in younger breast cancer survivors: a systematic review. J Natl Cancer Inst 104(5):386–405. https://doi.org/10.1093/jnci/djr541
Wolff AC, Tung NM, Carey LA (2019) Implications of neoadjuvant therapy in human epidermal growth factor receptor 2-positive breast cancer. J Clin Oncol 37(25):2189–2192. https://doi.org/10.1200/JCO.19.01159
CompassHER2-pCR: Decreasing Chemotherapy for Breast Cancer Patients After Pre-surgery Chemo and Targeted Therapy. (2020). https://clinicaltrials.gov/ct2/show/NCT04266249. Accessed 18 Sept 2020
Treweek S, Dryden R, McCowan C et al (2015) Do participants in adjuvant breast cancer trials reflect the breast cancer patient population? Eur J Cancer 51(8):907–914. https://doi.org/10.1016/j.ejca.2015.01.064
Giordano SH, Duan Z, Kuo YF et al (2006) Use and outcomes of adjuvant chemotherapy in older women with breast cancer. J Clin Oncol 24(18):2750–2756. https://doi.org/10.1200/JCO.2005.02.3028
Fu MR, Axelrod D, Guth AA et al (2015) Comorbidities and quality of life among breast cancer survivors: a prospective study. J Pers Med 5(3):229–242. https://doi.org/10.3390/jpm5030229
Braithwaite D, Moore DH, Satariano WA et al (2012) Prognostic impact of comorbidity among long-term breast cancer survivors: results from the LACE study. Cancer Epidemiol Biomarkers Prev 21(7):1115–1125. https://doi.org/10.1158/1055-9965.EPI-11-1228
Patnaik JL, Byers T, Diguiseppi C et al (2011) The influence of comorbidities on overall survival among older women diagnosed with breast cancer. J Natl Cancer Inst 103(14):1101–1111. https://doi.org/10.1093/jnci/djr188
Parrinello CM, Seidl-Rathkopf KN, Bourla AB, Nussbaum NC, Carson KR, Abernethy AP (2018) Comparison of Structured Versus Abstracted Comorbidities Using Oncology EHR Data from Cancer Patients in the Flatiron Health Network. Value Health 21:S14
Community Oncology Alliance. FACT Sheet: What is Community Oncology (2017). https://communityoncology.org/wp-content/uploads/2017/08/What-is-Comm-Onc.pdf. Accessed 25 Aug 2020
Funding
The Robert Wood Johnson Foundation (#76306) provided funding for this study. Dr. Rocque is supported by an American Cancer Society Mentored Research Scholar Grants (MRSG- 17–051-01 -PCSM).
Author information
Authors and Affiliations
Contributions
Study concept/design: GR, CW, AA, RG Provision of study material or patients: GR. Data collection/assembly: NC, JF, CW, MA, AA. Data analysis and interpretation: all authors. Manuscript writing: all authors. Final approval of manuscript: all authors.
Corresponding author
Ethics declarations
Conflict of interest
Dr. Rocque received research funding from Genentech, Pfizer, and Carevive and consulting fees for Genentech and Pfizer.
Ethical approval
This study was approved by the University of Alabama at Birmingham Institutional Review Board (IRB) and the WCG central IRB with waiver of informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Rocque, G.B., Caston, N.E., Franks, J.A. et al. Clinical trial representativeness and treatment intensity in a real-world sample of women with early stage breast cancer. Breast Cancer Res Treat 190, 531–540 (2021). https://doi.org/10.1007/s10549-021-06381-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-021-06381-7