Abstract
Purpose
Immunogenomics and earlier, pioneering studies, particularly by Whiteside and colleagues, have indicated a positive role for B-cells in breast cancer, as well as a positive role for gamma-delta T-cells. However, these studies have been completely limited to assessing breast cancer tumor tissue.
Methods and Results
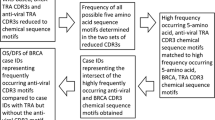
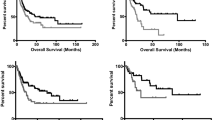
Our analyses here has shown that blood-borne T-cell receptor gamma (TRG) chain sequences were associated with greater overall survival, of particular note due to the comparative longevity of primary breast cancer patients, whereby assessments of disease-free, but rarely overall survival parameters are possible. Additional immunogenomics approaches narrowed the overall survival correlations to specific, TRG complementarity determining region-3, amino acid (AA) sequence chemical features, independently of many common, confounding variables in the breast cancer setting, such as estrogen or progesterone receptor status.
Conclusions
These results are discussed in the context of patient age and with regard to potential antigenic targets, based on the chemistry of the TRG CDR3 AA sequences associated with the higher survival rates.



Similar content being viewed by others
Abbreviations
- AA:
-
Amino acid
- AJCC:
-
American Joint Committee on Cancer
- BRCA:
-
Breast cancer
- CDR3:
-
Complementarity determining region-3
- KM:
-
Kaplan–Meier
- OS:
-
Overall survival
- DFS:
-
Disease-free survival
- RSSA:
-
Randomized subset survival assessment
- SPSS:
-
Statistical Package for the Social Sciences
- TCGA:
-
The Cancer Genome Atlas
- TIL:
-
Tumor-infiltrating lymphocyte
- TRG:
-
T-cell receptor gamma
- UCEC:
-
Uterine cancer
- WXS:
-
Whole-exome sequence
References
Errico A (2015) Breast cancer: tamoxifen—offering a long-term prevention option. Nat Rev ClinOncol 12(2):66. https://doi.org/10.1038/nrclinonc.2014.236 (PubMed PMID: 25583681)
Hamadeh IS, Patel JN, Rusin S, Tan AR (2018) Personalizing aromatase inhibitor therapy in patients with breast cancer. Cancer Treat Rev 70:47–55. https://doi.org/10.1016/j.ctrv.2018.07.014 (PubMed PMID: 30086432)
Sarosiek T, Morawski P (2018) Trastuzumab and its biosimilars. Pol MerkurLekarski 44(263):253–257 (PubMed PMID: 29813044)
Tong WL, Callahan BM, Tu YN, Zaman S, Chobrutskiy BI, Blanck G (2019) Immune receptor recombinations from breast cancer exome files, independently and in combination with specific HLA alleles, correlate with better survival rates. Breast Cancer Res Treat 173(1):167–177. https://doi.org/10.1007/s10549-018-4961-1 (PubMed PMID: 30229447)
Tong WL, Tu YN, Samy MD, Sexton WJ, Blanck G (2017) Identification of immunoglobulin V(D)J recombinations in solid tumor specimen exome files: evidence for high level B-cell infiltrates in breast cancer. Human VaccImmunother 13(3):501–506. https://doi.org/10.1080/21645515.2016.1246095 (PubMed PMID: 28085544; PubMed Central PMCID: PMCPMC5360147)
Disis ML, Stanton SE (2018) Immunotherapy in breast cancer: an introduction. Breast 37:196–199. https://doi.org/10.1016/j.breast.2017.01.013 (PubMed PMID: 28162837)
Denkert C, Loibl S, Noske A, Roller M, Muller BM, Komor M, Budczies J, Darb-Esfahani S, Kronenwett R, Hanusch C, von Torne C, Weichert W, Engels K, Solbach C, Schrader I, Dietel M, von Minckwitz G (2010) Tumor-associated lymphocytes as an independent predictor of response to neoadjuvant chemotherapy in breast cancer. J ClinOncol Off J Am SocClinOncol 28(1):105–113. https://doi.org/10.1200/JCO.2009.23.7370 (PubMed PMID: 19917869)
Sugie T (2018) Immunotherapy for metastatic breast cancer. Chin ClinOncol 7(3):28. https://doi.org/10.21037/cco.2018.05.05 (PubMed PMID: 30056730)
Arturo JF, Chobrutskiy BI, Yeagley M, Patel DN, Falasiri S, Patel JS, Blanck G (2020) Electrostatic complementarity of B-cell receptor CDR3s and TP53-mutant amino acids in breast cancer is associated with increased disease-free survival rates. Cell MolImmunol 17(7):776–778. https://doi.org/10.1038/s41423-019-0328-8 (PubMed PMID: 31729463; PubMed Central PMCID: PMCPMC7331692)
Chobrutskiy BI, Zaman S, Tong WL, Diviney A, Blanck G (2018) Recovery of T-cell receptor V(D)J recombination reads from lower grade gliomaexome files correlates with reduced survival and advanced cancer grade. J Neurooncol 140(3):697–704. https://doi.org/10.1007/s11060-018-03001-1 (PubMed PMID: 30382482)
Salam N, Rane S, Das R, Faulkner M, Gund R, Kandpal U, Lewis V, Mattoo H, Prabhu S, Ranganathan V, Durdik J, George A, Rath S, Bal V (2013) T cell ageing: effects of age on development, survival & function. Indian J Med Res. 138(5):595–608 (PubMed PMID: 24434315; PubMed Central PMCID: PMCPMC3928693)
Britanova OV, Putintseva EV, Shugay M, Merzlyak EM, Turchaninova MA, Staroverov DB, Bolotin DA, Lukyanov S, Bogdanova EA, Mamedov IZ, Lebedev YB, Chudakov DM (2014) Age-related decrease in TCR repertoire diversity measured with deep and normalized sequence profiling. J Immunol 192(6):2689–2698. https://doi.org/10.4049/jimmunol.1302064 (PubMed PMID: 24510963)
Fonseca S, Pereira V, Lau C, Teixeira MDA, Bini-Antunes M, Lima M (2020) Human peripheral blood gamma delta T Cells: report on a series of healthy Caucasian Portuguese adults and comprehensive review of the literature. Cells. https://doi.org/10.3390/cells9030729 (PubMed PMID: 32188103; PubMed Central PMCID: PMCPMC7140678)
Parker CM, Groh V, Band H, Porcelli SA, Morita C, Fabbi M, Glass D, Strominger JL, Brenner MB (1990) Evidence for extrathymic changes in the T cell receptor gamma/delta repertoire. J Exp Med 171(5):1597–1612. https://doi.org/10.1084/jem.171.5.1597 (PubMed PMID: 2185330; PubMed Central PMCID: PMCPMC2187908)
Sandberg Y, Almeida J, Gonzalez M, Lima M, Barcena P, Szczepanski T, van Gastel-Mol EJ, Wind H, Balanzategui A, van Dongen JJ, Miguel JF, Orfao A, Langerak AW (2006) TCRgammadelta+ large granular lymphocyte leukemias reflect the spectrum of normal antigen-selected TCRgammadelta+ T-cells. Leukemia 20(3):505–513. https://doi.org/10.1038/sj.leu.2404112 (PubMed PMID: 16437145)
Chen IH, Xue L, Hsu CC, Paez JS, Pan L, Andaluz H, Wendt MK, Iliuk AB, Zhu JK, Tao WA (2017) Phosphoproteins in extracellular vesicles as candidate markers for breast cancer. ProcNatlAcadSci USA 114(12):3175–3180. https://doi.org/10.1073/pnas.1618088114 (PubMed PMID: 28270605; PubMed Central PMCID: PMCPMC5373352)
Wu R, Liu F, Peng P, Qiu H, Xiong H, Yu S, Huang X, Zhang H, Zhuang L (2018) Tumor stress-induced phosphoprotein 1 as a prognostic biomarker for breast cancer. Ann Translat Med 6(15):302. https://doi.org/10.21037/atm.2018.06.46 (PubMed PMID: 30211190; PubMed Central PMCID: PMCPMC6123203)
Chen PM, Chu PY, Tung SL, Liu CY, Tsai YF, Lin YS, Wang WL, Wang YL, Lien PJ, Chao TC, Tseng LM (2017) Overexpression of phosphoprotein phosphatase 2A predicts worse prognosis in patients with breast cancer: a 15-year follow-up. Hum Pathol 66:93–100. https://doi.org/10.1016/j.humpath.2017.06.001 (PubMed PMID: 28603063)
Olayioye MA, Hoffmann P, Pomorski T, Armes J, Simpson RJ, Kemp BE, Lindeman GJ, Visvader JE (2004) The phosphoprotein StarD10 is overexpressed in breast cancer and cooperates with ErbB receptors in cellular transformation. Can Res 64(10):3538–3544. https://doi.org/10.1158/0008-5472.CAN-03-3731 (PubMed PMID: 15150109)
Valdes-Rives SA, Gonzalez-Arenas A (2017) Autotaxin-Lysophosphatidic acid: from inflammation to cancer development. Mediators Inflamm 2017:9173090. https://doi.org/10.1155/2017/9173090 (PubMed PMID: 29430083; PubMed Central PMCID: PMCPMC5753009)
Leblanc R, Houssin A, Peyruchaud O (2018) Platelets, autotaxin and lysophosphatidic acid signalling: win–win factors for cancer metastasis. Br J Pharmacol 175(15):3100–3110. https://doi.org/10.1111/bph.14362 (PubMed PMID: 29777586; PubMed Central PMCID: PMCPMC6031885)
Nam JS, Sharma AR, Nguyen LT, Jagga S, Lee YH, Sharma G, Lee SS (2018) Lysophosphatidic acid enhances breast cancer cells-mediated osteoclastogenesis. Korean J PhysiolPharmacol 22(5):503–511. https://doi.org/10.4196/kjpp.2018.22.5.503 (PubMed PMID: 30181697; PubMed Central PMCID: PMCPMC6115344)
Arkko S, Zlatev HP, Monkkonen H, Raikkonen J, Benzaid I, Clezardin P, Monkkonen J, Maatta JA (2015) Upregulation of the mevalonate pathway by cholesterol depletion abolishes tolerance to N-bisphosphonate induced Vgamma9Vdelta2 T cell cytotoxicity in PC-3 prostate cancer cells. Cancer Lett 357(1):279–285. https://doi.org/10.1016/j.canlet.2014.11.030 (PubMed PMID: 25444923)
Benzaid I, Monkkonen H, Bonnelye E, Monkkonen J, Clezardin P (2012) In vivo phosphoantigen levels in bisphosphonate-treated human breast tumors trigger Vgamma9Vdelta2 T-cell antitumor cytotoxicity through ICAM-1 engagement. Clin Cancer Res Offl J Am Assoc Cancer Res 18(22):6249–6259. https://doi.org/10.1158/1078-0432.CCR-12-0918 (PubMed PMID: 23032740)
Benzaid I, Monkkonen H, Stresing V, Bonnelye E, Green J, Monkkonen J, Touraine JL, Clezardin P (2011) High phosphoantigen levels in bisphosphonate-treated human breast tumors promote Vgamma9Vdelta2 T-cell chemotaxis and cytotoxicity in vivo. Can Res 71(13):4562–4572. https://doi.org/10.1158/0008-5472.CAN-10-3862 (PubMed PMID: 21646473)
Meraviglia S, Eberl M, Vermijlen D, Todaro M, Buccheri S, Cicero G, La Mendola C, Guggino G, D’Asaro M, Orlando V, Scarpa F, Roberts A, Caccamo N, Stassi G, Dieli F, Hayday AC (2010) In vivo manipulation of Vgamma9Vdelta2 T cells with zoledronate and low-dose interleukin-2 for immunotherapy of advanced breast cancer patients. ClinExpImmunol 161(2):290–297. https://doi.org/10.1111/j.1365-2249.2010.04167.x (PubMed PMID: 20491785; PubMed Central PMCID: PMCPMC2909411)
Caccamo N, Meraviglia S, Scarpa F, La Mendola C, Santini D, Bonanno CT, Misiano G, Dieli F, Salerno A (2008) Aminobisphosphonate-activated gammadelta T cells in immunotherapy of cancer: doubts no more. Expert OpinBiolTher 8(7):875–883. https://doi.org/10.1517/14712598.8.7.875 (PubMed PMID: 18549319)
Chabab G, Barjon C, Abdellaoui N, Salvador-Prince L, Dejou C, Michaud HA, Boissiere-Michot F, Lopez-Crapez E, Jacot W, Pourquier D, Bonnefoy N, Lafont V (2020) Identification of a regulatory Vdelta1 gamma delta T cell subpopulation expressing CD73 in human breast cancer. J LeukocBiol 107(6):1057–1067. https://doi.org/10.1002/JLB.3MA0420-278RR (PubMed PMID: 32362028)
Wu Y, Kyle-Cezar F, Woolf RT, Naceur-Lombardelli C, Owen J, Biswas D, Lorenc A, Vantourout P, Gazinska P, Grigoriadis A, Tutt A, Hayday A (2019) An innate-like Vdelta1(+) gammadelta T cell compartment in the human breast is associated with remission in triple-negative breast cancer. SciTransl Med. https://doi.org/10.1126/scitranslmed.aax9364 (PubMed PMID: 31597756; PubMed Central PMCID: PMCPMC6877350)
Acknowledgements
Authors wish to acknowledge the support of USF research computing; and Corinne Walters, for administrative support related to NIH dataset access; and the taxpayers of the State of Florida. AC, BC, MH, and SZ were RISE fellowship recipients. SZ is a Susan Komen fellowship recipient.
Author information
Authors and Affiliations
Contributions
AC wrote the first several drafts of the manuscripts, edited all drafts, conducted CDR3 motif, overall survival, and RNAseq analyses; conducted replication analyses, conducted SPSS confounding variable analyses. BC conceived of the CDR3 AA motif, survival-related algorithm and scripted the algorithm. BC and SZ developed motif/encoding process. MH contributed to the UCEC analysis. GB, supervised project, participated in data validation steps, assisted in preparation of manuscript, and assumes all responsibility for final version of the manuscript and data analyses.
Corresponding author
Ethics declarations
Conflict of interest
The authors have nothing to declare.
Informed consent
Not applicable. See above.
Research involving human participants and/or animals
This report represents non-human subjects research, but the WXS files represented controlled access data. As such, these files were accessed under dbGaP approval number 6300. This article does not contain any studies with animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chobrutskiy, A., Chobrutskiy, B.I., Zaman, S. et al. Chemical features of blood-borne TRG CDR3s associated with an increased overall survival in breast cancer. Breast Cancer Res Treat 185, 591–600 (2021). https://doi.org/10.1007/s10549-020-05996-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-020-05996-6