Abstract
Background
The tumor immune microenvironment plays a critical role in the prognosis and outcome of breast cancers. This study examined the role of tumor-infiltrating lymphocytes (TILs), CD8+, FOXP3+ lymphocytes, PD-L1 expression, and other clinicopathological parameters in HER2+ breast cancer and correlate with tumor response to neoadjuvant therapy.
Methods
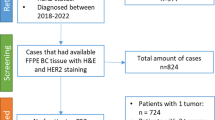
We included 173 HER2+ patients treated with neoadjuvant HER2-targeted chemotherapy regimens from 2010 to 2016. 67 cases had biopsy blocks to evaluate TIL, CD8, FOXP3, and PD-L1 immunohistochemistry staining. Tumors were classified as pCR vs non-pCR group. Clinicopathological parameters, TIL, CD8+ and FOXP3+ cell count, and PD-L1 expression were correlated with pCR rate.
Results
Univariate analyses showed that pCR rate was significantly correlated with low PR, low ER, high Ki-67, high FOXP3, HER2 IHC3+ , high HER2 ratio and copy number. By multivariate analysis, Ki-67 was the only variable significantly correlated with pCR. PD-L1 expression was detected in 9.2% cases. TIL hotspot has a non-significant correlation with pCR rate (p = 0.096).
Conclusions
High Ki-67 is a strong predictor for pCR in HER2+ breast cancer. TIL and FOXP3 T cells may play a role in tumor response in HER2+ cancer. PD-L1 is expressed in a subset of HER2+ breast cancer, supporting a role of immunotherapy in treating a subset of HER2+ breast cancers. The role of PD-L1, TIL, and other markers of immunogenicity as predictors of response to neoadjuvant chemotherapy in HER2+ breast cancer should be further evaluated.



Similar content being viewed by others
References
Cronin KA, Lake AJ, Scott S (2018) Annual Report to the Nation on the Status of Cancer, part I: National cancer statistics. Cancer 124:2785–2800
Arciero CA, Guo Y, Jiang R et al (2019) ER(+)/HER2(+) breast cancer has different metastatic patterns and better survival than ER(-)/HER2(+) breast cancer. Clin Breast Cancer 19:236–245
Li X, Wei B, Sonmez C et al (2017) High tumor budding count is associated with adverse clinicopathologic features and poor prognosis in breast carcinoma. Hum Pathol 66:222–229
Li X, Zhang Y, Meisel J et al (2018) Validation of the newly proposed American Joint Committee on Cancer (AJCC) breast cancer prognostic staging group and proposing a new staging system using the National Cancer Database. Breast Cancer Res Treat 171:303–313
Meisel J, Zhang C, Neely C et al (2018) Evaluation of prognosis in hormone receptor-positive/HER2-negative and lymph node-negative breast cancer with low oncotype DX recurrence score. Clin Breast Cancer 18:347–352
Li X, Oprea-Ilies GM, Krishnamurti U (2017) New developments in breast cancer and their impact on daily practice in pathology. Arch Pathol Lab Med 141:490–498
Li X, Yang J, Krishnamurti U et al (2017) Hormone receptor-positive breast cancer has a worse prognosis in male than in female patients. Clin Breast Cancer 17:356–366
Li X, Yang J, Peng L et al (2017) Triple-negative breast cancer has worse overall survival and cause-specific survival than non-triple-negative breast cancer. Breast Cancer Res Treat 161:279–287
Slamon D, Pegram M (2001) Rationale for trastuzumab (Herceptin) in adjuvant breast cancer trials. Semin Oncol 28:13–19
Schneeweiss A, Chia S, Hickish T et al (2013) Pertuzumab plus trastuzumab in combination with standard neoadjuvant anthracycline-containing and anthracycline-free chemotherapy regimens in patients with HER2-positive early breast cancer: a randomized phase II cardiac safety study (TRYPHAENA). Ann Oncol 24:2278–2284
Gianni L, Pienkowski T, Im YH et al (2012) Efficacy and safety of neoadjuvant pertuzumab and trastuzumab in women with locally advanced, inflammatory, or early HER2-positive breast cancer (NeoSphere): a randomised multicentre, open-label, phase 2 trial. Lancet Oncol 13:25–32
Symmans WF, Wei C, Gould R et al (2017) Long-term prognostic risk after neoadjuvant chemotherapy associated with residual cancer burden and breast cancer subtype. J Clin Oncol 35:1049–1060
von Minckwitz G, Huang CS, Mano MS et al (2019) Trastuzumab emtansine for residual invasive HER2-positive breast cancer. N Engl J Med 380:617–628
Denkert C, von Minckwitz G, Brase JC et al (2015) Tumor-infiltrating lymphocytes and response to neoadjuvant chemotherapy with or without carboplatin in human epidermal growth factor receptor 2-positive and triple-negative primary breast cancers. J Clin Oncol 33:983–991
Salgado R, Denkert C, Campbell C et al (2015) Tumor-infiltrating lymphocytes and associations with pathological complete response and event-free survival in HER2-positive early-stage breast cancer treated with lapatinib and trastuzumab: a secondary analysis of the NeoALTTO trial. JAMA Oncol 1:448–454
Nuciforo P, Pascual T, Cortes J et al (2018) A predictive model of pathologic response based on tumor cellularity and tumor-infiltrating lymphocytes (CelTIL) in HER2-positive breast cancer treated with chemo-free dual HER2 blockade. Ann Oncol 29:170–177
Llombart-Cussac A, Cortes J, Pare L et al (2017) HER2-enriched subtype as a predictor of pathological complete response following trastuzumab and lapatinib without chemotherapy in early-stage HER2-positive breast cancer (PAMELA): an open-label, single-group, multicentre, phase 2 trial. Lancet Oncol 18:545–554
Wolff AC, Hammond MEH, Allison KH et al (2018) Human epidermal growth factor receptor 2 testing in breast cancer: American Society of Clinical Oncology/College of American Pathologists Clinical Practice Guideline Focused Update. Arch Pathol Lab Med 142:1364–1382
Meisel JL, Zhao J, Suo A et al (2020) Clinicopathologic factors associated with response to neoadjuvant anti-HER2-directed chemotherapy in HER2-positive breast cancer. Clin Breast Cancer 20(1):19–24
Afghahi A, Purington N, Han SS (2018) Higher absolute lymphocyte counts predict lower mortality from early-stage triple-negative breast cancer. Clin Cancer 24:2851–2858
Curtis CN, West RB, Horst K et al (2014) Prognostic value of tumor-infiltrating lymphocytes in triple-negative breast cancers from two phase III randomized adjuvant breast cancer trials: ECOG 2197 and ECOG 1199. Clin Cancer Res 32:2959–2966
Loi S, Drubay D, Adams S et al (2019) Tumor-infiltrating lymphocytes and prognosis: a pooled individual patient analysis of early-stage triple-negative breast cancers. J Clin Oncol 37:559–569
Krishnamurti U, Wetherilt CS, Yang J et al (2017) Tumor-infiltrating lymphocytes are significantly associated with better overall survival and disease-free survival in triple-negative but not estrogen receptor-positive breast cancers. Hum Pathol 64:7–12
Li XB, Krishnamurti U, Bhattarai S et al (2016) Biomarkers predicting pathologic complete response to neoadjuvant chemotherapy in breast cancer. Am J Clin Pathol 145:871–878
Stanton SE, Disis ML (2016) Clinical significance of tumor-infiltrating lymphocytes in breast cancer. J Immunother Cancer 4:59
Perez EA, Ballman KV, Tenner KS et al (2016) Association of stromal tumor-infiltrating lymphocytes with recurrence-free survival in the N9831 adjuvant trial in patients with early-stage HER2-positive breast cancer. JAMA Oncol 2:56–64
Loi S, Michiels S, Salgado R et al (2014) Tumor infiltrating lymphocytes are prognostic in triple negative breast cancer and predictive for trastuzumab benefit in early breast cancer: results from the FinHER trial. Ann Oncol 25:1544–1550
Kurozumi S, Inoue K, Matsumoto H et al (2019) Clinicopathological values of PD-L1 expression in HER2-positive breast cancer. Sci Rep 9:16662
Peng GL, Li L, Guo YW et al (2019) CD8(+) cytotoxic and FoxP3(+) regulatory T lymphocytes serve as prognostic factors in breast cancer. Am J Transl Res 11:5039–5053
Lee KH, Kim EY, Yun JS et al (2018) The prognostic and predictive value of tumor-infiltrating lymphocytes and hematologic parameters in patients with breast cancer. BMC Cancer 18:938
Liu S, Chen B, Burugu S et al (2017) Role of cytotoxic tumor-infiltrating lymphocytes in predicting outcomes in metastatic HER2-positive breast cancer: a secondary analysis of a randomized clinical trial. JAMA Oncol 3:e172085
Takada K, Kashiwagi S (2018) Use of the tumor-infiltrating CD8 to FOXP3 lymphocyte ratio in predicting treatment responses to combination therapy with pertuzumab, trastuzumab, and docetaxel for advanced HER2-positive breast cancer. J Transl Med 16:86
De Angelis C, Nagi C, Hoyt CC et al (2020) Evaluation of the predictive role of tumor immune infiltrate in patients with HER2-positive breast cancer treated with neoadjuvant anti-HER2 therapy without chemotherapy. Clin Cancer 26:738–745
Glajcar A, Szpor J, Hodorowicz-Zaniewska D et al (2019) The composition of T cell infiltrates varies in primary invasive breast cancer of different molecular subtypes as well as according to tumor size and nodal status. Virchows Arch 475:13–23
Nederlof I, De Bortoli D, Bareche Y et al (2019) Comprehensive evaluation of methods to assess overall and cell-specific immune infiltrates in breast cancer. Breast Cancer 21:151
Li X, Wetherilt CS, Krishnamurti U et al (2016) Stromal PD-L1 expression is associated with better disease-free survival in triple-negative breast cancer. Am J Clin Pathol 146:496–502
Zhang L, Wang XI, Ding J et al (2019) The predictive and prognostic value of Foxp3+/CD25+ regulatory T cells and PD-L1 expression in triple negative breast cancer. Ann Diagn Pathol 40:143–151
Hou Y, Nitta H, Wei L et al (2018) PD-L1 expression and CD8-positive T cells are associated with favorable survival in HER2-positive invasive breast cancer. Breast J 24:911–919
Schmid P, Adams S, Rugo HS et al (2018) Atezolizumab and nab-paclitaxel in advanced triple-negative breast cancer. N Engl J Med 379:2108–2121
Schmid P, Rugo HS, Adams S et al (2020) Atezolizumab plus nab-paclitaxel as first-line treatment for unresectable, locally advanced or metastatic triple-negative breast cancer (IMpassion130): updated efficacy results from a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Oncol 21:44–59
Lawson NL, Dix CI, Scorer PW et al (2020) Mapping the binding sites of antibodies utilized in programmed cell death ligand-1 predictive immunohistochemical assays for use with immuno-oncology therapies. Mod Pathol 33:518–530
Martinez-Morilla S, McGuire J, Gaule P et al (2020) Quantitative assessment of PD-L1 as an analyte in immunohistochemistry diagnostic assays using a standardized cell line tissue microarray. Lab Invest 100:4–15
Hirsch FR, McElhinny A, Stanforth D et al (2017) PD-L1 immunohistochemistry assays for lung cancer: results from phase 1 of the blueprint PD-L1 IHC assay comparison project. J Thorac Oncol 12:208–222
Tsao MS, Kerr KM, Kockx M et al (2018) PD-L1 immunohistochemistry comparability study in real-life clinical samples: results of blueprint phase 2 project. J Thorac Oncol 13:1302–1311
Adams S, Schmid P, Rugo HS et al (2019) Pembrolizumab monotherapy for previously treated metastatic triple-negative breast cancer: cohort A of the phase II KEYNOTE-086 study. Ann Oncol 30:397–404
Adams S, Loi S, Toppmeyer D et al (2019) Pembrolizumab monotherapy for previously untreated, PD-L1-positive, metastatic triple-negative breast cancer: cohort B of the phase II KEYNOTE-086 study. Ann Oncol 30:405–411
Schmid P, Cortes J, Pusztai L et al (2020) Pembrolizumab for early triple-negative breast cancer. N Engl J Med 382:810–821
Voorwerk L, Slagter M, Horlings HM et al (2019) Immune induction strategies in metastatic triple-negative breast cancer to enhance the sensitivity to PD-1 blockade: the TONIC trial. Nat Med 25:920–928
Loibl S, Untch M, Burchardi N et al (2019) A randomised phase II study investigating durvalumab in addition to an anthracycline taxane-based neoadjuvant therapy in early triple-negative breast cancer: clinical results and biomarker analysis of GeparNuevo study. Ann Oncol 30:1279–1288
Emens L, Esteva F, Beresford M et al (2019) Abstract PD3–01: Results from KATE2, a randomized phase 2 study of atezolizumab (atezo)+trastuzumab emtansine (T-DM1) vs placebo (pbo)+T-DM1 in previously treated HER2+ advanced breast cancer (BC). Cancer Res 79:PD3-01-PD3-01
Loi S, Giobbie-Hurder A, Gombos A et al (2019) Pembrolizumab plus trastuzumab in trastuzumab-resistant, advanced, HER2-positive breast cancer (PANACEA): a single-arm, multicentre, phase 1b–2 trial. Lancet Oncol 20:371–382
Funding
Dr. Jing Zhao received research grant from National Natural Science Foundation of China (NSFC 81602320).
Author information
Authors and Affiliations
Contributions
Conception and design: XL; Analysis and interpretation of data: JZ, YG, XL; Manuscript drafting and reviewing: All authors; XL is responsible for the overall content.
Corresponding author
Ethics declarations
Conflict of interest
Dr. Jane Meisel has been advisor for Puma and Pfizer and received research grants from Seattle Genetics, Pfizer and Lilly. Other authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhao, J., Meisel, J., Guo, Y. et al. Evaluation of PD-L1, tumor-infiltrating lymphocytes, and CD8+ and FOXP3+ immune cells in HER2-positive breast cancer treated with neoadjuvant therapies. Breast Cancer Res Treat 183, 599–606 (2020). https://doi.org/10.1007/s10549-020-05819-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-020-05819-8