Abstract
Purpose
Metastatic triple-negative breast cancer (TNBC) is a phenotypic breast cancer subgroup with a very poor prognosis, despite standard treatments. Combined twice-weekly iniparib and gemcitabine/carboplatin (GC+tw-iniparib) showed benefit over gemcitabine/carboplatin in a randomized phase II trial, and a phase III was initiated comparing these regimens. The present phase II study was initiated to compare GC+tw-iniparib with a more practical once-weekly schedule (GC+w-iniparib) in TNBC.
Methods
Metastatic TNBC patients were randomized to receive iniparib weekly (11.2 mg/kg on days 1 and 8) or twice-weekly (5.6 mg/kg on days 1, 4, 8, and 11) with gemcitabine (1000 mg/m2) and carboplatin (area under the curve 2 on days 1 and 8), every 3 weeks. The primary endpoint was the overall response rate (ORR). Pharmacokinetics of iniparib and its two metabolites were analyzed.
Results
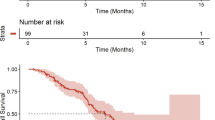
A total of 163 patients were randomized, 82 GC+w-iniparib and 81 GC+tw-iniparib. Demographic and baseline characteristics were well balanced. ORR was 34.1% (95% CI 23.9–44.4%) vs. 29.6% (95% CI 19.7–39.6%) and median progression-free survival was 5.5 months (95% CI 4.2–5.7) vs. 4.3 months (95% CI 3.0–5.8) for GC+w-iniparib and GC+tw-iniparib, respectively. Safety was similar across treatment arms in terms of event severity and type. Iniparib plasma concentrations and exposure were two-fold higher with w-iniparib compared to tw-iniparib. Iniparib and its metabolites were cleared rapidly with a terminal half-life of < 1 h, without accumulation.
Conclusions
Despite a doubled maximum concentration with weekly iniparib, no detectable differences in safety or efficacy were observed between the weekly and twice-weekly administration schedules in this population.
Trial registration
ClinicalTrial.gov Identifier NCT01045304.


Similar content being viewed by others
Abbreviations
- AE:
-
Adverse events
- AUC2:
-
Carboplatin area under the curve
- CBR:
-
Clinical benefit rate
- ER:
-
Estrogen receptor
- GC+w-iniparib:
-
Gemcitabine-carboplatin plus weekly iniparib
- GC+tw-iniparib:
-
Gemcitabine-carboplatin plus twice-weekly iniparib
- HER2:
-
Human epidermal growth factor receptor 2
- IABA:
-
4-Iodo-3-amino-benzoic acid
- IABM:
-
4-Iodo-aminobenzamide
- IHC:
-
Immunohistochemistry
- ITT:
-
Intent-to-treat
- ORR:
-
Overall response rate
- OS:
-
Overall survival
- PARP:
-
Poly(ADP-ribose)polymerase
- PFS:
-
Progression-free survival
- PR:
-
Progesterone receptor
- RECIST:
-
Response Evaluation Criteria in Solid Tumors
- TNBC:
-
Triple-negative breast cancers
- ULN:
-
Upper limit of normal
References
Howlader N, Altekruse SF, Li CI et al (2014) US incidence of breast cancer subtypes defined by joint hormone receptor and HER2 status. J Natl Cancer Inst. https://doi.org/10.1093/jnci/dju055
Carey LA, Perou CM, Livasy CA et al (2006) Race, breast cancer subtypes, and survival in the Carolina Breast Cancer Study. JAMA 295:2492–2502. https://doi.org/10.1001/jama.295.21.2492
Dent R, Trudeau M, Pritchard KI et al (2007) Triple-negative breast cancer: clinical features and patterns of recurrence. Clin Cancer Res 13:4429–4434. https://doi.org/10.1158/1078-0432.CCR-06-3045
Dent R, Hanna WM, Trudeau M et al (2009) Pattern of metastatic spread in triple-negative breast cancer. Breast Cancer Res Treat 115:423–428. https://doi.org/10.1007/s10549-008-0086-2
Lin NU, Vanderplas A, Hughes ME et al (2012) Clinicopathologic features, patterns of recurrence, and survival among women with triple-negative breast cancer in the National Comprehensive Cancer Network. Cancer 118:5463–5472. https://doi.org/10.1002/cncr.27581
Kennecke H, Yerushalmi R, Woods R et al (2010) Metastatic behavior of breast cancer subtypes. J Clin Oncol 28:3271–3277. https://doi.org/10.1200/JCO.2009.25.9820
Kassam F, Enright K, Dent R et al (2009) Survival outcomes for patients with metastatic triple-negative breast cancer: implications for clinical practice and trial design. Clin Breast Cancer 9:29–33. https://doi.org/10.3816/CBC.2009.n.005
Tutt A, Tovey H, Cheang MCU et al (2018) Carboplatin in BRCA1/2-mutated and triple-negative breast cancer BRCAness subgroups: the TNT Trial. Nat Med 24:628–637. https://doi.org/10.1038/s41591-018-0009-7
Schmid P, Adams S, Rugo HS et al (2018) Atezolizumab and nab-paclitaxel in advanced triple-negative breast cancer. N Engl J Med. https://doi.org/10.1056/NEJMoa1809615
Robson M, Im S-A, Senkus E et al (2017) Olaparib for metastatic breast cancer in patients with a germline BRCA mutation. N Engl J Med 377:523–533. https://doi.org/10.1056/NEJMoa1706450
Litton JK, Rugo HS, Ettl J et al (2018) Talazoparib in patients with advanced breast cancer and a germline BRCA mutation. N Engl J Med 379:753–763. https://doi.org/10.1056/NEJMoa1802905
Liu X, Shi Y, Maag DX et al (2012) Iniparib nonselectively modifies cysteine-containing proteins in tumor cells and is not a bona fide PARP inhibitor. Clin Cancer Res 18:510–523. https://doi.org/10.1158/1078-0432.CCR-11-1973
Patel AG, De Lorenzo SB, Flatten KS et al (2012) Failure of iniparib to inhibit poly(ADP-ribose) polymerase in vitro. Clin Cancer Res 18:1655–1662. https://doi.org/10.1158/1078-0432.CCR-11-2890
O’Shaughnessy J, Osborne C, Pippen JE et al (2011) Iniparib plus chemotherapy in metastatic triple-negative breast cancer. N Engl J Med 364:205–214. https://doi.org/10.1056/NEJMoa1011418
O’Shaughnessy J, Schwartzberg L, Danso MA et al (2014) Phase III study of iniparib plus gemcitabine and carboplatin versus gemcitabine and carboplatin in patients with metastatic triple-negative breast cancer. J Clin Oncol 32:3840–3847. https://doi.org/10.1200/JCO.2014.55.2984
Simon R, Wittes RE, Ellenberg SS (1985) Randomized phase II clinical trials. Cancer Treat Rep 69:1375–1381
Mendeleyev J, Kirsten E, Hakam A et al (1995) Potential chemotherapeutic activity of 4-iodo-3-nitrobenzamide. Metabolic reduction to the 3-nitroso derivative and induction of cell death in tumor cells in culture. Biochem Pharmacol 50:705–714
Lee JJ, Feng L (2005) Randomized phase II designs in cancer clinical trials: current status and future directions. J Clin Oncol 23:4450–4457. https://doi.org/10.1200/JCO.2005.03.197
Verweij J, Diéras V, Rockich K et al (2011) A134 Pharmacokinetics and metabolism of iniparib for the treatment of metastatic triple-negative breast cancer (TNBC). Mol Cancer Ther. https://doi.org/10.1158/1535-7163.targ-11-a134:1
Acknowledgements
We thank the patients, their families, and the investigators who participated in this study. We thank Nathalie Debbas and Sarah MacKenzie (MediAxe, France, funded by Sanofi) for assistance drafting the manuscript, and Wenjuan Zhang (Sanofi) for programming support.
Funding
This study was funded by Sanofi.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
EC, GTE and IGR are current or former employees and have stock options of Sanofi. JG and JV have received remuneration and/or had an advisory/consultancy role for Sanofi. VD, EA, AA, JG, and JV have/had a consultancy/advisory role with and/or received remuneration from pharmaceutical companies other than Sanofi. All other authors declare no potential conflicts of interest (HB, BC, XP, AJ, SZ, GL, RP).
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Diéras, V., Bonnefoi, H., Alba, E. et al. Iniparib administered weekly or twice-weekly in combination with gemcitabine/carboplatin in patients with metastatic triple-negative breast cancer: a phase II randomized open-label study with pharmacokinetics. Breast Cancer Res Treat 177, 383–393 (2019). https://doi.org/10.1007/s10549-019-05305-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-019-05305-w