Abstract
Purpose
This study aimed to identify patterns of relapse after neoadjuvant chemotherapy (NAC) for breast cancer to refine follow-up recommendations.
Methods
Retrospective analysis on 523 breast cancer patients treated with NAC at two public hospitals in Singapore between 2000 and 2014.
Results
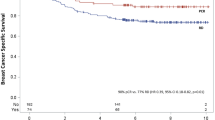
Majority of patients (71.9%) had locally advanced disease. Median follow-up was 55 months. 5-year recurrence rate was significantly higher in triple negative breast cancer (TNBC) than non-TNBC subtypes (38.4% vs. 29.5%; p = 0.042); 85% of recurrences involved distant sites. Among TNBC and HR (hormone receptor)-/HER2+ subtypes, 97.0% and 95.0% of relapses occurred within 3 years from diagnosis respectively while 10.6% of relapses among HR+ subgroup occurred beyond 5 years. Recurrence risk in high-grade tumours decreased with time. Stage III at diagnosis (hazard ratio = 2.94; p < 0.001), grade 3 tumours (hazard ratio = 2.87; p = 0.018), not achieving pathologic complete response (pCR) (hazard ratio = 8.77; p = 0.003) and not receiving adjuvant radiotherapy (hazard ratio = 3.19; p < 0.001) were independent predictors of inferior recurrence-free survival. Serum CA 15-3 was raised in 49% of patients upon relapse; it correlated with inferior post-relapse survival (median 11 months vs. 22 months; p = 0.019).
Conclusions
While more intensive follow-up during the first 3 years may be required for patients who do not achieve pCR, especially those with TNBC and HR−/HER2+ tumours, the benefit from blood tests such as CA 15-3 appears limited, and the benefit from intensification of surveillance remains to be addressed in prospective studies on high-risk patients.


Similar content being viewed by others
Data availability
The datasets during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Fisher B, Bryant J, Wolmark N, Mamounas E, Brown A, Fisher ER et al (1998) Effect of preoperative chemotherapy on the outcome of women with operable breast cancer. J Clin Oncol 16(8):2672–2685
van der Hage JA, van de Velde CJ, Julien JP, Tubiana-Hulin M, Vandervelden C, Duchateau L (2001) Preoperative chemotherapy in primary operable breast cancer: results from the European Organization for Research and Treatment of Cancer trial 10902. J Clin Oncol 19:4224–4237
Mauri D, Pavlidis N, Ioannidis JPA (2005) Neoadjuvant versus adjuvant systemic treatment in breast cancer: a meta-analysis. J Natl Cancer Inst 97(3):188–194
Early Breast Cancer Trialists’ Collaborative Group (EBCTCG) (2018) Long-term outcomes for neoadjuvant versus adjuvant chemotherapy in early breast cancer: meta-analysis of individual patient data from ten randomised trials. Lancet Oncol 19(1):27–39
Kong X, Moran MS, Zhang N, Haffty B, Yang Q (2011) Meta-analysis confirms achieving pathological complete response after neoadjuvant chemotherapy predicts favourable prognosis for breast cancer patients. Eur J Cancer 47(14):2084–2090
Cortazar P, Zhang L, Untch M, Mehta K, Costantino JP, Wolmark N et al (2014) Pathological complete response and long-term clinical benefit in breast cancer: the CTNeoBC pooled analysis. Lancet 384(9938):164–172
Carey LA, Dees EC, Sawyer L, Gatti L, Moore DT, Collichio F et al (2007) The triple negative paradox: primary tumor chemosensitivity of breast cancer subtypes. Clin Cancer Res 13(8):2329–2334
Liedtke C, Mazouni C, Hess KR, André F, Tordai A, Mejia JA et al (2008) Response to neoadjuvant therapy and long-term survival in patients with triple-negative breast cancer. J Clin Oncol 26(8):1275–1281
Kuerer HM, Newman LA, Smith TL, Ames FC, Hunt KK, Dhingra K et al (1999) Clinical course of breast cancer patients with complete pathologic primary tumor and axillary lymph node response to doxorubicin-based neoadjuvant chemotherapy. J Clin Oncol 17:460–469
Wolmark N, Wang J, Mamounas E, Bryant J, Fisher B (2001) Preoperative chemotherapy in patients with operable breast cancer: nine-year results from National Surgical Adjuvant Breast and Bowel Project B-18. J Natl Cancer Inst Monogr 15212(30):96–102
Chollet P, Amat S, Cure H, De Latour M, Le Bouedec G, Mouret-Reynier MA et al (2002) Prognostic significance of a complete pathological response after induction chemotherapy in operable breast cancer. Br J Cancer 86(7):1041–1046
Tanioka M, Shimizu C, Yonemori K, Yoshimura K, Tamura K, Kouno T et al (2010) Predictors of recurrence in breast cancer patients with a pathologic complete response after neoadjuvant chemotherapy. Br J Cancer 103(3):297–302
Takada M, Ishiguro H, Nagai S, Ohtani S, Kawabata H, Yanagita Y et al (2014) Survival of HER2-positive primary breast cancer patients treated by neoadjuvant chemotherapy plus trastuzumab: a multicenter retrospective observational study (JBCRG-C03 study). Breast Cancer Res Treat 145(1):143–153
Hamy-Petit AS, Belin L, Bonsang-Kitzis H, Paquet C, Pierga JY, Lerebours F et al (2016) Pathological complete response and prognosis after neoadjuvant chemotherapy for HER2-positive breast cancers before and after trastuzumab era: results from a real-life cohort. Br J Cancer 114(1):44–52
Hammond ME, Hayes DF, Dowsett M et al (2010) American Society of Clinical Oncology/College of American Pathologists guideline recommendations for immunohistochemical testing of estrogen and progesterone receptors in breast cancer (unabridged version). Arch Pathol Lab Med 134:48–72
Baulies S, Belin L, Mallon P, Senechal C, Pierga JY, Cottu P et al (2015) Time-varying effect and long-term survival analysis in breast cancer patients treated with neoadjuvant chemotherapy. Br J Cancer 113(1):30–36
Bardia A, Baselga J (2013) Neoadjuvant therapy as a platform for drug development and approval in breast cancer. Clin Cancer Res 19(23):6360–6370
Fei F, Messina C, Slaets L, Chakiba C, Cameron D, Bogaerts J et al (2015) Tumour size is the only predictive factor of distant recurrence after pathological complete response to neoadjuvant chemotherapy in patients with large operable or locally advanced breast cancers: a sub-study of EORTC 10994/BIG 1-00 phase III trial. Eur J Cancer 51(3):301–309
Ghezzi P, Magnanini S, Rinaldini M, Berardi F, Di Biagio G, Testare F et al (1994) Impact of follow-up testing on survival and health-related quality of life in breast cancer patients: a multicenter randomized controlled trial. JAMA 271(20):1587–1592
Rosselli Del Turco M, Palli D, Cariddi A, Ciatto S, Pacini P, Distante V (1994) Intensive diagnostic follow-up after treatment of primary breast cancer. A randomized trial. National Research Council Project on Breast Cancer follow-up. JAMA 271(20):1593–1597
Oltra A, Santaballa A, Munárriz B, Pastor M, Montalar J (2007) Cost-benefit analysis of a follow-up program in patients with breast cancer: a randomized prospective study. Breast J 13(6):571–574
Pivot X, Asmar L, Hortobagyi GN, Theriault R, Pastorini F, Buzdar A (2000) A retrospective study of first indicators of breast cancer recurrence. Oncology 58:185–190
Viot J, Bachour M, Meurisse A, Pivot X, Fiteni F (2017) Follow-up of patients with localized breast cancer and first indicators of advanced breast cancer recurrence: a retrospective study. Breast 34:53–57
Hojo T, Masuda N, Mizutani T, Shibata T, Kinoshita T, Tamura K et al (2015) Intensive vs. standard post-operative surveillance in high-risk breast cancer patients (INSPIRE): Japan clinical oncology group study JCOG1204. Jpn J Clin Oncol 45:983–986
Runowicz CD, Leach CR, Henry NL, Henry KS, Mackey HT, Cowens-Alvarado RL et al (2016) American cancer society/American society of clinical oncology breast cancer survivorship care guideline. J Clin Oncol 34:611–635
Funding
No funding was required for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr Yap reported consulting for and receiving honoraria, travel support from Novartis, Pfizer, Lilly, Astra Zeneca, Roche, Eisai, and research support from Novartis.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This study was done under approval of SingHealth Centralised Institutional Review Board (Reference Number: CIRB 2004/422/B) and was conducted according to institutional and ethical rules concerning research on patients, with waiver of consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Saw, S., Lim, J., Lim, S.H. et al. Patterns of relapse after neoadjuvant chemotherapy in breast cancer: implications for surveillance in clinical practice. Breast Cancer Res Treat 177, 197–206 (2019). https://doi.org/10.1007/s10549-019-05290-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-019-05290-0