Abstract
Purpose
To systematically review the literature on the expression of PD-L1 in primary BC, variation of expression between subtypes and effect on overall survival (OS), disease-free survival (DFS), and recurrence-free survival (RFS). Additionally, for studies in the neoadjuvant setting, we have reviewed the ability of PD-L1 to predict pathological complete response (pCR).
Methods
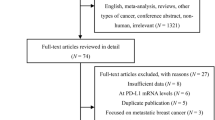
Articles included in this review were retrieved by searching PubMed (1966–2018) and EMBASE (1980–2018). The following search terms were used: “PD-L1 expression” and “breast cancer” (PubMed234; EMBASE 161).
Results
Thirty-seven articles were found relevant to this study. We summarize important findings from these works, and show that the observed PD-L1 expression in the studies varies greatly, with expression rates ranging from 0 to 83% across subtypes. PD-L1 expression in relation to prognosis both in the adjuvant and neoadjuvant chemotherapy setting remains controversial, with studies finding better, worse, or no effect on prognosis. We also show that a wide variety of strategies are used when evaluating PD-L1 immunohistochemically, e.g., different cut-off points, different cell types evaluated, and different perceptions of when a cell is positive for PD-L1 (cytoplasmic vs membrane staining).
Conclusion
Further investigation of PD-L1 expression in breast cancer and its effect on prognosis is required. There is little consensus on the methods used to evaluate PD-L1 expression immunohistochemically, and this may contribute to the diverging results found in this study.

Similar content being viewed by others
References
Barnet MB, Cooper WA, Boyer MJ et al (2018) Immunotherapy in non-small cell lung cancer: shifting prognostic paradigms. J Clin Med. https://doi.org/10.3390/jcm7060151
Marconcini R, Spagnolo F, Stucci LS et al (2018) Current status and perspectives in immunotherapy for metastatic melanoma. Oncotarget 9(15):12452–12470. https://doi.org/10.18632/oncotarget.23746
Polk A, Svane I-M, Andersson M et al (2018) Checkpoint inhibitors in breast cancer—current status. Cancer Treat Rev 63:122–134. https://doi.org/10.1016/j.ctrv.2017.12.008
Tolba MF, Omar HA (2018) Immunotherapy, an evolving approach for the management of triple negative breast cancer: converting non-responders to responders. Crit Rev Oncol Hematol 122:202–207. https://doi.org/10.1016/j.critrevonc.2018.01.005
Rugo HS, Delord J-P, Im S-A et al (2018) Safety and antitumor activity of pembrolizumab in patients with estrogen receptor-positive/human epidermal growth factor receptor 2-negative advanced breast cancer. Clin Cancer Res 24:2804–2811. https://doi.org/10.1158/1078-0432.CCR-17-3452
Perou CM, Sørlie T, Eisen MB et al (2000) Molecular portraits of human breast tumours. Nature 406:747–752. https://doi.org/10.1038/35021093
Ali HR, Glont S-EE, Blows FM et al (2015) PD-L1 protein expression in breast cancer is rare, enriched in basal-like tumours and associated with infiltrating lymphocytes. Ann Oncol 26:1488–1493. https://doi.org/10.1093/annonc/mdv192
Tsang JYS, Au W-L, Lo K-Y et al (2017) PD-L1 expression and tumor infiltrating PD-1 + lymphocytes associated with outcome in HER2 + breast cancer patients. Breast Cancer Res Treat 162:19–30. https://doi.org/10.1007/s10549-016-4095-2
Botti G, Collina F, Scognamiglio G et al (2017) Programmed death ligand 1 (PD-L1) tumor expression is associated with a better prognosis and diabetic disease in triple negative breast cancer patients. Int J Mol Sci. https://doi.org/10.3390/ijms18020459
Ghebeh H, Tulbah A, Mohammed S et al (2007) Expression of B7-H1 in breast cancer patients is strongly associated with high proliferative Ki-67-expressing tumor cells. Int J Cancer 121:751–758. https://doi.org/10.1002/ijc.22703
Zhang M, Sun H, Zhao S et al (2017) Expression of PD-L1 and prognosis in breast cancer: a meta-analysis. Oncotarget 8:31347–31354. https://doi.org/10.18632/oncotarget.15532
Prat A, Pineda E, Adamo B et al (2015) Clinical implications of the intrinsic molecular subtypes of breast cancer. Breast 24:S26–S35. https://doi.org/10.1016/j.breast.2015.07.008
Cheang MCU, Martin M, Nielsen TO et al (2015) Defining breast cancer intrinsic subtypes by quantitative receptor expression. Oncologist 20:474–482. https://doi.org/10.1634/theoncologist.2014-0372
Nielsen TO, Hsu FD, Jensen K et al (2004) Immunohistochemical and clinical characterization of the basal-like subtype of invasive breast carcinoma. Clin Cancer Res 10(16):5367–5374. https://doi.org/10.1158/1078-0432.CCR-04-0220
Keir ME, Butte MJ, Freeman GJ et al (2008) PD-1 and its ligands in tolerance and immunity. Annu Rev Immunol 26:677–704. https://doi.org/10.1146/annurev.immunol.26.021607.090331
Cimino-Mathews A, Thompson E, Taube JM et al (2016) PD-L1 (B7-H1) expression and the immune tumor microenvironment in primary and metastatic breast carcinomas. Hum Pathol 47:52–63. https://doi.org/10.1016/j.humpath.2015.09.003
Pardoll DM (2012) The blockade of immune checkpoints in cancer immunotherapy. Nat Rev Cancer 12:252–264. https://doi.org/10.1038/nrc3239
Ribas A, Hu-Lieskovan S (2016) What does PD-L1 positive or negative mean? J Exp Med 213:2835–2840. https://doi.org/10.1084/jem.20161462
Taube JM, Anders RA, Young GD et al (2012) Colocalization of inflammatory response with B7-h1 expression in human melanocytic lesions supports an adaptive resistance mechanism of immune escape. Sci Transl Med 4:127ra37. https://doi.org/10.1126/scitranslmed.3003689
Bedognetti D, Hendrickx W, Marincola FM et al (2015) Prognostic and predictive immune gene signatures in breast cancer. Curr Opin Oncol 27:433–444. https://doi.org/10.1097/CCO.0000000000000234
Buisseret L, Garaud S, de Wind A et al (2017) Tumor-infiltrating lymphocyte composition, organization and PD-1/ PD-L1 expression are linked in breast cancer. Oncoimmunology 6:e1257452. https://doi.org/10.1080/2162402X.2016.1257452
Schalper KA (2014) PD-L1 expression and tumor-infiltrating lymphocytes. Oncoimmunology 3:e29288. https://doi.org/10.4161//onci.29288
Wimberly H, Brown JR, Schalper K et al (2015) PD-L1 expression correlates with tumor-infiltrating lymphocytes and response to neoadjuvant chemotherapy in breast cancer. Cancer Immunol Res 3:326–332. https://doi.org/10.1158/2326-6066
Ghebeh H, Mohammed S, Al-Omair A et al (2006) The B7-H1 (PD-L1) T lymphocyte-inhibitory molecule is expressed in breast cancer patients with infiltrating ductal carcinoma: correlation with important high-risk prognostic factors. Neoplasia 8:190–198. https://doi.org/10.1593/neo.05733
Schalper KA, Velcheti V, Carvajal D et al (2014) In situ tumor PD-L1 mRNA expression is associated with increased TILs and better outcome in breast carcinomas. Clin Cancer Res 20:2773–2782. https://doi.org/10.1158/1078-0432.CCR-13-2702
Bae SB, Cho HD, Oh M-H et al (2016) Expression of programmed death receptor ligand 1 with high tumor-infiltrating lymphocytes is associated with better prognosis in breast cancer. J Breast Cancer 19:242–251. https://doi.org/10.4048/jbc.2016.19.3.242
Baptista MZ, Sarian LO, Derchain SFM et al (2016) Prognostic significance of PD-L1 and PD-L2 in breast cancer. Hum Pathol 47:78–84. https://doi.org/10.1016/j.humpath.2015.09.006
Beckers RK, Selinger CI, Vilain R et al (2016) Programmed death ligand 1 expression in triple-negative breast cancer is associated with tumour-infiltrating lymphocytes and improved outcome. Histopathology 69:25–34. https://doi.org/10.1111/his.12904
Sabatier R, Finetti P, Mamessier E et al (2015) Prognostic and predictive value of PDL1 expression in breast cancer. Oncotarget 6:5449–5464. https://doi.org/10.18632/oncotarget.3216
Qin T, Zeng Y, Qin G et al (2015) High PD-L1 expression was associated with poor prognosis in 870 Chinese patients with breast cancer. Oncotarget 6:33972–33981. https://doi.org/10.18632/oncotarget.5583
Mori H, Kubo M, Yamaguchi R et al (2017) The combination of PD-L1 expression and decreased tumor-infiltrating lymphocytes is associated with a poor prognosis in triple-negative breast cancer. Oncotarget 8:15584–15592. https://doi.org/10.18632/oncotarget.14698
Gandini S, Massi D, Mandalà M (2016) PD-L1 expression in cancer patients receiving anti PD-1/PD-L1 antibodies: a systematic review and meta-analysis. Crit Rev Oncol Hematol 100:88–98. https://doi.org/10.1016/j.critrevonc.2016.02.001
Aguiar PN, De Mello RA, Hall P et al (2017) PD-L1 expression as a predictive biomarker in advanced non-small-cell lung cancer: updated survival data. Immunotherapy 9:499–506. https://doi.org/10.2217/imt-2016-0150
Zou W, Wolchok JD, Chen L (2016) PD-L1 (B7-H1) and PD-1 pathway blockade for cancer therapy: mechanisms, response biomarkers, and combinations. Sci Transl Med 8:328rv4. https://doi.org/10.1126/scitranslmed.aad7118
Karnik T, Kimler BF, Fan F et al (2018) PD-L1 in breast cancer: comparative analysis of 3 different antibodies. Hum Pathol 72:28–34. https://doi.org/10.1016/j.humpath.2017.08.010
Sun WY, Lee YK, Koo JS (2016) Expression of PD-L1 in triple-negative breast cancer based on different immunohistochemical antibodies. J Transl Med 14:173. https://doi.org/10.1186/s12967-016-0925-6
Udall M, Rizzo M, Kenny J et al (2018) PD-L1 diagnostic tests: a systematic literature review of scoring algorithms and test-validation metrics. Diagn Pathol 13:12. https://doi.org/10.1186/s13000-018-0689-9
Sakane T, Murase T, Okuda K et al (2018) A comparative study of PD-L1 immunohistochemical assays with four reliable antibodies in thymic carcinoma. Oncotarget 9:6993–7009. https://doi.org/10.18632/oncotarget.24075
Roche Ventana. http://www.ventana.com/ventana-pd-l1-sp263-assay-2/. Accessed 13 June 2018
Muenst S, Schaerli AR, Gao F et al (2014) Expression of programmed death ligand 1 (PD-L1) is associated with poor prognosis in human breast cancer. Breast Cancer Res Treat 146:15–24. https://doi.org/10.1007/s10549-014-2988-5
Gatalica Z, Snyder C, Maney T et al (2014) Programmed cell death 1 (PD-1) and its ligand (PD-L1) in common cancers and their correlation with molecular cancer type. Cancer Epidemiol Biomark Prev 23:2965–2970. https://doi.org/10.1158/1055-9965.EPI-14-0654
Park IH, Kong S-Y, Ro JY et al (2016) Prognostic implications of tumor-infiltrating lymphocytes in association with programmed death ligand 1 expression in early-stage breast cancer. Clin Breast Cancer 16:51–58. https://doi.org/10.1016/j.clbc.2015.07.006
Li Z, Dong P, Ren M et al (2016) PD-L1 Expression Is associated with tumor FOXP3(+) regulatory T-cell Infiltration of breast cancer and poor prognosis of patient. J Cancer 7:784–793. https://doi.org/10.7150/jca.14549
Okabe M, Toh U, Iwakuma N et al (2017) Predictive factors of the tumor immunological microenvironment for long-term follow-up in early stage breast cancer. Cancer Sci 108:81–90. https://doi.org/10.1111/cas.13114
Joneja U, Vranic S, Swensen J et al (2017) Comprehensive profiling of metaplastic breast carcinomas reveals frequent overexpression of programmed death-ligand 1 (2017). J Clin Pathol 70:255–259. https://doi.org/10.1136/jclinpath-2016-203874
Wang Z-Q, Milne K, Derocher H et al (2017) PD-L1 and intratumoral immune response in breast cancer. Oncotarget 8(31):51641–51651. https://doi.org/10.18632/oncotarget.18305
Polónia A, Pinto R, Cameselle-Teijeiro JF et al (2017) Prognostic value of stromal tumour infiltrating lymphocytes and programmed cell death-ligand 1 expression in breast cancer. J Clin Pathol 70:860–867. https://doi.org/10.1136/jclinpath-2016-203990
Kim A, Lee SJ, Kim YK et al (2017) Programmed death-ligand 1 (PD-L1) expression in tumour cell and tumour infiltrating lymphocytes of HER2-positive breast cancer and its prognostic value. Sci Rep 7:11671. https://doi.org/10.1038/s41598-017-11905-7
Tung N, Garber JE, Hacker MR et al (2016) Prevalence and predictors of androgen receptor and programmed death-ligand 1 in BRCA1-associated and sporadic triple-negative breast cancer. NPJ breast cancer 2:16002. https://doi.org/10.1038/npjbcancer.2016.2
Guo L, Li W, Zhu X et al (2016) PD-L1 expression and CD274 gene alteration in triple-negative breast cancer: implication for prognostic biomarker. Springerplus 5:805. https://doi.org/10.1186/s40064-016-2513-x
Nanda R, Chow LQM, Dees EC et al (2016) Pembrolizumab in patients with advanced triple-negative breast cancer: phase Ib KEYNOTE-012 study. J Clin Oncol 34:2460–2467. https://doi.org/10.1200/JCO.2015.64.8931
Adams TA, Vail PJ, Ruiz A et al (2018) Composite analysis of immunological and metabolic markers defines novel subtypes of triple negative breast cancer. Mod Pathol 31:288–298. https://doi.org/10.1038/modpathol.2017
Choi SH, Chang JS, Koo JS et al (2018) Differential prognostic impact of strong PD-L1 expression and 18F-FDG uptake in triple-negative breast cancer. Am J Clin Oncol. https://doi.org/10.1097/COC.0000000000000426
Mittendorf EA, Philips AV, Meric-Bernstam F et al (2017) PD-L1 expression in triple-negative breast cancer. Cancer Immunol Res 2:361–370. https://doi.org/10.1158/2326-6066.CIR-13-0127
AiErken N, Shi H-J, Zhou Y et al (2017) High PD-L1 expression is closely associated with tumor-infiltrating lymphocytes and leads to good clinical outcomes in chinese triple negative breast cancer patients. Int J Biol Sci 13:1172–1179. https://doi.org/10.7150/ijbs.20868
Lou J, Zhou Y, Huang J et al (2017) Relationship between PD-L1 expression and clinical characteristics in patients with breast invasive ductal carcinoma. Open Med 12:288–292. https://doi.org/10.1515/med-2017-0042
Li F, Ren Y, Wang Z. Programmed death 1 Ligand 1 expression in breast cancer and its association with patients’ clinical parameters (2018). J Cancer Res Ther 14:150–154. https://doi.org/10.4103/jcrt.JCRT_602_17
Dill EA, Gru AA, Atkins KA et al (2017) PD-L1 expression and intratumoral heterogeneity across breast cancer subtypes and stages. Am J Surg Pathol 41:334–342. https://doi.org/10.1097/PAS.0000000000000780
McLemore LE, Janakiram M, Albanese J et al (2017) An immunoscore using PD-L1, CD68, and tumor-infiltrating lymphocytes (TILs) to predict response to neoadjuvant chemotherapy in invasive breast cancer. Appl Immunohistochem Mol Morphol 26(9):611–619. https://doi.org/10.1097/PAI.0000000000000485
Kitano A, Ono M, Yoshida M et al (2017) Tumour-infiltrating lymphocytes are correlated with higher expression levels of PD-1 and PD-L1 in early breast cancer. ESMO Open 2:e000150. https://doi.org/10.1136/esmoopen-2016-000150
Pelekanou V, Barlow WE, Nahleh ZA et al (2018) Tumor-infiltrating lymphocytes and PD-L1 expression in pre- and posttreatment breast cancers in the SWOG S0800 phase II neoadjuvant chemotherapy trial. Mol Cancer Ther 17:1324–1331. https://doi.org/10.1158/1535-7163.MCT-17-1005
Cerbelli B, Pernazza A, Botticelli A et al (2017) PD-L1 Expression in TNBC: a predictive biomarker of response to neoadjuvant chemotherapy? Biomed Res Int 2017:1750925. https://doi.org/10.1155/2017/1750925
Wang Y, Dong T, Xuan Q et al (2018) Lymphocyte-activation gene-3 expression and prognostic value in neoadjuvant-treated triple-negative breast cancer. J Breast Cancer 21:124–133. https://doi.org/10.4048/jbc.2018.21.2.124
Hou Y, Nitta H, Wei L et al (2018) Evaluation of immune reaction and PD-L1 expression using multiplex immunohistochemistry in HER2-positive breast cancer: the association with response to anti-HER2 neoadjuvant therapy. Clin Breast Cancer 18:e237–e244. https://doi.org/10.1016/j.clbc.2017.11.001
Büttner R, Gosney JR, Skov BG et al (2017) Programmed death-ligand 1 immunohistochemistry testing: a review of analytical assays and clinical implementation in non-small-cell lung cancer. J Clin Oncol 35:3867–3876. https://doi.org/10.1200/JCO.2017.74.7642
Gniadek TJ, Li QK, Tully E et al (2017) Heterogeneous expression of PD-L1 in pulmonary squamous cell carcinoma and adenocarcinoma: implications for assessment by small biopsy. Mod Pathol 30:530–538. https://doi.org/10.1038/modpathol.2016.213
Li M, Li A, Zhou S et al (2018) Heterogeneity of PD-L1 expression in primary tumors and paired lymph node metastases of triple negative breast cancer. BMC Cancer 18:4. https://doi.org/10.1186/s12885-017-3916-y
Ogiya R, Niikura N, Kumaki N et al (2016) Comparison of tumor-infiltrating lymphocytes between primary and metastatic tumors in breast cancer patients. Cancer Sci 107:1730–1735. https://doi.org/10.1111/cas.13101
Zins K, Heller G, Mayerhofer M et al (2018) Differential prognostic impact of interleukin-34 mRNA expression and infiltrating immune cell composition in intrinsic breast cancer subtypes. Oncotarget 9:23126–23148. https://doi.org/10.18632/oncotarget.25226
Salgado R, Denkert C, Campbell C et al (2015) Tumor-infiltrating lymphocytes and associations with pathological complete response and event-free survival in HER2-positive early-stage breast cancer treated with lapatinib and trastuzumab: a secondary analysis of the NeoALTTO trial. JAMA Oncol 1:448–454. https://doi.org/10.1001/jamaoncol.2015.0830
Schmid P, Adams S, Rugo HS et al (2018) Atezolizumab and nab-paclitaxel in advanced triple-negative breast cancer. N Engl J Med 379(22):2108–2121. https://doi.org/10.1056/NEJMoa1809615
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Stovgaard, E.S., Dyhl-Polk, A., Roslind, A. et al. PD-L1 expression in breast cancer: expression in subtypes and prognostic significance: a systematic review. Breast Cancer Res Treat 174, 571–584 (2019). https://doi.org/10.1007/s10549-019-05130-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-019-05130-1