Abstract
Purpose
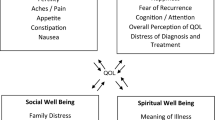
Compared with young White women, young Black women are more likely to present with aggressive breast cancer (BC) subtypes that are potentially linked to worse health-related quality of life (HRQOL); however, there is limited consensus regarding HRQOL needs among young Black BC survivors. Employing Ferrell’s framework on QOL in BC (i.e., physical, psychological, social, and spiritual well-being), we conducted a systematic review on HRQOL among Black BC survivors aged <50 years and proposed recommendations for advancing HRQOL research and care for this population.
Methods
Literature searches were conducted in MEDLINE/PubMed, EMBASE, CINAHL, and PsycINFO to identify relevant articles published from 1995 to 2015. Abstracts and full-text articles were screened using predetermined inclusion/exclusion criteria and evaluated for quality.
Results
A total of 2533 articles were identified, but six met eligibility criteria. Most studies examined multiple HRQOL domains, with the psychological domain most represented. Compared with their older, White, and BC-free counterparts, young Black BC survivors reported greater fear of dying, unmet supportive care needs, financial distress, and lower physical/functional well-being. However, spiritual well-being appeared favorable for young Black survivors. Research gaps include the absence of longitudinal studies and under-representation of studies examining physical, social, and particularly, spiritual HRQOL in young Black BC survivors.
Conclusions
Young Black BC survivors generally experience suboptimal HRQOL after BC diagnosis. As few studies have reported on HRQOL among this group, future research and oncology care should prioritize young Black women in ways that recognize their unique concerns, in order to ensure better HRQOL outcomes both during and after treatment.


Similar content being viewed by others
References
WHO (2013) Breast cancer: prevention and control. World Health Organization. http://www.who.int/cancer/detection/breastcancer/en/index1.html. Accessed 24 Sept 2013
ACS (2015) Breast cancer facts and figures 2015–2016. Am Cancer Soc. Access 02(03/2016):2016
Harper S, Lynch J, Meersman SC, Breen N, Davis WW, Reichman MC (2009) Trends in area-socioeconomic and race-ethnic disparities in breast cancer incidence, stage at diagnosis, screening, mortality, and survival among women ages 50 years and over (1987–2005). Cancer Epidemiol Biomarkers Prev 18(1):121–131. doi:10.1158/1055-9965.epi-08-0679
Reeder-Hayes KE, Wheeler SB, Mayer DK (2015) Health disparities across the breast cancer continuum. Semin Oncol Nurs 31(2):170–177. doi:10.1016/j.soncn.2015.02.005
Chlebowski RT, Chen Z, Anderson GL, Rohan T, Aragaki A, Lane D, Dolan NC, Paskett ED, McTiernan A, Hubbell FA, Adams-Campbell LL, Prentice R (2005) Ethnicity and breast cancer: factors influencing differences in incidence and outcome. J Natl Cancer Inst 97(6):439–448. doi:10.1093/jnci/dji064
Newman LA, Mason J, Cote D, Vin Y, Carolin K, Bouwman D, Colditz GA (2002) African–American ethnicity, socioeconomic status, and breast cancer survival: a meta-analysis of 14 studies involving over 10,000 African–American and 40,000 White American patients with carcinoma of the breast. Cancer 94(11):2844–2854. doi:10.1002/cncr.10575
Ghafoor A, Jemal A, Ward E, Cokkinides V, Smith R, Thun M (2003) Trends in breast cancer by race and ethnicity. CA Cancer J Clin 53(6):342–355
Vastag B (2003) Breast cancer racial gap examined: no easy answers to explain disparities in survival. J Am Med Assoc 290(14):1838–1842. doi:10.1001/jama.290.14.1838
Li CI, Malone KE, Daling JR (2003) Differences in breast cancer stage, treatment, and survival by race and ethnicity. Arch Intern Med 163(1):49–56
Smigal C, Jemal A, Ward E, Cokkinides V, Smith R, Howe HL, Thun M (2006) Trends in breast cancer by race and ethnicity: update 2006. CA 56(3):168–183
Millikan RC, Newman B, Tse CK, Moorman PG, Conway K, Dressler LG, Smith LV, Labbok MH, Geradts J, Bensen JT, Jackson S, Nyante S, Livasy C, Carey L, Earp HS, Perou CM (2008) Epidemiology of basal-like breast cancer. Breast Cancer Res Treat 109(1):123–139. doi:10.1007/s10549-007-9632-6
Anderson WF, Jatoi I, Devesa SS (2005) Distinct breast cancer incidence and prognostic patterns in the NCI’s SEER program: suggesting a possible link between etiology and outcome. Breast Cancer Res Treat 90(2):127–137. doi:10.1007/s10549-004-3777-3
Ahles TA, Saykin AJ, Furstenberg CT, Cole B, Mott LA, Titus-Ernstoff L, Skalla K, Bakitas M, Silberfarb PM (2005) Quality of life of long-term survivors of breast cancer and lymphoma treated with standard-dose chemotherapy or local therapy. J Clin Oncol 23(19):4399–4405. doi:10.1200/jco.2005.03.343
Carver CS, Smith RG, Petronis VM, Antoni MH (2006) Quality of life among long-term survivors of breast cancer: different types of antecedents predict different classes of outcomes. Psycho-oncology 15(9):749–758. doi:10.1002/pon.1006
Ganz PA, Rowland JH, Meyerowitz BE, Desmond KA (1998) Impact of different adjuvant therapy strategies on quality of life in breast cancer survivors. Recent Results Cancer Res 152:396–411
Ganz PA, Desmond KA, Leedham B, Rowland JH, Meyerowitz BE, Belin TR (2002) Quality of life in long-term, disease-free survivors of breast cancer: a follow-up study. J Natl Cancer Inst 94(1):39–49
Bauer KR, Brown M, Cress RD, Parise CA, Caggiano V (2007) Descriptive analysis of estrogen receptor (ER)−negative, progesterone receptor (PR)−negative, and HER2-negative invasive breast cancer, the so-called triple-negative phenotype: a population-based study from the California cancer registry. Cancer 109(9):1721–1728. doi:10.1002/cncr.22618
Ferrell BR, Grant M, Funk B, Garcia N, Otis-Green S, Schaffner ML (1996) Quality of life in breast cancer. Cancer Pract 4(6):331–340
Ferrell BR, Dow KH, Grant M (1995) Measurement of the quality of life in cancer survivors. Qual Life Res 4(6):523–531
Smith AW, Alfano CM, Reeve BB, Irwin ML, Bernstein L, Baumgartner K, Bowen D, McTiernan A, Ballard-Barbash R (2009) Race/ethnicity, physical activity, and quality of life in breast cancer survivors. Cancer Epidemiol Biomark Prev 18(2):656–663. doi:10.1158/1055-9965.epi-08-0352
Mollica M, Nemeth L, Newman SD, Mueller M (2015) Quality of life in african american breast cancer survivors: an integrative literature review. Cancer Nurs 38(3):194–204. doi:10.1097/ncc.0000000000000160
Pinheiro LC, Wheeler SB, Chen RC, Mayer DK, Lyons JC, Reeve BB (2015) The effects of cancer and racial disparities in health-related quality of life among older Americans: a case-control, population-based study. Cancer 121(8):1312–1320. doi:10.1002/cncr.29205
Ashing-Giwa KT, Tejero JS, Kim J, Padilla GV, Hellemann G (2007) Examining predictive models of HRQOL in a population-based, multiethnic sample of women with breast carcinoma. Qual Life Res 16(3):413–428. doi:10.1007/s11136-006-9138-4
Ashing-Giwa K (2000) Quality of life and psychosocial outcomes in long-term survivors of breast cancer. J Psychosoc Oncol 17(3–4):47–62. doi:10.1300/J077v17n03_03
Ashing-Giwa K, Ganz PA, Petersen L (1999) Quality of life of African-American and White long term breast carcinoma survivors. Cancer 85(2):418–426
Von Ah DM, Russell KM, Carpenter J, Monahan PO, Qianqian Z, Tallman E, Ziner KW, Storniolo AM, Miller KD, Giesler RB, Haase J, Otte J, Champion VL (2012) Health-related quality of life of african american breast cancer survivors compared with healthy African American women. Cancer Nurs 35(5):337–346. doi:10.1097/NCC.0b013e3182393de3
Hamilton JB, Powe BD, Pollard AB 3rd, Lee KJ, Felton AM (2007) Spirituality among African American cancer survivors: having a personal relationship with God. Cancer Nurs 30(4):309–316. doi:10.1097/01.NCC.0000281730.17985.f5
Howard-Anderson J, Ganz PA, Bower JE, Stanton AL (2012) Quality of life, fertility concerns, and behavioral health outcomes in younger breast cancer survivors: a systematic review. J Natl Cancer Inst 104(5):386–405. doi:10.1093/jnci/djr541
Arndt V, Merx H, Sturmer T, Stegmaier C, Ziegler H, Brenner H (2004) Age-specific detriments to quality of life among breast cancer patients one year after diagnosis. Eur J Cancer 40(5):673–680. doi:10.1016/j.ejca.2003.12.007
Ganz PA, Greendale GA, Petersen L, Kahn B, Bower JE (2003) Breast cancer in younger women: reproductive and late health effects of treatment. J clin Oncol 21(22):4184–4193. doi:10.1200/jco.2003.04.196
Mor V, Malin M, Allen S (1994) Age differences in the psychosocial problems encountered by breast cancer patients. J Natil Cancer Inst Monogr 16:191–197
Bines J, Oleske DM, Cobleigh MA (1996) Ovarian function in premenopausal women treated with adjuvant chemotherapy for breast cancer. J Clin Oncol 14(5):1718–1729
Goodwin PJ, Ennis M, Pritchard KI, Trudeau M, Hood N (1999) Risk of menopause during the first year after breast cancer diagnosis. J Clin Oncol 17(8):2365–2370
Woods-Giscombé CL, Lobel M (2008) Race and gender matter: a multidimensional approach to conceptualizing and measuring stress in African American women. Cult Divers Ethn Minor Psychol 14(3):173–182. doi:10.1037/1099-9809.14.3.173
Woods-Giscombe CL (2010) Superwoman schema: African American women’s views on stress, strength, and health. Qual Health Res 20(5):668–683. doi:10.1177/1049732310361892
Woods-Giscombe CL, Lobel M, Zimmer C, Wiley Cene C, Corbie-Smith G (2015) Whose stress is making me sick? Network-stress and emotional distress in African-American women. Issues Ment Health Nurs 36(9):710–717. doi:10.3109/01612840.2015.1011759
Black AR, Woods-Giscombé C (2012) Applying the stress and ‘strength’ hypothesis to black women’s breast cancer screening delays. Stress Health 28(5):389–396. doi:10.1002/smi.2464
Powe BD, Hamilton J, Hancock N, Johnson N, Finnie R, Ko J, Brooks P, Boggan M Jr (2007) Quality of life of African American cancer survivors—a review of the literature. Cancer 109(2 Suppl):435–445. doi:10.1002/cncr.22358
Chopra I, Kamal KM (2012) A systematic review of quality of life instruments in long-term breast cancer survivors. Health Qual life Outcomes 10:14. doi:10.1186/1477-7525-10-14
Mols F, Vingerhoets AJ, Coebergh JW, van de Poll-Franse LV (2005) Quality of life among long-term breast cancer survivors: a systematic review. Eur J Cancer 41(17):2613–2619. doi:10.1016/j.ejca.2005.05.017
Cho J, Jung SY, Lee JE, Shim EJ, Kim NH, Kim Z, Sohn G, Youn HJ, Kim KS, Kim H, Lee JW, Lee MH (2014) A review of breast cancer survivorship issues from survivors’ perspectives. J Breast Cancer 17(3):189–199. doi:10.4048/jbc.2014.17.3.189
Palmer JR, Rosenberg L, Wise LA, Horton NJ, Adams-Campbell LL (2003) Onset of natural menopause in African American women. Am J Public Health 93(2):299–306
McCarthy AM, Yang J, Armstrong K (2015) Increasing disparities in breast cancer mortality from 1979 to 2010 for US black women aged 20 to 49 years. Am J Public Health 105(Suppl 3):S446–S448. doi:10.2105/ajph.2014.302297
Howlader N, Noone AM, Krapcho M, Miller D, Bishop K, Altekruse SF, Kosary CL, Yu M, Ruhl J, Tatalovich Z, Mariotto A, Lewis DR, Chen HS, Feuer EJ, Cronin KA (2016) SEER Cancer Statistics Review, 1975–2013. National Cancer Institute, Bethesda
ACS (2014) Life after cancer: survivorship by the numbers. American Cancer Society
Elm V (2008) The strengthening the reporting of observational studies in epidemiology (STROBE)statement: guidelines for reporting observational studies. J Clin Epidemiol 61(4):344–349
CASP (2014) Critical appraisal skills programme (CASP). CASP Checklists
Derogatis LR (1986) The psychosocial adjustment to illness scale (PAIS). J Psychosom Res 30(1):77–91
Cohen SH, Hoberman HM (1983) Positive events and social supports as buffers of life change stress. J Appl Soc Psychol 13:99–125
Brady MJ, Cella DF, Mo F, Bonomi AE, Tulsky DS, Lloyd SR, Deasy S, Cobleigh M, Shiomoto G (1997) Reliability and validity of the functional assessment of cancer therapy-breast quality-of-life instrument. J Clin Oncol 15(3):974–986
Avis NE, Smith KW, McGraw S, Smith RG, Petronis VM, Carver CS (2005) Assessing quality of life in adult cancer survivors (QLACS). Qual Life Res 14(4):1007–1023
Furlanetto LM, Mendlowicz MV, Romildo Bueno J (2005) The validity of the Beck Depression Inventory-Short Form as a screening and diagnostic instrument for moderate and severe depression in medical inpatients. J Affect Disord 86(1):87–91. doi:10.1016/j.jad.2004.12.011
Schuldberg D (1992) Ego-strength revised: a comparison of the MMPI-2 and MMPI-1 versions of the barron ego-strength scale. J Clin Psychol 48(4):500–505
Beder J (1995) Perceived social support and adjustment to mastectomy in socioeconomically disadvantaged black women. Soc Work Health Care 22(2):55–71
Gibson LM, Thomas S, Parker V, Mayo R, Wetsel MA (2014) Breast cancer fear in African American breast cancer survivors. J Cult Divers 21(4):135–144
Lewis PE, Sheng M, Rhodes MM, Jackson KE, Schover LR (2012) Psychosocial concerns of young African American breast cancer survivors. J Psychosoc Oncol 30(2):168–184. doi:10.1080/07347332.2011.651259
Janz NK, Mujahid MS, Hawley ST, Griggs JJ, Alderman A, Hamilton AS, Graff J, Katz SJ (2009) Racial/ethnic differences in quality of life after diagnosis of breast cancer. J Cancer Surviv 3(4):212–222. doi:10.1007/s11764-009-0097-y
Sheppard VB, Llanos AA, Hurtado-de-Mendoza A, Taylor TR, Adams-Campbell LL (2013) Correlates of depressive symptomatology in African-American breast cancer patients. J Cancer Surviv 7(3):292–299. doi:10.1007/s11764-013-0273-y
Morrow PK, Broxson AC, Munsell MF, Basen-Enquist K, Rosenblum CK, Schover LR, Nguyen LH, Hsu L, Castillo L, Hahn KM, Litton JK, Kwiatkowski DN, Hortobagyi GN (2014) Effect of age and race on quality of life in young breast cancer survivors. Clin Breast Cancer 14(2):e21–e31. doi:10.1016/j.clbc.2013.10.003
Geronimus AT, Hicken M, Keene D, Bound J (2006) “Weathering” and age patterns of allostatic load scores among blacks and whites in the United States. Am J Public Health 96(5):826–833. doi:10.2105/ajph.2004.060749
Ware JE Jr (1984) Methodology in behavioral and psychosocial cancer research. conceptualizing disease impact and treatment outcomes. Cancer 53(10 Suppl):2316–2326
Wilson IB, Cleary PD (1995) Linking clinical variables with health-related quality of life. A conceptual model of patient outcomes. JAMA 273(1):59–65
Bourjolly JN (1998) Differences in religiousness among black and white women with breast cancer. Soc Work Health Care 28(1):21–39. doi:10.1300/J010v28n01_02
Gibson LM, Hendricks CS (2006) Integrative review of spirituality in African American breast cancer survivors. ABNF J 17(2):67–72
Holt CL, Schulz E, Caplan L, Blake V, Southward VL, Buckner AV (2012) Assessing the role of spirituality in coping among African Americans diagnosed with cancer. J Relig Health 51(2):507–521. doi:10.1007/s10943-011-9453-0
Torres E, Dixon C, Richman AR (2016) Understanding the breast cancer experience of survivors: a qualitative study of African American women in rural eastern North Carolina. J Cancer Educ 31(1):198–206. doi:10.1007/s13187-015-0833-0
MCC (2013) Psychological distress screening in cancer patients. Michigan Cancer Consortium, Lansing
CoC (2012) Cancer program standards 2012: ensuring patient-centered care. American College of Surgeons, Chicago
NCCN (2016) NCCN Distress thermometer and problem list for patients, 1st edn. National Comprehensive Cancer Network, Washington
Dabrowski M, Boucher K, Ward JH, Lovell MM, Sandre A, Bloch J, Carlquist L, Porter M, Norman L, Buys SS (2007) Clinical experience with the NCCN distress thermometer in breast cancer patients. J Natl Compr Cancer Netw 5(1):104–111
Whitehead NE, Hearn LE (2015) Psychosocial interventions addressing the needs of Black women diagnosed with breast cancer: a review of the current landscape. Psycho-Oncology 24(5):497–507. doi:10.1002/pon.3620
Woods-Giscombé CL, Black AR (2010) Mind-Body interventions to reduce risk for health disparities related to stress and strength among African American women: the potential of mindfulness-based stress reduction, loving-kindness, and the NTU therapeutic framework. Complement Health Pract Rev 15(3):115–131. doi:10.1177/1533210110386776
Duckett PAS (2013) Health coverage for the black population today and under the affordable care Ac. The Henry J Kaiser Family Foundation, Menlo Park
Murthy VH, Krumholz HM, Gross CP (2004) Participation in cancer clinical trials: race-, sex-, and age-based disparities. JAMA 291(22):2720–2726. doi:10.1001/jama.291.22.2720
Keating NL, Kouri E, He Y, Weeks JC, Winer EP (2009) Racial differences in definitive breast cancer therapy in older women: are they explained by the hospitals where patients undergo surgery? Med Care 47(7):765–773. doi:10.1097/MLR.0b013e31819e1fe7
Acknowledgment
CAS and SBW have received a Research Grant from Pfizer for another unrelated study. This article is dedicated in memory of Meleshia Daye, whose courage and strength as a Young Black Woman with Breast Cancer inspired this contribution to research and clinical practice.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
All other authors have no conflicts of interest to disclose.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Samuel, C.A., Pinheiro, L.C., Reeder-Hayes, K.E. et al. To be young, Black, and living with breast cancer: a systematic review of health-related quality of life in young Black breast cancer survivors. Breast Cancer Res Treat 160, 1–15 (2016). https://doi.org/10.1007/s10549-016-3963-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-016-3963-0