Abstract
Background
Recurrent acute and life-threatening metabolic decompensations are thought to be the major cause of mortality and morbidity in patients with propionic acidemia (PA). Since metabolic decompensations in these patients usually develop gradually, there is considerable uncertainty about the beginning and when emergency treatment should be initiated. The major aim of this study was to evaluate the usefulness of biochemical parameters for improving decision-making on the start of emergency treatment.
Methods
We analysed data of 16 PA patients continuously followed in our centre. Metabolic decompensation was defined clinically by the occurrence of at least one of three alarming symptoms: vomiting, food refusal or impaired consciousness. Thirty-eight biochemical parameters were analysed.
Results
A total of 259 metabolic decompensations were documented and compared with 625 routine visits. Among the symptoms used to clinically define metabolic decompensations, vomiting was most frequent (87 %). In total, 19 biochemical parameters differentiated between metabolic decompensations and routine visits. Among them ammonia, acid–base balance and anion gap were most reliable to identify a metabolic decompensation, and to estimate its severity. A comparative analysis of patients with PA and methylmalonic acidemia during metabolic decompensation showed similar results.
Conclusions
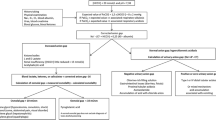
Ammonia, acid–base balance and anion gap are important biochemical parameters to identify an (impending) metabolic decompensation and to assess its severity in PA patients. The identified biochemical parameters should be integrated in an algorithm for clinical decision-making on emergency treatment and should be tested in a prospective trial.


Similar content being viewed by others
Abbreviations
- AC/FC:
-
Ratio of acylcarnitines to free carnitine
- MMA:
-
Methylmalonic acidemia
- PA:
-
Propionic acidemia
- PCC:
-
Propionyl CoA carboxylase, EC 6.4.1.3
- TCA:
-
Tricarboxylic acid
References
Abdi H (2007) Bonferroni and Sidak corrections for multiple comparisons. In: Salkind NJ (ed) Encyclopedia of measurement and statistics. Sage, Thousand Oaks, pp 103–107
Brock M, Buckel W (2004) On the mechanism of action of the antifungal agent propionate. Eur J Biochem 271(15):3227–3241
Brosnan JT, Brosnan ME (2006) Branched-chain amino acids: enzyme and substrate regulation. J Nutr 136(1 Suppl):207–211
Cathelineau L, Petit FP, Coude FX, Kamoun PP (1979) Effect of propionate and pyruvate on citrulline synthesis and ATP content in rat liver mitochondria. Biochem Biophys Res Commun 90:327–332
Chapman KA, Gropman A, Macleod E et al (2012) Acute management of propionic acidemia. Mol Genet Metab 105(1):16–25
Cheema-Dhadli S, Leznoff CC, Halperin ML (1975) Effect of 2-methylcitrate on citrate metabolism: implications for the management of patients with propionic acidemia and methylmalonic aciduria. Pediatr Res 9(12):905–908
Coombs CH, Dawes RM, Tversky A (1970) Mathematical psychology: an elementary introduction. Prentice-Hall, Englewood Cliff
Coude FX, Sweetman L, Nyhan WL (1979) Inhibition by propionyl-coenzyme A of N-acetylglutamate synthetase in rat liver mitochondria. A possible explanation for hyperammonemia in propionic and methylmalonic acidemia. J Clin Invest 64:1544–1551
Dixon MA, Leonard JV (1992) Intercurrent illness in inborn errors of intermediary metabolism. Arch Dis Child 67(11):1387–1391
Edgington ES (1995) Randomization tests, 2nd edn. Dekker, New York
Filipowicz HR, Ernst SL, Ashurst CL, Pasquali M, Longo N (2006) Metabolic changes associated with hyperammonemia in patients with propionic acidemia. Mol Genet Metab 88:123–130
Grünert SC, Müllerleile S, De Silva L et al (2013) Propionic acidemia: clinical course and outcome in 55 pediatric and adolescent patients. Orphanet J Rare Dis 8:6 doi:10.1186/1750-1172-8-6
Howell DC (2012) Resampling Procedures Version 1.3. Retrieved from 2012. [http://www.uvm.edu/∼dhowell/StatPages/Resampling/ResamplingPackage.zip]
Klein NP, Aukes L, Lee J et al (2011) Evaluation of immunization rates and safety among children with inborn errors of metabolism. Pediatrics 127(5):1139–1146
Kraus JP, Spector E, Venezia S et al (2012) Mutation analysis in 54 propionic academia patients. J Inherit Metab Dis 35(1):51–63
Leonard JV, Vijayaraghavan S, Walter JH (2003) The impact of screening for propionic and methylmalonic acidaemia. Eur J Pediatr 162:21–24
Liao JG, Wu YJ, Lin Y (2010) Improving Sheather and Jones bandwidth selector for difficult densities in kernel density estimation. J Nonparametric Stat 22(1):105–114
Morath MA, Okun JG, Müller IB, Sauer SW, Hörster F, Hoffmann GF, Kölker S (2008) Neurodegeneration and chronic renal failure in methylmalonic aciduria-a pathophysiological approach. J Inherit Metab Dis 31:35–43
R Development Core Team (2012) A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna
Sauer SW, Okun JG, Hoffmann GF, Kölker S, Morath MA (2008) Impact of short- and medium-chain organic acids, acylcarnitines, and acyl-CoAs on mitochondrial energy metabolism. Biochim Biophys Acta 1777:1276–1282
Schwab MA, Sauer SW, Okun JG et al (2006) Secondary mitochondrial dysfunction in propionic aciduria, a pathogenic role for endogenous mitochondrial toxins. Biochem J 398(1):107–112
Shih VE (2005) Amino acid analysis. In: Blau N, Duran M, Blaskovics ME, Gibson KM (eds) Physician’s guide to the laboratory diagnosis of metabolic diseases, 2nd edn. Chapman & Hall, London, pp 11–26
Smucker MD, Allan J, Carterette B (2007) A comparison of statistical significance tests for information retrieval evaluation. In Proceedings of the sixteenth ACM conference on Conference on Information and Knowledge Management (CIKM): 3–5 November 2007; Lisbon. Lisbon: ACM Press, 623–632
Zeileis A, Grothendieck G (2005) S3 infrastructure for regular and irregular time series. J Stat Softw 14(6):1–27
Zwickler T, Haege G, Riderer A, Hörster F, Hoffmann GF, Burgard P, Kölker S (2012) Metabolic decompensation in methylmalonic aciduria: which biochemical parameters are discriminative? J Inherit Metab Dis 35:797–806
Acknowledgments
This study is dedicated to the patients and their families whom the authors thank for their trust and kind cooperation. We are grateful to colleagues who participated throughout the years caring for and providing information on their patients, notably M. Lindner, D. Haas, F. Hörster, C. Manegold, C. Pontes and V. Konstantopoulou. We thank the “Arbeitsgemeinschaft für Pädiatrische Stoffwechselstörungen e.V.” for financial support to this study (to T.Z.).
Details of funding
The study was supported by the “Arbeitsgemeinschaft für Pädiatrische Stoffwechselstörungen e.V.” (APS; www.aps-med.de). The authors confirm independence from the sponsors; the content of the article has not been influenced by the sponsors.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
Communicated by: Carlo Dionisi-Vici
References to electronic databases: Propionic acidemia OMIM 606054. Propionyl-CoA carboxylase, α-subunit: PCCA, OMIM 232000, Propionyl-CoA carboxylase, β-subunit: PCCB, OMIM 232050. Propionyl-CoA carboxylase, EC 6.4.1.3, Methylmalonic aciduria due to methylmalonyl-CoA mutase activity deficiency (mut0, mut−), OMIM 251000. Methylmalonyl-CoA mutase, EC 5.4.99.2
Tamaris Zwickler and Alina Riderer contributed equally to this study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary Table 1
(DOC 78 kb)
Supplementary Table 2
(DOC 150 kb)
Supplementary Table 3
(DOC 24 kb)
Rights and permissions
About this article
Cite this article
Zwickler, T., Riderer, A., Haege, G. et al. Usefulness of biochemical parameters in decision-making on the start of emergency treatment in patients with propionic acidemia. J Inherit Metab Dis 37, 31–37 (2014). https://doi.org/10.1007/s10545-013-9621-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10545-013-9621-3