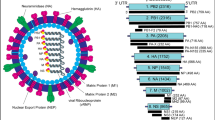
RNA interference in vertebrates acts as an antiviral mechanism only in undifferentiated embryonic stem cells and is mediated by microRNAs. In somatic cells, host microRNAs also bind to the genomes of RNA viruses, regulating their translation and replication. It has been shown that viral (+)RNA can evolve under the influence of host cell miRNAs. In more than two years of the pandemic, the SARS-CoV-2 virus has mutated significantly. It is quite possible that some mutations could be retained in the virus genome under the influence of miRNAs produced by alveolar cells. We demonstrated that microRNAs in human lung tissue exert evolutionary pressure on the SARS-CoV-2 genome. Moreover, a significant number of sites of host microRNA binding with the virus genome are located in the NSP3-NSP5 region responsible for autoproteolysis of viral polypeptides.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Ding SW, Voinnet O. Antiviral immunity directed by small RNAs. Cell. 2007;130(3):413-426. doi: https://doi.org/10.1016/j.cell.2007.07.039
Li Y, Lu J, Han Y, Fan X, Ding SW. RNA interference functions as an antiviral immunity mechanism in mammals. Science. 2013;342:231-234. doi: https://doi.org/10.1126/science.1241911
Siegal FP, Kadowaki N, Shodell M, Fitzgerald-Bocarsly PA, Shah K, Ho S, Antonenko S, Liu YJ. The nature of the principal type 1 interferon-producing cells in human blood. Science. 1999;284:1835-1837. doi: https://doi.org/10.1126/science.284.5421.1835
Turchinovich A, Tonevitsky AG, Cho WC, Burwinkel B. Check and mate to exosomal extracellular miRNA: new lesson from a new approach. Front. Mol. Biosci. 2015;2:11. doi: https://doi.org/10.3389/fmolb.2015.00011
Makarova J, Turchinovich A, Shkurnikov M, Tonevitsky A. Extracellular miRNAs and cell-cell communication: problems and prospects. Trends Biochem. Sci. 2021;46(8):640-651. doi: https://doi.org/10.1016/j.tibs.2021.01.007
Huang J, Wang F, Argyris E, Chen K, Liang Z, Tian H, Huang W, Squires K, Verlinghieri G, Zhang H. Cellular microRNAs contribute to HIV-1 latency in resting primary CD4+ T lymphocytes. Nat. Med. 2007;13(10):1241-1247. doi: https://doi.org/10.1038/nm1639
Ingle H, Kumar S, Raut AA, Mishra A, Kulkarni DD, Kameyama T, Takaoka A, Akira S, Kumar H. The microRNA miR-485 targets host and influenza virus transcripts to regulate antiviral immunity and restrict viral replication. Sci. Signal. 2015;8(406):ra126. doi: https://doi.org/10.1126/scisignal.aab3183
Yekta S, Shih IH, Bartel DP. MicroRNA-directed cleavage of HOXB8 mRNA. Science. 2004;304:594-596. doi: https://doi.org/10.1126/science.1097434
Trobaugh DW, Gardner CL, Sun C, Haddow AD, Wang E, Chapnik E, Mildner A, Weaver SC, Ryman KD, Klimstra WB. RNA viruses can hijack vertebrate microRNAs to suppress innate immunity. Nature. 2014;506:245-248. doi: https://doi.org/10.1038/nature12869
Shimakami T, Yamane D, Jangra RK, Kempf BJ, Spaniel C, Barton DJ, Lemon SM. Stabilization of hepatitis C virus RNA by an Ago2-miR-122 complex. Proc. Natl Acad. Sci. USA. 2012;109(3):941-946. doi: https://doi.org/10.1073/pnas.1112263109
Scheel TK, Luna JM, Liniger M, Nishiuchi E, Rozen-Gagnon K, Shlomai A, Auray G, Gerber M, Fak J, Keller I, Bruggmann R, Darnell RB, Ruggli N, Rice CM. A broad RNA virus survey reveals both miRNA dependence and functional sequestration. Cell Host Microbe. 2016;19(3):409-423. doi: https://doi.org/10.1016/j.chom.2016.02.007
Saçar Demirci MD, Adan A. Computational analysis of microRNA-mediated interactions in SARS-CoV-2 infection. PeerJ. 2020;8:e9369. doi: https://doi.org/10.7717/peerj.9369
Khan MA, Sany MRU, Islam MS, Islam ABMMK. Epigenetic regulator miRNA pattern differences among SARS-CoV, SARS-CoV-2, and SARS-CoV-2 world-wide isolates delineated the mystery behind the epic pathogenicity and distinct clinical characteristics of pandemic COVID-19. Front. Genet. 2020;11:765. doi: https://doi.org/10.3389/fgene.2020.00765
Lukiw WJ. microRNA heterogeneity, innate-immune defense and the efficacy of SARS-CoV-2 infection — a commentary. Noncoding RNA. 2021;7(2):37. doi: https://doi.org/10.3390/ncrna7020037
Nersisyan S, Engibaryan N, Gorbonos A, Kirdey K, Makhonin A, Tonevitsky A. Potential role of cellular miRNAs in coronavirus-host interplay. PeerJ. 2020;8:e9994. doi: https://doi.org/10.7717/peerj.9994
Nersisyan S, Gorbonos A, Makhonin A, Zhiyanov A, Shkurnikov M, Tonevitsky A. isomiRTar: a comprehensive portal of pan-cancer 5’-isomiR targeting. PeerJ. 2022;10:e14205. doi: https://doi.org/10.7717/peerj.14205
Nersisyan S, Zhiyanov A, Shkurnikov M, Tonevitsky A. T-CoV: a comprehensive portal of HLA-peptide interactions affected by SARS-CoV-2 mutations. Nucleic Acids Res. 2022;50(D1):D883-D887. doi: https://doi.org/10.1093/nar/gkab701
Khare S, Gurry C, Freitas L, Schultz MB, Bach G, Diallo A, Akite N, Ho J, Lee RT, Yeo W, Curation Team GC, Maurer-Stroh S. GISAID’s Role in Pandemic Response. China CDC Wkly. 2021;3(49):1049-1051. doi: https://doi.org/10.46234/ccdcw2021.255
O’Toole Á, Scher E, Underwood A, Jackson B, Hill V, McCrone JT, Colquhoun R, Ruis C, Abu-Dahab K, Taylor B, Yeats C, du Plessis L, Maloney D, Medd N, Attwood SW, Aanensen DM, Holmes EC, Pybus OG, Rambaut A. Assignment of epidemiological lineages in an emerging pandemic using the pangolin tool. Virus Evol. 2021;7(2):veab064. doi: https://doi.org/10.1093/ve/veab064
Robinson MD, McCarthy DJ, Smyth GK. edgeR: a Bioconductor package for differential expression analysis of digital gene expression data. Bioinformatics. 2010;26(1):139-140. doi: https://doi.org/10.1093/bioinformatics/btp616
Grimson A, Farh KK, Johnston WK, Garrett-Engele P, Lim LP, Bartel DP. MicroRNA targeting specificity in mammals: determinants beyond seed pairing. Mol. Cell. 2007;27(1):91-105. doi: https://doi.org/10.1016/j.molcel.2007.06.017
Katoh K, Misawa K, Kuma K, Miyata T. MAFFT: a novel method for rapid multiple sequence alignment based on fast Fourier transform. Nucleic Acids Res. 2002;30(14):3059-3066. doi: https://doi.org/10.1093/nar/gkf436
Badua CLDC, Baldo KAT, Medina PMB. Genomic and proteomic mutation landscapes of SARS-CoV-2. J. Med. Virol. 2021;93(3):1702-1721. doi: https://doi.org/10.1002/jmv.26548
Hartenian E, Nandakumar D, Lari A, Ly M, Tucker JM, Glaunsinger BA. The molecular virology of coronaviruses. J. Biol. Chem. 2020;295(37):12910-12934. doi: https://doi.org/10.1074/jbc.REV120.013930
Zhang Y, Chen Y, Li Y, Huang F, Luo B, Yuan Y, Xia B, Ma X, Yang T, Yu F, Liu J, Liu B, Song Z, Chen J, Yan S, Wu L, Pan T, Zhang X, Li R, Huang W, He X, Xiao F, Zhang J, Zhang H. The ORF8 protein of SARS-CoV-2 mediates immune evasion through down-regulating MHC-Ι. Proc. Natl Acad. Sci. USA. 2021;118(23):e2024202118. doi: https://doi.org/10.1073/pnas.2024202118
Matsuoka K, Imahashi N, Ohno M, Ode H, Nakata Y, Kubota M, Sugimoto A, Imahashi M, Yokomaku Y, Iwatani Y. SARS-CoV-2 accessory protein ORF8 is se-creted extracellularly as a glycoprotein homodimer. J. Biol. Chem. 2022;298(3):101724. doi: https://doi.org/10.1016/j.jbc.2022.101724
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Kletochnye Tekhnologii v Biologii i Meditsine, No. 4, pp. 216-221, December 2022
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhiyanov, A.P., Shkurnikov, M.Y. SARS-CoV-2 Mutations Lead to a Decrease in the Number of Tissue-Specific MicroRNA-Binding Regions in the Lung. Bull Exp Biol Med 174, 527–532 (2023). https://doi.org/10.1007/s10517-023-05742-0
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10517-023-05742-0