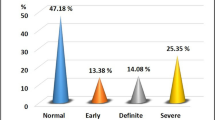
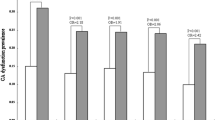
In a one-stage cross-sectional study, a continuous sample of 102 patients (mean age 47.81±0.63 years) with metabolic syndrome was examined. It was found that autonomic dysfunction determines specific features of arterial hypertension in this group of patients, it causes cardiac autonomic neuropathy and underlies the mechanisms of lower urinary tract symptoms development.
Similar content being viewed by others
References
Babunts IV, Miridzhanyan EM, Mashaekh YuA. Alphabet of the Analysis oh Heart Rate Variability. Moscow, 2011. Russian.
Vertkin AL, Zairat’yants OV, Zvyagintseva EI, Adonina EV, Lukashov MI, Lyubshina OV, Aristrakhova OYu, Gurgenidze MT, Shamuilova MM, Mikaberidze EN. Metabolic syndrome in the cardiovascular continuum. Lech. Vrach. 2008(3):71-77. Russian.
Udut VV, Kseneva SI, Borodulina EV, Trifonova OY. Patent RU No. 2585741. Method for early diagnosis of autonomic cardiac neuropathy in patients with arterial hypertension and metabolic disorders. Bull. No. 16. Published June 10, 2016.
Sakovets TG. Diabetic autonomic neuropathy as a risk factor for emergencies. Kazan. Med. Zh. 2016;97(6):931-934. Russian.
Tyuzikov IA, Martov AG, Grekov EA. The correlation of metabolic syndrome components and hormonal disorders in prostate diseases pathogenesis. Eksper. Klin. Urol. 2012(3):39-47. Russian.
Heart rate variability: standards of measurement, physiological interpretation and clinical use. Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. Circulation. 1996;93(5):1043-1065.
Kikuya M, Hozawa A, Ohokubo T, Tsuji I, Michimata M, Matsubara M, Ota M, Nagai K, Araki T, Satoh H, Ito S, Hisamichi S, Imai Y. Prognostic significance of blood pressure and heart rate varisbilities: the Ohasama Study. Hypertension. 2000;36(5):901-906.
McVary K. Lower urinary tract symptoms and sexual dysfunction: epidemiology and pathophysiology. BJU Int. 2006;97(Suppl. 2):23-28.
Sega R, Corrao G, Bombelli M, Beltrame L, Facchetti R, Grassi G, Ferrario M, Mancia G. Blood pressure variability and organ damage in a general population: results from the PAMELA Study. Hypertension. 2002;39(2, Pt 2):710-714.
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Byulleten’ Eksperimental’noi Biologii i Meditsiny, Vol. 164, No. 9, pp. 280-284, September, 2017
Rights and permissions
About this article
Cite this article
Kseneva, S.I., Borodulina, E.V. & Udut, V.V. Extension of the Metabolic Syndrome Cluster. Bull Exp Biol Med 164, 304–307 (2018). https://doi.org/10.1007/s10517-018-3977-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10517-018-3977-1