Abstract
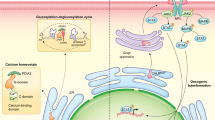
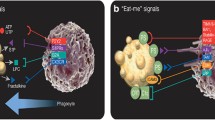
Calreticulin (CRT) is a pleiotropic and highly conserved molecule that is mainly localized in the endoplasmic reticulum. Recently, CRT has gained special interest for its functions outside the endoplasmic reticulum where it has immunomodulatory properties. CRT translocation to the cell membrane serves as an “eat me” signal and promotes efferocytosis of apoptotic cells and cancer cell removal with completely opposite outcomes. Efferocytosis results in a silenced immune response and homeostasis, while removal of dying cancer cells brought about by anthracycline treatment, ionizing-irradiation or photodynamic therapy results in immunogenic cell death with activation of the innate and adaptive immune responses. In addition, CRT impacts phagocyte activation and cytokine production. The effects of CRT on cytokine production depend on its conformation, species specificity, degree of oligomerization and/or glycosylation, as well as its cellular localization and the molecular partners involved. The controversial roles of CRT in cancer progression and the possible role of the CALR gene mutations in myeloproliferative neoplasms are also addressed. The release of CRT and its influence on the different cells involved during efferocytosis and immunogenic cell death points to additional roles of CRT besides merely acting as an “eat me” signal during apoptosis. Understanding the contribution of CRT in physiological and pathological processes could give us some insight into the potential of CRT as a therapeutic target.


Similar content being viewed by others
References
Spiro RG, Zhu Q, Bhoyroo V, Söling HD (1996) Definition of the lectin-like properties of the molecular chaperone, calreticulin, and demonstration of its copurification with endomannosidase from rat liver Golgi. J Biol Chem 271:11588–11594
Patil AR, Thomas CJ, Surolia A (2000) Kinetics and the mechanism of interaction of the endoplasmic reticulum chaperone, calreticulin, with monoglucosylated (Glc1 Man9 GlcNAc2) substrate. J Biol Chem 275:24348–24356. https://doi.org/10.1074/jbc.M003102200
Michalak M, Groenendyk J, Szabo E et al (2009) Calreticulin, a multi-process calcium-buffering chaperone of the endoplasmic reticulum. Biochem J 417:651–666. https://doi.org/10.1042/BJ20081847
Coppolino MG, Dedhar S (1998) Calreticulin. Int J Biochem Cell Biol 30:553–558
Rojiani MV, Finlay BB, Gray V, Dedhar S (1991) In vitro interaction of a polypeptide homologous to human Ro/SS-A antigen (calreticulin) with a highly conserved amino acid sequence in the cytoplasmic domain of integrin alpha subunits. Biochemistry 30:9859–9866
Burns K, Atkinson EA, Bleackley RC, Michalak M (1994) Calreticulin: from Ca2+ binding to control of gene expression. Trends Cell Biol 4:152–154
Ellgaard L, Riek R, Herrmann T et al (2001) NMR structure of the calreticulin P-domain. Proc Natl Acad Sci USA 98:3133–3138. https://doi.org/10.1073/pnas.051630098
Jiang Y, Dey S, Matsunami H (2014) Calreticulin: roles in cell-surface protein expression. Membranes (Basel) 4:630–641. https://doi.org/10.3390/membranes4030630
Baksh S, Michalak M (1991) Expression of calreticulin in Escherichia coli and identification of its Ca2+ binding domains. J Biol Chem 266:21458–21465
Muñoz LE, Lauber K, Schiller M et al (2010) The role of defective clearance of apoptotic cells in systemic autoimmunity. Nat Rev Rheumatol 6:280–289. https://doi.org/10.1038/nrrheum.2010.46
Clarke C, Smyth MJ (2007) Calreticulin exposure increases cancer immunogenicity. Nat Biotechnol 25:192–193. https://doi.org/10.1038/nbt0207-192
Henson PM (2017) Cell removal: efferocytosis. Annu Rev Cell Dev Biol 33:127–144. https://doi.org/10.1146/annurev-cellbio-111315-125315
Ogden CA, deCathelineau A, Hoffmann PR et al (2001) C1q and mannose binding lectin engagement of cell surface calreticulin and CD91 initiates macropinocytosis and uptake of apoptotic cells. J Exp Med 194:781–795
Wijeyesakere SJ, Bedi SK, Huynh D, Raghavan M (2016) The C-terminal acidic region of calreticulin mediates phosphatidylserine binding and apoptotic cell phagocytosis. J Immunol 196:3896–3909. https://doi.org/10.4049/jimmunol.1502122
Tarr JM, Young PJ, Morse R et al (2010) A mechanism of release of calreticulin from cells during apoptosis. J Mol Biol 401:799–812. https://doi.org/10.1016/j.jmb.2010.06.064
Osman R, Tacnet-Delorme P, Kleman J-P et al (2017) Calreticulin release at an early stage of death modulates the clearance by macrophages of apoptotic cells. Front Immunol 8:1–13. https://doi.org/10.3389/fimmu.2017.01034
Nayak A, Ferluga J, Tsolaki AG, Kishore U (2010) The non-classical functions of the classical complement pathway recognition subcomponent C1q. Immunol Lett 131:139–150. https://doi.org/10.1016/j.imlet.2010.03.012
Verneret M, Tacnet-Delorme P, Osman R et al (2014) Relative contribution of C1q and apoptotic cell-surface calreticulin to macrophage phagocytosis. J Innate Immun 6:426–434. https://doi.org/10.1159/000358834
Païdassi H, Tacnet-Delorme P, Verneret M et al (2011) Investigations on the C1q–calreticulin–phosphatidylserine interactions yield new insights into apoptotic cell recognition. J Mol Biol 408:277–290. https://doi.org/10.1016/j.jmb.2011.02.029
Stuart GR, Lynch NJ, Day AJ et al (1997) The C1q and collectin binding site within C1q receptor (cell surface calreticulin). Immunopharmacology 38:73–80
Païdassi H, Tacnet-Delorme P, Garlatti V et al (2008) C1q binds phosphatidylserine and likely acts as a multiligand-bridging molecule in apoptotic cell recognition. J Immunol 180:2329–2338
Vandivier RW, Ogden CA, Fadok VA et al (2002) Role of surfactant proteins A, D, and C1q in the clearance of apoptotic cells in vivo and in vitro: calreticulin and CD91 as a common collectin receptor complex. J Immunol 169:3978–3986
Takemura Y, Ouchi N, Shibata R et al (2007) Adiponectin modulates inflammatory reactions via calreticulin receptor-dependent clearance of early apoptotic bodies. J Clin Invest 117:375–386. https://doi.org/10.1172/JCI29709
Krispin A, Bledi Y, Atallah M et al (2006) Apoptotic cell thrombospondin-1 and heparin-binding domain lead to dendritic-cell phagocytic and tolerizing states. Blood 108:3580–3589. https://doi.org/10.1182/blood-2006-03-013334
Krysko DV, Ravichandran KS, Vandenabeele P (2018) Macrophages regulate the clearance of living cells by calreticulin. Nat Commun 9:4644. https://doi.org/10.1038/s41467-018-06807-9
Gardai SJ, McPhillips KA, Frasch SC et al (2005) Cell-surface calreticulin initiates clearance of viable or apoptotic cells through trans-activation of LRP on the phagocyte. Cell 123:321–334. https://doi.org/10.1016/j.cell.2005.08.032
Takizawa H, Manz MG (2007) Macrophage tolerance: CD47-SIRP-α-mediated signals matter. Nat Immunol 8:1287
Feng M, Marjon KD, Zhu F et al (2018) Programmed cell removal by calreticulin in tissue homeostasis and cancer. Nat Commun 9:3194. https://doi.org/10.1038/s41467-018-05211-7
Byrne JC, Ní Gabhann J, Stacey KB et al (2013) Bruton’s tyrosine kinase is required for apoptotic cell uptake via regulating the phosphorylation and localization of calreticulin. J Immunol 190:5207–5215. https://doi.org/10.4049/jimmunol.1300057
Feng M, Chen JY, Weissman-Tsukamoto R et al (2015) Macrophages eat cancer cells using their own calreticulin as a guide: roles of TLR and Btk. Proc Natl Acad Sci USA 112:2145–2150. https://doi.org/10.1073/pnas.1424907112
Berwin B, Hart JP, Rice S et al (2003) Scavenger receptor-A mediates gp96/GRP94 and calreticulin internalization by antigen-presenting cells. EMBO J 22:6127–6136. https://doi.org/10.1093/emboj/cdg572
Platt N, Suzuki H, Kurihara Y et al (1996) Role for the class A macrophage scavenger receptor in the phagocytosis of apoptotic thymocytes in vitro. Proc Natl Acad Sci USA 93:12456–12460
Ren Y, Tang J, Mok MY et al (2003) Increased apoptotic neutrophils and macrophages and impaired macrophage phagocytic clearance of apoptotic neutrophils in systemic lupus erythematosus. Arthritis Rheum 48:2888–2897. https://doi.org/10.1002/art.11237
Wermeling F, Chen Y, Pikkarainen T et al (2007) Class A scavenger receptors regulate tolerance against apoptotic cells, and autoantibodies against these receptors are predictive of systemic lupus. J Exp Med 204:2259–2265. https://doi.org/10.1084/jem.20070600
Chen X, Shen Y, Sun C et al (2011) Anti-class a scavenger receptor autoantibodies from systemic lupus erythematosus patients impair phagocytic clearance of apoptotic cells by macrophages in vitro. Arthritis Res Ther 13:R9. https://doi.org/10.1186/ar3230
Duo C-C, Gong F-Y, He X-Y et al (2014) Soluble calreticulin induces tumor necrosis factor-α (TNF-α) and interleukin (IL)-6 production by macrophages through mitogen-activated protein kinase (MAPK) and NFκB signaling pathways. Int J Mol Sci 15:2916–2928. https://doi.org/10.3390/ijms15022916
Hong C, Qiu X, Li Y et al (2010) Functional analysis of recombinant calreticulin fragment 39–272: implications for immunobiological activities of calreticulin in health and disease. J Immunol 185:4561–4569. https://doi.org/10.4049/jimmunol.1000536
Huang S-H, Zhao L-X, Hong C et al (2013) Self-oligomerization is essential for enhanced immunological activities of soluble recombinant calreticulin. PLoS ONE 8:e64951. https://doi.org/10.1371/journal.pone.0064951
Gong F-Y, Gong Z, Duo C-C et al (2018) Aberrant Glycosylation augments the immuno-stimulatory activities of soluble calreticulin. Molecules 23:523. https://doi.org/10.3390/molecules23030523
Bajor A, Tischer S, Figueiredo C et al (2011) Modulatory role of calreticulin as chaperokine for dendritic cell-based immunotherapy. Clin Exp Immunol 165:220–234. https://doi.org/10.1111/j.1365-2249.2011.04423.x
Bak SP, Amiel E, Walters JJ, Berwin B (2008) Calreticulin requires an ancillary adjuvant for the induction of efficient cytotoxic T cell responses. Mol Immunol 45:1414–1423. https://doi.org/10.1016/j.molimm.2007.08.020
Ramsamooj P, Notario V, Dritschilo A (1995) Enhanced expression of calreticulin in the nucleus of radioresistant squamous carcinoma cells in response to ionizing radiation. Cancer Res 55:3016–3021
Galluzzi L, Kroemer G (2017) Calreticulin and type I interferon: an unsuspected connection. Oncoimmunology 6:e1288334. https://doi.org/10.1080/2162402X.2017.1288334
Fucikova J, Becht E, Iribarren K et al (2016) Calreticulin expression in human non-small cell lung cancers correlates with increased accumulation of antitumor immune cells and favorable prognosis. Cancer Res 76:1746–1756. https://doi.org/10.1158/0008-5472.CAN-15-1142
Obeid M, Tesniere A, Ghiringhelli F et al (2007) Calreticulin exposure dictates the immunogenicity of cancer cell death. Nat Med 13:54–61. https://doi.org/10.1038/nm1523
Casares N, Pequignot MO, Tesniere A et al (2005) Caspase-dependent immunogenicity of doxorubicin-induced tumor cell death. J Exp Med 202:1691–1701. https://doi.org/10.1084/jem.20050915
Panaretakis T, Kepp O, Brockmeier U et al (2009) Mechanisms of pre-apoptotic calreticulin exposure in immunogenic cell death. EMBO J 28:578–590. https://doi.org/10.1038/emboj.2009.1
de Bruyn M, Wiersma VR, Helfrich W et al (2015) The ever-expanding immunomodulatory role of calreticulin in cancer immunity. Front Oncol 5:35. https://doi.org/10.3389/fonc.2015.00035
Twomey JD, Kim S-R, Zhao L et al (2015) Spatial dynamics of TRAIL death receptors in cancer cells. Drug Resist Updat 19:13–21. https://doi.org/10.1016/j.drup.2015.02.001
Lu YC, Weng WC, Lee H (2015) Functional roles of calreticulin in cancer biology. Biomed Res Int 2015:1–9
Mesaeli N, Phillipson C (2004) Impaired p53 expression, function, and nuclear localization in calreticulin-deficient cells. Mol Biol Cell 15:1862–1870. https://doi.org/10.1091/mbc.e03-04-0251
Stoll G, Iribarren K, Michels J et al (2016) Calreticulin expression: interaction with the immune infiltrate and impact on survival in patients with ovarian and non-small cell lung cancer. Oncoimmunology 5:e1177692. https://doi.org/10.1080/2162402X.2016.1177692
Chen C-N, Chang C-C, Su T-E et al (2009) Identification of calreticulin as a prognosis marker and angiogenic regulator in human gastric cancer. Ann Surg Oncol 16:524–533. https://doi.org/10.1245/s10434-008-0243-1
Becker J, Pavlakovic H, Ludewig F et al (2010) Neuroblastoma progression correlates with downregulation of the lymphangiogenesis inhibitor sVEGFR-2. Clin Cancer Res 16:1431–1441. https://doi.org/10.1158/1078-0432.CCR-09-1936
Weng W-C, Lin K-H, Wu P-Y et al (2015) Calreticulin regulates VEGF-A in neuroblastoma cells. Mol Neurobiol 52:758–770. https://doi.org/10.1007/s12035-014-8901-8
Pike SE, Yao L, Setsuda J et al (1999) Calreticulin and calreticulin fragments are endothelial cell inhibitors that suppress tumor growth. Blood 94:2461–2468
Zamanian M, Qader Hamadneh LA, Veerakumarasivam A et al (2016) Calreticulin mediates an invasive breast cancer phenotype through the transcriptional dysregulation of p53 and MAPK pathways. Cancer Cell Int 16:56. https://doi.org/10.1186/s12935-016-0329-y
Lu Y-C, Chen C-N, Wang B et al (2011) Changes in tumor growth and metastatic capacities of J82 human bladder cancer cells suppressed by down-regulation of calreticulin expression. Am J Pathol 179:1425–1433. https://doi.org/10.1016/j.ajpath.2011.05.015
Ito H, Seyama Y, Kubota S (2001) Calreticulin is directly involved in anti-alpha3 integrin antibody-mediated secretion and activation of matrix metalloprotease-2. Biochem Biophys Res Commun 283:297–302. https://doi.org/10.1006/bbrc.2001.4833
Nangalia J, Massie CE, Baxter EJ et al (2013) Somatic CALR mutations in myeloproliferative neoplasms with nonmutated JAK2. N Engl J Med 369:2391–2405. https://doi.org/10.1056/NEJMoa1312542
Nomani L, Bodo J, Zhao X et al (2016) CAL2 immunohistochemical staining accurately identifies CALR mutations in myeloproliferative neoplasms. Am J Clin Pathol 146:431–438. https://doi.org/10.1093/ajcp/aqw135
Rosso V, Petiti J, Bracco E et al (2017) A novel assay to detect calreticulin mutations in myeloproliferative neoplasms. Oncotarget 8:6399–6405. https://doi.org/10.18632/oncotarget.14113
Shide K, Kameda T, Yamaji T et al (2017) Calreticulin mutant mice develop essential thrombocythemia that is ameliorated by the JAK inhibitor ruxolitinib. Leukemia 31:1136–1144. https://doi.org/10.1038/leu.2016.308
Araki M, Yang Y, Masubuchi N et al (2016) Activation of the thrombopoietin receptor by mutant calreticulin in CALR-mutant myeloproliferative neoplasms. Blood 127:1307–1316. https://doi.org/10.1182/blood-2015-09-671172
Sollazzo D, Forte D, Polverelli N et al (2016) Circulating calreticulin is increased in myelofibrosis: correlation with interleukin-6 plasma levels, bone marrow fibrosis, and splenomegaly. Mediators Inflamm 2016:1–7. https://doi.org/10.1155/2016/5860657
Daitoku S, Takenaka K, Yamauchi T et al (2016) Calreticulin mutation does not contribute to disease progression in essential thrombocythemia by inhibiting phagocytosis. Exp Hematol 44:817–825.e3. https://doi.org/10.1016/j.exphem.2016.05.001
Mondet J, Hussein K, Mossuz P (2015) Circulating cytokine levels as markers of inflammation in Philadelphia negative myeloproliferative neoplasms: diagnostic and prognostic interest. Mediators Inflamm 2015:1–10. https://doi.org/10.1155/2015/670580
Romano M, Sollazzo D, Trabanelli S et al (2017) Mutations in JAK2 and Calreticulin genes are associated with specific alterations of the immune system in myelofibrosis. Oncoimmunology 6:e1345402. https://doi.org/10.1080/2162402X.2017.1345402
Cristina Castañeda-Patlán M, Razo-Paredes R, Carrisoza-Gaytán R et al (2010) Protein kinase C is involved in the regulation of several calreticulin posttranslational modifications. Int J Biochem Cell Biol 42:120–131. https://doi.org/10.1016/j.biocel.2009.09.019
Ling S, Cline EN, Haug TS et al (2013) Citrullinated calreticulin potentiates rheumatoid arthritis shared epitope signaling. Arthritis Rheum 65:618–626. https://doi.org/10.1002/art.37814
Clarke A, Perry E, Kelly C et al (2017) Heightened autoantibody immune response to citrullinated calreticulin in bronchiectasis: implications for rheumatoid arthritis. Int J Biochem Cell Biol 89:199–206. https://doi.org/10.1016/j.biocel.2017.06.013
Decca MB, Carpio MA, Bosc C et al (2007) Post-translational arginylation of calreticulin: a new isospecies of calreticulin component of stress granules. J Biol Chem 282:8237–8245. https://doi.org/10.1074/jbc.M608559200
Goitea VE, Hallak ME (2015) Calreticulin and arginylated calreticulin have different susceptibilities to proteasomal degradation. J Biol Chem 290:16403–16414. https://doi.org/10.1074/jbc.M114.626127
López Sambrooks C, Carpio MA, Hallak ME (2012) Arginylated calreticulin at plasma membrane increases susceptibility of cells to apoptosis. J Biol Chem 287:22043–22054. https://doi.org/10.1074/jbc.M111.338335
Comba A, Bonnet LV, Goitea VE et al (2019) Arginylated calreticulin increases apoptotic response induced by bortezomib in glioma cells. Mol Neurobiol 56:1653–1664. https://doi.org/10.1007/s12035-018-1182-x
Arimoto K, Fukuda H, Imajoh-Ohmi S et al (2008) Formation of stress granules inhibits apoptosis by suppressing stress-responsive MAPK pathways. Nat Cell Biol 10:1324–1332. https://doi.org/10.1038/ncb1791
Protter DSW, Parker R (2016) Principles and properties of stress granules. Trends Cell Biol 26:668–679. https://doi.org/10.1016/j.tcb.2016.05.004
Llovet JM, Ricci S, Mazzaferro V et al (2008) Sorafenib in advanced hepatocellular carcinoma. N Engl J Med 359:378–390. https://doi.org/10.1056/NEJMoa0708857
Muller-Taubenberger A (2001) Calreticulin and calnexin in the endoplasmic reticulum are important for phagocytosis. EMBO J 20:6772–6782. https://doi.org/10.1093/emboj/20.23.6772
Vaithilingam A, Teixeira JE, Miller PJ et al (2012) Entamoeba histolytica cell surface calreticulin binds human C1q and functions in amebic phagocytosis of host cells. Infect Immun 80:2008–2018. https://doi.org/10.1128/IAI.06287-11
Acknowledgements
This study received funding from the Department of Microbiology and Parasitology of the Faculty of Medicine at the Universidad Nacional Autonóma de Mexico (UNAM).
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Schcolnik-Cabrera, A., Oldak, B., Juárez, M. et al. Calreticulin in phagocytosis and cancer: opposite roles in immune response outcomes. Apoptosis 24, 245–255 (2019). https://doi.org/10.1007/s10495-019-01532-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10495-019-01532-0