Abstract
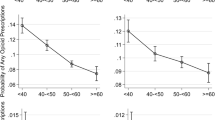
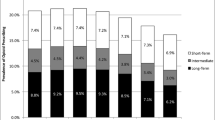
Longitudinal analyses of opioid use and overall disease severity among people with HIV (PWH) are lacking. We used joint-trajectory and Cox proportional hazard modeling to examine the relationship between self-reported opioid use and the Veterans Aging Cohort Study (VACS) Index 2.0, a validated measure of disease severity and mortality, among PWH engaged in care. Using data from 2002 and 2018, trajectory modeling classified 20% of 3658 PWH in low (i.e., lower risk of mortality), 40% in moderate, 28% in high, and 12% in extremely high VACS Index trajectories. Compared to those with moderate VACS Index trajectory, PWH with an extremely high trajectory were more likely to have high, then de-escalating opioid use (adjusted odds ratio [AOR], 95% confidence interval [CI] 5·17 [3·19–8·37]) versus stable, infrequent use. PWH who report high frequency opioid use have increased disease severity and mortality risk over time, even when frequency of opioid use de-escalates.


Similar content being viewed by others
Data Availability
A de-identified data set can be made available upon written request and approval by VACS leadership.
Code Availability
Please request information on code used by notifying corresponding author.
References
Degenhardt L, Grebely J, Stone J, Hickman M, Vickerman P, Marshall BDL, et al. Global patterns of opioid use and dependence: harms to populations, interventions, and future action. Lancet. 2019;394(10208):1560–79.
Control CfD, Prevention, Statistics NCfH. Compressed Mortality File 1999–2016 on CDC WONDER Online Database. 2017. Data are from the Compressed Mortality File. 1999;2016.
Stock Jonathan D, Chui P, Rosman L, Malm Brian J, Bastian L, Burg Matthew M. Abstract 12773: association of opioid use with atrial fibrillation in a post-9/11 veteran population. Circulation. 2018;138(Suppl_1):A12773-A.
Ronan MV, Herzig SJ. Hospitalizations related to opioid abuse/dependence and associated serious infections increased sharply, 2002–12. Health Aff. 2016;35(5):832–7.
Clausen T, Waal H, Thoresen M, Gossop M. Mortality among opiate users: opioid maintenance therapy, age and causes of death. Addiction. 2009;104(8):1356–62.
Gressler LE, Martin BC, Hudson TJ, Painter JT. Relationship between concomitant benzodiazepine-opioid use and adverse outcomes among US veterans. Pain. 2018;159(3):451–9.
Barry DT, Goulet JL, Kerns RK, Becker WC, Gordon AJ, Justice AC, et al. Nonmedical use of prescription opioids and pain in veterans with and without HIV. Pain. 2011;152(5):1133–8.
Roy S, Ninkovic J, Banerjee S, Charboneau RG, Das S, Dutta R, et al. Opioid drug abuse and modulation of immune function: consequences in the susceptibility to opportunistic infections. J Neuroimmune Pharmacol. 2011;6(4):442.
Edelman EJ, Gordon KS, Crothers K, Akgun K, Bryant KJ, Becker WC, et al. Association of prescribed opioids with increased risk of community-acquired pneumonia among patients with and without HIV. JAMA Intern Med. 2019;179(3):297–304.
McCance-Katz EF, Sullivan LE, Nallani S. Drug interactions of clinical importance among the opioids, methadone and buprenorphine, and other frequently prescribed medications: a review. Am J Addictions. 2010;19(1):4–16.
Lemons A, DeGroote N, Peréz A, Craw J, Nyaku M, Broz D, et al. Opioid misuse among HIV-positive adults in medical care: results from the medical monitoring project, 2009–2014. JAIDS J Acquir Immune Defic Syndr. 2019;80(2):127–34.
Edelman E, Gordon K, Tate J, Becker W, Bryant K, Crothers K, et al. The impact of prescribed opioids on CD4 cell count recovery among HIV-infected patients newly initiating antiretroviral therapy. HIV Med. 2016;17(10):728–39.
Tate JP, Justice AC, Hughes MD, Bonnet F, Reiss P, Mocroft A, et al. An internationally generalizable risk index for mortality after one year of antiretroviral therapy. AIDS. 2013;27(4):563–72.
Akgün KM, Gordon K, Pisani M, Fried T, McGinnis KA, Tate JP, et al. Risk factors for hospitalization and medical intensive care unit (MICU) admission among HIV-infected Veterans. J Acquir Immune Defic Syndr (1999). 2013;62(1):52–9.
Salinas JL, Rentsch C, Marconi VC, Tate J, Budoff M, Butt AA, et al. Baseline, time-updated, and cumulative HIV care metrics for predicting acute myocardial infarction and all-cause mortality. Clin Infect Dis. 2016;63(11):1423–30.
Marshall BDL, Tate JP, McGinnis KA, Bryant KJ, Cook RL, Edelman EJ, et al. Long-term alcohol use patterns and HIV disease severity. AIDS (London, England). 2017;31(9):1313–21.
McGinnis KA, Fiellin DA, Skanderson M, Hser YI, Lucas GM, Justice AC, et al. Opioid use trajectory groups and changes in a physical health biomarker among HIV-positive and uninfected patients receiving opioid agonist treatment. Drug Alcohol Depend. 2019;204:107511.
Justice AC, Dombrowski E, Conigliaro J, Fultz SL, Gibson D, Madenwald T, et al. Veterans aging cohort study (VACS): overview and description. Med Care. 2006;44(8 Suppl 2):S13.
Edelman EJ, Li Y, Barry D, Braden JB, Crystal S, Kerns RD, et al. Trajectories of self-reported opioid use among patients with HIV engaged in care: results from a national cohort study. JAIDS J Acquir Immune Defic Syndr. 2020;84:26.
Tate JP, Sterne JAC, Justice AC, Study ftVAC, Collaboration tATC. Albumin, white blood cell count, and body mass index improve discrimination of mortality in HIV-positive individuals. AIDS. 2019;33(5):903–12.
Sohn M-W, Arnold N, Maynard C, Hynes DM. Accuracy and completeness of mortality data in the Department of Veterans Affairs. Popul Health Metrics. 2006;4(1):2.
Gomes T, Greaves S, van den Brink W, Antoniou T, Mamdani MM, Paterson JM, et al. Pregabalin and the risk for opioid-related death: a nested case–control study. Ann Intern Med. 2018;169(10):732–4.
Jones BL, Nagin DS. Advances in group-based trajectory modeling and an SAS procedure for estimating them. Soc Methods Res. 2007;35(4):542–71.
Haviland AM, Jones BL, Nagin DS. Group-based trajectory modeling extended to account for nonrandom participant attrition. Soc Methods Res. 2011;40(2):367–90.
Freiberg MS, McGinnis KA, Kraemer K, Samet JH, Conigliaro J, CurtisEllison R, et al. The association between alcohol consumption and prevalent cardiovascular diseases among HIV-infected and HIV-uninfected men. J Acquir Immune Defic Syndr. 2010;53(2):247–53.
Lin LA, Bohnert ASB, Kerns RD, Clay MA, Ganoczy D, Ilgen MA. Impact of the opioid safety initiative on opioid-related prescribing in veterans. Pain. 2017;158(5):833–9.
Binswanger IA, Glanz JM, Faul M, Shoup JA, Quintana LM, Lyden J, et al. The association between opioid discontinuation and heroin use: a nested case-control study. Drug Alcohol Depend. 2020;217:108248.
Perez HR, Buonora M, Cunningham CO, Heo M, Starrels JL. Opioid taper is associated with subsequent termination of care: a retrospective cohort study. J Gen Intern Med. 2020;35(1):36–42.
Bruce RD, Merlin J, Lum PJ, Ahmed E, Alexander C, Corbett AH, et al. 2017 HIVMA of IDSA clinical practice guideline for the management of chronic pain in patients living with HIV. Clin Infect Dis. 2017;65(10):e1–37.
US Preventive Services Task Force. Draft recommendation statement: Illicit drug use, including nonmedical use of prescription drugs: screening. 2019.
Substance Abuse and Mental Health Services Administration. Medications for Opioid Use Disorder. Treatment Improvement Protocol (TIP) Series 63, Full Document. HHS Publication No. (SMA) 18–5063FULLDOC. Rockville, MD: Substance Abuse and Mental Health Services Administration; 2018.
Oldfield BJ, Munoz N, McGovern MP, Funaro M, Villanueva M, Tetrault JM, et al. Integration of care for HIV and opioid use disorder: a systematic review of interventions in clinical and community-based settings. AIDS. 2018;33:873.
Hernan MA. The hazards of hazard ratios. Epidemiology (Cambridge, Mass). 2010;21(1):13–5.
Bohnert ASB, Ilgen MA. Understanding links among opioid use, overdose, and suicide. N Engl J Med. 2019;380(1):71–9.
Elman I, Borsook D, Volkow ND. Pain and suicidality: insights from reward and addiction neuroscience. Prog Neurobiol. 2013;109:1–27.
Banerjee G, Edelman EJ, Barry DT, Becker WC, Cerdá M, Crystal S, et al. Non-medical use of prescription opioids is associated with heroin initiation among US veterans: a prospective cohort study. Addiction. 2016;111(11):2021–31.
Acknowledgements
We would like to acknowledge the veterans who participate in the Veterans Aging Cohort Study (VACS) and the study coordinators and staff at each VACS site and at the West Haven Coordinating Center. We would also like to thank Dr. Bobby Jones for his assistance with the joint-trajectory modeling procedures. The authors declare that they have no conflict of interest. This work was supported by supported by the National Institute on Drug Abuse (5R01DA040471-03), National Institute on Alcohol Abuse and Alcoholism (U10-AA13566), National Institute of Mental Health (F31-MH114736-01A1), and National Institute of Allergy and Infectious Diseases (T32-AI052074).
Funding
This work was supported by the National Institute on Drug Abuse (5R01DA040471-03, R25-DA037190), National Institute on Alcohol Abuse and Alcoholism (U10-AA13566), National Institute of Mental Health (F31-MH114736-01A1), and National Institute of Allergy and Infectious Diseases (T32-AI052074).
Author information
Authors and Affiliations
Contributions
JWA, YL, BDLM, and EJE conceptualized this specific analysis. YL performed the formal analysis. JWA and EJE wrote the resulting manuscript while YL, DTB, KSG, RDK, BO, CTR, and BDLM provided feedback and edits. All authors reviewed and approved submission.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
VACS received approval from the Institutional Review Boards at Yale University, VA Connecticut Healthcare System, and each participating site.
Informed Consent
All participants gave written informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
About this article
Cite this article
Adams, J.W., Li, Y., Barry, D.T. et al. Long-term Patterns of Self-reported Opioid Use, VACS Index, and Mortality Among People with HIV Engaged in Care. AIDS Behav 25, 2951–2962 (2021). https://doi.org/10.1007/s10461-021-03162-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-021-03162-7