Abstract
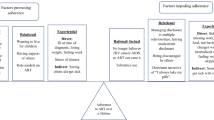
Realization of optimal treatment and prevention benefits in the era of universal antiretroviral therapy (ART) and “U=U” (undetectable = untransmittable) requires high adherence at all stages of HIV disease. This article draws upon qualitative interview data to characterize two types of influences on ART adherence for 100 Ugandans and South Africans initiating ART during early-stage HIV infection. Positive influences are: (a) behavioral strategies supporting adherence; (b) preserving health through adherence; (c) support from others; and (d) motivating effect of adherence monitoring. “De-stabilizing experiences” (mobility, loss, pregnancy) as barriers are posited to impact adherence indirectly through intervening consequences (e.g. exacerbation of poverty). Positive influences overlap substantially with adherence facilitators described for later-stage adherers in previous research. Adherence support strategies and interventions effective for persons initiating ART later in HIV disease are likely also to be helpful to individuals beginning treatment immediately upon confirmation of infection. De-stabilizing experiences merit additional investigation across varying populations.


Similar content being viewed by others
References
Cohen MS, Chen YQ, McCauley M, et al. Prevention of HIV-1 infection with early antiretroviral therapy. N Engl J Med. 2011;365(6):493–505.
Rodger AJ, Cambiano V, Bruun T, et al. Sexual activity without condoms and risk of HIV transmission in serodifferent couples when the HIV-positive partner is using suppressive antiretroviral therapy. JAMA. 2016;316(2):171–81.
Quinn TC, Wawer MJ, Sewankambo N, et al. Viral load and heterosexual transmission of human immunodeficiency virus type 1. N Engl J Med. 2000;342:921–9.
McCray E, Mermin J. HIV/AIDS in the United States: Letter from the CDC. 2017. https://docs.wixstatic.com/ugd/de0404_1f9f737da1674cdda5a42f7857cd4fa6.pdf. Accessed 12 March 2019.
Editorial. U=U Taking Off in 2017. Lancet HIV. 2017;4:e475.
World Health Organization. Consolidated guidelines on the use of antiretroviral drugs for treating and preventing HIV infection: recommendations for a public health approach. World Health Organization;2016.
UNAIDS. Miles to go: closing gaps, breaking barriers, righting injustices. 2018. https://www.unaids.org/en/20180718_GR2018. Accessed 15 Dec 2019.
Yebra G, Ragonnet-Cronin M, Ssemwanga D, et al. Analysis of the history and spread of HIV-1 in Uganda using phylodynamics. J Gen Virol. 2015;98(Pt 7):1890–8.
No author. Uganda tackles AIDS from the very top down. AIDS Alert.1999;14(8 Suppl):3–4.
Genuis SJ, Genuis SK. HIV/AIDS prevention in Uganda: why has it worked? BMJ. 2005;81(960):615–7.
Slutkin G, Okware S, Naamara W, et al. How Uganda reversed its HIV epidemic. AIDS Behav. 2006;10:351–61.
UNAIDS Country Fact Sheets Uganda. 2018. https://www.unaids.org/en/regionscountries/countries/uganda. Accessed 15 Dec 2019.
Mills EJ, Nachega JB, Buchan I, et al. Adherence to antiretroviral therapy in sub-Saharan Africa and North America: a meta-analysis. JAMA. 2006;296:679–90.
Oyugi JH, Byakika-Tusiime J, Charlebois ED, et al. Multiple validated measures of adherence indicate high levels of adherence to generic HIV antiretroviral therapy in a resource-limited setting. J Acquir Immune Defic Syndr. 2004;36(5):1100–2.
Oyugi JH, Byakika-Tusiime J, Ragland K, et al. Treatment interruptions predict resistance in HIV-positive individuals purchasing fixed-dose combination antiretroviral therapy in Kampala. Uganda. AIDS. 2007;21(8):965–71.
Bock P, James A, Nikuze A, et al. Baseline CD4 count and adherence to antiretroviral therapy: a systematic review and meta-analysis. J Acquir Immune Defic Syndr. 2016;73(5):514–21.
Haberer JE, Bwana B, Orrell C, et al. ART adherence and viral suppression are high among most non-pregnant individuals with early-stage, asymptomatic HIV infection: an observational cohort study from Uganda and South Africa. J Int AIDS Soc. 2019;22:e25232.
Hsieh HS, Shannon SE. Three approaches to qualitative content analysis. Qual Health Res. 2005;15:1277.
Croome N, Ahluwalia M, Hughes LD, Abas M. Patient-reported barriers and facilitators to antiretroviral adherence in sub-Saharan Africa. AIDS. 2017;31(7):995–1007.
Watt MH, Maman S, Earp JA, et al. "It's all the time in my mind": facilitators of adherence to antiretroviral therapy in a Tanzanian setting. Soc Sci Med. 2009;68(10):1793–800.
Martin F, Kiwanuka T, Kawuma R, et al. Tasks and strategies of self-management of living with antiretroviral therapy in Uganda. AIDS Patient Care STDs. 2013;27(12):697–706.
Bezabhe WM, Chalmers L, Bereznicki LR, et al. Barriers and facilitators of adherence to antiretroviral drug therapy and retention in care among adult HIV-positive patients: a qualitative study from Ethiopia. PLoS ONE. 2014;9(5):e97353.
Ryan GW, Wagner GJ. Pill taking ‘routinization’: a critical factor to understanding episodic medication adherence. AIDS Care. 2003;15:795–806.
Roberts KJ. Barriers to and facilitators of HIV-positive patients' adherence to antiretroviral treatment regimens. AIDS Patient Care STDS. 2000;14:155–68.
Adam BD, Maticka-Tyndale E, Cohen JJ. Adherence practices among people living with HIV. AIDS Care. 2003;15:263–74.
Sanjobo N, Frich JC, Fretheim A. Barriers and facilitators to patients' adherence to antiretroviral treatment in Zambia: a qualitative study. SAHARA J. 2008;5(3):136–43.
Lyimo RA, de Bruin M, van den Boogaard J, et al. Determinants of antiretroviral therapy adherence in northern Tanzania: a comprehensive picture from the patient perspective. BMC Public Health. 2012;12:716.
Ware NC, Pisarski EE, Tam M, et al. The meanings in the messages: how SMS reminders and real-time adherence monitoring improve antiretroviral therapy adherence in rural Uganda. AIDS. 2016;30(8):1287–94.
Lambert RF, Orrell C, Bangsberg DR, Haberer JE. Factors that motivated otherwise healthy HIV-positive young adults to access HIV testing and treatment in South Africa. AIDS Behav. 2018;22(3):733–41.
Horter S, Wringe A, Thabede Z, et al. “Is it making any difference?” A qualitative study examining the treatment-taking experiences of asymptomatic people living with HIV in the context of Treat-all in Eswatini. J Int AIDS Soc. 2019;22:e25220.
Adams AK, Zamberia AM. “I will take ARVs once my body deteriorates”: an analysis of Swazi men’s perceptions and acceptability of Test and Start. Afr J AIDS Res. 2017;16(4):295–303.
Hodgson I, Plummer ML, Konopka SN, et al. A systematic review of individual and contextual factors affecting ART initiation, adherence, and retention for HIV-infected pregnant and postpartum women. PLoS ONE. 2014;9(11):e111421.
Colvin CJ, Konopka S, Chalker JC, et al. A systematic review of health system barriers and enablers for antiretroviral therapy (ART) for HIV infected pregnant and postpartum women. PLoS ONE. 2014;9(10):e108150.
Nachega JB, Uthman OA, Anderson J, et al. Adherence to antiretroviral therapy during and after pregnancy in low-income, middle-income, and high-income countries: a systematic review and meta-analysis. AIDS. 2012;26(16):2039–52.
Acknowledgements
The authors gratefully acknowledge the contributions of qualitative participants, and the research assistants who collected the qualitative data: Catherine Kyampire, Regina Panda, and Khosi Tshangela. We thank the META Study team: Principal Investigators: Dr. Jessica E. Haberer, Dr. Catherine Orrell, Dr. Norma C. Ware, Dr. Mwebesa Bosco Bwana, Dr. Stephen Asiimwe, Dr. Gideon Amanyire, Hon. Dr. Elioda Tumwesigye, Dr. David R. Bangsberg. Co-Investigators: Dr. Alex Tsai, Dr. Mark Siedner, Dr. Lynn Matthews, Dr. Ingrid Katz, Monique Wyatt. Program Managers: Annet Kembabazi, Stephen Mugisha, Victoria Nanfuka, Anna Cross, Nicky Kelly, Daphne Moralie, Kate Bell. Statistician: Nicholas Musinguzi. Data Managers: Dolphina Cogill, Justus Ashaba, Zoleka Xapa, Mathias Orimwesiga, Elly Tuhanamagyezi, Catherine Kyampaire. Lab Managers: Don Bosco Mpanga, Leonia Kyarisima, Simone Kigozi. Research Assistants: Nomakhaya April (RN), Alienah Mpahleni, Vivie Situlo, Speech Mzamo, Nomsa Ngwenya, Khosi Tshangela, Regina Panda, Teboho Linda, Christine Atwiine, Sheila Moonlight, Edna Tindimwebwa, Nicholas Mugisha, Peace Atwogeire, Dr. Vian Namana, Catherine Kyampaire, Gabriel Nuwagaba. Drivers: Edgar October, Silver Mugisha, Ibrahim Kiviiri.
Funding
This study was funded by the Bill and Melinda Gates Foundation (OPP1056051).
Author information
Authors and Affiliations
Consortia
Contributions
NCW and MAW designed the qualitative study. MAW and EEP oversaw collection of the qualitative data. NCW and EEP analyzed the qualitative data. NM contributed quantitative data on personal characteristics of participants in the qualitative study, compared to META study participants. NCW wrote the first draft and subsequent revisions of the manuscript, with input from MAW, EEP, and JEH. All authors critically reviewed and approved the final version.
Corresponding author
Ethics declarations
Research Involving Human and Animal Participants
All procedures performed in studies involving human participants were in accordance with the ethical standards of: (1) Partners Healthcare/Massachusetts General Hospital, Boston, MA, USA; (2) Harvard Medical School, Boston, MA, USA; (3) Mbarara University of Science and Technology, Mbarara, Uganda; (4) the Uganda National Council for Science and Technology, Kampala, Uganda; (5) University of Cape Town, Cape Town, South Africa; and (5) Western Cape province, South Africa, and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ware, N.C., Wyatt, M.A., Pisarski, E.E. et al. Influences on Adherence to Antiretroviral Therapy (ART) in Early-Stage HIV Disease: Qualitative Study from Uganda and South Africa. AIDS Behav 24, 2624–2636 (2020). https://doi.org/10.1007/s10461-020-02819-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-020-02819-z