Abstract
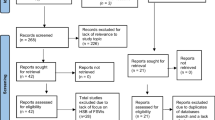
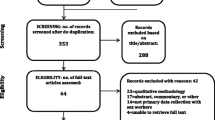
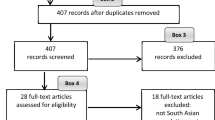
Access to safe and effective sexual healthcare services for transgender and male sex workers (TMSW) is a human right. Globally, TMSW experience a higher prevalence of human immunodeficiency virus (HIV) and sexually transmitted infections than the general population or other sex workers, suggesting the existence of unique challenges for this group when accessing healthcare. A systematic database search identified 22 qualitative papers addressing barriers to accessing sexual healthcare services for TMSW. These papers were critically evaluated for adherence to best practice standards for qualitative research and research with sex workers. A coding process identified five themes. Stigma was the predominant barrier, and was divided into stigma related to sexuality, gender identity, HIV status, sex worker status, and internalised stigma. Other barriers were confidentiality concerns, sexual health literacy, fatalism, and structural barriers. Each of these themes were informed by the wider context of stigma. The literature presents a complex syndemic of social disadvantage and exclusion acting to produce and reinforce health disparities related to sexual health and access to screening and treatment for TMSW.

Similar content being viewed by others
References
Kerrigan D, Kennedy CE, Morgan-Thomas R, Reza-Paul S, Mwangi P, Win KT, et al. A community empowerment approach to the HIV response among sex workers: effectiveness, challenges, and considerations for implementation and scale-up. Lancet. 2015;385(9963):172–85.
Decker MR, Crago A, Chu SKH, Sherman SG, Seshu MS, Buthelezi K, et al. Human rights violations against sex workers: burden and effect on HIV. Lancet. 2015;385(9963):186–99.
Clements-Nolle K, Marx R, Guzman R, Katz M. HIV prevalence, risk behaviours, healthcare use, and mental health status of transgender persons: implications for public health intervention. Am J Public Health. 2001;91:915–21.
Operario D, Soma T, Underhill K. Sex work and HIV status among transgender women: systematic review and meta-analysis. J Acquir Immune Defic Syndr. 2008;48(1):97–103.
Tang W, Mahapatra T, Liu F, Fu G, Yang B, Tucker JD, et al. Burden of HIV and syphilis: a comparative evaluation between male sex workers and non-sex-worker men who have sex with men in urban China. PLoS ONE. 2015;10(5):e0126604.
UNAIDS. Global report 2012: UNAIDS report of the global AIDS epidemic. Joint United Nations Programme on HIV/AIDS. UNAIDS; 2012.
Poteat T, Wirtz AL, Radix A, Borquez A, Silva-Santisteban A, Deutsch MB, et al. HIV risk and preventive interventions in transgender women sex workers. Lancet. 2015;385(9964):274–86.
Myers T, Allman D, Xu K, Remis RS, Aguinaldo J, Burchell A, et al. The prevalence and correlates of hepatitis C virus (HCV) infection and HCV-HIV co-infection in a community sample of gay and bisexual men. Int J Infect Dis. 2009;13(6):730–9.
Nguyen TA, Nguyen HT, Le GT, Detels R. Prevalence and risk factors associated with HIV infection among men having sex with men in Ho Chi Minh City, Vietnam. AIDS Behav. 2008;12(3):476–82.
Oldenburg CE, Perez-Brumer AG, Reisner SL, Mimiaga MJ. Transactional sex and the HIV epidemic among men who have sex with men (MSM): results from a systematic review and meta-analysis. AIDS Behav. 2015;19(12):2177–83.
Baral SD, Friedman MR, Geibel S, Rebe K, Bozhinov B, Diouf D, et al. Male sex workers: practices, contexts, and vulnerabilities for HIV acquisition and transmission. Lancet (Lond Engl). 2015;385(9964):260–73.
Sperber J, Landers S, Lawrence S. Access to health care for transgendered persons: results of a needs assessment in Boston. Int J Transgend. 2005;8(2–3):75–91.
Singh GK, Azuine RE, Siahpush M. Widening socioeconomic, racial, and geographic disparities in HIV/AIDS mortality in the United States, 1987–2011. Adv Prev Med. 2013;2013:657961.
Newman PA, Philbin MM, Hirsch JS, Wilson PA, Ly AT, Giang LM, et al. Structural barriers to HIV prevention among men who have sex with men (MSM) in Vietnam: diversity, stigma, and healthcare access. PLoS ONE. 2018. https://doi.org/10.1371/journal.pone.0195000.
White Hughto JM, Reisner SL, Pachankis JE. Transgender stigma and health: a critical review of stigma determinants, mechanisms, and interventions. Soc Sci Med. 2015;147:222–31.
Beattie TSH, Bhattacharjee P, Suresh M, Isac S, Ramesh BM, Moses S. Personal, interpersonal and structural challenges to accessing HIV testing, treatment and care services among female sex workers, men who have sex with men and transgenders in Karnataka State, South India. J Epidemiol Community Health. 2012;66(Suppl 2):42–8.
Chakrapani V, Newman PA, Shunmugam M, McLuckie A, Melwin F. Structural violence against Kothi-identified men who have sex with men in Chennai, India: a qualitative investigation. AIDS Educ Prev. 2007;19(4):346–64.
Earnshaw VA, Bogart LM, Dovidio JF, Williams DR. Stigma and racial/ethnic HIV disparities: moving toward resilience. Am Psychol. 2013;68(4):225–36.
Arnold EA, Rebchook GM, Kegeles SM. ‘Triply cursed’: racism, homophobia and HIV-related stigma are barriers to regular HIV testing, treatment adherence and disclosure among young Black gay men. Cult Health Sex. 2014;16(6):710–22.
Lazarus L, Deering KN, Nabess R, Gibson K, Tyndall MW, Shannon K. Occupational stigma as a primary barrier to health care for street-based sex workers in Canada. Cult Health Sex. 2012;14(2):139–50.
Logie CH, James L, Tharao W, Loutfy MR. HIV, gender, race, sexual orientation, and sex work: a qualitative study of intersectional stigma experienced by HIV-positive women in Ontario, Canada. PLoS Med. 2011;8(11):e1001124.
Ngo AD, Ratliff EA, McCurdy SA, Ross MW, Markham C, Pham HT. Health-seeking behaviour for sexually transmitted infections and HIV testing among female sex workers in Vietnam. AIDS Care. 2007;19(7):878–87.
Levesque J, Harris MF, Russell G. Patient-centred access to health care: conceptualising access at the interface of health systems and populations. Int J Equity Health. 2013;12(18):18.
Harcourt C, Donovan B. The many faces of sex work. Sex Transm Infect. 2005;81(3):201–6.
Jobson GA, Theron LB, Kaggwa JK, Kim HJ. Transgender in Africa: invisible, inaccessible, or ignored? SAHARA-J J Soc Asp HIV/AIDS. 2012;9(3):160–3.
Bungay V, Oliffe J, Atchison C. Addressing underrepresentation in sex work research: reflections on designing a purposeful sampling strategy. Qual Health Res. 2016;26(7):966–78.
Bonevski B, Randell M, Paul C, Chapman K, Twyman L, Bryant J, et al. Reaching the hard-to-reach: a systematic review of strategies for improving health and medical research with socially disadvantaged groups. BMC Med Res Methodol. 2014;14(1):42.
Dudwick N, Kuehnast K, Jones VN, Woolcock M. Analyzing social capital in context: a guide to using qualitative methods and data. Washington, DC: World Bank Institute; 2006.
Choy LT. The strengths and weaknesses of research methodology: comparison and complimentary between qualitative and quantitative approaches. IOSR J Humanit Soc Sci. 2014;19(4):99–104.
Chakrapani V, Newman PA, Shunmugam M, Dubrow R. Barriers to free antiretroviral treatment access among Kothi-identified men who have sex with men and Aravanis (transgender women) in Chennai, India. AIDS Care. 2011;23(12):1687–94.
Samudzi Z, Mannell J. Cisgender male and transgender female sex workers in South Africa: gender variant identities and narratives of exclusion. Cult Health Sex. 2016;18(1):1–14.
Aunon FM, Wagner GJ, Maher R, Khouri D, Kaplan RL, Mokhbat J. An exploratory study of HIV risk behaviors and testing among male sex workers in Beirut, Lebanon. Soc Work Public Health. 2015;30(4):373–84.
Barmania S, Aljunid SM. Navigating HIV prevention policy and Islam in Malaysia: contention, compatibility or reconciliation? Findings from in-depth interviews among key stakeholders. BMC Public Health. 2016;16:524.
Ganju D, Saggurti N. Stigma, violence and HIV vulnerability among transgender persons in sex work in Maharashtra, India. Cult Health Sex. 2017;19(8):903–17.
Sevelius JM, Keatley J, Calma N, Arnold E. ‘I am not a man’: trans-specific barriers and facilitators to PrEP acceptability among transgender women. Glob Public Health. 2016;11(7–8):1060–75.
Shaver FM. Sex work research: methodological and ethical challenges. J Interpers Violence. 2005;20(3):296–319.
Beyrer C, Crago A, Bekker L, Butler J, Shannon K, Kerrigan D, et al. An action agenda for HIV and sex workers. Lancet. 2015;385(9964):287–301.
Abel G, Fitzgerald L, Brunton C. Christchurch School of Medicine study: methodology and methods. In: Abel G, Fitzgerald L, Healy C, Taylor A, editors. Taking the crime out of sex work: New Zealand sex workers’ fight for decriminalisation. Bristol: The Policy Press; 2010. p. 159–62.
Graça M, Gonçalves M, Martins A. Participatory action research with sex workers and an outreach team: a co-authored case study. Action Res. 2017. https://doi.org/10.13140/RG.2.1.3688.4080..
Singh AA, Richmond K, Burnes TR. Feminist participatory action research with transgender communities: fostering the practice of ethical and empowering research designs. Int J Transgend. 2013;14(3):93–104.
Jeffreys E. Sex worker-driven research: best practice ethics. Dialogue e-J. 2010;8.
Baum F, MacDougall C, Smith D. Participatory action research. J Epidemiol Community Health. 2006;60(10):854–7.
van der Meulen E. Action research with sex workers: dismantling barriers and building bridges. Action Res. 2011;9(4):370–84.
Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7).
National Institute for Health and Care Excellence. Methods for the development of NICE public health guidance. London: National Institute for Health and Clinical Excellence; 2012.
Noyes J, Hannes K, Booth A, Harris J, Harden A, Popay J, et al. Qualitative research and Cochrane review. 2008. In: Cochrane handbook for systematic review of interventions (Internet). Cochrane Qualitative and Implementation Methods Group; p. 571.
Lui CW, Dean J, Mutch A, Mao L, Debattista J, Lemoire J, et al. HIV testing in men who have sex with men: a follow-up review of the qualitative literature since 2010. AIDS Behav. 2017. https://doi.org/10.1007/s10461-017-1752-3.
Lorenc T, Marrero-Guillamon I, Llewellyn A, Aggleton P, Cooper C, Lehmann A, et al. HIV testing among men who have sex with men (MSM): systematic review of qualitative evidence. Health Educ Res. 2011;26(5):834–46.
Toye F, Seers K, Allcock N, Briggs M, Carr E, Barker K. Meta-ethnography 25 years on: challenges and insights for synthesising a large number of qualitative studies. BMC Med Res Methodol. 2014;14:80.
Restar AJ, Tocco JU, Mantell JE, Lafort Y, Gichangi P, Masvawure TB, et al. Perspectives on HIV pre- and post-exposure prophylaxes (PrEP and PEP) among female and male sex workers in Mombasa, Kenya: implications for integrating biomedical prevention into sexual health services. AIDS Educ Prev. 2017;29(2):141–53.
Scorgie F, Nakato D, Harper E, Richter M, Maseko S, Nare P, et al. ‘We are despised in the hospitals’: sex workers’ experiences of accessing health care in four African countries. Cult Health Sex. 2013;15(4):450–65.
Sandelowski M, Barroso J, Voils CI. Using qualitative metasummary to synthesize qualitative and quantitative descriptive findings. Res Nurs Health. 2007;30(1):99–111.
Underhill K, Morrow KM, Colleran CM, Holcomb R, Operario D, Calabrese SK, et al. Access to healthcare, HIV/STI testing, and preferred pre-exposure prophylaxis providers among men who have sex with men and men who engage in street-based sex work in the US. PLoS ONE. 2014;9(11):e112425.
Underhill K, Morrow KM, Colleran C, Holcomb R, Calabrese SK, Operario D, et al. A qualitative study of medical mistrust, perceived discrimination, and risk behavior disclosure to clinicians by U.S. male sex workers and other men who have sex with men: implications for biomedical HIV prevention. J Urban Health. 2015;92(4):667–86.
Boyce S, Barrington C, Bolanos H, Arandi CG, Paz-Bailey G. Facilitating access to sexual health services for men who have sex with men and male-to-female transgender persons in Guatemala City. Cult Health Sex. 2012;14(3):313–27.
Okanlawon K, Adebowale AS, Titilayo A. Sexual hazards, life experiences and social circumstances among male sex workers in Nigeria. Cult Health Sex. 2013;15(Suppl 1):S22–33.
Reza-Paul S, Lorway R, O’Brien N, Lazarus L, Jain J, Bhagya M, et al. Sex worker-led structural interventions in India: a case study on addressing violence in HIV prevention through the Ashodaya Samithi Collective in Mysore. Indian J Med Res. 2012;135(1):98–106.
Xavier J, Bradford J, Hendricks M, Safford L, McKee R, Martin E, et al. Transgender health care access in Virginia: a qualitative study. Int J Transgend. 2013;14(1):3–17.
Giguere R, Frasca T, Dolezal C, Febo I, Cranston RD, Mayer K, et al. Acceptability of three novel HIV prevention methods among young male and transgender female sex workers in Puerto Rico. AIDS Behav. 2016;20(10):2192–202.
Jones JL, Rasch RFR, MacMaster S, Adams SM, Cooper RL. The experiences of African American male commercial sex workers at-risk for HIV: accessing outreach services. J Gay Lesbian Soc Serv. 2009;21(2–3):282–93.
Okal J, Luchters S, Geibel S, Chersich MF, Lango D, Temmerman M. Social context, sexual risk perceptions and stigma: HIV vulnerability among male sex workers in Mombasa, Kenya. Cult Health Sex. 2009;11(8):811–26.
Mimiaga MJ, Reisner SL, Closson EF, Perry N, Perkovich B, Nguyen T, et al. Self-perceived HIV risk and the use of risk reduction strategies among men who engage in transactional sex with other men in Ho Chi Minh City, Vietnam. AIDS Care. 2013;25(8):1039–44.
Reisner SL, Mimiaga MJ, Mayer KH, Tinsley JP, Safren SA. Tricks of the trade: sexual health behaviors, the context of HIV risk, and potential prevention intervention strategies for male sex workers. J LGBT Health Res. 2008;4(4):195–209.
Castaneda H. Structural vulnerability and access to medical care among migrant street-based male sex workers in Germany. Soc Sci Med. 2013;84:94–101.
Infante C, Sosa-Rubi SG, Cuadra SM. Sex work in Mexico: vulnerability of male, travesti, transgender and transsexual sex workers. Cult Health Sex. 2009;11(2):125–37.
Collumbien M, Qureshi AA, Mayhew SH, Rizvi N, Rabbani A, Rolfe B, et al. Understanding the context of male and transgender sex work using peer ethnography. Sex Transm Infect. 2009;85(Suppl 2):ii3–7.
Morrell R, Jewkes R, Lindegger G. Hegemonic masculinity/masculinities in South Africa. Men Masc. 2012;15(1):11–30.
Livingston JD, Boyd JE. Correlates and consequences of internalized stigma for people living with mental illness: a systematic review and meta-analysis. Soc Sci Med. 2010;71(12):2150–61.
Meyer-Weitz A. Understanding fatalism in HIV/AIDS protection: the individual in dialogue with contextual factors. Afr J AIDS Res. 2005;4(2):75–82.
Ma PHX, Chan ZCY, Loke AY. The socio-ecological model approach to understanding barriers and facilitators to the accessing of health services by sex workers: a systematic review. AIDS Behav. 2017;21(8):2412–38.
Stahlman S, Grosso A, Ketende S, Sweitzer S, Mothopeng T, Taruberekera N, et al. Depression and social stigma among MSM in Lesotho: implications for HIV and sexually transmitted infection prevention. AIDS Behav. 2015;19(8):1460–9.
Goffman E. Stigma: notes on the management of a spoiled identity. New York: Simon and Schuster; 1963.
Lacombe-Duncan A. An intersectional perspective on access to HIV-related healthcare for transgender women. Transgend Health. 2016;1(1):137–41.
Singer M, Bulled N, Ostrach B, Mendenhall E. Syndemics and the biosocial conception of health. Lancet. 2017;389(10072):941–50.
Biello KB, Colby D, Closson E, Mimiaga MJ. The syndemic condition of psychosocial problems and HIV risk among male sex workers in Ho Chi Minh City, Vietnam. AIDS Behav. 2014;18(7):1264–71.
Brennan J, Kuhns LM, Johnson AK, Belzer M, Wilson EC, Garofalo R. Syndemic theory and HIV-related risk among young transgender women: the role of multiple, co-occurring health problems and social marginalization. Am J Public Health. 2012;102(9):1751–7.
Dijkstra M, van der Elst EM, Micheni M, Gichuru E, Musyoki H, Duby Z, et al. Emerging themes for sensitivity training modules of African healthcare workers attending to men who have sex with men: a systematic review. Int Health. 2015;7(3):151–62.
van der Elst EM, Smith AD, Gichuru E, Wahome E, Musyoki H, Muraguri N, et al. Men who have sex with men sensitivity training reduces homoprejudice and increases knowledge among Kenyan healthcare providers in coastal Kenya. J Int AIDS Soc. 2013;16(Suppl 3):18748.
Reisner SL, Bradford J, Hopwood R, Gonzalez A, Makadon H, Todisco D, et al. Comprehensive transgender healthcare: the gender affirming clinical and public health model of Fenway Health. J Urban Health. 2015;92(3):584–92.
WHO. Guidelines: prevention and treatment of HIV and other sexually transmitted infections among men who have sex with men and transgender people: recommendations for a public health approach. Geneva: World Health Organisation; 2011.
Chillag K, Guest G, Bunce A, Johnson L, Kilmarx PH, Smith DK. Talking about sex in Botswana: social desirability bias and possible implications for HIV-prevention research. Afr J AIDS Res. 2006;5(2):123–31.
Kelly CA, Soler-Hampejsek E, Mensch BS, Hewett PC. Social desirability bias in sexual behavior reporting: evidence from an interview mode experiment in rural Malawi. Int Perspect Sex Reprod Health. 2013;39(1):14–21.
Perez-Brumer AG, Oldenburg CE, Reisner SL, Clark JL, Parker RG. Towards ‘reflexive epidemiology’: conflation of cisgender male and transgender women sex workers and implications for global understandings of HIV prevalence. Glob Public Health. 2016;11(7–8):849–65.
Dunkle KL, Wong FY, Nehl EJ, Lin L, He N, Huang J, et al. Male-on-male intimate partner violence and sexual risk behaviors among money boys and other men who have sex with men in Shanghai, China. Sex Transm Dis. 2013;40(5):362–5.
Shannon K, Crago A-L, Baral SD, Bekker L-G, Kerrigan D, Decker MR, et al. The global response and unmet actions for HIV and sex workers. Lancet. 2018;392(10148):698–710.
Funding
All funding for this review was provided by the HIV Foundation, Queensland.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
This research received ethical approval under the University of Queensland Human Research Ethics Committee (Approval Number #2016001287).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Brookfield, S., Dean, J., Forrest, C. et al. Barriers to Accessing Sexual Health Services for Transgender and Male Sex Workers: A Systematic Qualitative Meta-summary. AIDS Behav 24, 682–696 (2020). https://doi.org/10.1007/s10461-019-02453-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-019-02453-4