Abstract
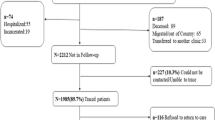
Poor retention in care is associated with higher viral load (VL) results and decreased rates of viral load suppression (VS) in people living with HIV (PLWH). Therefore, improving retention in HIV care is a priority of national significance. The NC-LINK Retention Project utilized a systematic approach to identify, locate, and attempt to return to care patients who did not attend a clinic appointment for 6–9 months. Clinical and surveillance data were used to evaluate associations between patient characteristics and VL outcomes. Between January 1, 2013 and December 31, 2014, 1118 patients at participating clinics were identified as out-of-care and referred to retention staff. Of these, 712 (64%) were located in North Carolina. Patients with recent prior medical care (aPR 1.43, 95% CI 1.25, 1.66) and recent VS (aPR 1.28, 95% CI 1.16, 1.41) were more likely to be located. Of located patients, 58% re-engaged in care within 90 days of retention referral. Patients who achieved VS within 180 days were more likely to be 40–49 years (aPR 1.19 95% CI 1.01–1.40; compared with 18–29 age group), had insurance at their last visit (aPR 1.19 95% CI 1.01–1.77), had a care visit in the prior year (aPR 1.37 95% CI 1.05–1.77), and had VS at the prior care visit (aPR 2.54 95% CI 1.98–3.25). Clinic-based retention efforts may be effective at helping PLWH decrease out-of-care periods, but prior patterns of care usage persist.


Similar content being viewed by others
References
Dombrowski JC, Kitahata MM, Van Rompaey SE, Crane HM, Mugavero MJ, Eron JJ, et al. High levels of antiretroviral use and viral suppression among persons in HIV care in the United States, 2010. J Acquir Immune Defic Syndr. 2013;63(3):299–306.
Giordano TP. Retention in HIV care: what the clinician needs to know. Top Antivir Med. 2011;19(1):12–6.
Cohen MS, Chen YQ, McCauley M, Gamble T, Hosseinipour MC, Kumarasamy N, et al. Prevention of HIV-1 infection with early antiretroviral therapy. N Engl J Med. 2011;365(6):493–505.
Tripathi A, Youmans E, Gibson JJ, Duffus WA. The impact of retention in early HIV medical care on viro-immunological parameters and survival: a statewide study. AIDS Res Hum Retroviruses. 2011;27(7):751–8.
Mugavero MJ, Westfall AO, Zinski A, Davila J, Drainoni ML, Gardner LI, et al. Measuring retention in HIV care: the elusive gold standard. J Acquir Immune Defic Syndr. 2012;61(5):574–80.
Mugavero MJ, Lin HY, Willig JH, Westfall AO, Ulett KB, Routman JS, et al. Missed visits and mortality among patients establishing initial outpatient HIV treatment. Clin Infect Dis. 2009;48(2):248–56.
Giordano TP, Gifford AL, White AC Jr, Suarez-Almazor ME, Rabeneck L, Hartman C, et al. Retention in care: a challenge to survival with HIV infection. Clin Infect Dis. 2007;44(11):1493–9.
Park WB, Choe PG, Kim SH, Jo JH, Bang JH, Kim HB, et al. One-year adherence to clinic visits after highly active antiretroviral therapy: a predictor of clinical progress in HIV patients. J Intern Med. 2007;261(3):268–75.
Shah M, Risher K, Berry SA, Dowdy DW. The epidemiologic and economic impact of improving HIV testing, linkage, and retention in care in the United States. Clin Infect Dis. 2016;62(2):220–9.
Stricker SM, Fox KA, Baggaley R, Negussie E, de Pee S, Grede N, et al. Retention in care and adherence to ART are critical elements of HIV care interventions. AIDS Behav. 2014;18(Suppl 5):S465–75.
Reif SS, Whetten K, Wilson ER, McAllaster C, Pence BW, Legrand S, et al. HIV/AIDS in the Southern USA: a disproportionate epidemic. AIDS Care. 2014;26(3):351–9.
Hanna DB, Selik RM, Tang T, Gange SJ. Disparities among US states in HIV-related mortality in persons with HIV infection, 2001–2007. AIDS. 2012;26(1):95–103.
Reif S, Pence BW, Hall I, Hu X, Whetten K, Wilson E. HIV diagnoses, prevalence and outcomes in nine Southern States. J Community Health. 2015;40(4):642–51.
HIV Care Outcomes in North Carolina, 2016. North Carolina HIV/STD/Hepatitis Surveillance Unit Communicable Disease Branch. 2017. http://epi.publichealth.nc.gov/cd/stds/figures/factsheet_HIV_care_outcomes_2016_rev3.pdf. Accessed 22 Nov 2017.
Adimora AA, Ramirez C, Schoenbach VJ, Cohen MS. Policies and politics that promote HIV infection in the Southern United States. AIDS. 2014;28(10):1393–7.
Kempf MC, McLeod J, Boehme AK, Walcott MW, Wright L, Seal P, et al. A qualitative study of the barriers and facilitators to retention-in-care among HIV-positive women in the rural southeastern United States: implications for targeted interventions. AIDS Patient Care STDS. 2010;24(8):515–20.
Toth M, Messer LC, Quinlivan EB. Barriers to HIV care for women of color living in the Southeastern US are associated with physical symptoms, social environment, and self-determination. AIDS Patient Care STDS. 2013;27(11):613–20.
Messer LC, Quinlivan EB, Parnell H, Roytburd K, Adimora AA, Bowditch N, et al. Barriers and facilitators to testing, treatment entry, and engagement in care by HIV-positive women of color. AIDS Patient Care STDS. 2013;27(7):398–407.
Berger MB, Sullivan KA, Parnell HE, Keller J, Pollard A, Cox ME, et al. Barriers and facilitators to retaining and reengaging HIV clients in care: a case study of North Carolina. J Int Assoc Provid AIDS Care. 2016;15(6):486–93.
Reif SS, Wilson E, McAllaster C. HIV stigma study in the deep south: descriptive findings. Southern HIV/AIDS Strategy Initiative. 2017. https://southernaids.files.wordpress.com/2017/08/revised-stigma-report-formatted-in-pdf.pdf. Accessed 27 Jan 2018.
Bradford JB, Coleman S, Cunningham W. HIV system navigation: an emerging model to improve HIV care access. AIDS Patient Care STDS. 2007;21(Suppl 1):S49–58.
Mugavero MJ, Norton WE, Saag MS. Health care system and policy factors influencing engagement in HIV medical care: piecing together the fragments of a fractured health care delivery system. Clin Infect Dis. 2011;52(Suppl 2):S238–46.
Craw JA, Gardner LI, Marks G, Rapp RC, Bosshart J, Duffus WA, et al. Brief strengths-based case management promotes entry into HIV medical care: results of the antiretroviral treatment access study-II. J Acquir Immune Defic Syndr. 2008;47(5):597–606.
Gardner LI, Metsch LR, Anderson-Mahoney P, Loughlin AM, del Rio C, Strathdee S, et al. Efficacy of a brief case management intervention to link recently diagnosed HIV-infected persons to care. AIDS. 2005;19(4):423–31.
Higa DH, Crepaz N, Mullins MM. Identifying best practices for increasing linkage to, retention, and re-engagement in HIV medical care: findings from a systematic review, 1996–2014. AIDS Behav. 2016;20(5):951–66.
Udeagu CC, Webster TR, Bocour A, Michel P, Shepard CW. Lost or just not following up: public health effort to re-engage HIV-infected persons lost to follow-up into HIV medical care. AIDS. 2013;27(14):2271–9.
Thompson MA, Mugavero MJ, Amico KR, Cargill VA, Chang LW, Gross R, et al. Guidelines for improving entry into and retention in care and antiretroviral adherence for persons with HIV: evidence-based recommendations from an International Association of Physicians in AIDS Care panel. Ann Intern Med. 2012;156(11):817-33, W-284, W-285, W-286, W-287, W-288, W-289, W-290, W-291, W-292, W-293, W-294.
Keller J, Heine A, LeViere AF, Donovan J, Wilkin A, Sullivan K, Quinlivan EBHIV. Patient retention: the implementation of a North Carolina clinic based protocol. AIDS Care. 2017;29(5):627–31.
Koester KA, Fuller SM, Maiorana A, Steward WT, Zamudio-Haas S, Xavier J, et al. Implementing multi-level interventions to improve HIV testing, linkage-to-and retention-in-care interventions. J Health Care Poor Underserved. 2016;27(3):1234–51.
Swygard H, Seña AC, Mobley V, Glenn K, Keller JE, Sampson LA, Heine A, Klein E, Berger M, Sullivan KA, Clymore J, Quinlivan EB. Connections to HIV care using a modified ARTAS program and a statewide team. In: 10th International Conference on HIV Treatment and Prevention Adherence; Miami, FL2015.
Seña AC, Donovan J, LeViere A, Swygard H, Clymore J, Mobley V, Sullivan K, Willis S, Heine A, Quinlivan EB. Outcomes from the “NC LINK” program: a statewide approach to HIV linkage and re-engagement to care in North Carolina. In: 11th International Conference on HIV Treatment and Prevention Adherence; Ft. Lauderdale, FL2016.
Davidoff F, Batalden P, Stevens D, Ogrinc G, Mooney S. Publication guidelines for quality improvement studies in health care: evolution of the SQUIRE project. J Gen Intern Med. 2008;23(12):2125–30.
Colasanti J, Kelly J, Pennisi E, Hu YJ, Root C, Hughes D, et al. Continuous retention and viral suppression provide further insights into the HIV care continuum compared to the cross-sectional HIV care cascade. Clin Infect Dis. 2016;62(5):648–54.
Marks G, Patel U, Stirratt MJ, Mugavero MJ, Mathews WC, Giordano TP, et al. Single viral load measurements overestimate stable viral suppression among HIV patients in care: clinical and public health implications. J Acquir Immune Defic Syndr. 2016;73:205–12.
Olson AD, Walker AS, Suthar AB, Sabin C, Bucher HC, Jarrin I, et al. Limiting cumulative HIV viremia copy-years by early treatment reduces risk of AIDS and death. J Acquir Immune Defic Syndr. 2016;73(1):100–8.
Gardner LI, Marks G, Craw JA, Wilson TE, Drainoni ML, Moore RD, et al. A low-effort, clinic-wide intervention improves attendance for HIV primary care. Clin Infect Dis. 2012;55(8):1124–34.
Gardner LI, Giordano TP, Marks G, Wilson TE, Craw JA, Drainoni ML, et al. Enhanced personal contact with HIV patients improves retention in primary care: a randomized trial in 6 US HIV clinics. Clin Infect Dis. 2014;59(5):725–34.
Lubelchek RJ, Fritz ML, Finnegan KJ, Trick WE. Use of a real-time alert system to identify and re-engage lost-to-care HIV patients. J Acquir Immune Defic Syndr. 2016;72(2):e52–5.
Christopoulos KA, Scheer S, Steward WT, Barnes R, Hartogensis W, Charlebois ED, et al. Examining clinic-based and public health approaches to ascertainment of HIV care status. J Acquir Immune Defic Syndr. 2015;69(Suppl 1):S56–62.
Bove JM, Golden MR, Dhanireddy S, Harrington RD, Dombrowski JC. Outcomes of a clinic-based surveillance-informed intervention to relink patients to HIV care. J Acquir Immune Defic Syndr. 2015;70(3):262–8.
Buskin SE, Kent JB, Dombrowski JC, Golden MR. Migration distorts surveillance estimates of engagement in care: results of public health investigations of persons who appear to be out of HIV care. Sex Transm Dis. 2014;41(1):35–40.
Sullivan KA, Berger MB, Quinlivan EB, Parnell HE, Sampson LA, Clymore JM, et al. Perspectives from the field: HIV testing and linkage to care in North Carolina. J Int Assoc Provid AIDS Care. 2016;15(6):477–85.
Funding
This research was supported by funds from HRSA’s Special Projects of National Significance Initiative: Systems Linkages (H97HA22695). The authors have no conflicts of interest to report. This study was conducted with the approval of the Institutional Review Board. The program was implemented as clinical care and did not require written consent. Written consent was obtained for focus groups and interviews. The authors also acknowledge the clinic staff, providers, and patients for their invaluable contributions to this research. The content is solely the responsibility of the authors and does not necessarily represent the official views of the Health Resources and Services Administration.
Author information
Authors and Affiliations
Contributions
All authors have made a contribution to the manuscript work, analysis, writing or editing and accept responsibility for publication. The authors also acknowledges the clinic staff, providers, and patients for their invaluable contributions to this research.
Corresponding author
Ethics declarations
Conflict of interest
A Wilkin receives research funding from Gilead, Janssen, Pfizer. All other authors report no real or perceived vested interests that relate to this article that could be construed as a conflict of interest.
Ethical Approval for Human Subjects
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Ethical Approval for Animal Research
This article does not contain any studies with animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Donovan, J., Sullivan, K., Wilkin, A. et al. Past Care Predicts Future Care in Out-of-Care People Living with HIV: Results of a Clinic-Based Retention-in-Care Intervention in North Carolina. AIDS Behav 22, 2687–2697 (2018). https://doi.org/10.1007/s10461-018-2106-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-018-2106-5