Abstract
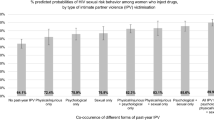
HIV/AIDS and intimate partner violence (IPV) are growing public health concerns in South Africa. Knowledge about adult men’s perpetration of IPV and links between HIV risk behaviours and IPV is limited. Respondent driven sampling was used to recruit men who have multiple concurrent female sexual partners. Forty-one percent of the 428 recruited men had perpetrated IPV. Inconsistent condom use was associated with physical IPV; experiencing a symptom of a sexually transmitted infection and engaging in transactional sex were associated with physical and sexual IPV; problem alcohol use was associated with physical, and any IPV, but not sexual IPV; having five or more partners was associated with sexual IPV; perceptions of partners’ infidelity were associated with physical and any IPV. HIV risk reduction interventions among men, especially those with multiple female sex partners, should incorporate strategies to change the underlying construction of masculinity that combines the anti-social and risky behaviours of IPV perpetration, inconsistent condom use, transactional sex and heavy alcohol consumption.
Similar content being viewed by others
References
Shisana O, Rehle T, Simbayi LC, et al. South African national HIV prevalence, incidence, behaviour and communication survey 2008: a turning tide among teenagers? Cape Town (South Africa): HSRC Press; 2009.
UNAIDS. Report on the global AIDS epidemic. Geneva (Switzerland): UNAIDS; 2006.
Mitchell Fuentes CM. Pathways from interpersonal violence to sexually transmitted infections: a mixed-method study of diverse women. J Womens Health. 2008;17(10):1591–602.
Norman R, Bradshaw D, Schneider M, et al. Estimating the burden of disease attributable to interpersonal violence in South Africa 2000. S Afr Med J. 2007;97(8):653–5.
Garcia-Moreno C, Jansen HAFM, Ellsberg M, Heise L, Watts CH. Prevalence of intimate partner violence: findings from the WHO multi-country study on women’s health and domestic violence. Lancet. 2006;368:1260–9.
Dunkle KL, Jewkes RK, Brown HC, et al. Prevalence and patterns of gender-based violence and revictimization among women attending antenatal clinics in Soweto, South Africa. Am J Epidemiol. 2004;160:230–9.
Dunkle KL, Jewkes RK, Brown HC, Gray GE, McIntyre JA, Harlow SD. Gender-based violence, relationship power, and risk of HIV infection in women attending antenatal clinics in South Africa. Lancet. 2004;363:1415–20.
Jewkes R, Dunkle K, Nduna M, et al. Factors associated with HIV sero-status in young rural South African women: connections between intimate partner violence and HIV. Int J Epidemiol. 2006;35:1461–8.
Kalichman SC, Simbayi LC. Sexual assault history and risks for sexually transmitted infections among women in an African township in Cape Town, South Africa. AIDS Care. 2004;16:681–9.
Jewkes R, Sikweyiya Y, Morrell R, Dunkle K (2009) Understanding men’s health and use of violence: interface of rape and HIV in South Africa [Technical Report]. Pretoria (South Africa): Medical Research Council; 2009 [cited 2009 October 20]. Available from: http://www.mspsouthafrica.org/files/page/264510/violence_hiv.pdf.
Dunkle KL, Jewkes RK, Nduna M, et al. Perpetration of partner violence and HIV risk behaviour among young men in the rural Eastern Cape, South Africa. AIDS. 2006;20:1–8.
Abrahams N, Jewkes R, Hoffman M, Laubscher R. Sexual violence against intimate partners in Cape Town: prevalence and risk factors reported by men. Bull World Health Organ. 2004;82:330–7.
Abrahams N, Jewkes R, Laubscher R, Hoffman M. Intimate partner violence: prevalence and risk factors for men in Cape Town, South Africa. Violence Vict. 2006;21:247–64.
Jewkes R. Intimate partner violence: causes and prevention. Lancet. 2002;359:1423–9.
Wood K, Jewkes R. “Dangerous” love: reflections on violence among Xhosa township youth. In: Cornwall A, editor. Readings in gender in Africa. Bloomington (IN): Indiana University Press; 2005. p. 95–102.
Luke N. Age and economic asymmetries in the sexual relationships of adolescent girls in sub-Saharan Africa. Stud Fam Plann. 2003;34(2):67–74.
Andersson N, Cockcroft A, Shea B. Gender-based violence and HIV: relevance for HIV prevention in hyperendemic countries of southern Africa. AIDS. 2008;22(Suppl 4):S73–86.
Dunkle KL, Jewkes R, Nduna M, et al. Transactional sex with casual and main partners among young South African men in the rural Eastern Cape: prevalence, predictors, and associations with gender-based violence. Soc Sci Med. 2007;65:1235–48.
Jewkes R, Dunkle K, Koss MP, et al. Rape perpetration by young, rural South African men: prevalence, patterns and risk factors. Soc Sci Med. 2006;63:2949–61.
Simbayi LC, Kalichman SC, Jooste S, Mathiti V, Cain D, Cherry C. HIV/AIDS risks among South African men who report sexually assaulting men. Am J Health Behav. 2006;30(2):158–66.
Hoffman S, O’Sullivan LF, Harrison A, Dolezal C, Monroe-Wise A. HIV risk behaviors and the context of sexual coercion in young adults’ sexual interactions: results from a diary study in rural South Africa. Sex Transm Dis. 2006;33:52–8.
Chersich MF, Rees HV. Vulnerability of women in southern Africa to infection with HIV: biological determinants and priority health sector interventions. AIDS. 2008;22(Suppl 4):S27–40.
Shisana O, Simbayi L. Nelson Mandela/HSRC study of HIV/AIDS: South African national HIV prevalence, behavioural risks and mass media household survey. Cape Town (South Africa): HSRC Press; 2002.
Parker W, Makhubele B, Nlabati P. Connolly C. Concurrent sexual partnerships amongst young adults in South Africa. Challenges for HIV prevention communication [e-report]. Grahamstown (South Africa): CADRE; 2007 [cited 2009 October 9]. Available from: http://www.cadre.org.za/node/140.
Halperin DT, Epstein H. Concurrent sexual partnerships help to explain Africa’s high HIV prevalence: implications for prevention. Lancet. 2004;364:3–6.
Soul City. Multiple and concurrent sexual partnerships in Southern Africa: a ten country research report. Johannesburg (South Africa): Soul City; 2008.
Halperin DT, Epstein H. Concurrent sexual partnerships help to explain Africa’s high HIV prevalence: implications for prevention. Lancet. 2004;364:3–6.
Mah TL, Halperin DT. Concurrent sexual partnerships and the HIV epidemics in Africa: Evidence to move forward. AIDS Behav [serial online]. 2008 [cited 2009 October 3]; 2008 July 22. Available from: http://www.springerlink.com/content/aq8244262614q762/.
Kendall C, Kerr LRFS, Gondim RC, et al. An empirical comparison of respondent-driven sampling, time location sampling, and snowball sampling for behavioral surveillance in men who have sex with men, Fortaleza, Brazil. AIDS Behav. 2008;12:S97–104.
Heckathorn DD. Extensions of respondent-driven sampling: analyzing continuous variables and controlling for differential recruitment. Sociol Methodol. 2007;37:151–207.
Malekinejad M, Johnston JG, Kendall C, Kerr LRFS, Rifkin M, Rutherford GW. Using respondent-driven sampling methodology for HIV biological and behavioral surveillance in international settings: a systematic review. AIDS Behav. 2008;12:S105–30.
Heckathorn D. Respondent driven sampling: a new approach to the study of hidden populations. Soc Probl. 1997;44:174–99.
Heckathorn D. Respondent driven sampling II: deriving valid population estimates from chain-referral samples of hidden populations. Soc Probl. 2002;49(1):11–34.
Leclerc-Madlala S. Age-disparate and intergenerational sex in southern Africa: the dynamics of hypervulnerability. AIDS. 2008;22(supp. 4):S17–25.
Zietsman HL. Recent changes in the population structure of Stellenbosch municipality. Stellenbosch (South Africa): Geographical Systems Research Bureau; 2007.
Common Ground Holdings and Neville Naidoo and Associates. Social survey 2005: Stellenbosch Municipality (WC24). Unpublished report compiled for Stellenbosch Municipality, Western Cape Province, South Africa; 2006.
Johnston LG. Conducting respondent driven sampling (RDS) Studies in diverse settings: a training manual for planning RDS studies [e-manual]. Centers for Disease Control and Prevention: Atlanta (GA) and Family Health International: Arlington (VA); 2007 [cited 2009 November 2]. Available from: http://globalhealthsciences.ucsf.edu/PPHG/assets/docs/respondent-driven-sampling-2008.pdf.
Shaikh N, Abdullah F, Lombard CJ, Smit L, Bradshaw D, Makubalo L. Masking through averages—intraprovincial heterogeneity in HIV prevalence within the Western Cape. S Afr Med J. 2006;96:538–43.
Ewing JA. Detecting alcoholism. JAMA. 1968;252:1905–7.
Dhalla S, Kopee JA. The CAGE questionnaire for alcohol misuse. A review of reliability and validity studies. Clin Invest Med. 2007;30:33–41.
Vittenghoff E, Glidden DV, Shiboski SC, McCullough CE. Regression methods in biostatistics: liner, logistic, survival, and repeated measures models. New York (NY): Springer; 2005.
Jewkes R, Levin J, Penn-Kekana L. Risk factors for domestic violence: findings from a South African cross-sectional study. Soc Sci Med. 2002;55:1603–17.
Zablotska IB, Gray RH, Koenig MA, et al. Alcohol use, intimate partner violence, sexual coercion and HIV among women aged 15–24 in Rakai, Uganda. AIDS Behav. 2009;13:225–33.
Townsend L, Ragnarsson A, Mathews C, Johnston LG, Ekström AM, Thorson A, Chopra M. “Taking Care of Business”: alcohol as currency in transactional sexual relationships among players in Cape Town, South Africa. Qual Health Res. 2010 (in press).
Ragnarsson A, Townsend L, Thorson A, Chopra M, Ekström AM. Social networks and concurrent sexual relationships—a qualitative study among men in an urban South African community. AIDS Care. 2009;21(10):1253–8.
Jewkes R, Nduna M, Levin J, et al. Impact of Stepping Stones on incidence of HIV and HSV-2 and sexual behaviour in rural South Africa: cluster randomised controlled trial. BMJ. 2008;337:a506.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Townsend, L., Jewkes, R., Mathews, C. et al. HIV Risk Behaviours and their Relationship to Intimate Partner Violence (IPV) Among Men Who Have Multiple Female Sexual Partners in Cape Town, South Africa. AIDS Behav 15, 132–141 (2011). https://doi.org/10.1007/s10461-010-9680-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-010-9680-5