Abstract
Background In recent years there has been a notable increase in respiratory diseases in industrialised countries, which is attributed to a combination of chemical atmospheric pollution and the allergens existing in the atmosphere of big cities. Few studies, however, have analysed the effect of different pollen species on the different causes of hospital admissions other than those exclusively owing to asthma. Objective The aim of this investigation was to analyse the influence of the most abundant pollen species with the highest allergenic potential in Madrid’s atmosphere on daily emergency hospital admissions – from all causes and specific causes – according to different age groups. Methods An ecological time-series design was adopted in which the effects were quantified using Poisson regression models, taking into account different confusion factors, such as chemical and acoustic atmospheric pollution. Results Statistically significant associations were found between pollen species and hospital admissions due to respiratory causes, and between pollen species and all causes of hospital admissions and, to a lesser degree, circulatory causes. The impact was greater in the younger age groups. Concentrations of Poaceae and Platanus pollen species were the factors showing the highest correlation to the different causes of admission. Conclusion The relative risks analysis revealed a significant effect between the pollen species analysed and health for admitted patients of all age groups; this effect was greater than that detected for the environmental variables traditionally analysed in urban atmospheres.

Similar content being viewed by others
Abbreviations
- ACF:
-
Simple autocorrelation function
- AR:
-
Attributable risk
- COPD:
-
Chronic obstructive pulmonary disease
- ICD-IX:
-
International Classification of Diseases version 9
- PACF:
-
Partial autocorrelation function
- RR:
-
Relative risk
References
Akaike, H. (1974). A New look at statistical model identification. IEEE Transactions on Automatic Control, 9, 716–722.
Akinbami, L. J., & Schoendord, K. C. (2002). Trends in childhood asthma: Prevalence, healthcare utilization and mortality. Pediatrics, 110, 315–322.
Anderson, H. R., Ponce de Leon, A., Bland, J. M., et al. (1998). Air pollution, pollens and daily admissions for asthma in London 1987–92. Thorax, 53, 842–848.
Brunekreef, B., Hoek, G., Fischer, P., et al. (2000). Relation between airborne pollen concentrations and daily cardiovascular and respiratory-disease mortality. The Lancet, 355, 1517–1518.
Campbell, M. J., & Tobias, A. (2000). Causality and temporality in the study of short-term effects of air pollution on health. International Journal Epidemiology, 29, 271–273.
Clot, B. (2003). Trends in airborne pollen : An overview of 21 years of data in Neuchâtel (Switzerland). Aerobiología, 19, 227–234.
Coste, J., & Spira, A. (1991). Le proportion de cas attributable en Santé Publique: definition(s), estimation(s) et interprétation. Reviste Epidemiologique Santé Publique, 51, 399–41.
Dales, R. E., Cakmak, S., Burnett, R. T., et al. (2000). Influence of ambient fungal spores on emergency visits for asthma to a regional children’s hospital. American Journal Respiratory Critical Care Medicine, 162, 2087–2090.
D’Amato, G. (2002). Environmental urban factors (air pollution and allergens) and the rising trends in allergic respiratory diseases. Allergy, 57(Suppl 72), 30–33.
D’Amato, G., Liccardi, G., D’Amato, M., et al. (2001). The role of outdoor air pollution and climatic changes on the rising trends in respiratory allergy. Respiratory Medicine, 95, 606–611.
Díaz, J., & Linares, C. (2007). Impact of high temperatures on hospital admissions in Madrid (Spain): A comparative analysis with mortality in heat waves. European Journal of Public Health (in press).
Díaz, J., García, R., Ribera, P., et al. (1999). Modelling of air pollution and its relationship with mortality and morbidity in Madrid, Spain. International Archives Occupational and Environmental Health, 73, 366–376.
Díaz, J., Alberdi, J. C., Pajares, M. S. et al. (2001). A model for forecasting emergency hospital admissions: Effect of environmental variables. Journal of Environmental Health, 2001, 64, 9–15.
Díaz, J., Linares, C., Sabariego, S., et al. (2006). Predictive model for Cupressceae-Taxaceae in Madrid Using ARIMA models”. In Proc 8th Int Congr Aerobiol. Neuchâtel.
EPA. (2003). Air pollution and children´s health. A fact sheet by Cal/EPA´s Office of Environmental Health Hazards Assessment and the American Lung Association of California.
Frenguelli, G., Tedechini, E., Veronesi, F., et al. (2002). Airborne pine (pinus spp.) pollen in the atmosphere of Perugia (Central Italy): Behavior of pollination in the two last decades. Aerobiología, 18, 223–228.
Galán, I., Tobías, A., Banegas, J. R., et al. (2003). Short-term effects of air pollution on daily asthma emergency room admissions in Madrid, Spain. European Respiratory Journal, 22, 802–808.
Gilmour, M. E., Jaakkola, M. S., London, S. J., et al. (2006). How exposure to environmental tobacco smoke, outdoor air pollutants and increased pollen burdens influences the incidence of asthma. Environmental Health Perspectives, 114, 627–633.
Gutierrez, M., Sáenz, C., Aránguez, E., et al. (2001). Polen atmosférico en la Comunidad de Madrid. Documentos Técnicos de Salud Pública no 70. Editor Consejeria de Sanidad, Madrid
Hospers, J. J., Rijcken, B., Schouten, J. P., et al. (1999). Eosinophilia and positive skin tests predict cardiovascular mortality in a general population sample followed for 30 years. American Journal Epidemiology, 150, 482–491.
Korhonen, K., Reijonen, T. M., Malmstrom, K., et al. (2002). Hospitalization trends for paediatric asthma in eastern Finland: A 10-yr survey. European Respiratory Journal, 19, 1035–1039.
Kroll-Smith, S., Brown, P., & Gunter, V. S. (2000) Illness and the environment: A reader in contested medicine. New York: University Press.
Landringan, P. J., Suk, W., & Amler, R. W. (1999). Chemical wastes, children´s health, and the Superfund basic research program. Environmental Health Perspectives, 107, 423–427.
Lee, J. T., Kim, H., Song, H., et al. (2002). Air pollution and asthma among children in Seoul, Korea. Epidemiology, 13, 481–484.
Lewis, S. A., Gorden, J. M., Forster, G. E., et al. (2000). Combined effects of aerobiological pollutants, chemical pollutants and meteorological conditions on asthma admissions and A&E attendances in Derbyshire UK, 1993–1996. Clinical Experimental Allergy, 30, 1724–1730.
Lierl, M. B., & Hornung, R. W. (2003). Relationship of outdoor air quality to pediatric asthma exacerbation. Annales Allergy Asthma Inmunologie, 90, 1–2.
Linares, C., Díaz, J., Tobías, A., et al. (2006a) Impact of urban air pollutants and noise levels over daily hospital admissions in children in Madrid: A time series analysis. International Archives Occupational and Environmental Health, 79, 143–152.
Linares, C., Díaz, J., Tobías, A., et al. (2006b). A review of epidemiological evidence on short term effects of environmental factors of respiratory problems in children. Current Respiratory Medicine Review, 2, 173–181.
Low, R. B., Bielory, L., Qureshi, A. I., et al. (2006). The relation of strode admissions to recent weather, airborne allergens, air pollution, seasons, upper respiratory infections and asthma incidence, September 11, 2001 and day of the week. Stroke, 37, 951–957.
McMichael, A. J., Wooddruff, R. E., & Hales, S. (2006). Climate change and human health: Present and future risks. The Lancet, 367, 859–869.
Morrison, D. S., & McLoone, P. (2001). Changing patterns of hospital admissions for asthma, 1981–1997. Thorax, 56, 687–690.
Newson, R., Strachan, D., Archiblad, E., et al. (1998). Acute asthma epidemics, weather and pollen in England, 1987–1994. European Respiratory Journal, 11, 694–701.
Ng, T. P., Niti, M., & Tan, W. C. (2003). Trends and ethnic differences in asthma hospitalisations rates in Singapore, 1991 to 1998. Annales Allergy Asthma Immunologie, 90, 51–55.
Schwartz, J., Spix, C., Touloumi, G., et al. (1996). Methodological issues in studies of air pollution and daily counts of deaths or hospital admissions. Journal Epidemiology Community Health, 50[Suppl 1], S3–11.
Soriano, J. B., Kiri, V. A., Maier, W. C. et al. (2003). Increasing prevalence of asthma in K primary care during 1990s. International Journal of Tuberculosis Lung Disease, 7, 415–421.
Stieb, D. M., Beveridge, R. C., Brook, J. R., et al. (2000). Journal Exposure Annales Environmental Epidemiology, 10, 461–477.
Subiza, J., Cabrera, M., Valdivieso, R., et al. (1994). Seasonal asthma caused by airborne platanus pollen. Clinical Experimental Allergy, 24, 1123–1129.
Subiza, J., Jerez, M., Jiménez, J. A., et al. (1995). Allergenic pollen and pollinosis in Madrid. Journal Allergy Clinical Immunology, 96, 15–23.
Thurston, G. D., Ito, K., & Kinney, P. L. (1992). A multi-year study of air pollution and respiratory hospital admissions in three New York State metropolitan areas: Results for 1988 and 1989 summers. Journal Exposure Annales Environmental Epidemiology, 2, 429–450.
Tobías, A., Díaz, J., Sáez, M., et al. (2001). Use of Poisson regression and Box-Jenkins models to evaluate the short-term effects of environmental noise levels on daily emergency admissions in Madrid, Spain. European Journal of Epidemiology, 151, 50–56.
Tobías, A., Galán, I., & Banegas, J. R. (2003). Short-term effects of airborne pollen concentrations on asthma epidemic. Thorax, 58, 708–710.
Acknowledgements
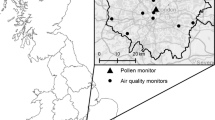
The authors gratefully acknowledge the Madrid Regional Health Authority Palynology Network (PALINOCAM) for providing the pollen data.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Díaz, J., Linares, C. & Tobías, A. Short-term effects of pollen species on hospital admissions in the city of Madrid in terms of specific causes and age. Aerobiologia 23, 231–238 (2007). https://doi.org/10.1007/s10453-007-9067-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10453-007-9067-x