Abstract
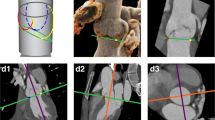
Patients with bicuspid aortic valve (BAV) commonly have associated aortic stenosis and aortopathy. The geometry of the aortic arch and BAV is not well defined quantitatively, which makes clinical classifications subjective or reliant on limited 2D measurements. The goal of this study was to characterize the 3D geometry of the aortic arch and BAV using objective and quantitative techniques. Pre-TAVR computed tomography angiogram (CTA) in patients with BAV and aortic stenosis (AS) were analyzed (n = 59) by assessing valve commissural angle, presence of a fused region, percent of fusion, and calcium volume. The ascending aorta and aortic arch were reconstructed from patient-specific imaging segmentation to generate a centerline and calculate maximum curvature and maximum area change for the ascending aorta and the descending aorta. Aortic valve commissural angle signified a bimodal distribution suggesting tricuspid-like (≤ 150°, 52.5% of patients) and bicuspid-like (> 150°, 47.5%) morphologies. Tricuspid like was further classified by partial (10.2%) or full (42.4%) fusion, and bicuspid like was further classified into valves with fused region (27.1%) or no fused region (20.3%). Qualitatively, the aortic arch was found to have complex patient-specific variations in its 3D shape with some showing extreme diameter changes and kinks. Quantitatively, subgroups were established using maximum curvature threshold of 0.04 and maximum area change of 30% independently for the ascending and descending aorta. These findings provide insight into the geometric structure of the aortic valve and aortic arch in patients presenting with BAV and AS where 3D characterization allows for quantitative classification of these complex anatomic structures.












Similar content being viewed by others
Abbreviations
- AS:
-
Aortic stenosis
- AV:
-
Aortic valve
- BAV:
-
Bicuspid aortic valve
- CTA:
-
Computed tomography angiogram
- MRI:
-
Magnetic resonance imaging
- STJ:
-
Sinotubular junction
- TAVR:
-
Transcatheter aortic valve replacement
References
Siu, S. C., and C. K. Silversides. Bicuspid aortic valve disease. Journal of the American College of Cardiology. 55(25):2789–2800, 2010.
Verma, S., and S. C. Siu. Aortic dilatation in patients with bicuspid aortic valve. N Engl J Med. 370:1920–1929, 2014.
Carabello, B. A., and W. J. Paulus. Aortic stenosis. The Lancet. 373(9667):956–966, 2009.
Lindman, B. R., et al. Calcific aortic stenosis. Nature reviews Disease primers. 2(1):1–28, 2016.
Yang, L.-T., et al., Aortic Stenosis Progression, Cardiac Damage, and Survival: Comparison Between Bicuspid and Tricuspid Aortic Valves. JACC: Cardiovascular Imaging %@ 1936-878X, 2021.
Blanke, P., et al. Computed tomography imaging in the context of transcatheter aortic valve implantation (TAVI)/transcatheter aortic valve replacement (TAVR) an expert consensus document of the Society of Cardiovascular Computed Tomography. JACC: Cardiovascular Imaging. 12(1):1–24, 2019.
Bax, J. J., et al. Transcatheter aortic valve replacement: role of multimodality imaging in common and complex clinical scenarios. Cardiovascular Imaging. 13(1_Part):124–139, 2020.
Burzotta, F., et al. Clinical and procedural impact of aortic arch anatomic variants in carotid stenting procedures. Catheterization and Cardiovascular Interventions. 86(3):480–489, 2015.
Shen, S., et al. Effect of aortic arch type on technical indicators in patients undergoing carotid artery stenting. Journal of International Medical Research. 47(2):682–688, 2019.
Frydrychowicz, A., et al. Interdependencies of aortic arch secondary flow patterns, geometry, and age analysed by 4-dimensional phase contrast magnetic resonance imaging at 3 Tesla. European Radiology. 22(5):1122–1130, 2012.
Grabenwöger, M., et al. Thoracic Endovascular Aortic Repair (TEVAR) for the treatment of aortic diseases: a position statement from the European Association for Cardio-Thoracic Surgery (EACTS) and the European Society of Cardiology (ESC), in collaboration with the European Association of Percutaneous Cardiovascular Interventions (EAPCI). European Heart Journal. 33(13):1558–1563, 2012.
Abramowitz, Y., et al. Aortic angulation attenuates procedural success following self-expandable but not balloon-expandable TAVR. JACC: Cardiovascular Imaging. 9(8):964–972, 2016.
O’Flynn, P. M., G. O’Sullivan, and A. S. Pandit. Methods for three-dimensional geometric characterization of the arterial vasculature. Annals of Biomedical Engineering. 35(8):1368–1381, 2007.
Müller-Eschner, M., et al. Accuracy and variability of semiautomatic centerline analysis versus manual aortic measurement techniques for TEVAR. European Journal of Vascular and Endovascular Surgery. 45(3):241–247, 2013.
Suh, G.-Y., et al. Aortic arch vessel geometries and deformations in patients with thoracic aortic aneurysms and dissections. Journal of Vascular and Interventional Radiology. 25(12):1903–1911, 2014.
Chiu, P., et al. Anatomical characteristics of the thoracic aortic arch in an Asian population. Asian Cardiovascular and Thoracic Annals. 21(2):151–159, 2013.
Alhafez, B. A., et al. Aortic arch tortuosity, a novel biomarker for thoracic aortic disease, is increased in adults with bicuspid aortic valve. International Journal of Cardiology. 284:84–89, 2019.
Kilner, P. J., et al. Helical and retrograde secondary flow patterns in the aortic arch studied by three-directional magnetic resonance velocity mapping. Circulation. 88(5):2235–2247, 1993.
Hatoum, H., B. L. Moore, and L. P. Dasi. On the significance of systolic flow waveform on aortic valve energy loss. Annals of Biomedical Engineering. 46(12):2102–2111, 2018.
Michelena, H. I., et al. International consensus statement on nomenclature and classification of the congenital bicuspid aortic valve and its aortopathy, for clinical, surgical, interventional and research purposes. European Journal of Cardio-Thoracic Surgery. 60(3):448–476, 2021.
Sievers, H.-H., and C. Schmidtke. A classification system for the bicuspid aortic valve from 304 surgical specimens. Journal of Thoracic and Cardiovascular Surgery. 133(5):1226–1233, 2007.
Jackson, P. R., G. T. Tucker, and H. F. Woods. Testing for bimodality in frequency distributions of data suggesting polymorphisms of drug metabolism-histograms and probit plots. British Journal of Clinical Pharmacology. 28(6):647–653, 1989.
Jilaihawi, H., et al. A bicuspid aortic valve imaging classification for the TAVR era. JACC: Cardiovascular Imaging. 9(10):1145–1158, 2016.
Yoon, S.-H., et al. Bicuspid aortic valve morphology and outcomes after transcatheter aortic valve replacement. Journal of the American College of Cardiology. 76(9):1018–1030, 2020.
Fukui, M., et al. Deformation of transcatheter aortic valve prostheses: implications for hypoattenuating leaflet thickening and clinical outcomes. Circulation. 146(6):480–493, 2022.
Gunning, P. S., et al. An in vitro evaluation of the impact of eccentric deployment on transcatheter aortic valve hemodynamics. Annals of Biomedical Engineering. 42(6):1195–1206, 2014.
Bettinger, N., et al. Practical determination of aortic valve calcium volume score on contrast-enhanced computed tomography prior to transcatheter aortic valve replacement and impact on paravalvular regurgitation: elucidating optimal threshold cutoffs. Journal of Cardiovascular Computed Tomography. 11(4):302–308, 2017.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Breandan B. Yeats has a patent pending as co-inventor of patents related to computational predictive modeling of heart valves and is a stakeholder in DASI Simulations. Sri Krishna Sivakumar has a patent pending as co-inventor of patents related to computational predictive modeling of heart valves. Pradeep K. Yadav is a consultant for Edwards Lifesciences, Medtronic Inc., Abbott Vascular, and Shockwave Medical. Vinod H. Thourani is a consultant or research with Abbott Vascular, Boston Scientific, Cryolife, Edwards Lifesciences, Medtronic Corp, and Shockwave Medical and stakeholder in Dasi Simulations. Lakshmi P. Dasi is a stakeholder in DASI Simulations and has a patent pending as co-inventor of patents related to computational predictive modeling of heart valves. Other authors report no conflicts of interest.
Additional information
Associate Editor Stefan M. Duma oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yeats, B.B., Galvez, D., Sivakumar, S.K. et al. 3D Characterization of the Aortic Valve and Aortic Arch in Bicuspid Aortic Valve Patients. Ann Biomed Eng (2024). https://doi.org/10.1007/s10439-024-03527-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10439-024-03527-8