Abstract
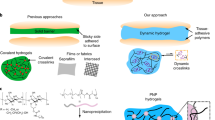
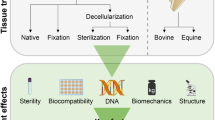
Postoperative adhesion is a very common and serious complication that occurs frequently in cardiac surgery. The purpose of this study was to evaluate the efficacy of a fibrin hydrogel layer-anchored decellularized pericardial matrix in preventing pericardial adhesions in a miniature pig model with a myocardial injury. Fibrin hydrogel layer-anchored decellularized pericardial matrix was prepared by spraying a mixture of fibrinogen and thrombin on a fibrinogen-doped decellularized pericardium. Cardiac injury was generated by abrading and desiccating the epicardial surface of a miniature pig to induce severe postoperative adhesions. The adhesion between the epicardial surface and fibrin hydrogel layer-anchored decellularized pericardial matrix in three different regions (left outer, front, and right outer) was evaluated macroscopically one month after surgery. The fibrin hydrogel layer-anchored decellularized pericardial matrix showed significantly less adhesion than an autologous pericardium (0.2 ± 0.7 in DPM-FHG0.5 and 0.4 ± 0.8 in DPM-FHG1, p < 0.01) and expanded polytetrafluoroethylene (ePTFE) (1.6 ± 0.5, p < 0.05). The fibrin hydrogel concentration had no effect on preventing postoperative adhesion. A thinner fibrin hydrogel layer was observed on the decellularized pericardial matrix one month after surgery; however, the inside of the matrix was filled with fibrin hydrogel. Fibrin hydrogel layer-anchored decellularized pericardial matrix prevented postoperative epicardial adhesions in a miniature pig model. Our findings suggest that pericardial closure using a fibrin hydrogel layer-anchored decellularized pericardial matrix is a promising method for preventing adverse outcomes in reoperative surgeries.





Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Arnold, P. B., C. W. Green, P. A. Foresman, and G. T. Rodeheaver. Evaluation of resorbable barriers for preventing surgical adhesions. Fertil Steril. 73:157–161, 2000. https://doi.org/10.1016/s0015-0282(99)00464-1.
Bahn, C. H., L. S. Annest, and M. Miyamoto. Pericardial closure. Am J Surg. 151:612–615, 1986.
Bel, A., M. Ricci, J. Piquet, P. Bruneval, M. C. Perier, C. Gagnieu, J. N. Fabiani, and P. Menasché. Prevention of postcardiopulmonary bypass pericardial adhesions by a new resorbable collagen membrane. Interact Cardiovasc Thorac Surg. 14:469–473, 2012. https://doi.org/10.1093/icvts/ivr159.
Cannata, A., D. Petrella, C. F. Russo, G. Bruschi, P. Fratto, M. Gambacorta, and L. Martinelli. Postsurgical intrapericardial adhesions: mechanisms of formation and prevention. Ann Thorac Surg. 95:1818–1826, 2013. https://doi.org/10.1016/j.athoracsur.2012.11.020.
Chen, Z., J. Zheng, J. Zhang, and S. Li. A novel bioabsorbable pericardial membrane substitute to reduce postoperative pericardial adhesions in a rabbit model. Interact Cardiovasc Thorac Surg. 21:565–572, 2015. https://doi.org/10.1093/icvts/ivv213.
Erikssen, G., K. Liestøl, E. Seem, S. Birkeland, K. J. Saatvedt, T. N. Hoel, G. Døhlen, H. Skulstad, J. L. Svennevig, E. Thaulow, et al. Achievements in congenital heart defect surgery: a prospective, 40-year study of 7038 patients. Circulation. 131:337–346, 2015. https://doi.org/10.1161/CIRCULATIONAHA.114.012033.
Fujita, M., G. M. Policastro, A. Burdick, H. T. Lam, J. L. Ungerleider, R. L. Braden, D. Huang, K. G. Osborn, J. H. Omens, M. M. Madani, et al. Preventing post-surgical cardiac adhesions with a catechol-functionalized oxime hydrogel. Nat Commun. 12:3764, 2021. https://doi.org/10.1038/s41467-021-24104-w.
Funamoto, S., Y. Hashimoto, A. Kishida, and J. Negishi. A fibrin-coated pericardial extracellular matrix prevented heart adhesion in a rat model. J Biomed Mater Res B Appl Biomater. 107:1088–1094, 2019. https://doi.org/10.1002/jbm.b.34201.
Gabbay, S. The need for intensive study of pericardial substitution after open heart surgery. ASAIO Trans. 36:789–791, 1990. https://doi.org/10.1097/00002480-199010000-00002.
Hashimoto, Y., A. Yamashita, J. Negishi, T. Kimura, S. Funamoto, and A. Kishida. 4-Arm PEG-functionalized decellularized pericardium for effective prevention of postoperative adhesion in cardiac surgery. ACS Biomater Sci Eng. 8:261–272, 2022. https://doi.org/10.1021/acsbiomaterials.1c00990.
Heydorn, W. H., J. S. Daniel, and C. E. Wade. A new look at pericardial substitutes. J Thorac Cardiovasc Surg. 94:291–296, 1987. https://doi.org/10.1016/S0022-5223(19)36296-8.
Hu, C., F. Tang, Q. Wu, B. Guo, W. A. Long, Y. Ruan, and L. Li. Novel trilaminar polymeric antiadhesion membrane prevents postoperative pericardial adhesion. Ann Thorac Surg. 111:184–189, 2021. https://doi.org/10.1016/j.athoracsur.2020.03.011.
Kaushal, S., S. K. Patel, S. K. Goh, A. Sood, B. L. Walker, and C. L. Backer. A novel combination of bioresorbable polymeric film and expanded polytetrafluoroethylene provides a protective barrier and reduces adhesions. J Thorac Cardiovasc Surg. 141:789–795, 2011. https://doi.org/10.1016/j.jtcvs.2010.11.043.
Kheilnezhad, B., and A. Hadjizadeh. A review: progress in preventing tissue adhesions from a biomaterial perspective. Biomater Sci. 9:2850–2873, 2021. https://doi.org/10.1039/d0bm02023k.
Komatsu, K., A. Fujii, and T. Higami. Haemostatic fleece (TachoComb) to prevent intrapleural adhesions after thoracotomy: a rat model. Thorac Cardiovasc Surg. 55:385–390, 2007. https://doi.org/10.1055/s-2007-965174.
Kumthekar, R. N., L. Sinha, J. D. Opfermann, P. Mass, B. C. Clark, C. Yerebakan, and C. I. Berul. Surgical pericardial adhesions do not preclude minimally invasive epicardial pacemaker lead placement in an infant porcine model. J Cardiovasc Electrophysiol. 31:2975–2981, 2020. https://doi.org/10.1111/jce.14724.
Kuschel, T. J., A. Gruszka, B. Hermanns-Sachweh, J. Elyakoubi, J. S. Sachweh, J. F. Vázquez-Jiménez, and H. Schnoering. Prevention of postoperative pericardial adhesions with TachoSil. Ann Thorac Surg. 95:183–188, 2013. https://doi.org/10.1016/j.athoracsur.2012.08.057.
Lefort, B., J. M. El Arid, A. L. Bouquiaux, N. Soulé, J. Chantreuil, E. Tavernier, A. Chantepie, and P. Neville. Is Seprafilm valuable in infant cardiac redo procedures? J Cardiothorac Surg. 10:47, 2015. https://doi.org/10.1186/s13019-015-0257-2.
Liu, Z., C. Chang, J. Liu, and Q. Wang. Right ventricular rupture in redo coronary artery bypass grafting. Heart Surg Forum. 23:E685–E688, 2020. https://doi.org/10.1532/hsf.3161.
Lunney, J. K., A. Van Goor, K. E. Walker, T. Hailstock, J. Franklin, and C. Dai. Importance of the pig as a human biomedical model. Sci Transl Med. 13:eabd5758, 2021. https://doi.org/10.1126/scitranslmed.abd5758.
Maltais, S., R. J. Widmer, M. R. Bell, R. C. Daly, J. A. Dearani, K. L. Greason, D. L. Joyce, L. D. Joyce, H. V. Schaff, and J. M. Stulak. Reoperation for coronary artery bypass grafting surgery: Outcomes and considerations for expanding interventional procedures. Ann Thorac Surg. 103:1886–1892, 2017. https://doi.org/10.1016/j.athoracsur.2016.09.097.
Mutsaers, S. E. The mesothelial cell. Int J Biochem Cell Biol. 36:9–16, 2004. https://doi.org/10.1016/s1357-2725(03)00242-5.
Nkere, U. U., S. A. Whawell, C. E. Sarraf, J. B. Schofield, J. N. Thompson, and K. M. Taylor. Pericardial trauma and adhesions in relation to reoperative cardiac surgery. Thorac Cardiovasc Surg. 43:338–346, 1995. https://doi.org/10.1055/s-2007-1013806.
Okuyama, N., C. Y. Wang, E. A. Rose, K. E. Rodgers, E. Pines, G. S. diZerega, and M. C. Oz. Reduction of retrosternal and pericardial adhesions with rapidly resorbable polymer films. Ann Thorac Surg. 68:913–918, 1999.
Seeger, J. M., L. D. Kaelin, E. M. Staples, Y. Yaacobi, J. C. Bailey, S. Normann, J. W. Burns, and E. P. Goldberg. Prevention of postoperative pericardial adhesions using tissue-protective solutions. J Surg Res. 68:63–66, 1997. https://doi.org/10.1006/jsre.1996.4990.
Steele, P. M., J. H. Chesebro, A. W. Stanson, D. R. Holmes, M. K. Dewanjee, L. Badimon, and V. Fuster. Balloon angioplasty. Natural history of the pathophysiological response to injury in a pig model. Circ Res. 57:105–112, 1985. https://doi.org/10.1161/01.res.57.1.105.
Thompson, J. N., and S. A. Whawell. Pathogenesis and prevention of adhesion formation. Br J Surg. 82:3–5, 1995. https://doi.org/10.1002/bjs.1800820103.
Tsukihara, H., S. Takamoto, K. Kitahori, K. Matsuda, A. Murakami, R. J. Novick, and Y. Suematsu. Prevention of postoperative pericardial adhesions with a novel regenerative collagen sheet. Ann Thorac Surg. 81:650–657, 2006. https://doi.org/10.1016/j.athoracsur.2005.07.022.
Yamashita, A., S. Funamoto, Y. Zhang, Y. Hashimoto, and A. Kishida. Rabbit model for evaluation of anti-adhesive materials after open heart surgery. Kyobu Geka. 71:658–663, 2018.
Zhang, E., J. Yang, K. Wang, B. Song, H. Zhu, X. Han, Y. Shi, C. Yang, Z. Zeng, and Z. Cao. Biodegradable zwitterionic cream gel for rffective prevention of postoperative adhesion. Adv Funct Mater. 31:2009431, 2021. https://doi.org/10.1002/adfm.202009431.
Zhou, J., J. M. Lee, P. Jiang, S. Henderson, and T. D. Lee. Reduction in postsurgical adhesion formation after cardiac surgery by application of N,O-carboxymethyl chitosan. J Thorac Cardiovasc Surg. 140:801–806, 2010. https://doi.org/10.1016/j.jtcvs.2009.11.030.
Zhou, D., P. Y. Yang, B. Zhou, and Y. C. Rui. Fibrin D-dimer fragments enhance inflammatory responses in macrophages: role in advancing atherosclerosis. Clin Exp Pharmacol Physiol. 34:185–190, 2007. https://doi.org/10.1111/j.1440-1681.2007.04570.x.
Acknowledgments
The Division of Acellular Tissue and Regenerative Medical Materials is an endowment department, established with a grant from ADEKA Corporation. This work was supported by funding from the ADEKA Corporation. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript. We thank KM Biologics Co., Ltd. for providing the fibrin glue (Bolheal®), which is commercially available. We thank Ashleigh Cooper, PhD, from Edanz (www.edanzediting.com/ac) for editing a draft of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Yoshihide Hashimoto, Akitatsu Yamashita, Yongwei Zhang, Seiichi Funamoto, and Akio Kishida receive a research support from ADEKA Corporation. Masaki Tabuchi has no conflict of interest.
Additional information
Associate Editor Andreas Anayiotos oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hashimoto, Y., Yamashita, A., Tabuchi, M. et al. Fibrin Hydrogel Layer-Anchored Pericardial Matrix Prevents Epicardial Adhesion in the Severe Heart Adhesion-Induced Miniature Pig Model. Ann Biomed Eng 52, 282–291 (2024). https://doi.org/10.1007/s10439-023-03373-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-023-03373-0