Abstract
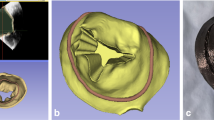
Functional mitral regurgitation (FMR) is a complex pathology involving valvular and subvalvular structures reconfiguration, and its treatment is considered challenging. There is a lack of experimental models allowing for reliable preclinical FMR treatments’ evaluation in a realistic setting. A novel approach to simulate FMR was developed and incorporated into an ex vivo passive beating heart platform. FMR was obtained by dilating the mitral annulus (MA) mainly in the antero-posterior direction and displacing the papillary muscles (PMs) apically and laterally by ad hoc designed and 3D printed dilation and displacing devices. It caused hemodynamic and valve morphology alterations. Isolated MA dilation (MAD) led to significantly increased antero-posterior distance (A-P) and decreased coaptation height (CH), tenting area (TA) and systolic leaflets angulation, resembling clinically recognized type I of mitral regurgitation with normal leaflet motion. Whereas concomitant MAD with PM displacement caused an increase in A-P, TA, CH. This geometrical configuration replicated typical determinants of type IIIb lesion with restricted leaflet motion. The proposed methods provided a realistic and repeatable ex vivo FMR model featuring two lesions clinically associated with the pathology. It bears a promise to be successfully utilized in preclinical studies, clinical training and medical education.







Similar content being viewed by others
Abbreviations
- MV:
-
Mitral valve
- FMR:
-
Functional mitral regurgitation
- MA:
-
Mitral annulus
- PM:
-
Papillary muscle
- CMV:
-
Competent mitral valve
- MAD:
-
Mitral annulus dilation
- PMD:
-
Papillary muscle displacement
- CO :
-
Cardiac output
- AoP :
-
Mean aortic pressure
- LAP :
-
Left atrial pressure
- LAP tot :
-
Mean whole-cycle left atrial pressure
- LAP syst :
-
Mean systolic left atrial pressure
- LAP diast :
-
Mean diastolic left atrial pressure
- ABF :
-
Aortic backflow fraction
- Δp :
-
Differential systolic pressure across mitral valve
- A-P :
-
Antero-posterior distance
- CH :
-
Coaptation height
- TA :
-
Tenting area
- PLA :
-
Posterior leaflet angle
- ALA :
-
Anterior leaflet angle
References
Alkhouli, M., S. Wolfe, F. Alqahtani, S. Aljohani, J. Mills, S. Gnegy, and V. Badhwar. The feasibility of transcatheter edge-to-edge repair in the management of acute severe ischemic mitral regurgitation. JACC Cardiovasc. Interv. 2017. doi:10.1016/j.jcin.2016.11.056.
Bhattacharya, S., T. Pham, Z. He, and W. Sun. Tension to passively cinch the mitral annulus through coronary sinus access: an ex vivo study in ovine model. J. Biomech. 47:1382–1388, 2014.
Carpentier, A., D. H. Adams, and F. Filsoufi. Carpentier’s Reconstructive Valve Surgery: From Valve Analysis to Valve Reconstruction. Maryland Heights, MO: Saunders/Elsevier, 2010.
Dal-Bianco, J. P., J. Beaudoin, M. D. Handschumacher, and R. A. Levine. Basic mechanisms of mitral regurgitation. Can. J. Cardiol. 30:971–981, 2014.
Enriquez-Sarano, M., et al. Mitral regurgitation. Lancet (Lond. Engl.) 373:1382–1394, 2009.
Feldman, T., and A. Young. Percutaneous approaches to valve repair for mitral regurgitation. J. Am. Coll. Cardiol. 63:2057–2068, 2014.
Fukamachi, K., M. Inoue, K. Doi, S. Schenk, H. Nemeh, C. Faber, J. L. Navia, and P. M. McCarthy. Reduction of mitral regurgitation using the Coapsys device: a novel ex vivo method using excised recipients hearts. ASAIO J. 51:82–84, 2005.
Gaemperli, O., P. Biaggi, R. Gugelmann, M. Osranek, J. J. Schreuder, I. Bühler, D. Sürder, T. F. Lüscher, C. Felix, D. Bettex, J. Grünenfelder, and R. Corti. Real-time left ventricular pressure–volume loops during percutaneous mitral valve repair with the Mitraclip system. Circulation 127:1018–1027, 2013.
Gertz, Z. M., A. Raina, L. Saghy, E. S. Zado, D. J. Callans, F. E. Marchlinski, M. G. Keane, and F. E. Silvestry. Evidence of atrial functional mitral regurgitation due to atrial fibrillation. J. Am. Coll. Cardiol. 58:1474–1481, 2011.
He, S., A. A. Fontaine, E. Schwammenthal, A. P. Yoganathan, and R. A. Levine. Integrated mechanism for functional mitral regurgitation. Circulation 96:1826–1834, 1997.
Jaworek, M., M. Piola, F. Lucherini, G. Gelpi, M. Castagna, G. Lentini, C. Antona, G. B. Fiore, and R. Vismara. Functional tricuspid regurgitation model in a beating heart platform. ASAIO J. 63:438–444, 2017. doi:10.1097/MAT.0000000000000510.
Khabbaz, K. R., F. Mahmood, O. Shakil, H. J. Warraich, J. H. Gorman, R. C. Gorman, R. Matyal, P. Panzica, and P. E. Hess. Dynamic 3-dimensional echocardiographic assessment of mitral annular geometry in patients with functional mitral regurgitation. Ann. Thorac. Surg. 95:105–110, 2013.
Kwan, J. Geometric differences of the mitral apparatus between ischemic and dilated cardiomyopathy with significant mitral regurgitation: real-time three-dimensional echocardiography study. Circulation 107:1135–1140, 2003.
Leopaldi, A. M., R. Vismara, M. Lemma, L. Valerio, M. Cervo, A. Mangini, M. Contino, A. Redaelli, C. Antona, and G. B. Fiore. In vitro hemodynamics and valve imaging in passive beating hearts. J. Biomech. 45:1133–1139, 2012.
Levine, R. A., et al. Mitral valve disease—morphology and mechanisms. Nat. Rev. Cardiol. 12:689–710, 2015.
Messas, E., A. Bel, C. Szymanski, I. Cohen, B. Touchot, M. D. Handschumacher, M. Desnos, A. Carpentier, P. Menasché, A. A. Hagège, and R. A. Levine. Relief of mitral leaflet tethering following chronic myocardial infarction by chordal cutting diminishes left ventricular remodeling. Circ. Cardiovasc. Imaging 3:679–686, 2010.
Nappi, F., M. Lusini, C. Spadaccio, A. Nenna, E. Covino, C. Acar, and M. Chello. Papillary muscle approximation versus restrictive annuloplasty alone for severe ischemic mitral regurgitation. J. Am. Coll. Cardiol. 67:2334–2346, 2016.
Nkomo, V. T., J. M. Gardin, T. N. Skelton, J. S. Gottdiener, C. G. Scott, and M. Enriquez-Sarano. Burden of valvular heart diseases: a population-based study. Lancet 368:1005–1011, 2006.
Richards, A. L., R. C. Cook, G. Bolotin, and G. D. Buckner. A dynamic heart system to facilitate the development of mitral valve repair techniques. Ann. Biomed. Eng. 37:651–660, 2009.
Siefert, A. W., and R. L. Siskey. Bench models for assessing the mechanics of mitral valve repair and percutaneous surgery. Cardiovasc. Eng. Technol. 6:193–207, 2015.
Sturla, F., R. Vismara, M. Jaworek, E. Votta, P. Romitelli, O. A. Pappalardo, F. Lucherini, C. Antona, G. B. Fiore, and A. Redaelli. In vitro and in silico approaches to quantify the effects of the Mitraclip® system on mitral valve function. J. Biomech. 50:83–92, 2017.
Taramasso, M., M. Y. Emmert, D. Reser, A. Guidotti, N. Cesarovic, M. Campagnol, A. Addis, F. Nietlispach, S. P. Hoerstrup, and F. Maisano. Pre-clinical in vitro and in vivo models for heart valve therapies. J. Cardiovasc. Transl. Res. 8:319–327, 2015.
Tibayan, F. A., F. Rodriguez, M. K. Zasio, L. Bailey, D. Liang, G. T. Daughters, F. Langer, N. B. Ingels, and D. C. Miller. Geometric distortions of the mitral valvular–ventricular complex in chronic ischemic mitral regurgitation. Circulation 108:116–121, 2003.
Timek, T. A., and D. C. Miller. Another multidisciplinary look at ischemic mitral regurgitation. Semin. Thorac. Cardiovasc. Surg. 23:220–231, 2011.
Timek, T. A., P. Dagum, D. T. Lai, D. Liang, G. T. Daughters, N. B. Ingels, and D. C. Miller. Pathogenesis of mitral regurgitation in tachycardia-induced cardiomyopathy. Circulation 104:I-47–I-53, 2001.
Vismara, R., A. Pavesi, E. Votta, M. Taramasso, F. Maisano, and G. B. Fiore. A pulsatile simulator for the in vitro analysis of the mitral valve with tri-axial papillary muscle displacement. Int. J. Artif. Organs 34:383–391, 2011.
Vismara, R., G. Gelpi, S. Prabhu, P. Romitelli, L. G. Troxler, A. Mangini, C. Romagnoni, M. Contino, D. T. Van Hoven, F. Lucherini, M. Jaworek, A. Redaelli, G. B. Fiore, and C. Antona. Transcatheter edge-to-edge treatment of functional tricuspid regurgitation in an ex vivo pulsatile heart model. J. Am. Coll. Cardiol. 68:1024–1033, 2016.
Vismara, R., A. M. Leopaldi, M. Piola, C. Asselta, M. Lemma, C. Antona, A. Redaelli, F. van de Vosse, M. Rutten, and G. B. Fiore. In vitro assessment of mitral valve function in cyclically pressurized porcine hearts. Med. Eng. Phys. 38:346–353, 2016.
Yamauchi, H., E. N. Feins, N. V. Vasilyev, S. Shimada, D. Zurakowski, and P. J. Del Nido. Creation of nonischemic functional mitral regurgitation by annular dilatation and nonplanar modification in a chronic in vivo swine model. Circulation 2013. doi:10.1161/CIRCULATIONAHA.112.000396.
Yamauchi, H., E. N. Feins, N. V. Vasilyev, S. Shimada, D. Zurakowski, and P. J. Del Nido. Creation of nonischemic functional mitral regurgitation by annular dilatation and nonplanar modification in a chronic in vivo swine model. Circulation 128:S263–S270, 2013.
Acknowledgments
The authors would like to thank Valeria Quattrocchi (Philips SpA Healthcare, Monza, Italy) for the technical support in obtaining the echocardiographic images.
Disclosures
None.
Funding
This work was supported in part by the European Commission within the Horizon 2020 Framework through the MSCA-ITN-ETN European Training Networks (Project Number 642458) and by Fondazione per la Ricerca in Cardiochirurgia ONLUS, Milano, Italy.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Scott I. Simon oversaw the review of this article.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary Video (AVI 15070 kb)
Rights and permissions
About this article
Cite this article
Jaworek, M., Lucherini, F., Romagnoni, C. et al. Modelling of Lesions Associated with Functional Mitral Regurgitation in an Ex Vivo Platform. Ann Biomed Eng 45, 2324–2334 (2017). https://doi.org/10.1007/s10439-017-1885-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-017-1885-6