Abstract
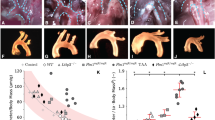
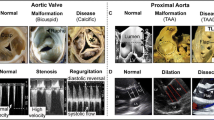
Aortopathy is characterized by vascular smooth muscle cell (VSMC) abnormalities and elastic fiber fragmentation. Elastin insufficient (Eln +/−) mice demonstrate latent aortopathy similar to human disease. We hypothesized that aortopathy manifests primarily in the aorto-pulmonary septal (APS) side of the thoracic aorta due to asymmetric cardiac neural crest (CNC) distribution. Anatomic (aortic root vs. ascending aorta) and molecular (APS vs. non-APS) regions of proximal aorta tissue were examined in adult and aged wild type (WT) and mutant (Eln +/−) mice. CNC, VSMCs, elastic fiber architecture, proteoglycan expression, morphometrics and biomechanical properties were examined using histology, 3D reconstruction, micropipette aspiration and in vivo magnetic resonance imaging (MRI). In the APS side of Eln +/− aorta, Sonic Hedgehog (SHH) is decreased while SM22 is increased. Elastic fiber architecture abnormalities are present in the Eln +/− aortic root and APS ascending aorta, and biglycan is increased in the aortic root while aggrecan is increased in the APS aorta. The Eln +/− ascending aorta is stiffer than the aortic root, the APS side is thicker and stiffer than the non-APS side, and significant differences in the individual aortic root sinuses are observed. Asymmetric structure–function abnormalities implicate regional CNC dysregulation in the development and progression of aortopathy.








Similar content being viewed by others
Abbreviations
- APS:
-
Aorto-pulmonary septum
- CNC:
-
Cardiac neural crest
- ECM:
-
Extracellular matrix
- EFF:
-
Elastic fiber fragmentation
- Eln −/− :
-
Homozygous deletion of elastin gene
- Eln +/− :
-
Heterozygous deletion of elastin gene
- IOD:
-
Integrated optical density
- MRI:
-
Magnetic resonance imaging
- MRSD:
-
Maximum rate of systolic distension
- PTA:
-
Persistent truncus arteriosus
- SHH:
-
Sonic hedgehog
- TAA:
-
Thoracic aortic aneurysm
- VSMC:
-
Vascular smooth muscle cell
- WT:
-
Wild type
References
Anderson, R. H. Clinical anatomy of the aortic root. Heart 84:670–673, 2000.
Bauer, M., M. Pasic, R. Meyer, N. Goetze, U. Bauer, H. Siniawski, and R. Hetzer. Morphometric analysis of aortic media in patients with bicuspid and tricuspid aortic valve. Ann. Thorac. Surg. 74:58–62, 2002.
Becker, A. E., M. J. Becker, and J. E. Edwards. Pathology of the semilunar valve in persistent truncus arteriosus. J. Thorac. Cardiovasc. Surg. 62:16–26, 1971.
Bergwerff, M., M. C. DeRuiter, R. E. Poelmann, and A. C. Gittenberger-de Groot. Onset of elastogenesis and downregulation of smooth muscle actin as distinguishing phenomena in artery differentiation in the chick embryo. Anat. Embryol. (Berl). 194:545–557, 1996.
Bergwerff, M., M. E. Verberne, M. C. DeRuiter, R. E. Poelmann, and A. C. Gittenberger-de Groot. Neural crest cell contribution to the developing circulatory system: implications for vascular morphology? Circ. Res. 82:221–231, 1998.
Bruneau, B. G. The developmental genetics of congenital heart disease. Nature 451:943–948, 2008.
Calder, L., R. Van Praagh, S. Van Praagh, W. P. Sears, R. Corwin, A. Levy, J. D. Keith, and M. H. Paul. Truncus arteriosus communis. Clinical, angiocardiographic, and pathologic findings in 100 patients. Am. Heart J. 92:23–38, 1976.
Carlo, W. F., E. D. McKenzie, and T. C. Slesnick. Root dilation in patients with truncus arteriosus. Congenit. Heart Dis. 6:228–233, 2011.
Cattell, M. A., P. S. Hasleton, and J. C. Anderson. Glycosaminoglycan content is increased in dissecting aneurysms of human thoracic aorta. Clin. Chim. Acta 226:29–46, 1994.
Cheung, C., A. S. Bernardo, M. W. Trotter, R. A. Pedersen, and S. Sinha. Generation of human vascular smooth muscle subtypes provides insight into embryological origin-dependent disease susceptibility. Nat. Biotechnol. 30:165–173, 2012.
Choudhary, B., Y. Ito, T. Makita, T. Sasaki, Y. Chai, and H. M. Sucov. Cardiovascular malformations with normal smooth muscle differentiation in neural crest-specific type II TGFbeta receptor (Tgfbr2) mutant mice. Dev. Biol. 289:420–429, 2006.
Creazzo, T. L., R. E. Godt, L. Leatherbury, S. J. Conway, and M. L. Kirby. Role of cardiac neural crest cells in cardiovascular development. Annu. Rev. Physiol. 60:267–286, 1998.
Dodou, E., M. P. Verzi, J. P. Anderson, S. M. Xu, and B. L. Black. Mef2c is a direct transcriptional target of ISL1 and GATA factors in the anterior heart field during mouse embryonic development. Development 131:3931–3942, 2004.
Donato Aquaro, G., L. Ait-Ali, M. L. Basso, M. Lombardi, A. Pingitore, and P. Festa. Elastic properties of aortic wall in patients with bicuspid aortic valve by magnetic resonance imaging. Am. J. Cardiol. 108:81–87, 2011.
Eronen, M., M. Peippo, A. Hiippala, M. Raatikka, M. Arvio, R. Johansson, and M. Kahkonen. Cardiovascular manifestations in 75 patients with Williams syndrome. J. Med. Genet. 39:554–558, 2002.
Faury, G., M. Pezet, R. H. Knutsen, W. A. Boyle, S. P. Heximer, S. E. McLean, R. K. Minkes, K. J. Blumer, A. Kovacs, D. P. Kelly, D. Y. Li, B. Starcher, and R. P. Mecham. Developmental adaptation of the mouse cardiovascular system to elastin haploinsufficiency. J. Clin. Invest. 112:1419–1428, 2003.
Feng, M., S. Whitesall, Y. Zhang, M. Beibel, L. D’Alecy, and K. DiPetrillo. Validation of volume-pressure recording tail-cuff blood pressure measurements. Am. J. Hypertens. 21:1288–1291, 2008.
Goddeeris, M. M., R. Schwartz, J. Klingensmith, and E. N. Meyers. Independent requirements for Hedgehog signaling by both the anterior heart field and neural crest cells for outflow tract development. Development 134:1593–1604, 2007.
Goergen, C. J., K. N. Barr, D. T. Huynh, J. R. Eastham-Anderson, G. Choi, M. Hedehus, R. L. Dalman, A. J. Connolly, C. A. Taylor, P. S. Tsao, and J. M. Greve. In vivo quantification of murine aortic cyclic strain, motion, and curvature: implications for abdominal aortic aneurysm growth. J. Magn. Reson. Imaging 32:847–858, 2010.
Grande, K. J., R. P. Cochran, P. G. Reinhall, and K. S. Kunzelman. Stress variations in the human aortic root and valve: the role of anatomic asymmetry. Ann. Biomed. Eng. 26:534–545, 1998.
Guilak, F., L. G. Alexopoulos, M. A. Haider, H. P. Ting-Beall, and L. A. Setton. Zonal uniformity in mechanical properties of the chondrocyte pericellular matrix: micropipette aspiration of canine chondrons isolated by cartilage homogenization. Ann. Biomed. Eng. 33:1312–1318, 2005.
Gundiah, N., K. Kam, P. B. Matthews, J. Guccione, H. A. Dwyer, D. Saloner, T. A. Chuter, T. S. Guy, M. B. Ratcliffe, and E. E. Tseng. Asymmetric mechanical properties of porcine aortic sinuses. Ann. Thorac. Surg. 85:1631–1638, 2008.
Hahn, R. T., M. J. Roman, A. H. Mogtader, and R. B. Devereux. Association of aortic dilation with regurgitant, stenotic and functionally normal bicuspid aortic valves. J. Am. Coll. Cardiol. 19:283–288, 1992.
Hallidie-Smith, K. A., and S. Karas. Cardiac anomalies in Williams-Beuren syndrome. Arch. Dis. Child. 63:809–813, 1988.
Heiberg, E., J. Sjogren, M. Ugander, M. Carlsson, H. Engblom, and H. Arheden. Design and validation of segment—freely available software for cardiovascular image analysis. BMC Med. Imaging 10:1, 2010.
Hinton, R. B. Bicuspid aortic valve and thoracic aortic aneurysm: three patient populations, two disease phenotypes, and one shared genotype. Cardiol. Res. Pract. 2012:926975, 2012.
Hinton, R. B., J. Adelman-Brown, S. Witt, V. K. Krishnamurthy, H. Osinska, B. Sakthivel, J. F. James, D. Y. Li, D. A. Narmoneva, R. P. Mecham, and D. W. Benson. Elastin haploinsufficiency results in progressive aortic valve malformation and latent valve disease in a mouse model. Circ. Res. 107:549–557, 2010.
Hinton, Jr., R. B., J. Lincoln, G. H. Deutsch, H. Osinska, P. B. Manning, D. W. Benson, and K. E. Yutzey. Extracellular matrix remodeling and organization in developing and diseased aortic valves. Circ. Res. 98:1431–1438, 2006.
Hiratzka, L. F., G. L. Bakris, J. A. Beckman, R. M. Bersin, V. F. Carr, D. E. Casey, Jr., K. A. Eagle, L. K. Hermann, E. M. Isselbacher, E. A. Kazerooni, N. T. Kouchoukos, B. W. Lytle, D. M. Milewicz, D. L. Reich, S. Sen, J. A. Shinn, L. G. Svensson, and D. M. Williams. 2010 ACCF/AHA/AATS/ACR/ASA/SCA/SCAI/SIR/STS/SVM guidelines for the diagnosis and management of patients with Thoracic Aortic Disease: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines, American Association for Thoracic Surgery, American College of Radiology, American Stroke Association, Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, Society of Interventional Radiology, Society of Thoracic Surgeons, and Society for Vascular Medicine. Circulation 121:e266–e369, 2010.
Ho, S. Y. Structure and anatomy of the aortic root. Eur. J. Echocardiogr. 10:i3–i10, 2009.
Keane, J. F., K. E. Fellows, C. G. LaFarge, A. S. Nadas, and W. F. Bernhard. The surgical management of discrete and diffuse supravalvar aortic stenosis. Circulation 54:112–117, 1976.
Kirby, M. L., T. F. Gale, and D. E. Stewart. Neural crest cells contribute to normal aorticopulmonary septation. Science 220:1059–1061, 1983.
Kirby, M. L., and K. L. Waldo. Role of neural crest in congenital heart disease. Circulation 82:332–340, 1990.
Krishnamurthy, V. K., F. Guilak, D. A. Narmoneva, and R. B. Hinton. Regional structure-function relationships in mouse aortic valve tissue. J. Biomech. 44:77–83, 2011.
Krishnamurthy, V. K., A. M. Opoka, C. B. Kern, F. Guilak, D. A. Narmoneva, and R. B. Hinton. Maladaptive matrix remodeling and regional biomechanical dysfunction in a mouse model of aortic valve disease. Matrix Biol. 31:197–205, 2012.
Li, D. Y., B. Brooke, E. C. Davis, R. P. Mecham, L. K. Sorensen, B. B. Boak, E. Eichwald, and M. T. Keating. Elastin is an essential determinant of arterial morphogenesis. Nature 393:276–280, 1998.
Li, D. Y., G. Faury, D. G. Taylor, E. C. Davis, W. A. Boyle, R. P. Mecham, P. Stenzel, B. Boak, and M. T. Keating. Novel arterial pathology in mice and humans hemizygous for elastin. J. Clin. Invest. 102:1783–1787, 1998.
Majesky, M. W. Developmental basis of vascular smooth muscle diversity. Arterioscler. Thromb. Vasc. Biol. 27:1248–1258, 2007.
McLean, M., and J. W. Prothero. Three-dimensional reconstruction from serial sections. V. Calibration of dimensional changes incurred during tissue preparation and data processing. Anal. Quant. Cytol. Histol. 13:269–278, 1991.
Morrison, T. M., G. Choi, C. K. Zarins, and C. A. Taylor. Circumferential and longitudinal cyclic strain of the human thoracic aorta: age-related changes. J. Vasc. Surg. 49:1029–1036, 2009.
Nakamura, T., M. C. Colbert, and J. Robbins. Neural crest cells retain multipotential characteristics in the developing valves and label the cardiac conduction system. Circ. Res. 98:1547–1554, 2006.
Neeb, Z., J. D. Lajiness, E. Bolanis, and S. J. Conway. Cardiac outflow tract anomalies. Wiley Interdiscip. Rev. Dev. Biol. 2:499–530, 2013.
Owens, G. K., M. S. Kumar, and B. R. Wamhoff. Molecular regulation of vascular smooth muscle cell differentiation in development and disease. Physiol. Rev. 84:767–801, 2004.
Pachulski, R. T., A. L. Weinberg, and K. L. Chan. Aortic aneurysm in patients with functionally normal or minimally stenotic bicuspid aortic valve. Am. J. Cardiol. 67:781–782, 1991.
Passman, J. N., X. R. Dong, S. P. Wu, C. T. Maguire, K. A. Hogan, V. L. Bautch, and M. W. Majesky. A sonic hedgehog signaling domain in the arterial adventitia supports resident Sca1+ smooth muscle progenitor cells. Proc. Natl Acad. Sci. U.S.A. 105:9349–9354, 2008.
Pezet, M., M. P. Jacob, B. Escoubet, D. Gheduzzi, E. Tillet, P. Perret, P. Huber, D. Quaglino, R. Vranckx, D. Y. Li, B. Starcher, W. A. Boyle, R. P. Mecham, and G. Faury. Elastin haploinsufficiency induces alternative aging processes in the aorta. Rejuvenation Res. 11:97–112, 2008.
Rosenquist, T. H., and A. C. Beall. Elastogenic cells in the developing cardiovascular system. Smooth muscle, nonmuscle, and cardiac neural crest. Ann. N. Y. Acad. Sci. 588:106–119, 1990.
Rosenquist, T. H., A. C. Beall, L. Modis, and R. Fishman. Impaired elastic matrix development in the great arteries after ablation of the cardiac neural crest. Anat. Rec. 226:347–359, 1990.
Schonherr, E., H. T. Jarvelainen, L. J. Sandell, and T. N. Wight. Effects of platelet-derived growth factor and transforming growth factor-beta 1 on the synthesis of a large versican-like chondroitin sulfate proteoglycan by arterial smooth muscle cells. J. Biol. Chem. 266:17640–17647, 1991.
Snarr, B. S., E. E. Wirrig, A. L. Phelps, T. C. Trusk, and A. Wessels. A spatiotemporal evaluation of the contribution of the dorsal mesenchymal protrusion to cardiac development. Dev. Dyn. 236:1287–1294, 2007.
Stoller, J. Z., and J. A. Epstein. Cardiac neural crest. Semin. Cell Dev. Biol. 16:704–715, 2005.
Szabo, Z., M. W. Crepeau, A. L. Mitchell, M. J. Stephan, R. A. Puntel, K. Yin Loke, R. C. Kirk, and Z. Urban. Aortic aneurysmal disease and cutis laxa caused by defects in the elastin gene. J. Med. Genet. 43:255–258, 2006.
Tadros, T. M., M. D. Klein, and O. M. Shapira. Ascending aortic dilatation associated with bicuspid aortic valve: pathophysiology, molecular biology, and clinical implications. Circulation 119:880–890, 2009.
Theret, D. P., M. J. Levesque, M. Sato, R. M. Nerem, and L. T. Wheeler. The application of a homogeneous half-space model in the analysis of endothelial cell micropipette measurements. J. Biomech. Eng. 110:190–199, 1988.
Treasure, T., J. Pepper, T. Golesworthy, R. Mohiaddin, and R. H. Anderson. External aortic root support: NICE guidance. Heart 98:65–68, 2012.
Wagenseil, J. E., and R. P. Mecham. Vascular extracellular matrix and arterial mechanics. Physiol. Rev. 89:957–989, 2009.
Wagenseil, J. E., N. L. Nerurkar, R. H. Knutsen, R. J. Okamoto, D. Y. Li, and R. P. Mecham. Effects of elastin haploinsufficiency on the mechanical behavior of mouse arteries. Am. J. Physiol. Heart Circ. Physiol. 289:H1209–H1217, 2005.
Waldo, K. L., M. R. Hutson, C. C. Ward, M. Zdanowicz, H. A. Stadt, D. Kumiski, R. Abu-Issa, and M. L. Kirby. Secondary heart field contributes myocardium and smooth muscle to the arterial pole of the developing heart. Dev. Biol. 281:78–90, 2005.
Wang, J., A. Nagy, J. Larsson, M. Dudas, H. M. Sucov, and V. Kaartinen. Defective ALK5 signaling in the neural crest leads to increased postmigratory neural crest cell apoptosis and severe outflow tract defects. BMC Dev. Biol. 6:51, 2006.
Washington Smoak, I., N. A. Byrd, R. Abu-Issa, M. M. Goddeeris, R. Anderson, J. Morris, K. Yamamura, J. Klingensmith, and E. N. Meyers. Sonic hedgehog is required for cardiac outflow tract and neural crest cell development. Dev. Biol. 283:357–372, 2005.
Wyffels, J. T. Principles and techniques of electron microscopy: biological applications, fourth edition, by M. A. Hayat. Microsc. Microanal. 7:66, 2001.
Xie, W. B., Z. Li, N. Shi, X. Guo, J. Tang, W. Ju, J. Han, T. Liu, E. P. Bottinger, Y. Chai, P. A. Jose, and S. Y. Chen. Smad2 and myocardin-related transcription factor B cooperatively regulate vascular smooth muscle differentiation from neural crest cells. Circ. Res. 113:e76–e86, 2013.
Ke, Y., and R. Sukthankar. PCA-SIFT: a more distinctive representation for local image descriptors. Proceedings of Computer Vision and Pattern Recognition, 2004.
Yacoub, M. H., P. J. Kilner, E. J. Birks, and M. Misfeld. The aortic outflow and root: a tale of dynamism and crosstalk. Ann. Thorac. Surg. 68:S37–S43, 1999.
Zhao, X., R. Pratt, and J. Wansapura. Quantification of aortic compliance in mice using radial phase contrast MRI. J. Magn. Reson. Imaging 30:286–291, 2009.
Acknowledgments
We thank Amy Opoka for her assistance. We also thank Dr. Dean Y. Li (University of Utah) for providing the elastin knockout mice and Dr. Robert P. Mecham (Washington University) for helpful discussions. Present address for Varun K. Krishnamurthy: Department of Bioengineering, Rice University, Houston, TX 77005, USA. This work was supported by the AHA 11PRE7210044 (VKK), NIH HL086856-01 (RLG), NIH HL085122 (RBH), and Cincinnati Children’s Research Foundation (RBH).
Disclosures
The authors have nothing to disclose.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Jane Grande-Allen oversaw the review of this article.
Varun K. Krishnamurthy and Ashlie N. Evans contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary material 1 (M4 V 7873 kb)
Supplementary material 2 (M4 V 8715 kb)
Rights and permissions
About this article
Cite this article
Krishnamurthy, V.K., Evans, A.N., Wansapura, J.P. et al. Asymmetric Cell–Matrix and Biomechanical Abnormalities in Elastin Insufficiency Induced Aortopathy. Ann Biomed Eng 42, 2014–2028 (2014). https://doi.org/10.1007/s10439-014-1072-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-014-1072-y