Abstract
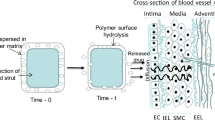
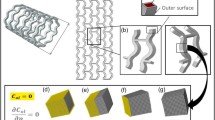
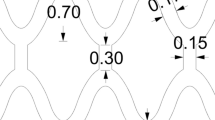
Fully bioresorbable vascular scaffolds (BVS) are attractive platforms for the treatment of ischemic artery disease owing to their intrinsic ability to uncage the treated vessel after the initial scaffolding phase, thereby allowing for the physiological conditioning that is essential to cellular function and vessel healing. Although scaffold erosion confers distinct advantages over permanent endovascular devices, high transient by-product concentrations within the arterial wall could induce inflammatory and immune responses. To better understand these risks, we developed in this study an integrated computational model that characterizes the bulk degradation and by-product fate for a representative BVS composed of poly(l-lactide) (PLLA). Parametric studies were conducted to evaluate the relative impact of PLLA degradation rate, arterial remodeling, and metabolic activity on the local lactic acid (LA) concentration within arterial tissue. The model predicts that both tissue remodeling and PLLA degradation kinetics jointly modulate LA fate and suggests that a synchrony of these processes could minimize transient concentrations within local tissue. Furthermore, simulations indicate that LA metabolism is a relatively poor tissue clearance mechanism compared to convective and diffusive transport processes. Mechanistic understanding of factors governing by-product fate may provide further insights on clinical outcome and facilitate development of future generation scaffolds.






Similar content being viewed by others
References
Adachi, T., Y. Osako, M. Tanaka, M. Hojo, and S. J. Hollister. Framework for optimal design of porous scaffold microstructure by computational simulation of bone regeneration. Biomaterials 27(21):3964–3972, 2006.
Antheunis, H., J.-C. van der Meer, M. de Geus, W. Kingma, and C. E. Koning. Improved mathematical model for the hydrolytic degradation of aliphatic polyesters. Macromolecules 42(7):2462–2471, 2009.
Balakrishnan, B., J. F. Dooley, G. Kopia, and E. R. Edelman. Intravascular drug release kinetics dictate arterial drug deposition, retention, and distribution. J. Control Release 123(2):100–108, 2007.
Chen, Y., S. Zhou, and Q. Li. Mathematical modeling of degradation for bulk-erosive polymers: applications in tissue engineering scaffolds and drug delivery systems. Acta Biomater. 7(3):1140–1149, 2011.
Chen, Y., S. Zhou, and Q. Li. Microstructure design of biodegradable scaffold and its effect on tissue regeneration. Biomaterials 32(22):5003–5014, 2011.
Colombo, A., and E. Karvouni. Biodegradable stents: “fulfilling the mission and stepping away”. Circulation 102(4):371–373, 2000.
Deen, W. M. Analysis of Transport Phenomena. New York: Oxford University Press, 597 pp, 1998.
Flory, P. J. Principles of Polymer Chemistry. Ithaca: Cornell University Press, 688 pp, 1953.
Göpferich, A. Mechanisms of polymer degradation and erosion. Biomaterials 17(2):103–114, 1996.
Han, X., and J. Pan. Polymer chain scission, oligomer production and diffusion: a two-scale model for degradation of bioresorbable polyesters. Acta Biomater. 7(2):538–547, 2011.
Higo, T., Y. Ueda, J. Oyabu, K. Okada, M. Nishio, A. Hirata, K. Kashiwase, N. Ogasawara, S. Hirotani, and K. Kodama. Atherosclerotic and thrombogenic neointima formed over sirolimus drug-eluting stent: an angioscopic study. JACC Cardiovasc. Imaging 2(5):616–624, 2009.
Iakovou, I., T. Schmidt, E. Bonizzoni, L. Ge, G. M. Sangiorgi, G. Stankovic, F. Airoldi, A. Chieffo, M. Montorfano, M. Carlino, I. Michev, N. Corvaja, C. Briguori, U. Gerckens, E. Grube, and A. Colombo. Incidence, predictors, and outcome of thrombosis after successful implantation of drug-eluting stents. J. Am. Med. Assoc. 293(17):2126–2130, 2005.
Jagur-Grodzinski, J. Polymers for tissue engineering, medical devices, and regenerative medicine. Concise general review of recent studies. Polym. Adv. Technol. 17(6):395–418, 2006.
Kedem, O., and A. Katchalsky. Thermodynamic analysis of the permeability of biological membranes to non-electrolytes. Biochim. Biophys. Acta 27:229–246, 1958.
Kimura, T., K. Abe, S. Shizuta, K. Odashiro, Y. Yoshida, K. Sakai, K. Kaitani, K. Inoue, Y. Nakagawa, H. Yokoi, M. Iwabuchi, N. Hamasaki, H. Nosaka, and M. Nobuyoshi. Long-term clinical and angiographic follow-up after coronary stent placement in native coronary arteries. Circulation 105(25):2986–2991, 2002.
Kobayashi, M., I. Fujita, S. Itagaki, T. Hirano, and K. Iseki. Transport mechanism for L-lactic acid in human myocytes using human prototypic embryonal rhabdomyosarcoma cell line (RD cells). Biol. Pharm. Bull. 28(7):1197–1201, 2005.
Kolachalama, V. B., E. G. Levine, and E. R. Edelman. Luminal flow amplifies stent-based drug deposition in arterial bifurcations. PLoS One 4(12):e8105, 2009.
Kolachalama, V. B., A. R. Tzafriri, D. Y. Arifin, and E. R. Edelman. Luminal flow patterns dictate arterial drug deposition in stent-based delivery. J. Control Release 133(1):24–30, 2009.
Leenslag, J. W., A. J. Pennings, R. R. M. Bos, F. R. Rozema, and G. Boering. Resorbable materials of poly(l-lactide): VII. In vivo and in vitro degradation. Biomaterials 8(4):311–314, 1987.
Meyer, G., R. Merval, and A. Tedgui. Effects of pressure-induced stretch and convection on low-density lipoprotein and albumin uptake in the rabbit aortic wall. Circ. Res. 79(3):532–540, 1996.
Miller, R. A., J. M. Brady, and D. E. Cutright. Degradation rates of oral resorbable implants (polylactates and polyglycolates): rate modification with changes in PLA/PGA copolymer ratios. J. Biomed. Mater. Res. 11(5):711–719, 1977.
Onuma, Y., P. W. Serruys, L. E. L. Perkins, T. Okamura, N. Gonzalo, H. M. García-García, E. Regar, M. Kamberi, J. C. Powers, R. Rapoza, H. van Beusekom, W. van der Giessen, and R. Virami. Intracoronary optical coherence tomography and histology at 1 month and 2, 3, and 4 years after implantation of everolimus-eluting bioresorbable vascular scaffolds in a porcine coronary artery model. Circulation 122(22):2288–2300, 2010.
Pamula, E., and E. Menaszek. In vitro and in vivo degradation of poly(l: -lactide-co-glycolide) films and scaffolds. J. Mater. Sci. Mater. Med. 19(5):2063–2070, 2008.
Perale, G., P. Arosio, D. Moscatelli, V. Barri, M. Müller, S. Maccagnan, and M. Masi. A new model of resorbable device degradation and drug release: transient 1-dimension diffusional model. J. Control Release 136(3):196–205, 2009.
Prabhu, S., and S. Hossainy. Modeling of degradation and drug release from a biodegradable stent coating. J. Biomed. Mater. Res. A 80A(3):732–741, 2007.
Siepmann, J., K. Elkharraz, F. Siepmann, and D. Klose. How autocatalysis accelerates drug release from PLGA-based microparticles: a quantitative treatment. Biomacromolecules 6(4):2312–2319, 2005.
Soares, J. S., and P. Zunino. A mixture model for water uptake, degradation, erosion and drug release from polydisperse polymeric networks. Biomaterials 31(11):3032–3042, 2010.
Sun, N., N. Wood, A. Hughes, S. Thom, and X. Xu. Fluid-wall modelling of mass transfer in an axisymmetric stenosis: effects of shear-dependent transport properties. Ann. Biomed. Eng. 34(7):1119–1128, 2006.
Tada, S., and J. Tarbell. Fenestral pore size in the internal elastic lamina affects transmural flow distribution in the artery wall. Ann. Biomed. Eng. 29(6):456–466, 2001.
Thombre, A. G., and K. J. Himmelstein. A simultaneous transport-reaction model for controlled drug delivery from catalyzed bioerodable polymer matrices. AICHE J. 31(5):759–766, 1985.
von Burkersroda, F., L. Schedl, and A. Göpferich. Why degradable polymers undergo surface erosion or bulk erosion. Biomaterials 23(21):4221–4231, 2002.
von Recum, H. A., R. L. Cleek, S. G. Eskin, and A. G. Mikos. Degradation of polydispersed poly(l-lactic acid) to modulate lactic acid release. Biomaterials 16(6):441–447, 1995.
Wang, Y., J. Pan, X. Han, C. Sinka, and L. Ding. A phenomenological model for the degradation of biodegradable polymers. Biomaterials 29(23):3393–3401, 2008.
Weir, N. A., F. J. Buchanan, J. F. Orr, and G. R. Dickson. Degradation of poly-l-lactide. Part 1: in vitro and in vivo physiological temperature degradation. Proc. IME H. J. Eng. Med. 218(5):307–319, 2004.
Yang, N., and K. Vafai. Modeling of low-density lipoprotein (LDL) transport in the artery—effects of hypertension. Int. J. Heat Mass Transf. 49(5–6):850–867, 2006.
Acknowledgments
This study was supported by the NIH grant (R01 GM-49039) to ERE and the National Science Foundation/EPSCoR Grant (EPS-0903795) to TS. The authors thank Tecplot, Inc. for generously providing software licenses for data visualization.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Kent Leach oversaw the review of this article.
Tarek Shazly and Vijaya B. Kolachalama contributed equally in this study.
Rights and permissions
About this article
Cite this article
Shazly, T., Kolachalama, V.B., Ferdous, J. et al. Assessment of Material By-Product Fate from Bioresorbable Vascular Scaffolds. Ann Biomed Eng 40, 955–965 (2012). https://doi.org/10.1007/s10439-011-0445-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-011-0445-8