Abstract
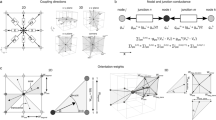
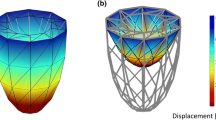
We introduce a 3D model of cardiac tissue to study at a microscopic level the relationship between tissue morphology and propagation of depolarization. Unlike the classical bidomain approach, in which tissue properties are described by the apparent conductivity of the tissue, in this “microdomain” approach, we included histology by modeling the actual shape of the intracellular and extracellular spaces that contain spatially distributed gap-junctions and membranes. The histological model of the tissue was generated by a computer algorithm that can be tuned to model different histological changes. For healthy tissue, the model predicted a realistic conduction velocity of 0.42 m/s based solely on the parameters derived from histology. A comparison with a brick-shaped, simplified model showed that conduction depended to a moderate extent on the shape of myocytes; a comparison with a one-dimensional bidomain model with the same overall shape and structure showed that the apparent conductivity of the tissue can be used to create an equivalent bidomain model. In summary, the microdomain approach offers a means of directly incorporating structural and functional parameters into models of cardiac activation and propagation and thus provides a valuable bridge between the cellular and tissue domains in the myocardium.








Similar content being viewed by others
References
Barnard, A. C. L., I. M. Duck, and M. S. Lynn. The application of electromagnetic theory to electrocardiology. I. Derivation of the integral equations. Biophys. J. 7:433–462, 1967.
Baumann, S. B., D. R. Wozny, S. K. Kelly, and F. M. Meno. The electrical conductivity of human cerebrospinal fluid at body temperature. IEEE Trans. Biomed. Eng. 44:220–223, 1997.
Brown, A. M., K. S. Lee, and T. Powell. Voltage clamp and internal perfusion of single rat heart muscle cells. J. Physiol. 318:455–477, 1981.
Campbell, S. E., A. M. Gerdes, and T. D. Smith. Comparison of regional differences in cardiac myocytes dimensions in rats, hamsters and guinea pigs. Anat. Rec. 219:53–59, 1987.
Cascio, W. E., H. Yang, T. A. Johnson, B. J. Muller-Borer, and J. J. Lemasters. Electrical properties and conduction in perfused papillary muscle. Circ. Res. 89:807–814, 2001.
Clerc, L. Directional differences of impulse spread in trabecular muscle from mammalian heart. J. Physiol. 255:335–346, 1976.
Crank, J., and O. Nicolson. A practical method for numerical evaluation of solutions of partial differential equations of the heat-conduction type. Proc. Camb. Phil. Soc. 43:50–67, 1947.
Forbes, M. S., and N. Sperelakis. Chapter 1—ultrastructure of mammalian cardiac muscle. In: Physiology and Pathophysiology of the Heart (3rd ed.). Norwell, MA: Kluwer Academic Publishers, 1995, pp. 1–35.
Gabriel, S., R. W. Lau, and C. Gabriel. The dielectric properties of biological tissues: I. Literature survey. Phys. Med. Biol. 41:2231–2249, 1996.
Gerdes, A. M., and F. H. Kasten. Morphometric study of endomyocardium and epimyocardium of the left ventricle in adult dogs. Am. J. Anat. 159(4):389–394, 1980.
Geselowitz, D. B. On the magnetic field generated outside an inhomogeneous volume conductor by internal current sources. IEEE Trans. Magn. MAG-6(2):346–347, 1970.
Harrild, D. M., and C. S. Henriquez. A computer model of normal conduction in the human atria. Circ. Res. 87:e25, 2000.
Henriquez, C. S. Simulating the electrical behavior of cardiac tissue using the bidomain model. Crit. Rev. Biomed. Eng. 21:1–77, 1993.
Hoyt, R. H., M. L. Cohen, and J. E. Saffitz. Distribution and three-dimensional structure of intercellular junctions in canine myocardium. Circ. Res. 64(3):563–574, 1989.
Luo, C. H., and Y. Rudy. A model of the ventricular cardiac action potential. Depolarization, repolarization, and their interaction. Circ. Res. 68(6):1501–1526, 1991.
Metzger, P., and R. Weingart. Electric current flow in cell pairs isolated from adult rat hearts. J. Physiol. 366:177–195, 1985.
Peters, N. S., N. J. Severs, S. M. Rothery, C. Lincoln, M. H. Yacoub, and C. R. Green. Spatiotempoaral relation between gap junctions and fascia adherens junctions during human ventricular myocardium. Circulation 90:713–725, 1994.
Plonsey, R., and D. B. Heppner. Considerations of quasi-stationarity in electrophysiological systems. Bull. Math. Biophys. 29:657–664, 1967.
Roberts, D. E., L. T. Hersch, and A. M. Scher. Influence of cardiac fiber orientation on wavefront voltage, conduction velocity and tissue resistivity. Circ. Res. 44:701–712, 1979.
Roberts, D. E., and A. M. Scher. Effect of tissue anisotropy on extracellualar potential fields in canine myocardium in situ. Circ. Res. 50:342–351, 1982.
Roberts, S. F., J. G. Stinstra, and C.S. Henriquez. Discrete multidomain: a unique computational model to study effects of a discontinuous cardiac microstructure on impulse propagation. Biophys. J. 95:3724–3737, 2008.
Satoh, H., L. M. D. Delbridge, L. A. Blatter, and D. M. Bers. Surface:volume relationship in cardiac myocytes studied with confocal microscopy and membrane capacitance measurements: species-dependence and developmental effects. Biophys. J. 70:1494–1504, 1996.
Shome, S., J. G. Stinstra, C. S. Henriquez, and R. S. MacLeod. Influence of extracellular potassium and reduced extracellular space on conduction velocity during acute ischemia: a simulation study. J. Electrocardiol. 39:S84–S85, 2006.
Sommer, J. R., and E. A. Johnson. Ultrastructure of cardiac muscle. In: Handbook of Physiology, Section 2: The Cardiovascular System, Vol. 1. American Physiological Society, 1979, pp. 113–186.
Spach, M. S. Microfibrosis produces electrical load variations due to loss of side-to-side cell connections. PACE 20:397–413, 1997.
Spach, M. S., J. F. Heidlage, E. R. Darken, E. Hofer, K. H. Raines, and C. F. Starmer. Cellular dvmax/dt reflects both membrane properties and the load presented by adjoining cells. Am. J. Physiol. (Heart Circ. Physiol.) 32:H1855–H1863, 1992.
Stinstra, J. G., B. Hopenfeld, and R. S. MacLeod. On the passive cardiac conductivity. Ann. Biomed. Eng. 33(12):1743–1751, 2005.
Stinstra, J. G., S. Roberts, J. Pormann, R. S. MacLeod, and C. S. Henriquez. A model of 3d propagation in discrete cardiac tissue. Comput. Cardiol. 33:41–44, 2006.
Stinstra, J. G., S. Shome, B. Hopenfeld, and R. S. MacLeod. Modeling the passive cardiac electrical conductivity during ischemia. Med. Biol. Eng. Comput. 43(6):776–782, 2005.
Trautman, E. D., and R. S. Newbower. A practical analysis of the electrical conductivity of blood. IEEE Trans. Biomed. Eng. 30(3):141–153, 1983.
Trayanova, N., G. Plank, and B. Rodriguez. What have we learned from mathematical models of defibrillation and postshock arrythmogenesis? Application of bidomain simulations. Heart Rhythm 3(10):1232–1235, 2006.
Acknowledgments
We acknowledge support for this work through NIH grants RO1 HL076767 and P41-RR12553-07 as well as the Nora Eccles Treadwell Foundation.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Peter E. McHugh oversaw the review of this article.
Rights and permissions
About this article
Cite this article
Stinstra, J., MacLeod, R. & Henriquez, C. Incorporating Histology into a 3D Microscopic Computer Model of Myocardium to Study Propagation at a Cellular Level. Ann Biomed Eng 38, 1399–1414 (2010). https://doi.org/10.1007/s10439-009-9883-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-009-9883-y